What Is MRI: Magnetic Resonance Imaging Explained
What is MRI? Comprehensive explanation of magnetic resonance imaging — how it works, what it shows, common uses, safety, and patient experience.
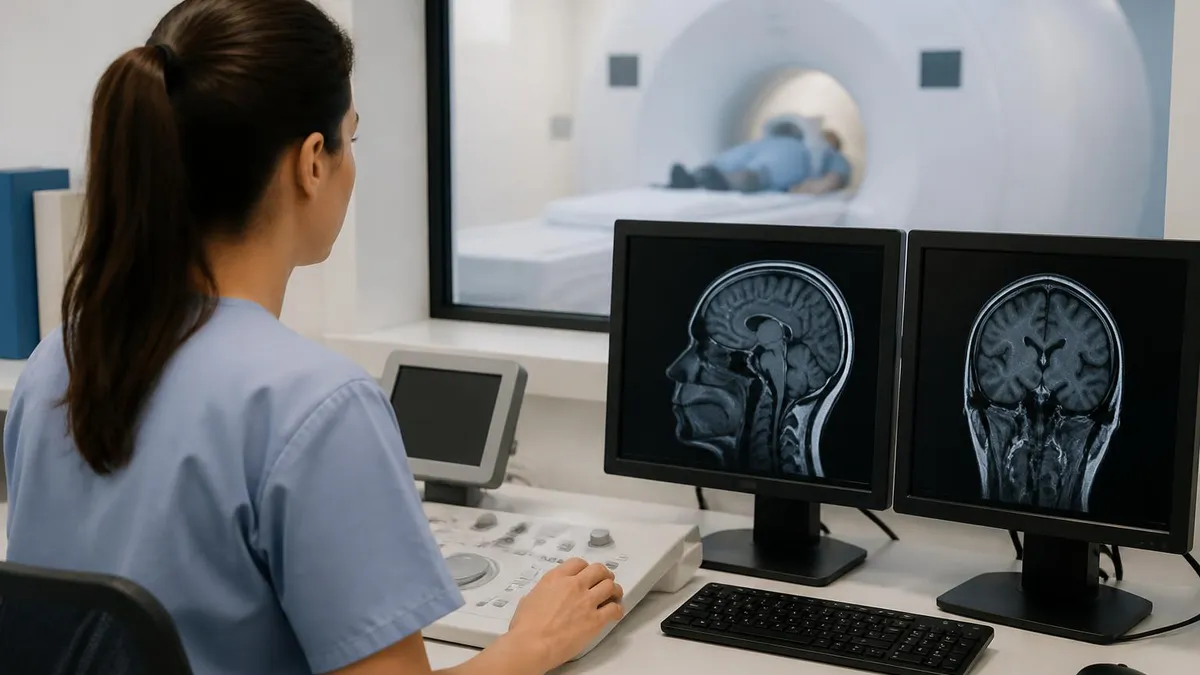
MRI stands for Magnetic Resonance Imaging — a medical imaging technique using powerful magnetic fields and radio waves to create detailed images of structures inside the body. Unlike X-rays and CT scans which use ionizing radiation, MRI uses no radiation, instead exploiting the magnetic properties of hydrogen atoms (abundant in body water and fat) to generate images.
The technology developed through scientific work spanning decades earned multiple Nobel Prizes recognizing its fundamental importance to physics and medicine. Modern MRI represents one of the most important diagnostic tools in healthcare, providing information about soft tissue, organs, and various structures that other imaging methods cannot match.
The basic operation involves placing the patient inside a powerful superconducting magnet (typically 1.5 Tesla or 3 Tesla in clinical use). The magnet aligns the protons in body water molecules. Radio frequency pulses then disturb this alignment, and as protons relax back to original position, they emit radio signals that the scanner detects and processes into images. Different tissue types relax at different rates, creating contrast between gray matter, white matter, cerebrospinal fluid, blood, fat, muscle, and various pathological tissues. Specialized sequences highlight specific features — diffusion-weighted imaging shows acute strokes, FLAIR sequences highlight white matter abnormalities, and many others.
What Is MRI Quick Facts
Full name: Magnetic Resonance Imaging. Technology: Powerful magnets plus radio frequency pulses; no ionizing radiation. Uses: Brain, spine, joints, organs, vascular evaluation. Strengths: Soft tissue detail superior to CT; detects acute stroke quickly; multiple sequences provide different information. Limitations: Long scan times (30-60 min), loud noise, confined space (claustrophobia), metal implant restrictions. Cost: $400-$3,500 typical without insurance.
What MRI shows differs substantially from other imaging modalities. MRI provides exceptional soft tissue detail — distinguishing different brain tissues, identifying inflammation, characterizing tumors, evaluating ligament and cartilage damage, assessing organ structure. Bone shows less detail on MRI than on CT or X-ray (bone has minimal water content), but bone marrow and surrounding soft tissue show extensively. The combination makes MRI superior to other modalities for many clinical questions including most brain pathology, spine conditions, joint injuries, and various soft tissue concerns. Different MRI sequences (T1, T2, FLAIR, DWI, etc.) highlight different tissue characteristics providing comprehensive information from single examination.
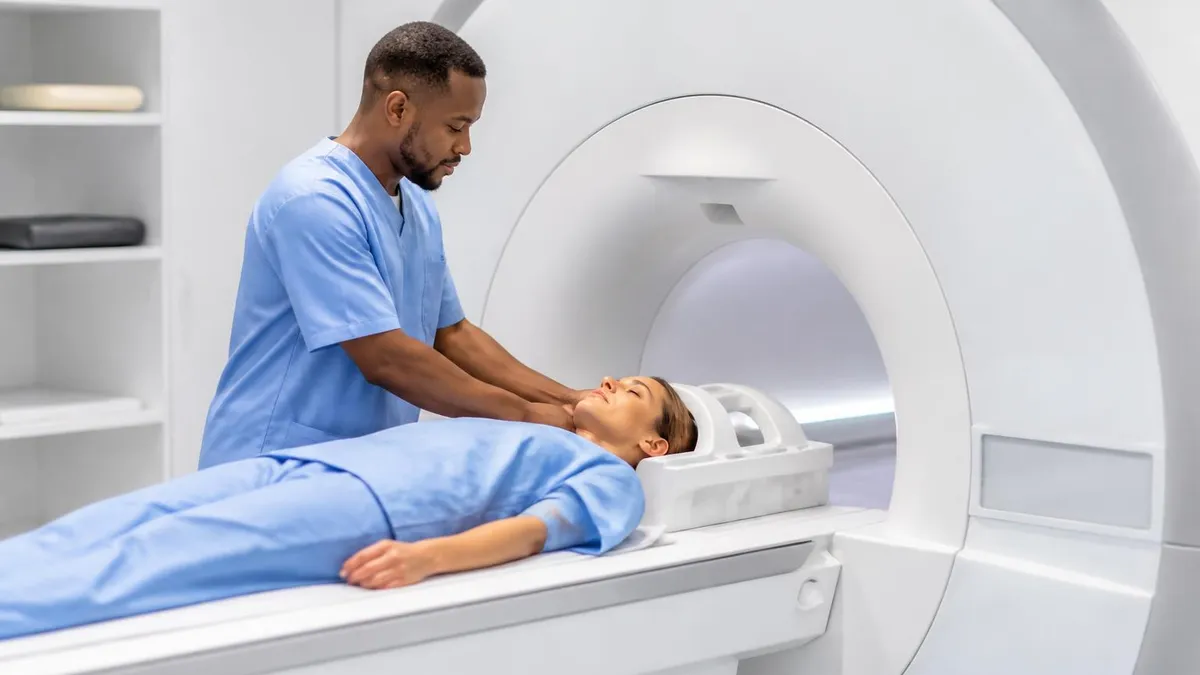
Common MRI Applications
Tumors, stroke, multiple sclerosis, dementia evaluation, infections, hemorrhage, congenital abnormalities.
Disc herniation, spinal stenosis, tumors, infections, traumatic injuries, degenerative changes.
Knee, shoulder, hip, ankle, wrist evaluation. Ligament tears, cartilage damage, fractures.
Heart muscle evaluation, congenital heart disease, cardiomyopathy, scar tissue identification.
Liver, kidney, pancreas, adrenal glands. Tumor characterization and various organ evaluations.
Prostate (men), uterus and ovaries (women), bladder, rectum evaluation for various conditions.
The history of MRI development reflects fundamental physics research applied to medicine. Nuclear magnetic resonance phenomenon discovered in 1938 by Isidor Rabi (Nobel Prize 1944). Felix Bloch and Edward Purcell developed practical NMR techniques in 1946 (Nobel Prize 1952). Paul Lauterbur and Peter Mansfield pioneered MRI imaging in 1970s-80s (Nobel Prize 2003). Raymond Damadian developed first commercial MRI scanner.
Each contribution built toward modern clinical MRI now used in millions of examinations annually worldwide. The progression from basic physics to clinical application took decades but produced one of the most important diagnostic tools in modern medicine providing information unavailable through any other modality.
How MRI differs from other imaging deserves clarification. X-ray uses ionizing radiation showing primarily bone and dense structures with limited soft tissue detail. CT scan uses ionizing radiation showing better detail than X-ray with both bone and soft tissue but less soft tissue detail than MRI. Ultrasound uses sound waves providing real-time imaging without radiation but limited tissue penetration and image quality affected by various factors.
MRI uses no ionizing radiation providing exceptional soft tissue detail but with longer scan times and various restrictions. Each modality has strengths and weaknesses — physicians select appropriate modality based on clinical question, patient factors, and various other considerations. MRI excels for many soft tissue questions but isn't always best choice depending on situation.
Clinical applications of MRI span virtually every body system. Neurology uses MRI extensively for brain and spine evaluation. Orthopedics uses MRI for joint, ligament, and soft tissue evaluation. Oncology uses MRI for tumor characterization and treatment monitoring. Cardiology uses MRI for cardiac structure and function evaluation. Gastroenterology uses MRI for various abdominal organ evaluation. Urology uses MRI for prostate and other genitourinary evaluation. Gynecology uses MRI for pelvic organ evaluation. Each specialty has specific MRI applications serving their clinical questions. The breadth of applications reflects MRI's fundamental capability for soft tissue evaluation across most medical specialties.
MRI basic operation: Patient placed inside powerful superconducting magnet (1.5T or 3T typical clinical). Magnet aligns protons in body water molecules. Radio frequency pulses disturb alignment. As protons relax back, they emit radio signals scanner detects. Different tissues relax at different rates creating contrast in images. Various pulse sequences (T1, T2, FLAIR, DWI, etc.) highlight different tissue characteristics. Computer processes signals into cross-sectional images. Total examination typically 30-60 minutes with various sequences capturing different information.
Patient preparation for MRI is generally minimal but specific items matter. Disclose all metal implants and devices that might be affected by magnetic field. Pacemakers and most cardiac defibrillators historically prevented MRI but newer MRI-conditional devices allow scanning under specific conditions. Cochlear implants prevent MRI in most cases. Aneurysm clips, certain orthopedic hardware, retained metal fragments (particularly in eyes), and other implants need verification of MRI compatibility. Bring records of any implants — manufacturer documentation typically includes MRI safety information. Some examinations require fasting or other preparation depending on body part being imaged.
The scanner experience is loud — much louder than most patients expect. The various MRI sequences produce knocking, banging, beeping, and whirring sounds at volumes that can exceed 100 decibels. Standard practice provides earplugs and over-ear headphones for hearing protection and to play music or audiobooks during scanning. Modern scanners are progressively quieter through engineering improvements, but they remain significantly louder than typical medical procedures. The noise serves a purpose — it's caused by gradient coils rapidly switching the magnetic field to enable spatial encoding of signals. Without these gradient pulses, images couldn't be created.
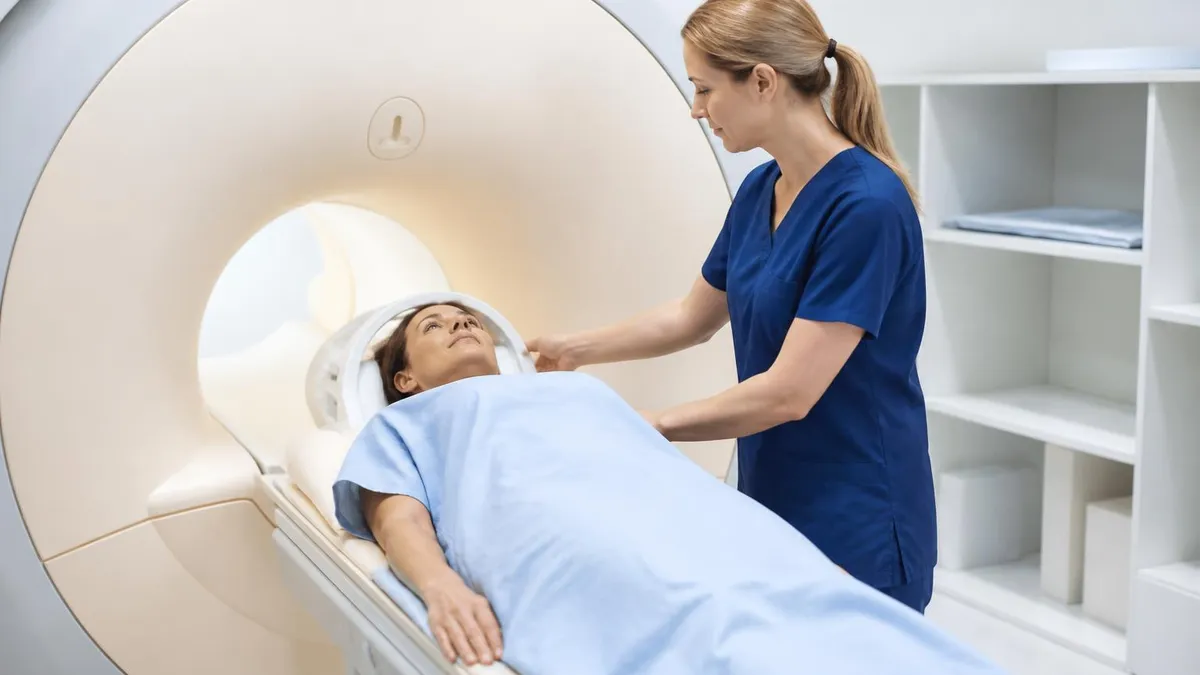
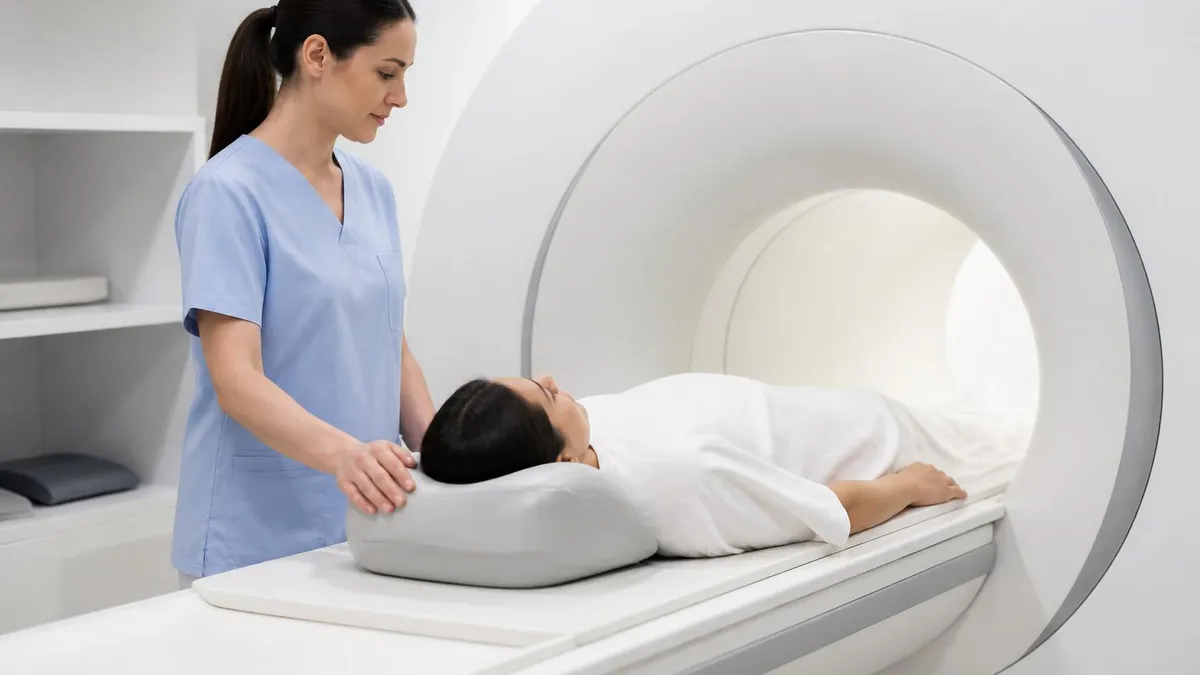
Stillness during scanning matters because patient motion blurs images. Even small movements create motion artifacts that obscure findings or require sequences to be repeated. Different body parts have different positioning requirements — head positioned in specialized coil receiver for brain MRI; specific positioning for joints, spine, abdomen. Patients are instructed to remain still and breathe normally — actual breathing motion at the chest doesn't significantly affect head or extremity images. Some examinations require breath-holding for short periods (cardiac, abdominal) supporting specific image quality. Closing your eyes can help reduce the impulse to move during long scans.
Always disclose metal implants: pacemakers, defibrillators, cochlear implants, aneurysm clips, surgical implants, retained metal fragments (especially eyes), tattoos with metallic ink. Some prevent MRI entirely. Pregnancy: MRI generally avoided in first trimester unless absolutely necessary. Gadolinium contrast specifically avoided during pregnancy. Severe kidney disease: Restricts gadolinium use due to nephrogenic systemic fibrosis risk. Claustrophobia: Discuss with ordering physician for accommodations including anti-anxiety medication or open MRI alternatives.
Closed (tunnel) MRI scanners produce best image quality through high field strength (1.5T or 3T) and tight coil designs. The tunnel is approximately 24 inches in diameter and patients lie within it for 30-60 minutes. Open MRI scanners are more comfortable for claustrophobic patients but typically lower field strength (0.3T-0.7T) producing lower-quality images. Wide-bore scanners (70cm vs traditional 60cm) provide more comfortable closed MRI option without sacrificing image quality. For most clinical questions where image quality matters substantially for diagnosis, closed scanners are preferred. Sedation and anti-anxiety medication can help claustrophobic patients tolerate closed scanners.
What to wear for MRI matters because metal in clothing can affect image quality. Most facilities provide gowns; if you wear your own clothes, choose items without metal zippers, snaps, hooks, or printed designs that might contain metallic ink. Remove all jewelry, watches, hair accessories, hearing aids, and dental retainers (unless permanently affixed). Makeup containing metallic particles (some mascara, eye shadow) should be removed since it can affect image quality. Bring case for eyeglasses or contacts since vision aids must be removed. Quality preparation supports best examination experience and image quality.
Result interpretation typically takes 1-3 business days for routine MRI. The radiologist generates a report describing findings sequence by sequence, with overall impression and recommendations. Report goes to ordering physician who shares results with you, often during follow-up appointment. For urgent findings (suspected stroke, large tumor, acute hemorrhage), the radiologist will call the ordering physician immediately rather than waiting for written report. Some facilities offer patient portals for direct access to imaging reports — discuss with your physician how you'll receive results.
Before Your MRI
- ✓Disclose all metal implants, devices, and surgical history
- ✓Disclose pregnancy status if applicable
- ✓Inform facility of claustrophobia concerns to plan accommodations
- ✓Disclose kidney disease history (affects contrast use)
- ✓Remove all jewelry, watches, hair clips before scan
- ✓Bring list of medications and allergies
- ✓Arrange driver if anti-anxiety medication will be used
- ✓Plan for 30-60 minute scan in confined space
Understanding your MRI report requires medical knowledge beyond what most non-physicians have. Reports use specific medical terminology and reference specific anatomical structures. Common findings have specific implications that require clinical context to interpret. Discuss the report with the ordering physician rather than trying to interpret independently. The physician will explain what was found, what it means in your specific context, and what next steps (additional testing, treatment, monitoring) follow. If you don't understand something in the explanation, ask questions until you do — informed decisions require understanding what's happening.
Incidental findings on MRI are common — small abnormalities discovered while looking for something else. These might include small white matter changes that may be age-related or related to vascular risk factors, small benign cysts, mild atrophy, or minor anatomical variants without clinical significance. Some incidental findings warrant follow-up (small aneurysms, ambiguous lesions); others are clearly benign and need no action. Your physician interprets findings in context of your symptoms, age, and overall health. Don't panic about incidental findings before discussing with the ordering physician — many require no action at all.
For radiology technologists and students considering MRI as a career specialty, MRI represents one of the most demanding and rewarding subspecialties. Patient interaction is substantial including communication about claustrophobia, explaining procedures, helping with positioning. Technical knowledge of various sequences and protocols requires substantial training. ARRT (American Registry of Radiologic Technologists) certification in MRI requires specific clinical hours and examination passing. Salaries for experienced MRI technologists in major medical centers typically run $75,000-$120,000+ depending on location and experience. Career-long learning supports staying current as technology evolves.
New MRI technologists typically begin with general radiography certification before pursuing MRI subspecialty certification through additional clinical training and examination. Many MRI technologists work rotating shifts including evenings and weekends since MRI services frequently operate extended hours to maximize equipment utilization. Hospital-based positions typically offer more comprehensive benefits while imaging center positions sometimes offer higher hourly rates and more predictable schedules. Senior MRI technologists often advance into supervisory positions, lead technologist roles, or applications specialist positions with equipment manufacturers. Educational pathways include formal academic programs, hospital-based clinical training, and online didactic coursework combined with supervised clinical hours.
Cost considerations for MRI vary dramatically by region, facility type, and insurance coverage. Hospital-based MRI typically costs more than outpatient imaging center MRI for the same study. Insurance coverage usually applies when MRI is medically indicated by physician order. Without insurance, costs range from $400-$3,500 with substantial regional variation. Cash-pay rates at outpatient imaging centers are often dramatically lower than the rates billed to insurance. Some patients without insurance specifically seek cash-pay rates that can be 50-80% less than insurance-billed rates. Health savings account (HSA) and flexible spending account (FSA) funds can be used for MRI expenses.
The technology landscape continues evolving. 3 Tesla scanners produce sharper images than 1.5 Tesla scanners and are increasingly common but cost more and have different safety considerations for some implants. 7 Tesla scanners are starting to appear in research and select clinical applications, providing extraordinary detail particularly for high-resolution brain imaging. Functional MRI (fMRI) maps brain activity by detecting blood oxygenation changes. Diffusion tensor imaging (DTI) maps white matter tracts. MR spectroscopy analyzes chemical composition of tissue. These advanced techniques are increasingly part of standard clinical MRI for specific indications.
Artificial intelligence is increasingly involved in MRI interpretation. AI algorithms can detect specific abnormalities (some tumors, hemorrhages, large vessel occlusions) with sensitivity comparable to or exceeding human radiologists for those specific tasks. Current clinical use typically involves AI as second-reader assistance — flagging potential findings for human radiologist review rather than replacing the radiologist. The technology continues to advance rapidly, and AI's role in MRI interpretation will likely grow substantially over the coming decade. The fundamental clinical relationship between you, your physician, and your imaging will continue but with increasingly sophisticated tools assisting interpretation.
Image reconstruction algorithms using AI can produce diagnostic-quality images from substantially shorter scan acquisitions, reducing scan times for many protocols. Automated quality checks during scanning help technologists identify motion artifacts or positioning issues before scan completion. Pre-scan workflow tools can help patient screening for contraindications. Clinical decision support tools can help radiologists ensure consistent reporting and reduce missed findings. These innovations collectively support faster scanning, better images, and more reliable interpretations across diverse clinical settings.
MRI Quick Stats
MRI vs Other Imaging Modalities
X-ray fast and cheap with bone detail; MRI provides far superior soft tissue detail without radiation.
CT faster and better for bone trauma and acute hemorrhage; MRI superior for soft tissue and uses no radiation.
Ultrasound real-time and no radiation; MRI provides better detail and not limited by air or bone interference.
PET shows metabolic activity; MRI shows anatomical detail. Often combined as PET/MRI for comprehensive evaluation.
Mammography screens breast cancer; MRI for high-risk screening or further evaluation of abnormalities.
Endoscopy direct visualization with biopsy capability; MRI noninvasive imaging without biopsy capability.
For specific medical specialties, MRI plays substantial role. Neurology relies on MRI for nearly all brain and spine conditions including stroke, multiple sclerosis, dementia, epilepsy, headache evaluation, infections, tumors, traumatic injuries. Without MRI, modern neurological diagnosis would be substantially limited. Orthopedics uses MRI extensively for joint injuries (knee, shoulder, hip, ankle), spine conditions, soft tissue injuries, sports injuries. Oncology uses MRI for tumor evaluation, staging, treatment monitoring, recurrence detection. Each specialty has specific MRI applications matching their clinical questions and patient populations served.
For people experiencing health concerns considering whether MRI might be appropriate, several considerations apply. Talk to primary care physician or relevant specialist about whether MRI is appropriate for your specific situation. Understanding what MRI can and cannot determine — MRI shows specific findings but doesn't always definitively diagnose conditions (sometimes additional testing or biopsy required). Considering specific clinical question being addressed. Understanding subsequent decision pathway based on different possible findings. Discussion with physician about whether MRI is most appropriate next diagnostic step versus alternatives supports informed decisions about pursuing imaging.
For technologists considering MRI as career specialty, several characteristics support success. Technical aptitude managing complex equipment and various imaging protocols. Patient interaction skills supporting diverse populations including anxious or claustrophobic patients. Attention to detail ensuring quality images meeting diagnostic needs. Physical capability for substantial standing and patient positioning. Continuous learning supporting ongoing technology evolution. The combination of technical and interpersonal skills required makes MRI technology demanding career but with rewarding work supporting essential medical diagnosis. Career-long technologists develop substantial expertise across various MRI applications throughout their careers.
The intellectual challenge of constantly learning new sequences, new applications, and new clinical contexts keeps the work interesting throughout a career. Senior technologists often mentor newer staff, develop institutional protocols, and participate in research collaborations with radiologists and clinicians. Some technologists pursue advanced credentials in cardiac MRI, breast MRI, or neuroimaging that allow specialization within the broader field. Continuing education through professional society meetings, vendor training sessions, and online courses keeps practitioners current with rapidly advancing technology. The combination of patient care, technical expertise, and continuous learning makes MRI technology a rewarding long-term career path.
MRI: Pros and Cons
- +No ionizing radiation — safe for repeated imaging
- +Superior soft tissue detail vs CT or X-ray
- +Multiple sequences provide different information
- +Detects acute stroke within minutes of onset
- +Comprehensive tumor characterization
- +Functional and advanced techniques available
- −Higher cost than CT in most regions
- −Longer scan time (30-60 min vs CT minutes)
- −Loud scanner noise can be uncomfortable
- −Confined tunnel triggers claustrophobia in many patients
- −Some implants prevent MRI use
- −Gadolinium contrast restricted in kidney disease
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.