Breast MRI: What It Is, When It Is Used, and What to Expect
Breast MRI guide: who needs one, how it differs from a mammogram, what happens during the scan, what breast MRI detects, and how to prepare for the appointment.
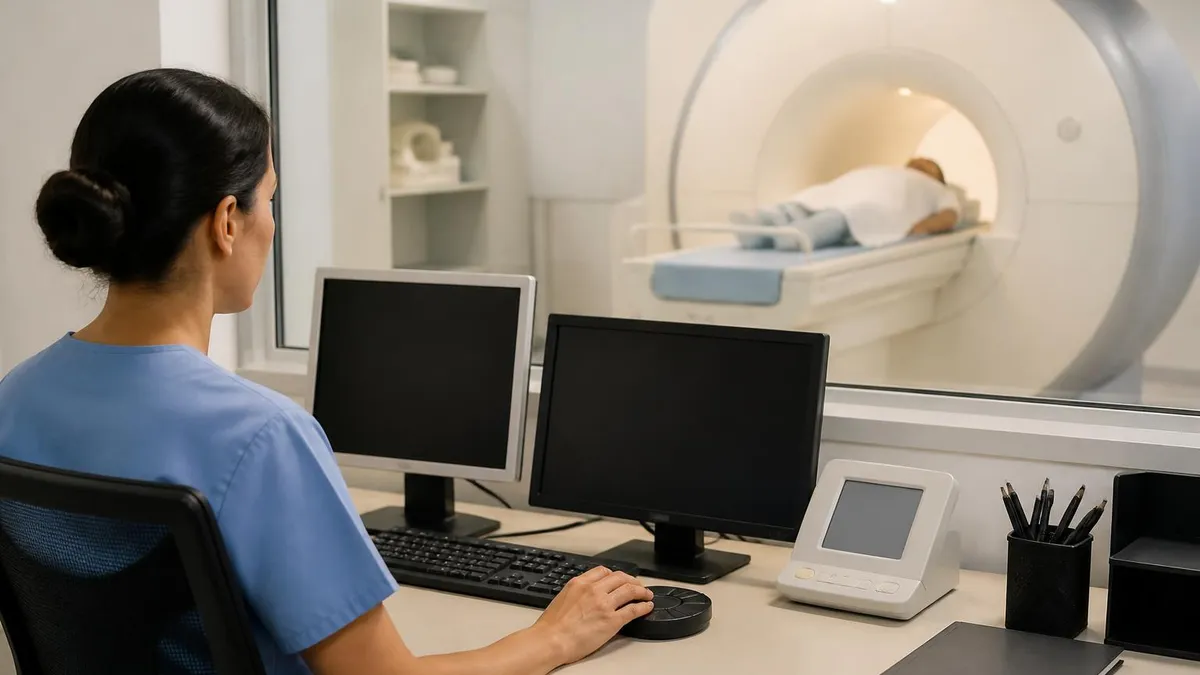
A breast MRI uses magnetic fields and radio waves to create detailed images of breast tissue without radiation. The procedure is more sensitive than a mammogram for detecting certain types of breast cancer, particularly in women with dense breast tissue, high genetic risk, or prior breast cancer history. Breast MRI isn't a replacement for mammography in routine screening for average-risk women — it produces more false positives, takes longer, costs more, and requires contrast dye injection. It's used as a supplemental tool in specific clinical situations where its higher sensitivity justifies the added complexity and cost.
The primary difference between breast MRI and a mammogram is sensitivity versus specificity. A mammogram uses X-ray imaging and is efficient, inexpensive, and widely available. It's the standard first-line screening tool for breast cancer because it catches a broad range of cancers at a reasonable false-positive rate for general population screening.
Breast MRI is more sensitive — it detects a higher percentage of cancers that are present — but it also flags more false positives, meaning more follow-up testing (additional imaging, biopsies) for findings that turn out not to be cancer. For average-risk women, this tradeoff doesn't favor MRI as a screening tool. For high-risk women, the additional sensitivity of MRI is valuable enough to accept the higher false-positive rate as part of the screening strategy.
The contrast dye used in breast MRI, gadolinium, is injected intravenously before or during the scan. Gadolinium highlights areas of increased blood supply, which is a marker for rapidly growing tissue — including cancer. Cancerous tumors typically have higher blood vessel density than surrounding normal tissue, and the contrast enhancement makes these areas appear brighter on the MRI images.
The imaging radiologist looks for characteristic patterns of enhancement — the shape, size, timing, and degree of enhancement — to distinguish suspicious areas from benign findings. Not all enhancing areas are cancer; certain benign conditions including fibrocystic changes, fibroadenomas, and normal breast tissue during certain phases of the menstrual cycle also enhance on contrast MRI, which is why timing the scan in the second week of the menstrual cycle is recommended for premenopausal women.
Understanding the clinical indications for breast MRI — the situations where it's medically appropriate — helps patients understand why their doctor has ordered one or why they might request one. The most common indications are high-risk screening, staging after a breast cancer diagnosis, evaluation of inconclusive mammogram or ultrasound findings, monitoring response to neoadjuvant chemotherapy, and screening for implant rupture. Each of these situations uses breast MRI for a different purpose and produces different expectations about what the scan should find and what happens next based on the results.
Ultrasound-guided biopsy remains the standard method for sampling suspicious breast MRI findings, even though the MRI found them. Most lesions visible on MRI can also be seen on targeted ultrasound, which makes ultrasound-guided biopsy faster and less expensive than MRI-guided biopsy. A small percentage of MRI findings are truly MRI-only — visible only on contrast MRI and not reproducible on targeted ultrasound — and these require MRI-guided biopsy, which is a specialized procedure available at dedicated breast imaging centers.
Breast MRI at a Glance
High-risk breast cancer screening is the most common reason for breast MRI in women who have never had breast cancer. The American Cancer Society (ACS) and the American College of Radiology (ACR) recommend annual breast MRI screening alongside annual mammography for women with certain elevated-risk profiles.
The primary qualifying criteria are: lifetime breast cancer risk estimated at 20% or greater based on validated risk models, known BRCA1 or BRCA2 gene mutation, first-degree relative with a BRCA mutation, history of chest radiation therapy between ages 10–30 (as treatment for lymphoma or other conditions), and certain rare genetic syndromes (Li-Fraumeni, Cowden, or Bannayan-Riley-Ruvalcaba syndrome).
For women with dense breast tissue without other elevated risk factors, breast MRI is not universally recommended as routine supplemental screening, though it's an option that some clinicians discuss in the context of shared decision-making. Dense breast tissue appears as white on a mammogram, which is the same appearance as many cancers, reducing the mammogram's ability to detect cancers within dense tissue.
Breast MRI is not affected by tissue density in the same way — the contrast enhancement pattern is the key signal regardless of background tissue density. However, the decision to use supplemental MRI for dense-breast-only risk needs to account for the false positive rate and the costs, which may not be covered by insurance in the absence of additional risk factors.
Breast MRI for staging after a breast cancer diagnosis evaluates the extent of disease before treatment. When a cancer is found on mammogram or biopsy, an MRI can show whether the cancer is confined to one area of the breast, whether there are additional foci in the same breast (multifocal or multicentric disease), and whether there is involvement in the other breast (bilateral disease). This information directly affects surgical planning — finding additional cancer sites in the same breast may change a planned lumpectomy to a mastectomy, and finding cancer in the contralateral breast changes the surgical approach entirely.
The staging MRI is typically ordered by the breast surgeon before the surgical consultation or before definitive surgery is scheduled.
Monitoring response to neoadjuvant chemotherapy is another established indication for breast MRI. Neoadjuvant chemotherapy is given before surgery to shrink the tumor. Serial MRI scans — typically before treatment starts, midway through, and after completion — show whether the tumor is responding to treatment by measuring changes in size and enhancement characteristics. A tumor that shrinks significantly on MRI during neoadjuvant treatment has a higher likelihood of pathologic complete response, which correlates with better long-term outcomes for certain cancer types.
Imaging response doesn't replace surgical pathology, but it guides clinical decision-making about continuing, modifying, or completing the planned chemotherapy course before surgery. The comparison between MRI and CT scan imaging explains the technical differences between MRI and CT approaches to tumor staging that inform which modality is used in different clinical situations.
Women diagnosed with breast cancer who are considering contralateral prophylactic mastectomy — removing the healthy breast to reduce future cancer risk — benefit from pre-surgical MRI to establish a baseline and evaluate whether both breasts show concerning findings that might affect surgical timing or approach.
Genetic testing for BRCA mutations, which is now covered by many insurance plans for newly diagnosed breast cancer patients, influences the staging MRI interpretation because BRCA carriers have a substantially elevated contralateral cancer risk that affects surgical counseling. Women awaiting BRCA test results at the time of initial diagnosis sometimes defer the staging MRI until results are back, so the imaging can inform a comprehensive conversation about bilateral versus unilateral surgery with complete information.
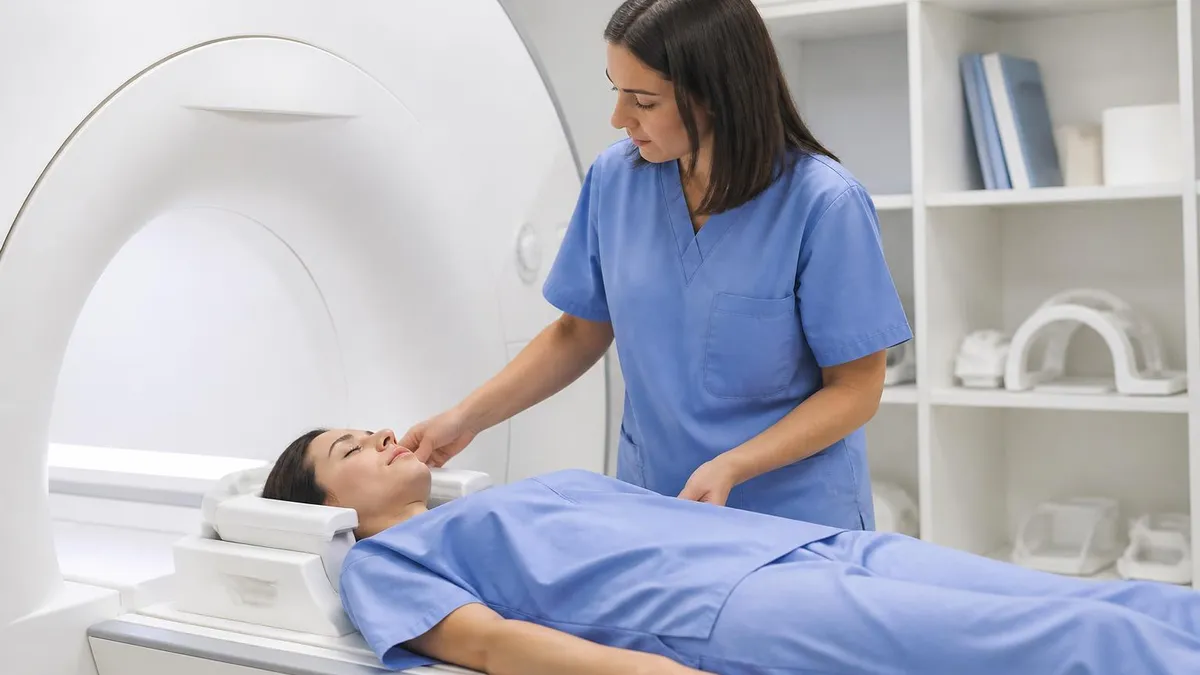
Breast MRI is ordered for women with BRCA1/2 mutations, a family history placing them in the 20%+ lifetime risk category, prior chest radiation therapy as a teenager, prior breast cancer diagnosis, or inconclusive findings on mammogram or ultrasound. It's also used for implant rupture evaluation and chemotherapy response monitoring. Most women in these categories have annual MRI plus annual mammogram, not MRI instead of mammogram.
The breast MRI procedure itself is different from a standard brain or spine MRI in a significant way: patients lie face-down on the MRI table with their breasts positioned inside padded openings in a specialized breast coil, rather than lying flat on their back as in most other MRI scans. This positioning allows the breasts to hang freely inside the coil without compression, which is better for imaging than lying on the breast.
The position feels unusual but shouldn't be painful. The table slides into the MRI machine, which is a large cylindrical tunnel — the same machine used for other body MRIs. The scan itself takes 30 to 60 minutes, during which the machine makes loud repetitive clicking and knocking sounds. Earplugs or headphones are typically provided.
Gadolinium contrast is injected through an intravenous line placed before the scan begins. The contrast injection happens partway through the scan sequence, after baseline (non-contrast) images are acquired. After injection, a series of contrast-enhanced images are acquired at intervals to capture the timing and degree of tissue enhancement.
Most patients don't feel the contrast injection beyond a brief cold sensation in the arm. Rarely, some patients experience nausea, warmth, or a metallic taste. Severe allergic reactions to gadolinium are uncommon but do occur — patients with prior contrast reactions, kidney disease, or gadolinium-related concerns should discuss this with their radiologist before the scan.
Patients with claustrophobia, back pain, or limited ability to lie face-down for extended periods sometimes find breast MRI uncomfortable. Unlike a head MRI where the patient's head enters the machine but the body is partially outside, most of the patient's upper body is inside the machine bore during a breast MRI.
Patients with significant claustrophobia may need an anxiolytic medication prescribed by their referring physician before the scan. Some facilities offer open-bore MRI machines with wider diameters that reduce claustrophobia, but these may produce lower image quality for breast MRI applications — discussing this option with the imaging center before the appointment establishes whether it's available and appropriate.
The breast MRI exam report is typically read by a breast imaging radiologist and communicated to the referring physician within 24 to 72 hours. Results are categorized using the ACR BI-RADS (Breast Imaging Reporting and Data System) scale, the same system used for mammography results. BI-RADS 1 and 2 are normal or benign findings. BI-RADS 3 is probably benign — short-interval follow-up imaging in 6 months is recommended.
BI-RADS 4 and 5 are suspicious and highly suggestive of malignancy respectively, and biopsy is recommended. BI-RADS 6 is used for a known cancer that has been biopsied. Most patients receive BI-RADS 1 or 2 results — the high false-positive rate associated with breast MRI does not mean most results are suspicious, only that compared to mammography, MRI triggers follow-up more often for the same population of cancers found.
After the scan, the radiologist reviews the images and writes a formal report using the BI-RADS classification system. The interpreting radiologist at a dedicated breast imaging center typically has more experience reading breast MRI than a general radiologist — for complex or high-risk cases, having the exam read at a center that performs high volumes of breast MRI is worth considering.
The radiologist's report uses standardized BI-RADS language that your referring physician or breast surgeon is trained to interpret. Asking your referring doctor to explain the specific findings and BI-RADS category at your follow-up appointment gives you a complete picture of what was seen and what the next steps are.
Breast MRI vs Mammogram
Breast MRI detects 75–90% of cancers present. Mammogram detects 70–85%. MRI is more sensitive, particularly in dense tissue and high-risk genetic carriers.
Breast MRI has a higher false-positive rate than mammography — more benign findings trigger follow-up imaging or biopsy. This is why MRI isn't used for routine average-risk screening.
Mammogram uses X-ray radiation (low dose). Breast MRI uses magnetic fields and radio waves — no radiation. Both require contrast for detailed views: mammogram uses compression, MRI uses injected gadolinium dye.
Mammogram: $100–$300, widely available. Breast MRI: $1,000–$3,000+, requires specialized equipment. Insurance coverage for screening MRI depends on documented risk factors.
Mammogram: average-risk women 40+, annual screening. Breast MRI: high-risk women (BRCA, 20%+ lifetime risk, dense tissue with added risk factors), annual supplemental screening.
Mammogram delivers a small dose of ionizing radiation (similar to a few days of background radiation). Breast MRI uses no ionizing radiation. For high-risk women who begin screening at 25–30, the lack of radiation in MRI is an advantage.
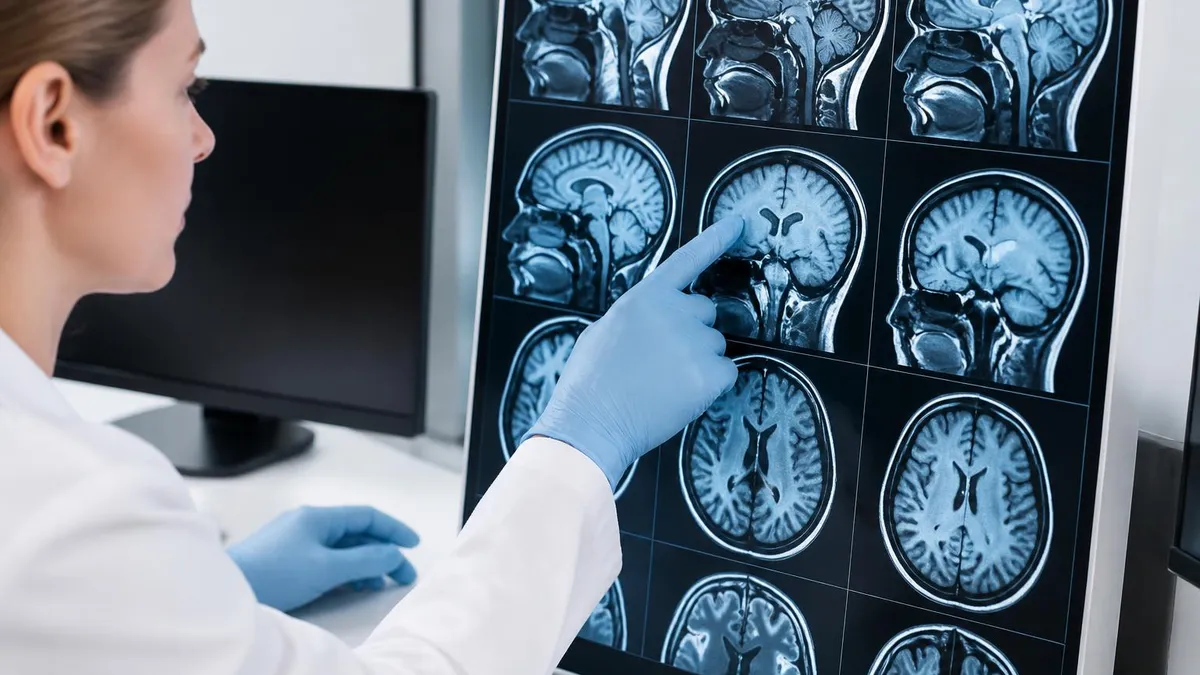
Insurance coverage for breast MRI depends heavily on the documented clinical indication. Most insurance plans, including Medicare and Medicaid, cover breast MRI when there is documented medical necessity — a BRCA mutation, a lifetime risk calculation above 20%, prior chest radiation, or a breast cancer diagnosis requiring staging. Coverage for supplemental screening in women with dense breast tissue but no other risk factors varies by plan and state.
Some states have enacted laws requiring coverage for supplemental screening in dense-tissue patients, while others leave coverage to plan-specific policies. Calling the insurance company to verify coverage and get a pre-authorization number before scheduling a breast MRI prevents unexpected bills for a procedure that may or may not be covered under your specific plan.
Preparing for a breast MRI involves a few specific steps that differ from other imaging procedures. Metallic implants, pacemakers, and certain orthopedic hardware may contraindicate MRI — the imaging center will screen for these before scheduling. All metal jewelry and accessories must be removed before the scan. For premenopausal women who are scheduled for high-risk screening (not diagnostic), the scan should be scheduled in the second week of the menstrual cycle (days 7–14) to minimize background enhancement from normal hormonal variation in breast tissue.
This timing window reduces the chance that normal hormonal enhancement is mistaken for suspicious enhancement. Scheduling the scan on the right cycle day requires planning ahead — many imaging centers request that the patient call when menstruation begins to schedule the appointment for day 7–14 of that cycle.
Silicone breast implants are well-visualized on MRI, and breast MRI is the standard imaging modality for evaluating suspected implant rupture. An intact implant appears as a smooth, complete shell on MRI. An intracapsular rupture — where the silicone stays within the fibrous capsule that the body forms around the implant — appears as the distinctive "linguine sign" where the implant shell is folded within the intact capsule. An extracapsular rupture — where silicone has leaked outside the capsule into surrounding tissue — is more serious and appears as irregular silicone signal in the breast tissue surrounding the implant.
The FDA has recommended that people with silicone gel-filled implants get a baseline MRI five to six years after implantation and every two to three years thereafter to screen for silent rupture, though compliance with this recommendation is low and insurance coverage is inconsistent. Patients with symptoms (firmness, shape change, pain) should request a diagnostic MRI rather than waiting for the scheduled screening interval.
The out-of-pocket cost for breast MRI without insurance coverage can reach several thousand dollars at hospital-based imaging centers. Free-standing imaging centers and radiology practices affiliated with academic medical centers often charge significantly less for the same procedure. Calling multiple imaging facilities in your area to compare facility fees, and checking whether your referral requires you to go to a specific in-network facility, can meaningfully reduce costs for patients without comprehensive insurance coverage. Some facilities offer payment plans or financial assistance programs for patients facing large out-of-pocket costs for medically necessary imaging.
Breast MRI Preparation Checklist
- ✓Verify insurance coverage and pre-authorization requirements before scheduling
- ✓Schedule in cycle days 7–14 if you're premenopausal and having screening (not diagnostic) MRI
- ✓Remove all metal jewelry, piercings, and accessories before the appointment
- ✓Inform the imaging center of any metallic implants, pacemakers, or prior metal injuries
- ✓Inform the radiologist of any prior gadolinium contrast reactions or kidney disease
- ✓Tell your referring doctor if you have significant claustrophobia — anxiolytic may be needed
- ✓Plan for 30–60 minutes for the scan plus check-in and IV placement time
- ✓Arrange transportation if you are taking an anxiolytic for claustrophobia
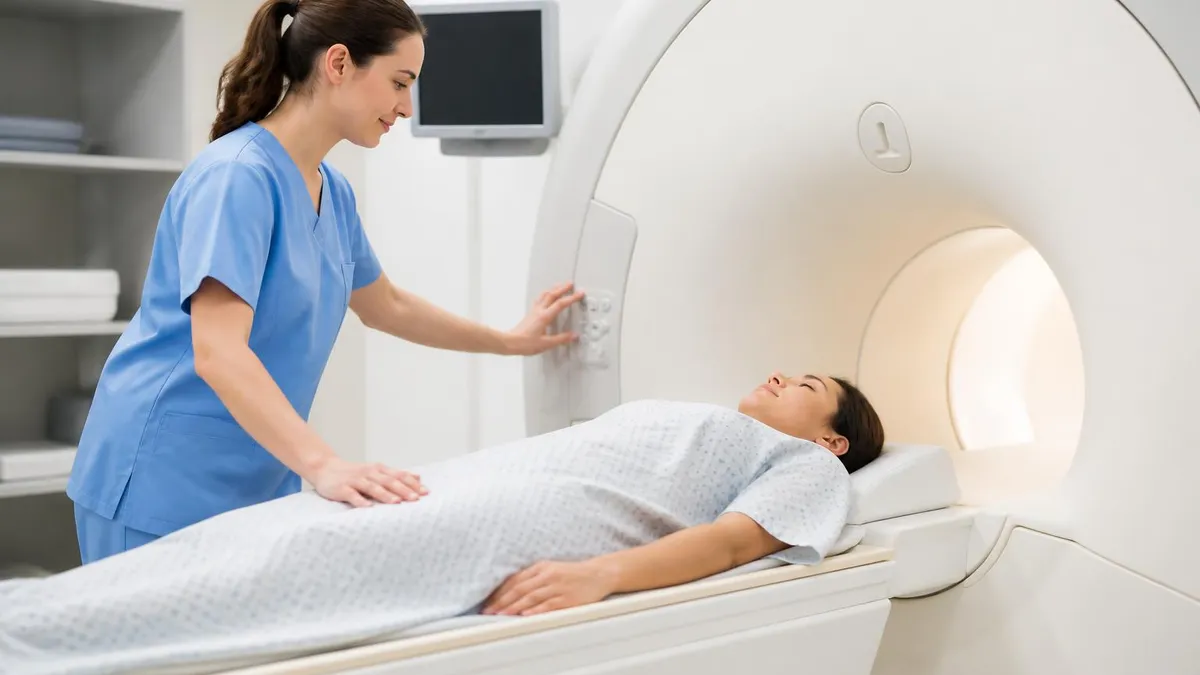
Breast MRI by Clinical Scenario
Women with BRCA1 or BRCA2 mutations, a lifetime risk estimated at 20% or greater by a validated model (Tyrer-Cuzick, BRCAPRO), prior chest radiation at ages 10–30, or a first-degree relative with a known BRCA mutation are recommended to have annual breast MRI supplementing annual mammography. High-risk screening typically begins at age 25–30 rather than waiting until 40. The annual MRI and mammogram are often scheduled 6 months apart to alternate imaging every 6 months throughout the year. Women who are uncertain about their risk level can be referred to a genetic counselor or a breast cancer risk assessment clinic for a formal risk calculation using standardized models.
Breast MRI: Benefits and Limitations
- +Higher sensitivity than mammogram — detects more cancers, especially in dense tissue
- +No ionizing radiation — advantageous for high-risk women who begin screening at a young age
- +Can evaluate implant integrity and detect silicone implant rupture not visible on other imaging
- +Excellent for evaluating disease extent before breast cancer surgery
- +Detects cancer in the opposite breast in newly diagnosed patients — can change surgical plan
- −Higher false-positive rate than mammogram — more follow-up imaging and biopsies for benign findings
- −Requires contrast dye injection — not appropriate for patients with gadolinium allergy or kidney disease
- −Expensive ($1,000–$3,000+) — insurance coverage depends on documented indication
- −Time-consuming — 30–60 minutes, face-down position in machine, claustrophobia is an issue for some
- −Not recommended for average-risk women — added sensitivity doesn't outweigh false-positive burden
Breast MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.