What Is MRI Scan? Plain-English Guide for Patients and Techs
What is MRI scan? Clear, plain-English answer with how it works, what to expect, safety, prep, and an MRI practice test to lock in the basics.
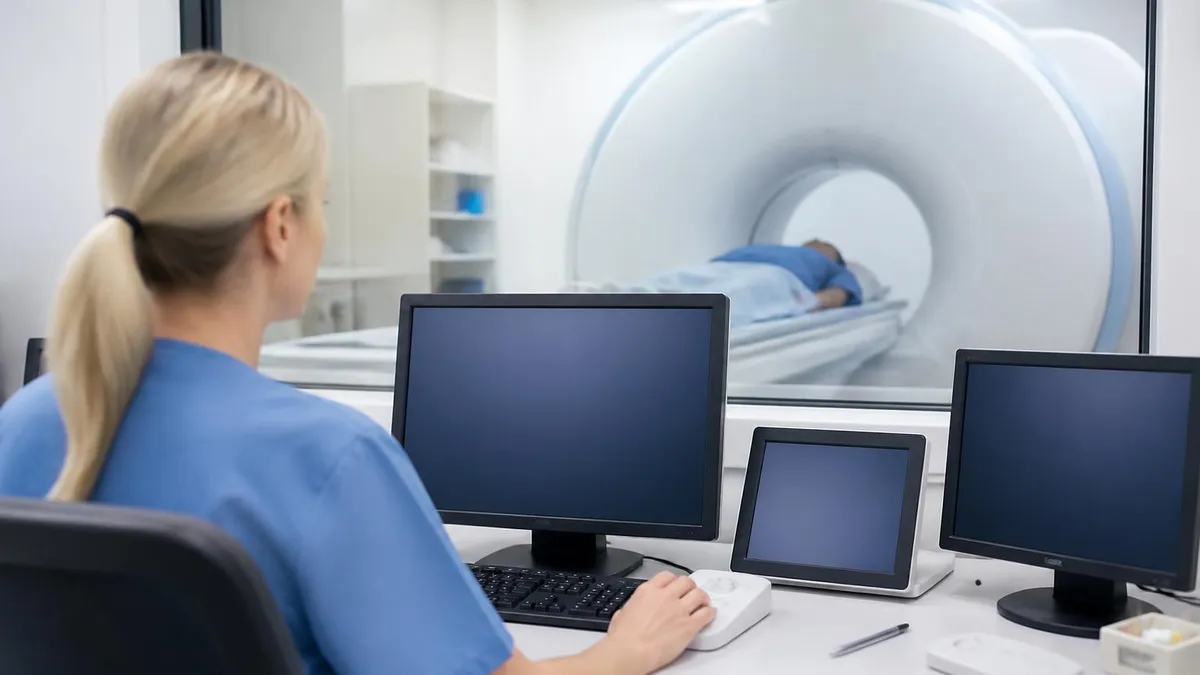
What Is an MRI Scan?
You schedule an MRI and the front desk hands you a clipboard, a metal-screening form, and a polite warning that it’s loud. So what is MRI scan, really? In plain English: an MRI (magnetic resonance imaging) is a non–X-ray imaging test that uses a strong magnet and radio waves to make detailed pictures of soft tissues—brain, spine, joints, organs—without any ionizing radiation. Hospitals lean on it because it sees nerves, ligaments, and tumors better than CT, and patients lean toward it because no radiation feels safer.
Here’s the part most articles skip—an MRI is not one thing. It’s a family of techniques. The same scanner can run a T1 sequence to outline anatomy, a T2 to highlight fluid, a diffusion-weighted scan to spot a fresh stroke, or a functional MRI to watch oxygen shifting through the brain while you wiggle your fingers. The magnet is the same. The recipe changes. That’s why your radiologist orders a “3T brain MRI with and without contrast” instead of just “an MRI.”
If you’re a patient, this guide tells you what to expect from the moment you walk in. If you’re a tech student prepping for a certification exam, the same explanation doubles as a clean review of the physics and safety rules you’ll be tested on. Either way, by the end you should be able to answer the question yourself—and you’ll have a short practice quiz to prove it.
MRI by the Numbers
How MRI Actually Works (Without the Heavy Math)
Your body is mostly water, and water is full of hydrogen atoms. Each hydrogen atom has a proton that spins like a tiny top with its own little magnetic field. Normally those spins point every which way. Drop the patient inside an MRI scanner—basically a giant superconducting magnet—and most of those spins line up along the magnet’s field.
Now the scanner sends in a quick burst of radio waves tuned to the resonant frequency of hydrogen. The protons absorb the energy, tip out of alignment, then relax back into place. As they relax, they emit a tiny radio signal of their own. The scanner’s coils pick up that signal, a computer maps it in three dimensions, and out the other side comes a grayscale image where fat, muscle, fluid, and tumor each have their own distinct shade.
Different tissues relax at different speeds. Fat snaps back fast. Water lingers. The scanner exploits that difference using two timing values—TR (repetition time) and TE (echo time)—to weight the image. Short TR and short TE gives you a T1-weighted image where fat looks bright and water looks dark. Long TR and long TE gives you T2, where water glows. That single trick—changing the timing recipe—is why one machine can answer a thousand different clinical questions.
The loud banging? That’s the gradient coils. They’re smaller magnets layered around the main one that switch on and off rapidly to encode spatial location. Every clunk and buzz is a gradient pulse changing the magnetic field by a few millitesla. Earplugs are mandatory for a reason.
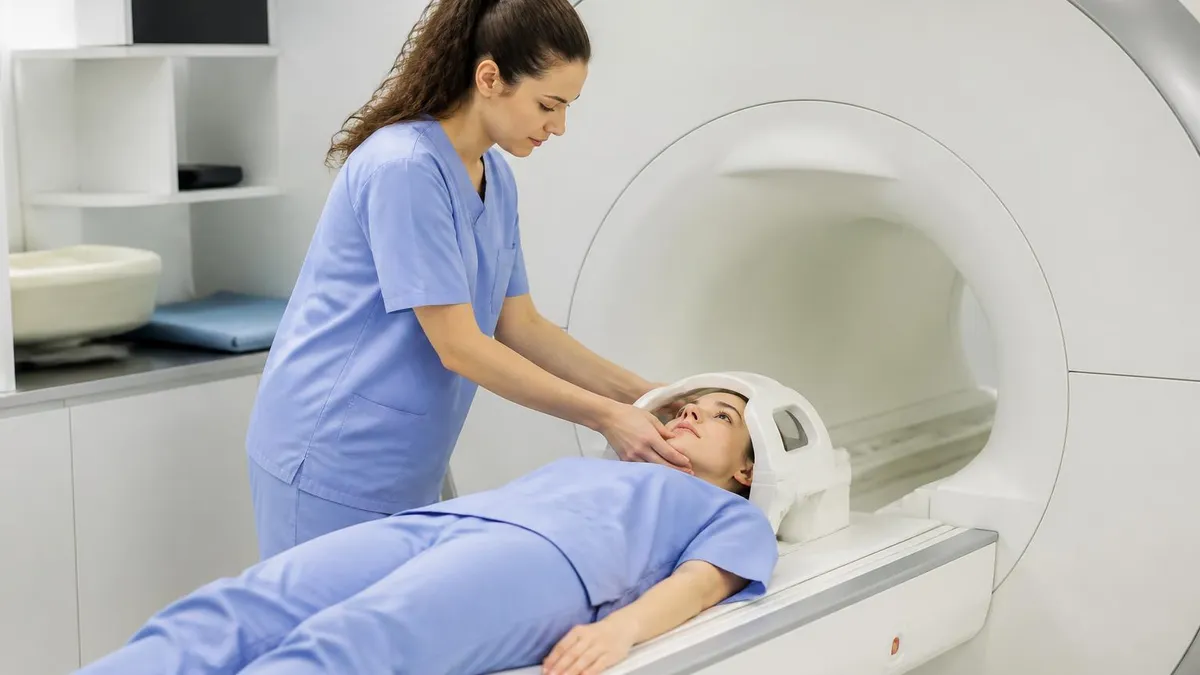
MRI = giant magnet + radio waves + math. The magnet lines up your hydrogen protons. Radio waves knock them sideways. As they snap back, they whisper a tiny signal that gets turned into an image. No X-rays, no radiation—just physics borrowed from chemistry labs in the 1940s.
MRI vs. CT vs. X-ray: Why Doctors Pick MRI
If MRI is so good, why does anyone get a CT? Speed and bone. CT scans take seconds, MRIs take 30 to 60 minutes. CT also crushes MRI when it comes to imaging bone fractures, lung tissue, and acute bleeds—places where radiation is a fair trade for a fast, sharp picture.
X-rays do one job well: a flat 2D view of dense structures, mostly bone and a bit of lung. Cheap, fast, low dose, but limited. MRI is the opposite end of the spectrum—slow, expensive, and exquisite at showing soft tissue. A torn ACL barely whispers on an X-ray. On a knee MRI, you can practically see the fibers fraying.
The decision tree most radiologists use looks something like this. Bone fracture? X-ray first. Head trauma in the ER? CT, because it catches bleeding fast. Sudden weakness or numbness? MRI of the brain or spine, because soft-tissue detail matters more than speed. Joint pain that won’t quit? MRI, because cartilage, tendons, and ligaments don’t show up on the others. The right tool depends on the question.
Common MRI Scan Types
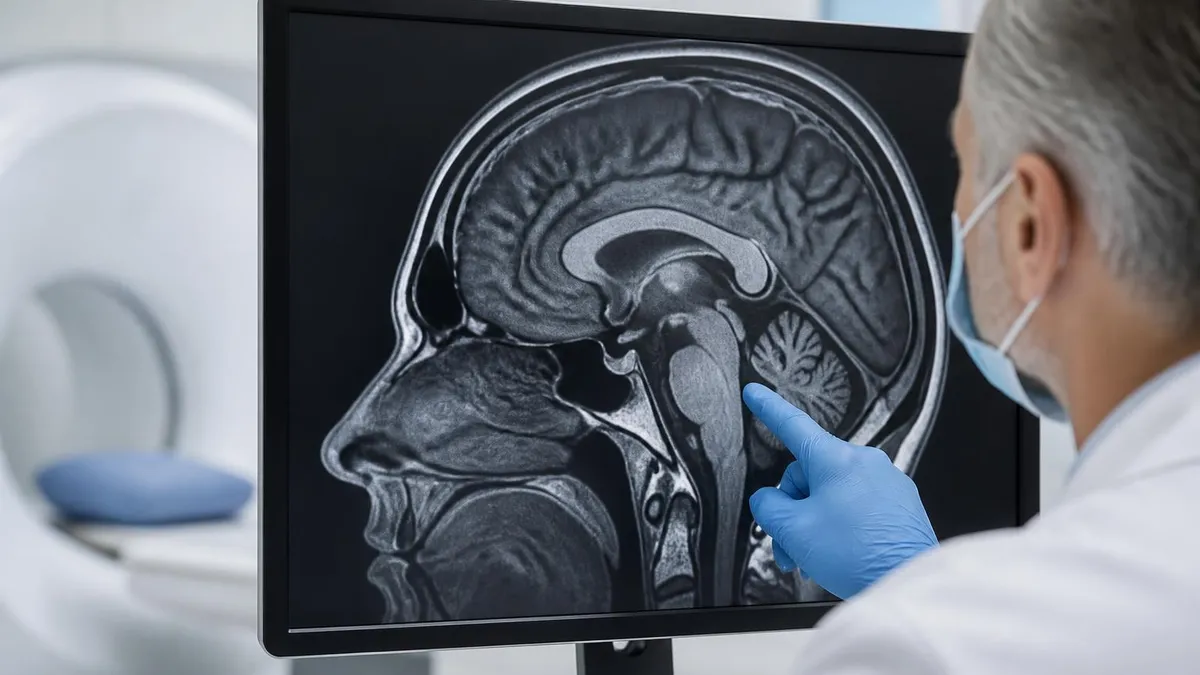
Detects strokes (especially acute ischemic ones via diffusion-weighted imaging), tumors, multiple sclerosis lesions, aneurysms, hydrocephalus, and dementia-related atrophy. Often ordered with and without gadolinium contrast. Standard sequences include T1, T2, FLAIR, DWI, and post-contrast T1.
Cervical, thoracic, or lumbar. Shows disc herniations, nerve compression, spinal stenosis, cord lesions, infections, and post-surgical complications. Sagittal and axial T1 and T2 sequences are the workhorse views. Contrast added when tumor or infection is suspected.
Knee, shoulder, hip, ankle, wrist. Gold standard for ligament tears (ACL, PCL, rotator cuff), cartilage damage, labral injuries, stress fractures, and tendon ruptures. Proton density and fat-saturated sequences highlight different tissues. Arthrograms inject contrast directly into the joint for finer detail.
Liver, kidneys, pancreas, uterus, prostate, bowel. Often paired with MRCP for bile and pancreatic ducts, or multiparametric protocols for prostate cancer staging. Breath-hold sequences keep motion artifact low. Diffusion-weighted imaging helps spot tumors and abscesses.
Measures ejection fraction, valve function, scars from prior heart attack, congenital defects, and inflammation like myocarditis. Cine sequences show the heart beating in real time. Late gadolinium enhancement reveals fibrosis and infarct patterns.
Maps brain activity by tracking blood oxygen level changes (BOLD signal). Used to plan brain surgery near eloquent cortex, study language lateralization, and as the main imaging tool in cognitive neuroscience research.
What to Expect During an MRI Scan
The day starts with paperwork. A tech will hand you a metal-screening form that asks about pacemakers, aneurysm clips, cochlear implants, shrapnel, and any prior surgery involving metal. This is not boilerplate—ferromagnetic metal inside the scanner can heat, move, or in rare cases cause real injury. Be honest, even about the BB pellet from a 1998 birthday party.
You’ll change into a gown to make sure no metal hides in your clothes—underwire bras, zippers, decorative studs all stay in the locker. Jewelry, watches, hearing aids, removable dentures, and credit cards (the magnetic strip wipes) go in a basket. If you wear makeup, the tech may ask you to wipe it off; some mascaras and tattoo inks contain metallic pigments that can heat up.
Inside the room, you lie on a padded table that slides into the bore of the magnet. Depending on the body part, a surface coil—basically a specialized antenna—gets placed over you. You’ll be given earplugs or headphones, a panic-button bulb, and sometimes a mirror that lets you see out of the tunnel. The tech talks to you through an intercom from the next room.
Once the scan starts, the trick is to stay still. Even small movements blur the image, and a blurred sequence often has to be repeated, adding ten minutes you don’t want. Breathe normally for most exams. For abdominal MRI, you may be coached to hold your breath for 15–20 seconds at a time. The scanner will bang, buzz, click, and occasionally make a sound that resembles a small drum solo. That’s normal.
If contrast is ordered, an IV gets placed in your arm. Halfway through the scan, a small dose of gadolinium-based contrast goes in. Most patients feel nothing or a brief cool sensation. After the scan, you stand up, get your stuff, and walk out. There’s no recovery time, no driving restriction, no dose limit to worry about. Results usually go to the ordering doctor within a day or two.
MRI Prep by Scan Type
No fasting required for non-contrast studies. Take your regular medications with a small sip of water. Remove all metal jewelry, hairpins, and removable dental work. If you’re claustrophobic, ask your doctor about a mild oral sedative (often lorazepam) or an open or wide-bore MRI scanner. Arrive 15 minutes early to fill out the screening form.
MRI Safety: What Actually Matters
MRI is one of the safest imaging tests available. There’s no ionizing radiation, no cumulative dose, and no documented long-term effects from the magnetic field itself. The risks that exist are nearly all mechanical or device-related—and they’re almost entirely preventable with good screening.
The big four risks: projectiles, implant interactions, contrast reactions, and burns. Projectiles happen when ferrous metal gets too close to the magnet. Oxygen tanks, mop buckets, scissors, and stretchers have all been pulled into scanners—sometimes fatally. That’s why the room has zoned access and metal detectors at the door of every modern MRI suite.
Implants are trickier. Most modern pacemakers, cochlear implants, and spinal cord stimulators are now labeled “MR-conditional,” meaning they’re safe under specific conditions—a particular field strength, a defined region, sometimes a special programming step. Older implants may be “MR-unsafe.” Tattoos with iron-based pigments can warm slightly. Joint replacements, surgical clips, and IUDs are generally fine but should always be flagged.
Gadolinium contrast is well tolerated but not zero-risk. Patients with severely impaired kidney function (eGFR under 30) face a small risk of nephrogenic systemic fibrosis with older gadolinium agents. Newer macrocyclic agents have largely eliminated that concern, but renal function still gets checked before contrast. Allergic reactions exist but are far less common than with iodinated CT contrast.
Pregnancy is not an absolute contraindication. MRI without contrast is considered safe in any trimester when medically necessary. Gadolinium crosses the placenta, so contrast is usually avoided unless the benefit clearly outweighs the theoretical risk.
- A pacemaker, defibrillator, or implanted nerve stimulator
- An aneurysm clip or cochlear implant
- Any metal in your eye (welders and machinists, especially)
- Shrapnel, bullets, or BBs anywhere in your body
- Severe kidney disease (if contrast is planned)
- Pregnancy or possible pregnancy
- Severe claustrophobia—sedation can be arranged in advance
Contrast: When You Need It and When You Don’t
Roughly a third of MRI scans use gadolinium-based contrast. It’s injected through an IV, circulates through the bloodstream, and shortens the T1 relaxation time of nearby tissue—making vessels, inflammation, and many tumors light up brightly on T1-weighted sequences. Without contrast, those structures can hide in plain sight.
You’ll see contrast ordered routinely for brain tumor follow-up, multiple sclerosis surveillance, breast cancer screening in high-risk patients, vascular imaging, and characterizing liver lesions. You’ll often see it skipped for routine knee, shoulder, and lumbar spine scans where the anatomy speaks for itself.
Gadolinium is not the same as the iodinated contrast used in CT. People with shellfish allergies don’t automatically need to avoid it. Patients with mild kidney impairment are usually fine with newer agents. The dose is small—about 10–20 mL for an adult—and most of it clears through the kidneys within 24 hours.
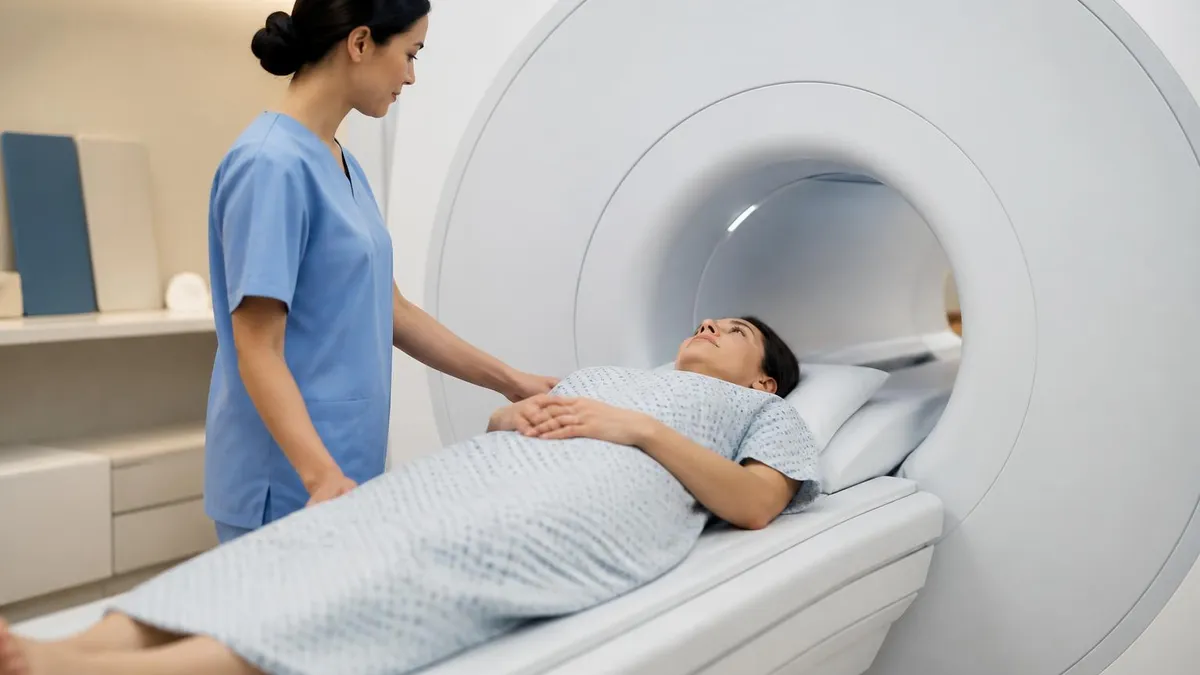
Before Your MRI Appointment
- ✓Fill out the metal-screening form completely and honestly
- ✓Bring a list of past surgeries, especially any involving metal implants
- ✓Bring your insurance card and prior imaging on disc if relevant
- ✓Leave jewelry, watches, and credit cards at home or in your locker
- ✓Skip makeup and hair products with metallic pigments
- ✓Ask about claustrophobia options (open MRI, mild sedation, headphones with music)
- ✓Follow fasting instructions if you got them
- ✓Arrange a ride home if you’ll be sedated
Closed vs. Open MRI—and What to Do About Claustrophobia
The traditional MRI is a tube. Long, narrow, and not particularly forgiving if small spaces make your chest tighten. Roughly one in twenty patients can’t complete a closed-bore scan because of claustrophobia, and another good chunk dread it but get through.
Open MRI was designed exactly for that crowd. The magnet has a C-shape or open sides, so most of the room is visible while you’re on the table. The trade-off is field strength—most open scanners run at 0.3T to 1.2T compared to 1.5T or 3T for closed bore, which means slightly lower resolution and sometimes longer scan times. For routine brain, spine, and joint imaging, the difference is rarely clinically meaningful. For specialized imaging like prostate MRI or cardiac MRI, a high-field closed bore is usually preferred.
A newer option is the wide-bore closed MRI, which keeps the 1.5T or 3T strength but uses a 70–75 cm bore instead of the older 60 cm. Most claustrophobic patients can tolerate a wide bore with no medication.
If you know you struggle, ask the scheduler. Options include music through headphones, a mirror that lets you see outside the tunnel, prism glasses, a weighted blanket, a low-dose oral benzodiazepine like lorazepam taken an hour before, or in severe cases, IV sedation with a nurse monitoring. There is no prize for white-knuckling it.
MRI: Strengths and Limitations
- +Zero ionizing radiation—safe for repeat use
- +Exceptional soft-tissue contrast (brain, spine, joints, organs)
- +Detects strokes, tumors, and MS lesions earlier than CT
- +Can image in any plane without moving the patient
- +Functional and diffusion sequences add unique clinical info
- −Long scan times (30–60 minutes typical)
- −Loud noise—hearing protection required
- −Claustrophobic environment for some patients
- −Expensive and less widely available than CT or X-ray
- −Contraindicated with certain metal implants
- −Less effective for bone fractures and acute lung imaging
Why “What Is MRI Scan” Matters for Tech and Patient Education Exams
If you’re studying for an MRI tech certification or a radiologic technologist board exam, the question “what is MRI scan” sounds insultingly simple—until it shows up disguised as something harder. Expect items like: which nucleus produces the MR signal in clinical imaging? (Hydrogen.) What does T1-weighting emphasize? (Fat appears bright, water appears dark.) Which sequence is most sensitive to acute stroke? (Diffusion-weighted imaging, DWI.)
Patient-facing roles get tested differently. Nursing and patient-education exams ask whether MRI uses radiation (it doesn’t), what to remove before the scan (all metal, including hidden items), and what to tell patients about gadolinium (small risk, mostly safe, contraindicated with severe renal failure). The depth varies, but the foundation is the same: a clear mental model of what the machine actually does.
The fastest way to lock in the basics is repetition with retrieval. Read a section, close the tab, and try to explain it out loud or write it down. Then take a short quiz to see what stuck and what slipped. The MRI practice test below was built for exactly that loop—quick recall on the high-yield concepts, with explanations that fill in the gaps.
MRI Questions and Answers
The Bottom Line on What an MRI Scan Is
Strip away the jargon and an MRI is a clever trick of physics. A magnet lines up the hydrogen in your body. Radio waves nudge it. A computer listens to the echo and draws a picture. No radiation, no cutting, no recovery time—just a loud half-hour that can tell your doctor more about your soft tissues than almost any other test on earth.
If you’re heading in for one, the prep is mostly common sense: be honest on the screening form, leave metal at home, plan for the noise, and ask about claustrophobia options if you need them. If you’re studying the topic for an exam, lean on the mental model—magnet, radio waves, hydrogen, signal—and let the quiz fill in the rest.
The same loop that helped countless techs pass their boards works for patients too: read, recall, test. Use the practice quiz to find the gaps, then come back here for the explanation. By the third pass, “what is MRI scan” stops being a question and starts being something you can explain to the next person who asks.
A Quick History So It Sticks
It helps to know that MRI grew out of nuclear magnetic resonance, a chemistry-lab technique from the 1940s. Felix Bloch and Edward Purcell shared the 1952 Nobel Prize for showing that atomic nuclei could be made to resonate in a magnetic field. For decades, it stayed in chemistry departments, used to figure out the structure of molecules. Then in the early 1970s, Paul Lauterbur figured out how to add gradients to encode spatial information, and Peter Mansfield worked out fast imaging math.
By the late 1970s the first human images appeared—grainy, slow, but unmistakably real anatomy. Today’s 3-Tesla scanner is the descendant of those early experiments, and the underlying physics has not changed. Only the magnets got bigger, the gradients got faster, and the computers got smart enough to reconstruct images in real time.
What an MRI Actually Costs in the U.S.
Prices vary wildly. A standard MRI of the brain or knee can run anywhere from $400 at a freestanding outpatient center to $3,500 at a major hospital, before insurance. With insurance, your out-of-pocket cost depends on your deductible, copay, and whether the facility is in-network. The advice most patients hear and ignore: call ahead, ask for the cash price, and compare two or three facilities.
Imaging is one of the few areas of medicine where shopping around can save thousands of dollars on the exact same scan. Most facilities will quote a self-pay price over the phone, and some discount it by 30 to 50 percent if you pay up front. A radiologist’s read of the images is usually a separate small fee, often bundled in but worth asking about.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.