MRI Machine: How It Works, Types, Field Strengths, and What to Expect
Learn how an MRI machine works, understand different magnet strengths, open vs. closed designs, what happens during your scan, and how to prepare.
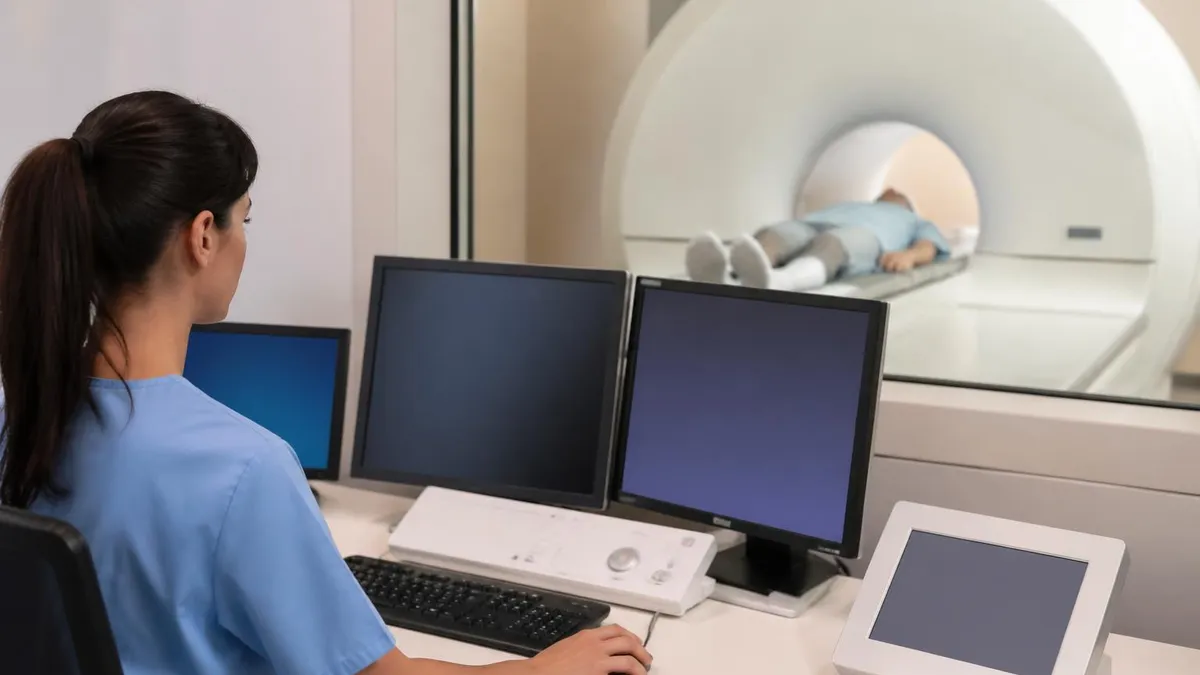
An MRI machine generates images of the body's internal structures using a powerful magnetic field and radiofrequency (RF) pulses — no ionizing radiation involved. Inside the bore (the tunnel) of the scanner, a superconducting electromagnet creates a magnetic field typically 1.5 to 3 Tesla in clinical settings — roughly 30,000 to 60,000 times stronger than the Earth's magnetic field.
That field aligns the hydrogen nuclei in your body's water molecules. RF pulses then knock those nuclei out of alignment. As they return to equilibrium, they emit signals that the scanner captures and reconstructs into cross-sectional images. The whole process is silent to the patient except for the loud knocking sounds the gradient coils make during each sequence.
MRI's key clinical advantage is soft tissue contrast — it distinguishes between different types of tissue far better than CT or X-ray. A brain tumor surrounded by white matter, a torn knee ligament, a herniated disc pressing on a nerve root, a focal lesion in the liver — all of these appear with remarkable detail on MRI sequences that CT simply can't replicate. That's why MRI is the imaging modality of choice for neurological conditions, musculoskeletal injuries, and many abdominal and pelvic evaluations.
Whether you're a patient preparing for a scan, a radiologic technologist (RT) studying for the ARRT MRI certification exam, or a radiology student building foundational knowledge, understanding the machine itself — its physics, its components, its different types, and its limitations — is essential context for everything else about MRI. This guide covers the hardware and physics fundamentals, patient preparation, what to expect during a scan, and how different machine types affect image quality and clinical utility.
MRI Machine at a Glance
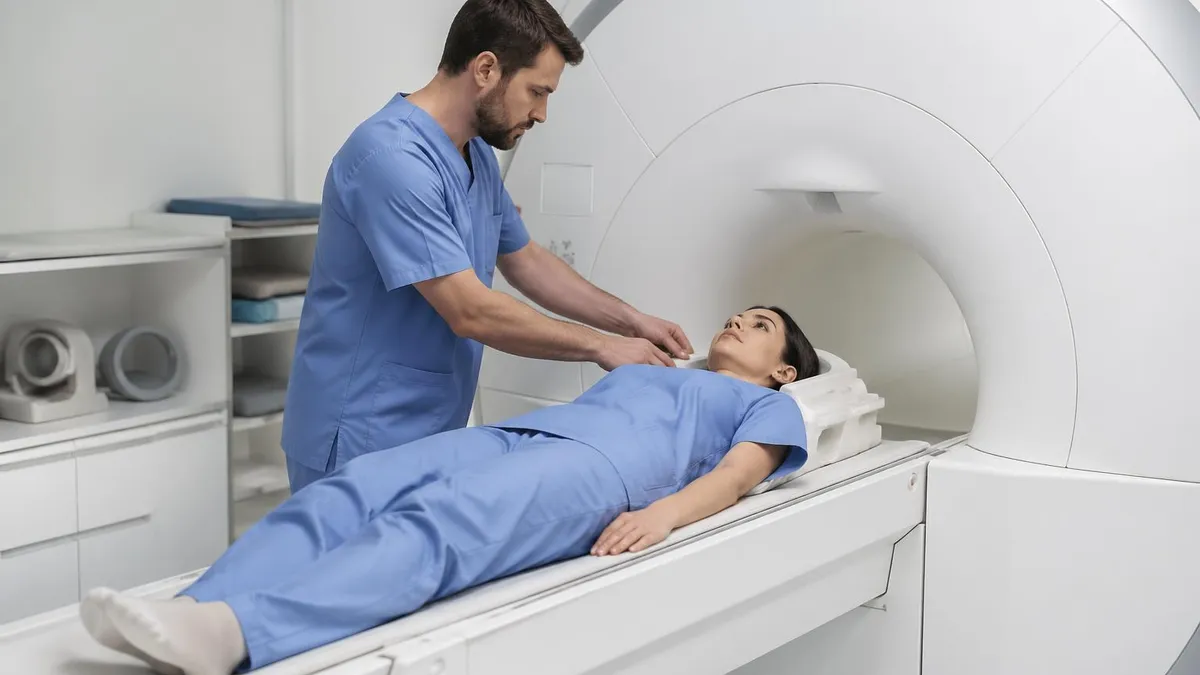
The physics of MRI begins with nuclear magnetic resonance (NMR) — a phenomenon discovered in 1946 by physicists Felix Bloch and Edward Purcell (who shared the 1952 Nobel Prize for it). In a strong magnetic field, hydrogen protons (single-proton nuclei abundant in water and fat) align with the field and precess (spin) at a characteristic frequency called the Larmor frequency, which is proportional to field strength. At 1.5T, hydrogen protons precess at about 63.8 MHz; at 3T, about 127.7 MHz. An RF pulse at exactly this frequency tips the protons out of alignment.
When the RF pulse ends, protons return to equilibrium in two simultaneous but independent processes: T1 relaxation (longitudinal recovery, the time constant for the spin-lattice interaction) and T2 relaxation (transverse decay, the time constant for spin-spin dephasing). Different tissues have different T1 and T2 values — and those differences are what create image contrast. Fat has a short T1 (bright on T1-weighted images), water has a long T1 (dark on T1-weighted images). Water has a long T2 (bright on T2-weighted images), which makes fluid-sensitive sequences the primary tool for detecting edema, inflammation, and most pathology.
Pulse sequences — the programmed timing of RF pulses and gradient field changes — control which tissue properties dominate the image. A T1-weighted sequence (short TR, short TE) shows anatomy and enhances gadolinium contrast. A T2-weighted sequence (long TR, long TE) detects pathology, edema, and fluid. FLAIR (Fluid Attenuated Inversion Recovery) suppresses CSF signal, making white matter lesions in the brain more visible. STIR (Short Tau Inversion Recovery) suppresses fat, revealing bone marrow edema and soft tissue pathology adjacent to fat. Knowing which sequence to use for which clinical question is a core competency for MRI technologists and radiologists alike.
Clinical MRI machines are categorized primarily by field strength. The 1.5 Tesla (1.5T) scanner is the workhorse of clinical radiology — it balances image quality, scan speed, safety profile, and equipment cost in a way that makes it the most widely deployed field strength globally. Most clinical MRI protocols are designed around 1.5T, and the diagnostic performance across a wide range of indications is well-established.
The 3 Tesla (3T) scanner offers higher signal-to-noise ratio (SNR) — roughly twice that of 1.5T in theory — enabling finer spatial resolution, faster scan times, or both. 3T is preferred for brain imaging, functional MRI (fMRI), and applications where subtle anatomy matters most.
Higher field strengths have tradeoffs. At 3T, susceptibility artifacts are more pronounced — metallic implants, surgical clips, and air-tissue interfaces create more distortion than at 1.5T. Specific absorption rate (SAR) — the rate at which RF energy is deposited in tissue — increases with field strength, limiting how rapidly some sequences can be run at 3T without exceeding safety limits. And equipment cost is substantially higher: a 3T scanner costs $2–3 million versus $1–1.5 million for 1.5T, influencing which systems smaller hospitals and outpatient centers can deploy.
7 Tesla (7T) scanners exist primarily in research settings, with a small number of FDA-cleared clinical applications. At 7T, the spatial resolution achievable in the brain — sub-millimeter in all three dimensions — enables visualization of hippocampal subfields, cortical layers, and small vascular malformations not detectable at lower field strengths. The challenges are significant: SAR limitations are severe, image homogeneity across large FOVs is problematic, and B1 field inhomogeneity requires sophisticated RF pulse design to compensate. 7T remains a specialized tool rather than a clinical standard.
Types of MRI Machines
The classic closed-bore cylindrical scanner — what most people picture when they hear MRI — houses a superconducting magnet cooled with liquid helium to near absolute zero (approximately -269°C). The superconducting coils carry current with zero electrical resistance, maintaining the static magnetic field continuously without power draw. Bore diameter is typically 60–70 cm; some wide-bore designs reach 70–75 cm to accommodate larger patients or reduce claustrophobia.
Closed-bore scanners provide the highest field strengths and best image quality. The bore length (typically 150–180 cm) and the noise produced by gradient coils during sequences can be challenging for claustrophobic patients. Short-bore designs (bore length under 150 cm) reduce this significantly, and combined with wider bore diameters, they've made closed-bore MRI accessible to the majority of patients who previously might have required sedation or an open scanner.
MRI anatomy knowledge is the clinical application layer that turns physics and hardware knowledge into diagnostic value. A brain MRI protocol typically includes T1-weighted axial and sagittal images, T2/FLAIR axial images for lesion detection, DWI (Diffusion Weighted Imaging) for acute ischemia, and post-contrast T1 images if pathology requires enhancement evaluation.
Knowing which structures are visible on which sequence and why — white matter appears bright on T1 because of its myelin lipid content; CSF appears white on T2 because of its long T2 relaxation — is the knowledge that allows technologists to recognize and report quality issues and allows radiologists to interpret findings accurately.
Musculoskeletal MRI requires anatomical precision in both positioning and sequence selection. A knee MRI protocol includes T1-weighted coronal and sagittal images for anatomy, fat-suppressed T2 or PD (Proton Density) for menisci and cartilage, and STIR or fat-suppressed T2 for bone marrow and soft tissue edema. The orientation of the scan plane matters: ACL evaluation requires oblique sagittal alignment along the ACL's long axis; meniscal evaluation uses strictly coronal and sagittal planes. Suboptimal positioning causes artifacts or misses pathology — a technically correct but clinically inadequate scan.
Pathology recognition on MRI requires understanding both normal anatomy and the appearance of common pathological processes. Edema appears as increased signal on T2-weighted and STIR sequences — in bone marrow, it suggests fracture, tumor, or infection; in soft tissue, it suggests acute injury or inflammation. Gadolinium contrast enhancement indicates breakdown of the blood-brain barrier or blood-vessel permeability — it's the primary tool for identifying active inflammation, tumors, and infectious processes. Understanding these patterns is what the ARRT MRI certification registry examination tests, alongside physics and safety knowledge.
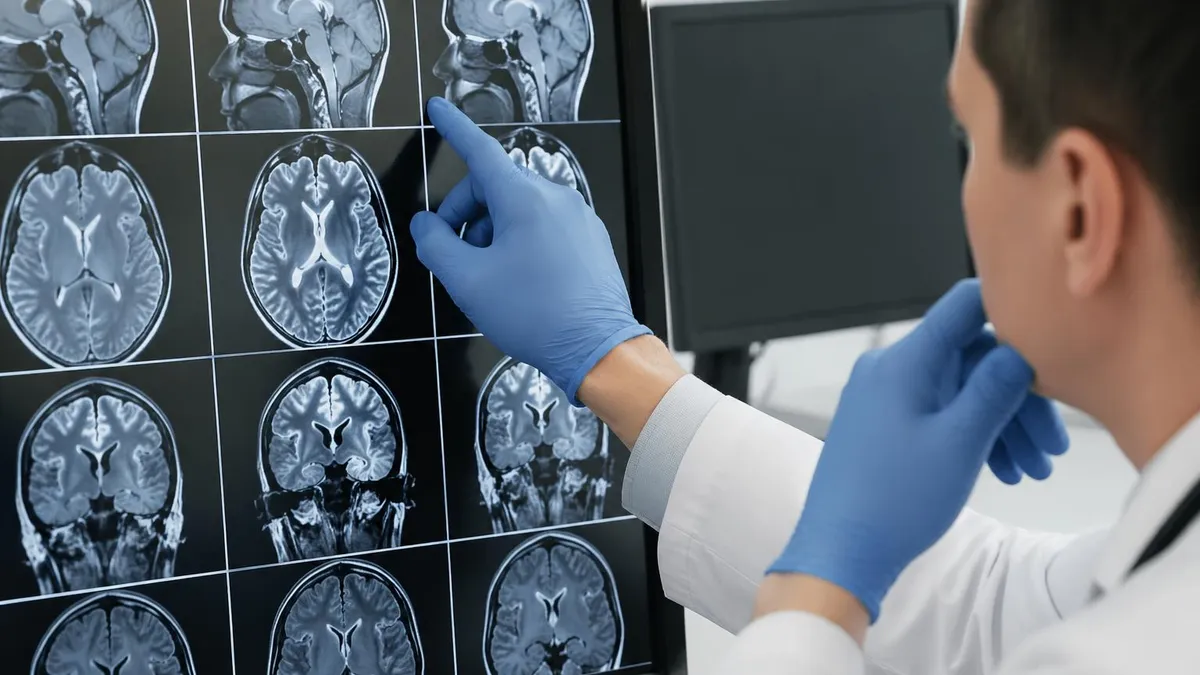
Key Components of an MRI Machine
The superconducting electromagnet creates the static B0 field that aligns hydrogen protons. Cooled to near absolute zero with liquid helium, it maintains the field continuously without power. The magnet's homogeneity (measured in ppm) directly affects image quality — inhomogeneity causes geometric distortion and signal variation.
Three sets of coils (X, Y, Z) create small, precisely controlled variations in the magnetic field that spatially encode the MRI signal — allowing the computer to determine where each signal originates. Gradient coils are the source of the loud knocking sounds during MRI scans, as they flex under high electrical current pulses.
Transmit RF pulses at the Larmor frequency to excite hydrogen protons, then receive the signals emitted during relaxation. Surface coils (head coil, knee coil, shoulder coil) are placed close to the anatomy being imaged for maximum SNR. Body coil is built into the bore for larger anatomy and whole-body applications.
Receives raw k-space data (the spatial frequency data encoded by the gradients), applies Fourier Transform to reconstruct MRI images, and manages the complex timing sequences that define each pulse protocol. Modern MRI workstations also apply AI-based reconstruction algorithms that reduce noise and improve spatial resolution.
Patient preparation for MRI begins with a thorough safety screening questionnaire — and this screening is genuinely life-critical, not bureaucratic formality. Certain metal implants are incompatible with MRI: some older cardiac pacemakers and defibrillators, cochlear implants, some cerebral aneurysm clips, metallic foreign bodies in the eye, and various other devices can malfunction, heat, or be physically displaced in the magnetic field. The ACR (American College of Radiology) maintains the ACR Manual on MR Safety, which is the authoritative reference for implant compatibility, and MRISafety.com (the Shellock online database) lists specific device models with conditional or unsafe ratings.
Gadolinium contrast agents — used to highlight areas of abnormal vascular permeability or blood-brain barrier breakdown — are administered intravenously when the clinical indication requires it. Standard gadolinium-based contrast agents (GBCAs) have an excellent safety profile in patients with normal kidney function. In patients with severely reduced kidney function (eGFR below 30), some GBCAs carry risk of nephrogenic systemic fibrosis (NSF), a serious fibrotic condition. Macrocyclic GBCAs (like gadobutrol) are safer than linear agents in this context. The prescribing physician and radiologist must weigh the clinical need for contrast against renal risk for each patient.
Claustrophobia is the most common patient complaint — estimates suggest 4–20% of patients experience anxiety significant enough to affect scan quality or require intervention. Management options include wide-bore scanner selection, music or video goggles during the scan, conscious sedation (requires nursing monitoring and recovery time), and for some patients, anxiolytic medication prescribed before the appointment. Many facilities have developed specific protocols for claustrophobic patients that reduce scan time and minimize bore exposure time while maintaining diagnostic quality.
MRI Machine: Advantages and Limitations
- +No ionizing radiation — safe for repeated scans and pediatric patients without cumulative exposure risk
- +Superior soft tissue contrast compared to CT, X-ray, or ultrasound for brain, spine, and musculoskeletal pathology
- +Multi-planar imaging in any plane without moving the patient — axial, sagittal, coronal, oblique
- +Functional imaging capability — fMRI, MR spectroscopy, diffusion tensor imaging, perfusion imaging
- +No bone artifact — bone appears dark on MRI (cortical bone has few mobile protons), improving visualization of adjacent structures
- +Contrast agents are generally safer than CT iodinated contrast for patients with iodine allergy
- −Loud — gradient coil noise reaches 100–110 dB during sequences; hearing protection is required
- −Claustrophobic — the closed-bore design causes anxiety or panic in 4–20% of patients
- −Slow compared to CT — a typical MRI takes 20–60 minutes versus 5–10 minutes for a CT
- −Metal contraindications — many implants are incompatible or require careful assessment before entering the magnet
- −Motion sensitivity — patient movement blurs MRI images more severely than CT due to longer acquisition times
- −High equipment cost ($1–3M+) limits availability in lower-resource settings, creating access inequities
MRI anatomy and positioning knowledge — the bread and butter of the ARRT MRI registry examination — covers both correct anatomical localization and the technical factors that determine image quality. Positioning errors cause more failed or repeated MRI examinations than equipment malfunctions. Placing the anatomy of interest at the isocenter of the magnet (the point of highest field homogeneity) maximizes SNR. Appropriate coil selection for the anatomy — a dedicated knee coil versus a flexible surface coil versus the body coil — directly affects spatial resolution and signal quality.
The ARRT MRI certification examination tests across three content areas: Patient Care (17%), Safety (15%), and Imaging Procedures (68%). The imaging procedures section covers pulse sequences, image quality parameters, anatomical cross-sectional knowledge, and artifact recognition and correction. Artifacts — the specific image distortions that occur due to patient motion, magnetic susceptibility, chemical shift, aliasing, and other physical phenomena — are heavily tested because recognizing them is essential for quality assurance and accurate diagnosis.
Aliasing (wrap-around) artifact occurs when anatomy outside the field of view wraps into the image from the opposite side. Chemical shift artifact appears as a bright or dark band at fat-water interfaces along the frequency-encoding direction. Susceptibility artifact — blooming or signal dropout near metal or air-tissue interfaces — is field-strength dependent and worse at 3T than 1.5T. Each artifact has specific causes and specific remedies: adjusting FOV, swapping phase and frequency encoding directions, applying fat saturation, choosing a different sequence type. Knowing the cause, appearance, and correction for each major artifact is registry-level knowledge that also improves daily practice.
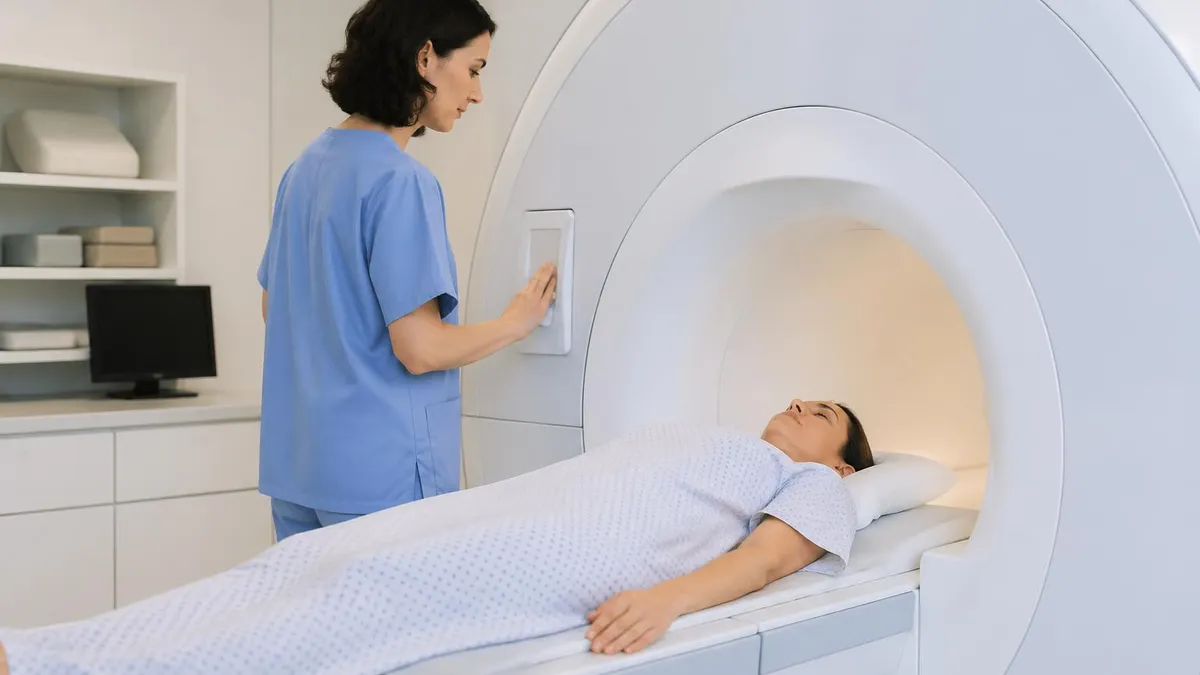
MRI Safety and Patient Prep: Key Steps
The ARRT MRI certification exam requires a radiologic technologist to have completed an accredited MRI education program or have equivalent structured on-the-job training documented per ARRT requirements, in addition to holding a primary ARRT credential (typically R — Radiography). Candidates must pass a 200-question multiple-choice exam covering the content areas above. The passing rate for first-time ARRT MRI candidates runs approximately 70–75%. Candidates who fail can retake the exam after a waiting period, but each retake requires a new application and fee.
Structured study for the ARRT MRI registry should prioritize the imaging procedures section (68% of the exam) while ensuring solid coverage of safety (15%) and patient care (17%). Safety content is particularly important because errors in safety screening carry the highest consequence in clinical practice — a missed cardiac pacemaker or aneurysm clip entering a magnet room is a potentially fatal event. The exam tests safety knowledge specifically because it's non-negotiable in clinical practice, not just academically important.
Practice examinations are among the most effective preparation tools because the ARRT exam's format — long multiple-choice questions with nuanced distractors — requires familiarity with the question style, not just knowledge recall. Working through registry-format practice questions, reviewing explanations for incorrect answers, and identifying the specific content areas where your knowledge is weakest allows systematic targeted review rather than broad re-reading of textbooks that covers both strong and weak areas equally.
The MRI Magnet Is Always On — Even When Not Scanning
Unlike an X-ray machine or CT scanner, the MRI magnet cannot be turned off quickly in most installations — it must be ramped down slowly over hours, a process called quenching. The fringe field extends beyond the scanner bore and outside the scan room. Anyone entering the MRI suite must be screened for metallic implants and ferromagnetic objects before entering the zone where the fringe field poses risk. This is why the ACR's Zone 4 model — the area within the scanner bore and immediate surroundings — requires controlled access at all times, even when no patient is being scanned.
Advanced MRI applications — diffusion MRI, functional MRI (fMRI), MR spectroscopy, MR angiography, cardiac MRI — expand beyond the anatomical imaging that defines most clinical MRI. Diffusion-weighted imaging (DWI) detects restricted water diffusion at the cellular level, allowing acute ischemic stroke to be identified within minutes of onset — far earlier than conventional T2 changes appear. It's also the primary tool for differentiating benign from malignant tissue in many organs (restricted diffusion in densely cellular tumors), and for detecting abscess versus tumor in the brain.
Cardiac MRI — when performed at centers with dedicated expertise — provides the most comprehensive assessment of cardiac function, morphology, and tissue characterization available by any imaging modality. Myocardial fibrosis (late gadolinium enhancement), myocarditis, cardiac sarcoidosis, and cardiomyopathy evaluation are clinical scenarios where cardiac MRI provides information that echocardiography cannot. The technical demands are high: cardiac gating, breath-holding coordination, and the need for ECG-triggered sequences make cardiac MRI more complex to perform and to quality-control than standard body MRI.
MR spectroscopy adds biochemical information to anatomical imaging — measuring the concentrations of specific metabolites (NAA, choline, creatine, lactate) in a defined brain region to characterize tissue. It's used in neuro-oncology to differentiate tumor recurrence from treatment effect (radiation necrosis), in epilepsy to localize abnormal metabolite patterns, and in pediatric brain disorders. Like cardiac MRI, it requires specific technical training and quality control expertise that isn't universally available — it's a capability that distinguishes specialized neuroradiology centers from general radiology practices.
MRI technologist careers are strong and growing. The BLS projects 6% job growth for radiologic technologists through 2032, and MRI specialists command a salary premium over general radiologic technologists — national median salaries for MRI technologists run approximately $79,000–$95,000 depending on location, facility type, and experience level. Travel MRI techs earn considerably more — $2,000–$3,000+ per week in high-demand markets, at the cost of temporary placements rather than permanent positions. Specialization in cardiac MRI or body MRI at academic centers offers the highest salaries and the most technically demanding work.
The field is evolving rapidly toward AI-assisted acquisition and reconstruction. MRI vendors now offer AI-based scan acceleration that reconstructs diagnostic-quality images from undersampled data — cutting scan times by 50–70% for some protocols. These tools require that technologists understand what the AI is doing and can recognize when its reconstruction has introduced artifacts or missed pathology. Technical literacy about AI reconstruction is becoming a professional competency, not just a vendor marketing term, for MRI specialists at facilities that deploy these systems.
Whether you're preparing for the ARRT registry exam, building MRI knowledge for clinical practice, or simply trying to understand what that machine does when you're inside it, the same fundamentals apply: strong magnetic field, RF excitation, tissue-specific relaxation, signal encoding, and image reconstruction. The clinical value — the ability to see a tumor, characterize tissue, guide a biopsy, or confirm a diagnosis without exposing the patient to radiation — is the product of that physics applied with precision and expertise at every step of the imaging chain.
Positioning and anatomy knowledge for the ARRT MRI registry exam covers the major body regions examined with MRI: brain, spine (cervical, thoracic, lumbar), musculoskeletal (shoulder, knee, hip, wrist, ankle), abdomen, pelvis, and breast. Each region has standard protocols — defined sequences, orientations, and coverage — that represent the minimum for a diagnostically adequate study. Deviating from protocol requires specific clinical justification; for example, adding a diffusion sequence for a brain tumor follow-up or a dedicated MRCP (Magnetic Resonance Cholangiopancreatography) sequence for a suspected biliary obstruction.
Cross-sectional anatomy proficiency — recognizing structures on axial, sagittal, and coronal MRI images — is tested with image identification questions on the registry exam. The brain's major structures (cortex, basal ganglia, thalamus, hippocampus, cerebellum, brainstem), the spine's components (disc, end plate, neural foramen, spinal cord, conus), and the knee's anatomy (menisci, ACL, PCL, collateral ligaments, articular cartilage) are all fair game. Systematic study of cross-sectional anatomy using dedicated MRI anatomy atlases builds this competency more efficiently than clinical exposure alone.
The practice tests linked throughout this article cover the exact content domains tested on the ARRT MRI registry exam and relevant for clinical MRI practice. Start with the knowledge foundation (physics, safety screening, contrast agent use), build depth in anatomy and pathology recognition, and systematically review imaging procedures including artifact identification and pulse sequence selection. Consistent practice across these domains — not just the areas you already know well — is what moves registry performance from marginal to confident pass.
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.