MRI Meaning: What Is an MRI Scan? Complete Guide 2026
MRI meaning explained — how MRI scans work, what they detect, types of MRI, patient preparation, and MRI technologist career overview 2026.
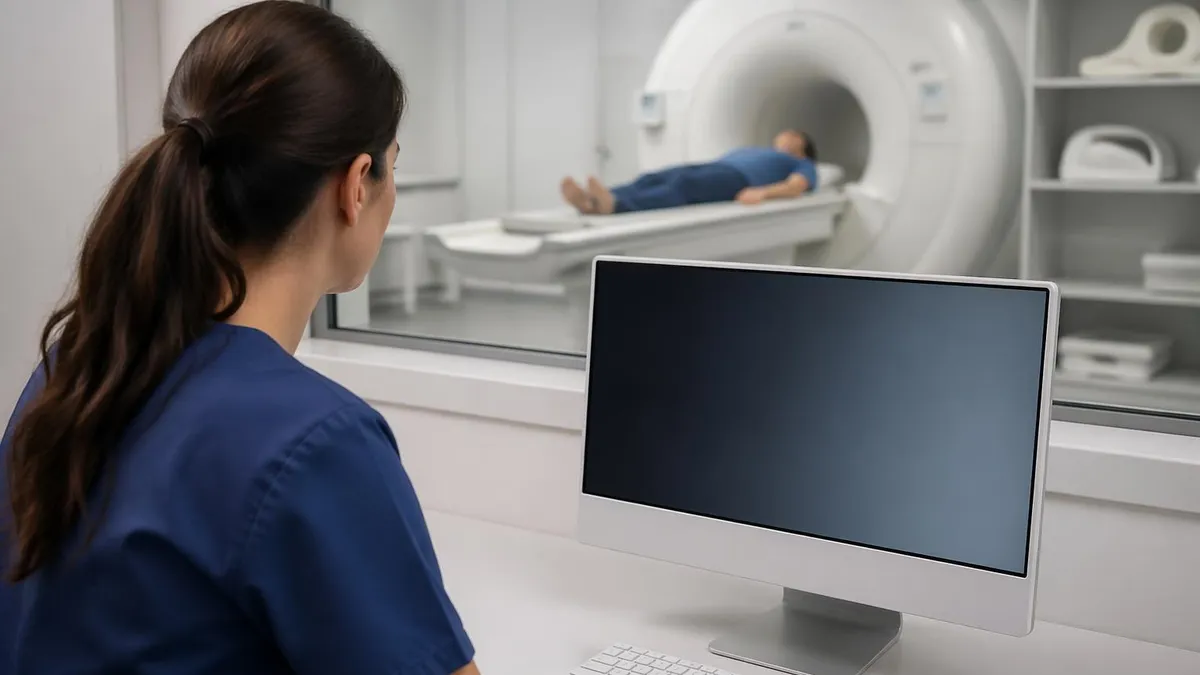
How MRI Works
Magnetic Resonance Imaging works by exploiting the magnetic properties of hydrogen atoms in the human body. Since the body is approximately 60–70% water — and water molecules contain hydrogen — the human body is an ideal subject for MRI.
The MRI scanner generates a powerful static magnetic field (typically 1.5 Tesla or 3.0 Tesla in clinical settings, compared to Earth's magnetic field of approximately 0.00005 Tesla). When a patient enters this field, the hydrogen protons in their body align with the magnetic field, much like compass needles aligning with Earth's magnetic north.
The scanner then emits brief pulses of radiofrequency (RF) energy. These pulses temporarily knock the hydrogen protons out of alignment. When the RF pulse ends, the protons 'relax' back to their aligned position, releasing energy as a radio signal. Receiver coils in the scanner detect these signals, and sophisticated computer algorithms convert the signal data into detailed cross-sectional images of the body.
Two key MRI parameters — T1 relaxation time and T2 relaxation time — measure different aspects of how protons return to equilibrium. Different tissues have characteristic T1 and T2 values, allowing the MRI system to distinguish fat from muscle from fluid from pathology. By varying the timing parameters of the RF pulses (TR: repetition time, TE: echo time), radiographers can produce T1-weighted or T2-weighted images that highlight different tissue characteristics and pathologies.
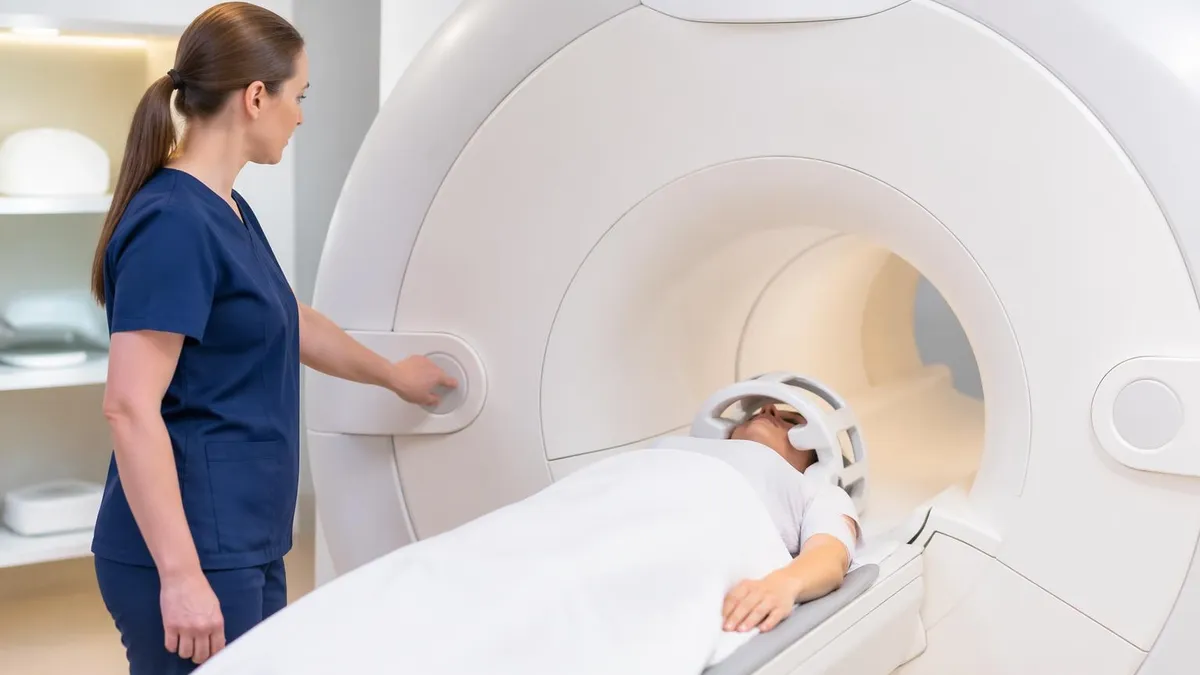
Standard (Conventional) MRI
The most common type of MRI, performed in a cylindrical bore magnet. The patient lies on a table that slides into the center of the magnet for the duration of the scan. Standard bore diameter is 60–70 cm. Scan duration ranges from 20 to 90 minutes depending on the body region and number of sequences acquired. Produces the highest quality images for most diagnostic applications including brain, spine, joints, and abdominal organs.
What MRI Can Detect
MRI excels at imaging soft tissue structures that are poorly visualized by X-ray and sometimes by CT. The conditions and body regions where MRI provides the most diagnostic value include:
Brain and nervous system: Brain tumors (primary and metastatic), stroke (diffusion-weighted imaging detects acute infarction within minutes), multiple sclerosis plaques, cerebral edema, hemorrhage, demyelinating disease, hydrocephalus, epilepsy (structural causes), and neurodegenerative conditions. Brain MRI is often the first-choice imaging study for new neurological symptoms.
Spine: Herniated discs, spinal cord compression, epidural abscess, spinal tumors, degenerative disc disease, and post-surgical changes. MRI is the definitive study for evaluating radiculopathy (nerve root compression) and myelopathy (spinal cord dysfunction).
Musculoskeletal system: Ligament tears (ACL, rotator cuff), meniscal tears, cartilage damage, bone marrow edema, soft tissue tumors, and stress fractures. MRI can detect bone stress injuries before they appear on X-ray, making it invaluable in sports medicine.
Abdominal organs: Liver masses (distinguishing benign hemangiomas from metastases or hepatocellular carcinoma), biliary system (MRCP for pancreatic and bile duct evaluation without invasive endoscopy), kidney masses, uterine fibroids, ovarian cysts, and adrenal lesions.
Cancer staging: MRI is the preferred modality for staging prostate cancer (multiparametric MRI, or mpMRI), rectal cancer (determining local extent), and breast cancer (bilateral breast MRI for high-risk screening and extent of disease).
MRI vs CT vs X-Ray: When Is Each Used?
Understanding the relative strengths and limitations of MRI, CT, and X-ray helps clarify why physicians choose each modality for specific clinical questions.
X-ray is the fastest and least expensive imaging modality, using ionizing radiation. It excels at imaging bone (fractures, alignment), chest (pneumonia, heart size, pulmonary edema), and foreign body detection. X-ray is poor for soft tissue visualization. A standard chest X-ray takes under a minute and is available in virtually every clinical setting.
CT (Computed Tomography) also uses ionizing radiation but acquires multiple cross-sectional images that can be reconstructed in any plane. CT is faster than MRI (whole-body scans in seconds with modern 64-slice scanners) and is ideal for emergency settings, trauma evaluation, abdominal pain, pulmonary embolism (CTA), and any situation where speed is critical. CT provides excellent bone detail and good soft tissue detail with IV contrast. The primary limitation is radiation dose — a concern for cumulative exposures, particularly in children.
MRI offers superior soft tissue contrast without radiation. It is slower, more expensive, and less widely available than CT. MRI is the preferred choice for brain and spine pathology, joint injuries, soft tissue tumors, and any situation where radiation should be minimized (pregnancy, pediatrics, repeated imaging). MRI is also more sensitive to patient motion — even slight movement during the 20–90 minute scan can degrade image quality. Metal implants are another consideration: most modern implants are MRI-compatible, but screening is required before every scan.
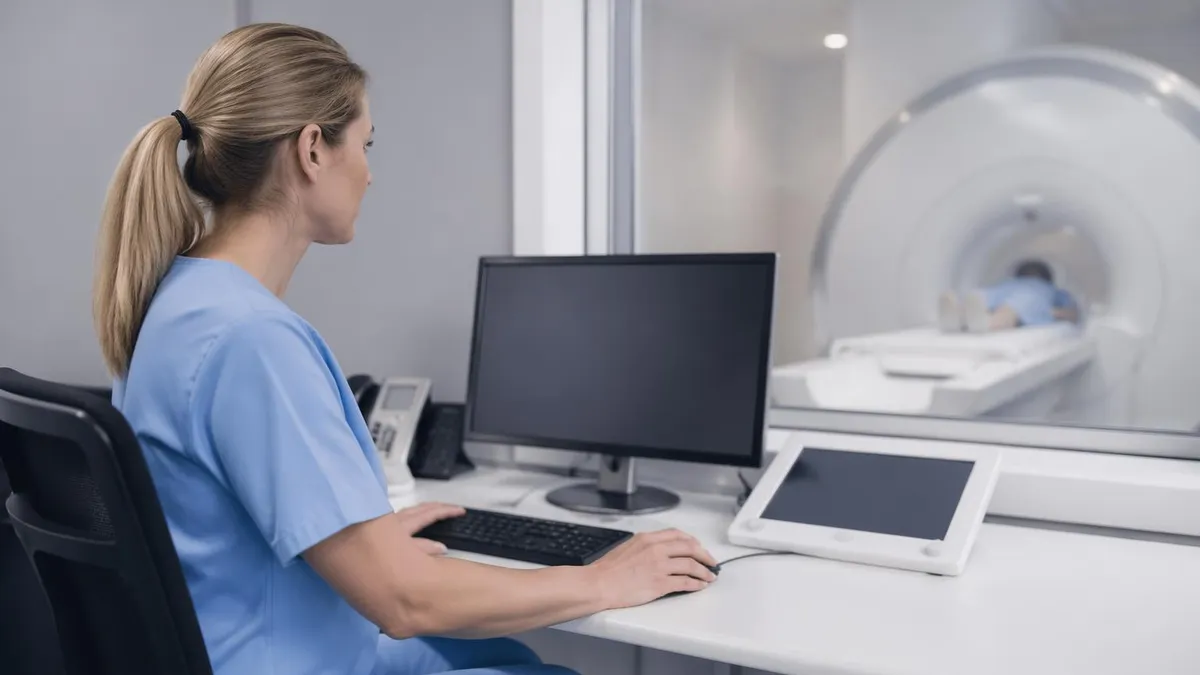
What to Expect During Your MRI
When you arrive for an MRI, a technologist will complete a detailed safety screening questionnaire. You will change into a hospital gown and store all metallic items in a locker outside the scan room. The technologist will explain the procedure and answer any questions before you enter the scanner room.
During the scan, you will hear loud knocking and banging sounds — these are normal and come from the gradient coils rapidly switching on and off. Most facilities provide earplugs or headphones with music. An intercom lets you communicate with the technologist at any time, and a squeeze bulb allows you to signal the technologist if you need to pause the scan. Staying completely still during each sequence is critical; any movement degrades image quality and may require the sequence to be repeated.
If intravenous contrast is needed, the technologist or nurse will place an IV before or during the scan. Gadolinium contrast is typically administered partway through the protocol. Most patients feel only a brief sensation of coolness during injection. After the scan, there are no restrictions — you can drive, eat, and resume normal activities immediately unless you received sedation.
MRI Technologist Career Overview
An MRI technologist (MRI tech) is the healthcare professional who operates MRI equipment, positions patients, selects imaging sequences, and produces diagnostic images for radiologist interpretation. MRI techs work in hospitals, outpatient imaging centers, physician offices, and mobile MRI services.
The standard educational pathway is either an associate's or bachelor's degree in radiologic technology, followed by specialized MRI registry examination through the American Registry of Radiologic Technologists (ARRT). Alternatively, candidates who hold another ARRT certification (such as Radiography or Nuclear Medicine) can qualify through a primary pathway exam or post-primary certification.
The ARRT MRI certification exam covers equipment operation and quality control, MRI safety, patient care, image production, and imaging procedures. For a detailed breakdown of MRI tech education programs and requirements, see our guide on MRI tech school programs, which covers accredited program lists, admission requirements, and clinical hour expectations.
Salary and job outlook are strong. The Bureau of Labor Statistics (BLS) reports a 2023 median salary of $77,870 for MRI technologists, with top earners exceeding $100,000. The field is projected to grow 7% from 2022–2032, driven by the aging population's increased need for diagnostic imaging and continued expansion of MRI indications in clinical medicine.
ARRT MRI Registry Exam Preparation
The ARRT MRI examination is a computer-adaptive test covering the full scope of MRI practice. The exam contains 200 questions (175 scored, 25 pretest), and a passing score requires demonstrated competency across all content categories. The exam is administered at Prometric testing centers nationwide.
The ARRT MRI content specifications are organized into four major categories:
- Patient Care (10%) — screening, contrast administration, patient monitoring, IV access
- Safety (30%) — magnetic field zones, ferromagnetic object hazards, SAR (specific absorption rate), implant screening, RF and gradient safety, quench procedures
- Image Production (46%) — pulse sequences (SE, GRE, EPI), image quality parameters, k-space, coil selection, artifacts and correction, contrast mechanisms (T1, T2, PD, DWI)
- Procedures (14%) — imaging protocols by body region: brain, spine, MSK, abdomen/pelvis, cardiovascular, breast
The highest-weighted category is Image Production at 46%, making it the primary focus of exam preparation. Candidates should allocate proportional study time to each content area. The MRI safety practice tests and MRI anatomy and pathology quizzes on this site align with ARRT content specifications and provide scored practice with explanations to identify knowledge gaps before test day.
Most candidates spend 3–6 months in dedicated exam preparation. Standard resources include the Woodward MRI Complete review text, the Elsevier registry review question bank, and category-specific practice tests. Candidates who have recently completed clinical training report that image production concepts are most improved by active case review — looking at real MRI sequences and practicing sequence identification — rather than passive reading alone.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.