What Is an MRI? How Magnetic Resonance Imaging Works
Learn what an MRI is, how magnetic resonance imaging works, types of MRI scans, what to expect during the procedure, costs, and how it differs from CT.
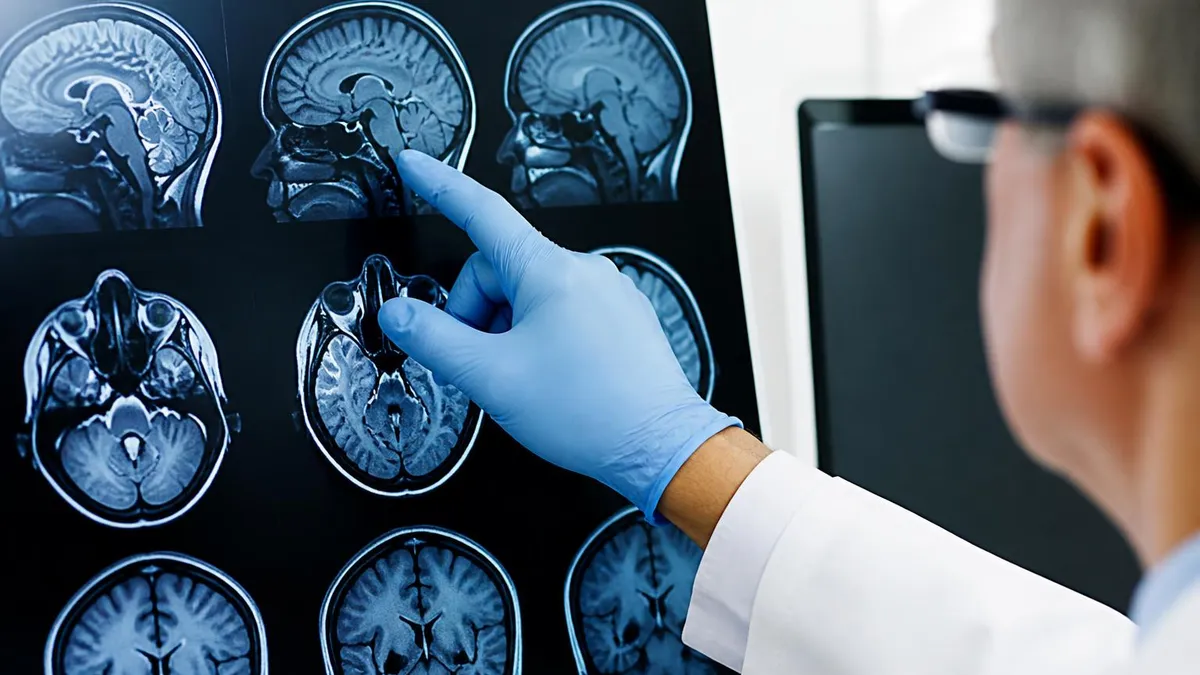
MRI at a Glance
An MRI — short for Magnetic Resonance Imaging — is a medical imaging technique that uses powerful magnetic fields and radio waves to create detailed images of the inside of the body. Unlike X-rays or CT scans, MRI produces no ionizing radiation. Instead, the MRI machine temporarily aligns the hydrogen atoms in your body using a strong magnetic field, then uses radio waves to knock those atoms out of alignment. As they snap back into place, they emit signals that a computer converts into cross-sectional images of tissues and organs with exceptional soft-tissue detail.
The result is an MRI scan that can distinguish between different types of tissue — muscle, fat, cartilage, ligaments, and organs — with a level of clarity that X-rays and CT scans cannot match for soft tissue. This makes MRI the preferred imaging tool for conditions affecting the brain and spinal cord, joints, abdominal organs, the heart, and the breast. Radiologists read MRI images as thin-slice cross-sections viewed from multiple angles — axial (top to bottom), sagittal (front to back), and coronal (side to side) — giving them a three-dimensional picture without ever making an incision.
The core physics of MRI involves the behavior of hydrogen protons in a magnetic field. The human body is approximately 60% water, and water molecules contain hydrogen atoms. When you enter the MRI bore (the circular tunnel of the machine), the machine's magnet — running at 1.5 to 3 Tesla, roughly 30,000 to 60,000 times Earth's natural magnetic field — aligns those protons in a uniform direction. A radiofrequency pulse then temporarily disturbs this alignment.
When the pulse stops, the protons return to their aligned state and release the absorbed energy as a radio signal. Different tissues release this energy at different rates (called T1 and T2 relaxation times), and the MRI system translates those differences into image contrast. Bone, which contains little water, appears dark on MRI. Fat, with abundant hydrogen, appears bright. Fluid-filled structures like cysts appear distinctly different from solid tissue — which is exactly what makes MRI so useful for detecting pathology.
The strength of the magnet matters for image quality. Most hospitals and outpatient imaging centers use 1.5T scanners for routine imaging. 3T scanners provide higher resolution and are preferred for detailed brain imaging, small joint studies, and functional MRI (fMRI) research. Some specialized research and academic medical centers have 7T magnets, which provide extraordinary resolution but are not in routine clinical use. Higher field strength generally produces sharper images and faster scans, though it also increases susceptibility to certain artifacts and has more restrictions on implanted devices.
The MRI machine's powerful magnetic field can cause certain metal implants to move, heat up, or malfunction. Before any MRI, you must disclose all metal in your body — including pacemakers, cochlear implants, certain aneurysm clips, joint replacements, surgical staples, shrapnel, and body piercings. Most modern joint replacements and many cardiac devices are MRI-conditional (safe in specific MRI environments), but some older devices are not. Never assume a previous surgery makes you MRI-safe — always tell the technologist and radiologist about any implants, prior surgeries, or foreign bodies before entering the MRI room.
MRI is used across virtually every medical specialty because of its ability to image soft tissues with detail that other modalities can't match. In neurology and neurosurgery, brain MRI is the primary tool for evaluating stroke, multiple sclerosis lesions, tumors, brain hemorrhage, dementia, epilepsy, and traumatic brain injury.
A brain MRI with contrast (using gadolinium dye injected intravenously) enhances the visibility of areas with disrupted blood-brain barriers — the hallmark of active inflammation, tumors, and abscesses. Functional MRI (fMRI), a specialized protocol, maps brain activity by detecting blood flow changes during tasks, used in surgical planning to identify regions to avoid during brain tumor resection.
In musculoskeletal medicine, MRI is the gold standard for evaluating ligament and tendon tears, meniscal injuries, cartilage damage, stress fractures, and bone marrow abnormalities that don't appear on X-ray. Orthopedic surgeons rely on MRI images to decide whether a knee injury requires surgery, whether a spine shows disc herniation or stenosis causing nerve compression, and whether a shoulder has a full-thickness rotator cuff tear. The knee, shoulder, hip, wrist, and spine are among the most commonly MRI-scanned body parts in outpatient orthopedics.
Abdominal and pelvic MRI provides detailed evaluation of the liver, pancreas, kidneys, adrenal glands, uterus, ovaries, and prostate. MRI of the liver is particularly valuable for characterizing liver lesions seen on ultrasound or CT — differentiating benign hemangiomas from metastatic disease or hepatocellular carcinoma.
Breast MRI is used for high-risk screening in women with BRCA gene mutations, surgical planning after breast cancer diagnosis, and evaluation of unexplained nipple discharge. Cardiac MRI assesses heart structure, function, and viability after heart attack — providing information about scar tissue and remaining healthy muscle that guides decisions about stent placement, bypass surgery, or device implantation.
MRI vs. CT vs. X-Ray: How They Compare
- Technology: Magnetic fields and radio waves — no radiation
- Best for: Soft tissue (brain, spinal cord, joints, ligaments, abdominal organs, breast)
- Limitations: Expensive, slow (15–90 min), loud, cannot image patients with certain implants, claustrophobia risk
- Contrast agent: Gadolinium (lower risk than CT contrast for most patients, but avoided in severe kidney disease)
- Radiation dose: Zero
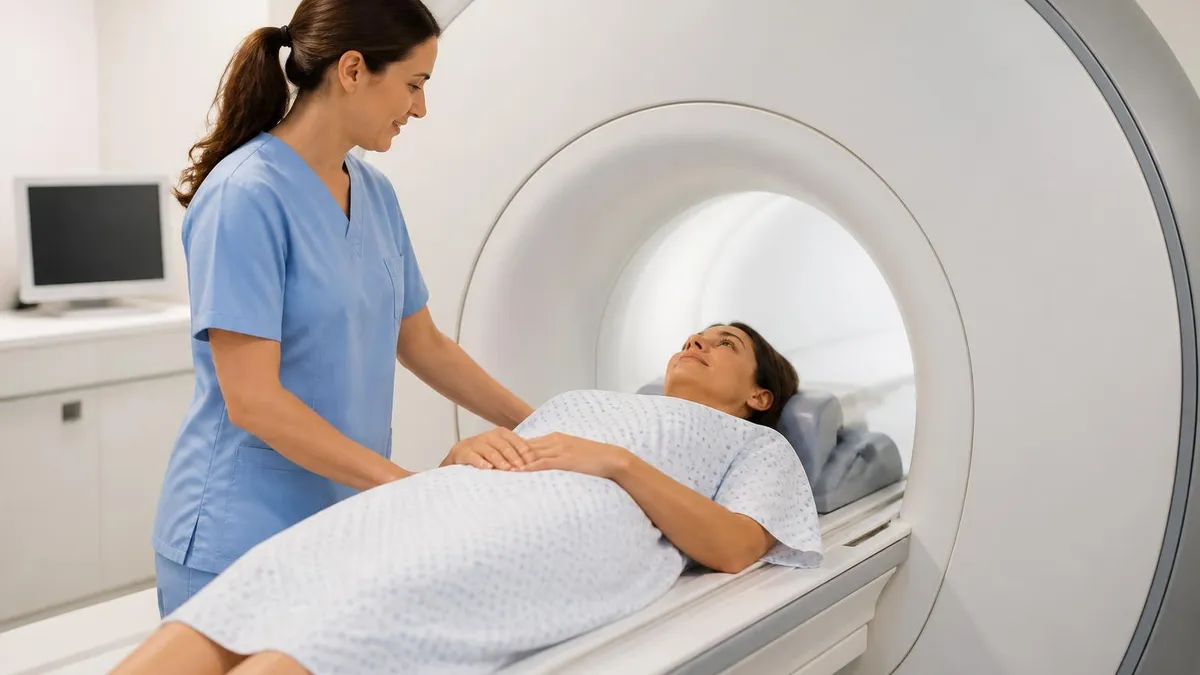
The experience of getting an MRI varies depending on what's being scanned, but the basic setup is consistent. You'll lie on a motorized table that slides into the machine's bore — a hollow cylinder surrounded by the magnet. For most body scans you enter feet first; for brain and neck scans you typically go in head first, with your head inside the bore.
The technologist positions positioning coils (specialized antenna arrays that improve image quality) around the body part being scanned, gives you earplugs or headphones to reduce the loud banging and knocking sounds the machine makes during imaging, and then leaves the room to operate the equipment from a nearby control area through a window.
The sounds are genuinely loud — some sequences produce 95 to 115 dB of banging and clanking as the machine's gradient coils rapidly switch on and off to encode spatial information. Earplugs are essential, and most centers offer to play music through headphones during the scan.
You must stay as still as possible throughout, especially for brain and spine scans where movement blurs the images. Scans typically last 15 to 90 minutes depending on the body part and how many sequences the radiologist has ordered. Understanding how long does an MRI take for specific body parts helps you plan your schedule around the appointment.
Claustrophobia is a real concern for approximately 1 in 10 patients in traditional closed-bore scanners. The bore opening is typically 60 to 70 centimeters wide. If you're anxious about enclosed spaces, tell your doctor before your appointment — mild sedation is often available for anxious patients, and open MRI machines eliminate the enclosed bore entirely.
Open MRI uses a different magnet configuration with open sides, which dramatically reduces claustrophobic symptoms. The trade-off is lower magnetic field strength (typically 0.7T to 1.0T), which means lower image resolution — acceptable for many routine studies but not ideal for complex neurological or small joint imaging where 1.5T or 3T quality is important.

MRI Contraindications and Precautions
- Pacemakers and ICDs: Most older devices are MRI-incompatible — newer MRI-conditional devices may be safe in specific settings
- Cochlear implants: Most are MRI-incompatible unless specifically MRI-conditional
- Ferromagnetic aneurysm clips: Can shift under magnetic force — titanium clips are generally safe
- Metal shrapnel near eyes: Orbital metal requires X-ray clearance before MRI in patients with history of metalworking or combat injury
- Certain spinal cord stimulators: Variable — check device specifics with manufacturer
- Pregnancy (first trimester): MRI generally avoided in first trimester unless urgently indicated; gadolinium contrast avoided throughout pregnancy
Preparing for an MRI is straightforward for most patients. You'll be asked to remove all metal objects — jewellery, hairpins, hearing aids, watches, underwire bras, and any removable piercings. You'll change into a hospital gown. Leave valuables at home if possible — storage lockers are provided but the MRI environment is inherently incompatible with most electronic devices and metallic personal items. Most MRI scans don't require fasting, though some abdominal and pelvic studies request nothing by mouth for several hours before the scan. Your ordering physician or the imaging centre will provide preparation instructions specific to your study.
If your scan requires contrast, a gadolinium-based contrast agent (GBCA) is injected intravenously through an IV line placed in your arm. Gadolinium enhances the visibility of blood vessels and areas with disrupted tissue barriers — essential for detecting active inflammation, tumors, and vascular abnormalities.
Gadolinium is generally well-tolerated, with a very low rate of allergic reactions (far lower than iodinated CT contrast). However, it's avoided in patients with severe kidney disease due to the rare but serious risk of nephrogenic systemic fibrosis (NSF). Your kidney function (creatinine or eGFR) may be checked before contrast is administered if there's any concern about renal function.
Doctors order MRIs when they need imaging that goes beyond what X-ray or CT can provide. The most common clinical scenarios that prompt an MRI order: neurological symptoms (new headache, vision changes, weakness, numbness, suspected stroke), back or neck pain with nerve symptoms (radiculopathy, myelopathy), sports injuries to joints and soft tissues, evaluation of a mass or lesion seen on another imaging study, monitoring of a known condition like multiple sclerosis or a brain tumor, cancer staging and treatment response assessment, and cardiovascular assessment when echocardiography is insufficient.
MRI's lack of radiation makes it particularly appropriate for pediatric patients and for conditions requiring repeated imaging over time.
Functional MRI (fMRI) is worth a separate mention because it represents a fundamentally different use of MRI technology. Standard anatomical MRI shows static structure. fMRI shows dynamic function — it detects the tiny changes in blood oxygen level that occur when specific brain regions become active during a task.
Neurosurgeons use fMRI to map language, motor, and visual cortex before tumor resection, so they can plan a surgical approach that removes as much tumor as possible while preserving critical function. Researchers use fMRI to study cognition, emotion, addiction, and psychiatric disorders. Diffusion tensor imaging (DTI), another advanced MRI technique, maps the white matter tracts connecting brain regions and helps surgeons identify pathways that shouldn't be disrupted during surgery.
The choice between MRI and CT comes down to what needs to be imaged and how quickly. In emergencies — suspected stroke, aortic dissection, pulmonary embolism, traumatic injury — CT is faster and available 24/7 at most hospitals. MRI takes longer to set up and run, and some patients can't tolerate it. For non-emergency soft tissue evaluation — brain lesions, spinal pathology, joint injuries, abdominal organ characterization — MRI generally provides superior information and avoids radiation. When in doubt about why one was ordered over the other, your radiologist or ordering physician can explain the clinical reasoning.
MRI vs. CT: Advantages and Trade-Offs
- +MRI: No ionizing radiation — important for children, pregnant patients, and conditions requiring repeated imaging
- +MRI: Superior soft-tissue contrast — distinguishes tissue types that CT cannot differentiate
- +MRI: Multiplanar capability — images in any plane without moving the patient
- +CT: Faster scan time — critical in emergencies when waiting 45–90 minutes for MRI isn't an option
- +CT: More widely available — every hospital has CT; not all have MRI or 24/7 MRI access
- −MRI: Expensive — typically $400–$3,500 depending on body part, facility, and contrast use
- −MRI: Incompatible with many implanted devices — limits who can safely be scanned
- −MRI: Claustrophobia risk — 10% of patients struggle with closed-bore machines
- −CT: Significant radiation dose — cumulative exposure is a real concern for patients who need frequent scans
- −CT: Less useful for soft tissue — misses many findings that MRI would detect, particularly in brain and spinal cord
MRI costs vary significantly depending on the body part scanned, whether contrast is used, the type of facility (hospital vs. outpatient imaging center), your geographic location, and your insurance coverage. In the United States, a brain MRI without contrast at an outpatient imaging center might cost $400 to $700 with a cash-pay discount; the same study at a hospital outpatient department can run $1,500 to $3,500 before insurance adjustments.
Contrast adds cost — both for the gadolinium agent itself and for the radiologist's interpretation of the additional sequences. Most commercial insurance plans cover medically necessary MRI with a valid physician order, though prior authorization is required by many plans — meaning your doctor's office must obtain approval before you can schedule.
If you're uninsured or underinsured, outpatient imaging centers and free-standing radiology facilities typically offer substantially lower cash-pay rates than hospital-affiliated imaging. Some major outpatient chains publish transparent pricing; others will provide quotes by phone. Medicare and Medicaid cover MRI when medically necessary, though reimbursement rates differ from commercial insurance. For patients who receive a bill that seems unexpectedly high, itemizing the charges and negotiating with the billing department — or requesting a financial assistance review if the facility is nonprofit — often results in a reduced balance. Never assume the first bill is the final amount.
International differences in MRI costs are stark and worth noting for anyone who has received a large bill. In Canada, the UK, and most of Western Europe, MRI is provided through the public health system at little or no direct cost to the patient — though wait times for non-urgent studies can be weeks to months.
In the US, the combination of facility fees, radiologist professional fees, and contrast charges creates a complex billing structure where a single study can generate two or three separate invoices from different billing entities. Understanding that the facility fee and the radiologist's professional fee are billed separately can help patients anticipate and reconcile their explanation of benefits from insurance.
After your scan, a radiologist — a physician who specializes in interpreting medical images — reads the images and produces a written report. This report is sent to your ordering physician, who reviews it in the context of your symptoms and medical history and communicates the findings to you. Radiologists rarely speak directly with patients. If you want to understand your MRI report, ask your doctor to explain the key findings during your follow-up appointment. Request a copy of the images (usually available on CD or via a patient portal) if you're seeking a second opinion — you're entitled to your own records.
Behind every MRI scan is an MRI technologist — the healthcare professional who operates the scanner, positions the patient, adjusts scan parameters, monitors image quality in real time, and ensures patient safety throughout the procedure. MRI technologists are trained to recognize when a patient is becoming too uncomfortable to continue, when image quality has been compromised by motion, and when a finding on the scout images warrants alerting the supervising radiologist before proceeding. The role requires technical knowledge of MRI physics, anatomy, patient care, and safety protocols.
Becoming a licensed MRI technologist typically requires completing an accredited radiologic technology program followed by MRI specialty training, or completing an MRI-specific educational program directly. The American Registry of Radiologic Technologists (ARRT) administers the primary credentialing exam. Demand for MRI technologists is strong — the Bureau of Labor Statistics projects above-average employment growth for radiologic technologists as the population ages and demand for diagnostic imaging increases. Attending an accredited MRI tech school is the most direct path to entering the field, with programs available at community colleges, hospitals, and universities across the country.
MRI technology continues to advance rapidly. Artificial intelligence-assisted image reconstruction now allows faster scan protocols without sacrificing resolution — reducing scan times that previously took 60 minutes to 20 or 30 minutes for certain protocols. MRI-guided focused ultrasound, a technique that uses MRI to target high-intensity ultrasound energy at specific tissue targets, is expanding treatment options for movement disorders like essential tremor and Parkinson's disease tremor.
MRI-linac systems — combining an MRI scanner with a radiation therapy linear accelerator — allow real-time tumor tracking during radiation treatment for cancer. The MRI platform, once primarily a diagnostic tool, is becoming a platform for guided therapy as well.
For patients who've recently had an MRI and are waiting on results, understanding what the imaging report contains can reduce anxiety while awaiting your physician's call. Most MRI reports start with a clinical history summary — the reason the scan was ordered — followed by a technique section describing the sequences performed, and then a findings section detailing what was observed in each anatomical region.
The final section is the impression or conclusion, which is the radiologist's interpretive summary and the part most relevant to your clinical care. Knowing this structure helps you follow along when your doctor walks you through the findings and explains what the next steps in your care should be.
Common Types of MRI Scans
The most frequently ordered MRI study. Evaluates stroke, multiple sclerosis, tumors, hemorrhage, epilepsy, dementia, headaches, and cranial nerve pathology. Brain MRI with and without contrast is standard for tumor characterization and inflammatory conditions. MR angiography (MRA) visualizes cerebral blood vessels without catheter-based angiography.
Evaluates disc herniation, spinal stenosis, cord compression, nerve root impingement, fractures (stress and compression), tumors, and inflammatory conditions of the spine and cord. Cervical, thoracic, and lumbar spine studies are ordered separately based on symptoms. One of the highest-volume outpatient MRI studies in orthopedics and neurology.
Knee, shoulder, hip, wrist, ankle — evaluated for ligament and tendon tears, meniscal pathology, cartilage loss, stress fractures, labral tears, and bone marrow lesions. MRI arthrography (with intra-articular contrast) provides superior labral and cartilage detail. The gold standard before most joint surgeries where soft tissue pathology is the primary question.
Liver lesion characterization, pancreatic assessment, kidney and adrenal evaluation, uterine fibroids, endometriosis, ovarian pathology, and prostate cancer staging. MRCP (magnetic resonance cholangiopancreatography) evaluates bile ducts and pancreatic ducts without contrast or radiation. MRI of the prostate (mpMRI) has become essential for targeting biopsies in suspected prostate cancer.
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.