Cat Scan vs MRI: Key Differences and When Each Is Used
Cat scan vs MRI: learn how they differ in radiation, speed, cost, and image quality, and why doctors choose one over the other for different conditions.
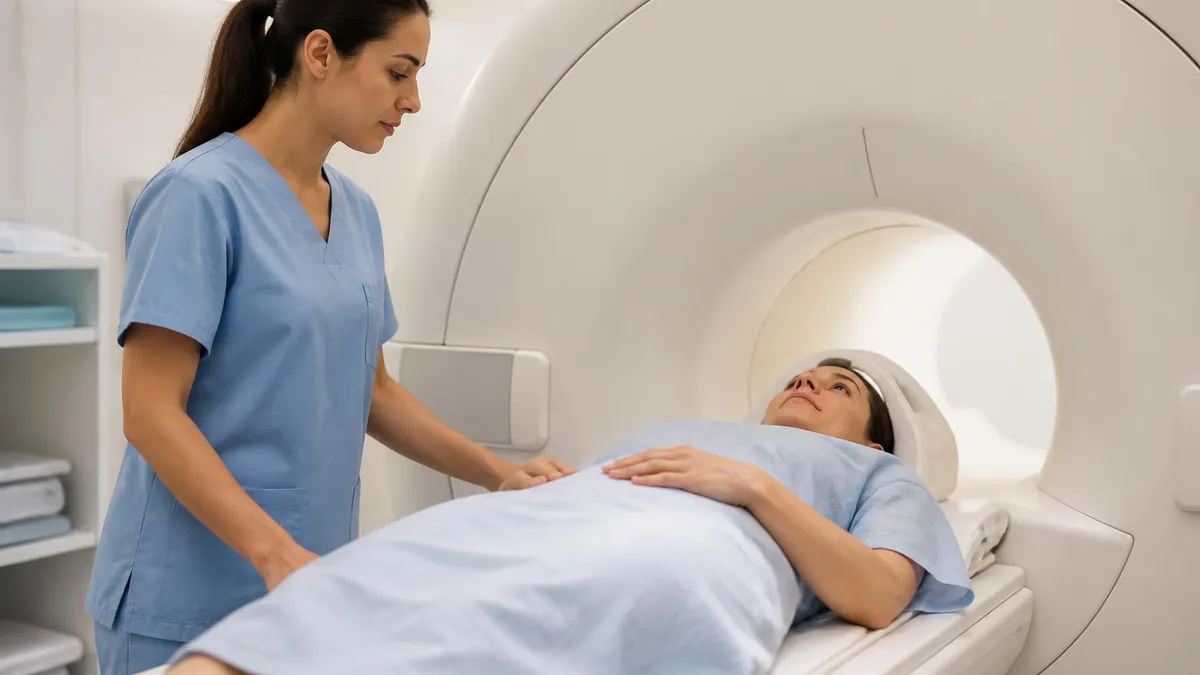
When your doctor orders imaging, the choice between a cat scan and an MRI isn't arbitrary — each technology captures different information, takes different amounts of time, and carries different considerations for your body. Understanding the distinction helps you know what to expect and why your physician chose one test over the other for your specific situation.
A cat scan, also called a CT scan (computed tomography), uses X-rays to create cross-sectional images of your internal structures. A detector array rotates around your body capturing multiple X-ray slices, and software reconstructs them into a three-dimensional picture. The entire scan typically finishes in five to ten minutes, making it the preferred choice when speed matters — emergencies, trauma workups, and rapid screening situations where time is critical.
An MRI scan — magnetic resonance imaging — works without any radiation at all. Instead, it uses a powerful magnetic field and radio waves to excite hydrogen atoms in your body's water and fat tissue. The way those atoms respond generates the signal that gets reconstructed into highly detailed images. MRI scans take longer (typically 30 to 60 minutes), but they produce exceptional soft tissue detail that CT simply can't match.
Both technologies produce cross-sectional 'slice' images of internal structures, which is why they're sometimes confused by patients. The critical difference lies in what they're measuring: CT measures X-ray absorption, while MRI measures the magnetic response of hydrogen protons. That fundamental difference shapes everything — image quality, scan time, appropriate use cases, cost, and whether you're exposed to ionizing radiation.
Neither scan is universally better. Radiologists and clinicians choose based on the clinical question, the body part involved, urgency, patient anatomy, and other medical factors. What looks like a routine preference is actually a carefully considered decision about which imaging modality best answers the diagnostic question at hand.
The decision isn't always straightforward, and patients sometimes receive different answers from different physicians about which scan is most appropriate. This reflects the genuine clinical judgment involved — not inconsistency. Two radiologists might recommend different modalities for the same clinical question if one has access to a faster MRI protocol or knows the patient has a metal implant. Your referring physician's experience and the equipment available at your imaging facility both influence the final choice.
Insurance authorization requirements also shape which scan gets ordered. Some insurers require a CT first before authorizing an MRI, even when the physician believes MRI is clinically superior for the indication. This step-therapy approach can delay diagnosis. If your doctor believes MRI is definitively appropriate for your situation, they can often submit a clinical appeal letter explaining the medical necessity. Patients who understand the difference between the scans are better positioned to ask informed questions if they receive an authorization denial for their preferred imaging.
Open MRI is an option for patients who experience severe claustrophobia in standard bore scanners. Open MRI machines have a more spacious design without the narrow tube, but typically operate at lower magnetic field strength (0.3T to 1.0T versus 1.5T or 3.0T for standard scanners). The lower field strength reduces image quality for some studies, but for many routine indications — spinal MRI, basic brain imaging, joint assessments — open MRI produces diagnostically adequate images while eliminating the confinement that makes standard MRI intolerable for claustrophobic patients.
CT Scan vs MRI at a Glance
CT technology was developed in the early 1970s and became standard in hospitals within a decade. The scanner looks like a large white ring, and the table slides you through the opening while the X-ray tube and detector array rotate around you. Modern multi-detector CT scanners complete a chest or abdominal scan in a single breath-hold — seconds of actual acquisition time, even if the whole appointment takes longer.
The images CT produces are particularly clear for dense structures: bone, calcifications, and calcified blood vessels show up in sharp contrast against surrounding tissue. CT is excellent for detecting bleeding in the brain, fractures, kidney stones, aortic aneurysms, and lung nodules. It also handles larger body areas more easily — a full-body CT can be completed in under a minute in a trauma bay.
MRI scanners look more imposing: a long tube with a narrow bore (the opening) that generates a magnetic field up to 60,000 times stronger than Earth's. You lie still inside the tube while the scanner produces a series of knocking or banging sounds — those are gradient coils switching on and off to generate the radio frequency pulses. The sounds are normal and expected, though earplugs or headphones are provided.
The magnetic field in an MRI is extremely strong, which is why ferromagnetic metal objects — certain implants, pacemakers, cochlear implants — can be contraindicated. Before scheduling an MRI, your care team will review your complete implant and surgical history. Most modern implants are MRI-safe or conditionally safe, but the safety review is non-negotiable. For patients with metal concerns, CT may be the only viable option even when MRI would otherwise be preferred.
Contrast agents can enhance either scan type. CT contrast uses iodine-based dyes injected intravenously to highlight blood vessels and tumors. MRI contrast uses gadolinium-based agents that also enhance vascular structures and areas of active inflammation or tumor growth. Both types of contrast carry small risks of allergic reaction and kidney stress, particularly in patients with pre-existing kidney disease.
The type of contrast used makes a meaningful difference in what the scan reveals. Intravenous iodine contrast for CT enhances blood vessels and areas where the blood-brain barrier is disrupted, helping identify active tumors, abscesses, and vascular malformations. The timing of the contrast injection matters as much as the contrast itself — arterial phase images (captured seconds after injection) show arteries at peak enhancement, while venous phase captures veins, and delayed phase images show tissue that traps contrast longer, which can indicate certain tumor types.
Gadolinium contrast for MRI works through a different mechanism. Gadolinium shortens the relaxation time of nearby hydrogen protons, making enhanced areas appear brighter on T1-weighted images. This enhancement pattern helps distinguish scar tissue from active tumor, identifies areas of active inflammation in multiple sclerosis plaques, and delineates abscesses from surrounding edema. Nephrogenic systemic fibrosis is a rare but serious risk of gadolinium in patients with severe kidney disease, so gadolinium is avoided or used cautiously when the creatinine level is significantly elevated.
Both contrast types can cause allergic reactions ranging from mild hives to severe anaphylaxis. Pre-medication with steroids and antihistamines significantly reduces reaction risk for patients with a prior contrast reaction. Inform your radiology team of any prior contrast reactions before your scan — this history directly influences whether premedication is prescribed and which contrast agent is selected for your procedure.
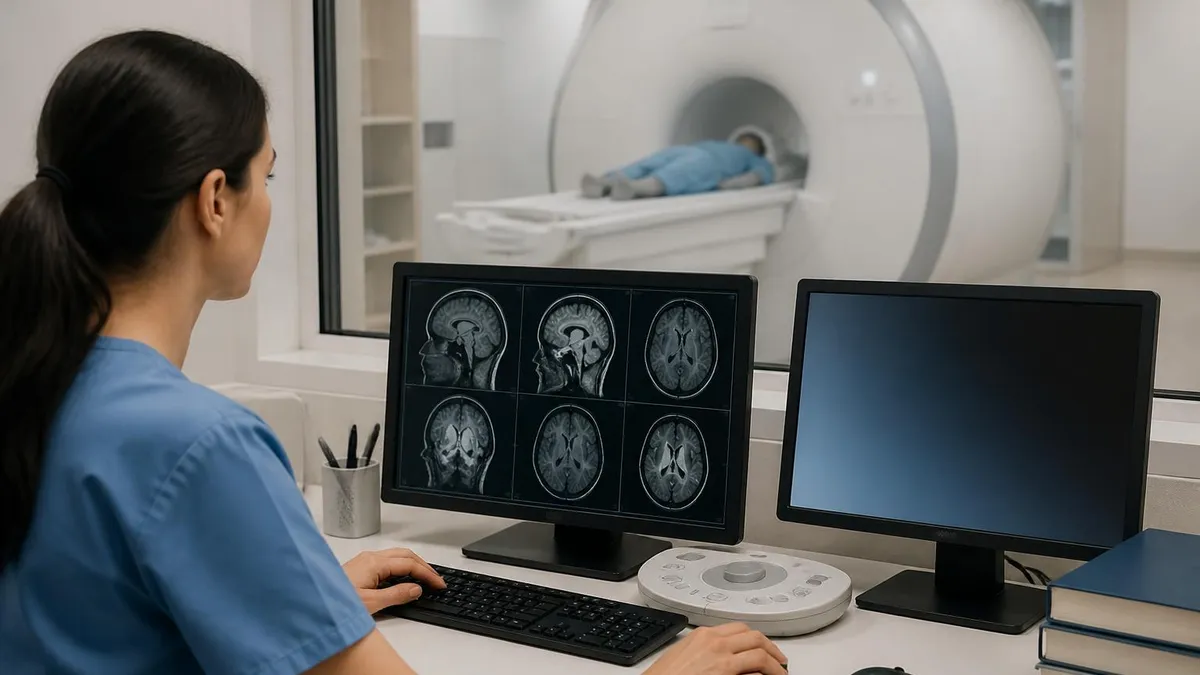
A CT scan of the abdomen delivers roughly 10 millisieverts (mSv) of radiation — equivalent to about three years of background environmental radiation. MRI delivers zero ionizing radiation. For young patients, repeated scans, or people with a cancer diagnosis requiring frequent monitoring, the radiation difference matters. MRI is generally preferred when equivalent or better imaging is available without radiation exposure.
CT is the go-to scan in emergency medicine. When a patient arrives after a car accident, the trauma team can have a complete internal injury assessment in under fifteen minutes using CT. The speed is simply unmatched — MRI requires the patient to lie perfectly still for thirty minutes or more, which isn't feasible for someone in acute distress or unable to cooperate.
Stroke evaluation often starts with CT. A non-contrast CT of the brain can quickly rule out hemorrhagic stroke (bleeding), which must be identified before blood-thinning treatment is given. If the CT shows no bleeding, physicians can proceed with treatment decisions. MRI gives more detail for ischemic stroke (blockage), but the urgency of ruling out bleeding first often makes CT the immediate first step in the evaluation chain.
Bone and joint injuries are another CT strength. The thin slices CT produces reveal subtle fractures that plain X-rays miss, including complex fractures of the wrist, ankle, spine, and facial bones. Before orthopedic surgery on a fractured bone, surgeons often want a CT to plan the exact hardware placement based on the fracture pattern in three dimensions.
Chest imaging for pneumonia, pulmonary embolism, and lung cancer screening all rely on CT. The lung tissue is mostly air, which creates natural contrast that CT captures well. MRI of the lungs is technically more difficult because lung tissue moves with breathing and has less water content than other organs, making the MRI signal weaker. For lung pathology, CT is almost always the preferred modality.
Kidney stone evaluation is virtually always done with CT. A low-dose non-contrast CT of the abdomen and pelvis identifies stones as small as 1 millimeter in any part of the urinary tract, with sensitivity that exceeds ultrasound and far exceeds plain X-ray. The scan takes under two minutes and gives the urologist precise information about stone size, location, and whether it's likely to pass on its own.
In oncology, CT is the standard imaging backbone for cancer staging and treatment monitoring. Most staging systems for lung, colon, liver, and lymphoma use CT findings to assign tumor, node, and metastasis (TNM) categories that guide treatment decisions. Response to chemotherapy is tracked with serial CT scans measuring whether tumors are shrinking, stable, or growing according to RECIST criteria.
The reproducibility of CT measurements from scan to scan — using the same scanner, the same protocol, and the same section thickness — is why it's been adopted as the standard for oncologic monitoring rather than MRI, despite MRI's superior soft tissue resolution.
Cardiac CT is a growing specialized application. Coronary CT angiography uses ultra-fast CT scanners to capture images of the coronary arteries without the invasive catheter required for traditional coronary angiography. Calcium scoring — a separate CT protocol — quantifies the amount of calcium in the coronary arteries as a proxy for plaque burden and cardiovascular risk. These applications have made CT the most important non-invasive tool in cardiology for detecting early coronary artery disease before it causes symptoms.
Radiation dose reduction in CT has improved dramatically over the past two decades. Iterative reconstruction algorithms, automatic exposure control, and organ-based dose modulation cut radiation doses by 40 to 80 percent compared to older protocols without sacrificing diagnostic image quality. The current low-dose chest CT protocol used for lung cancer screening delivers as little as 1.5 mSv — far less than early CT protocols.
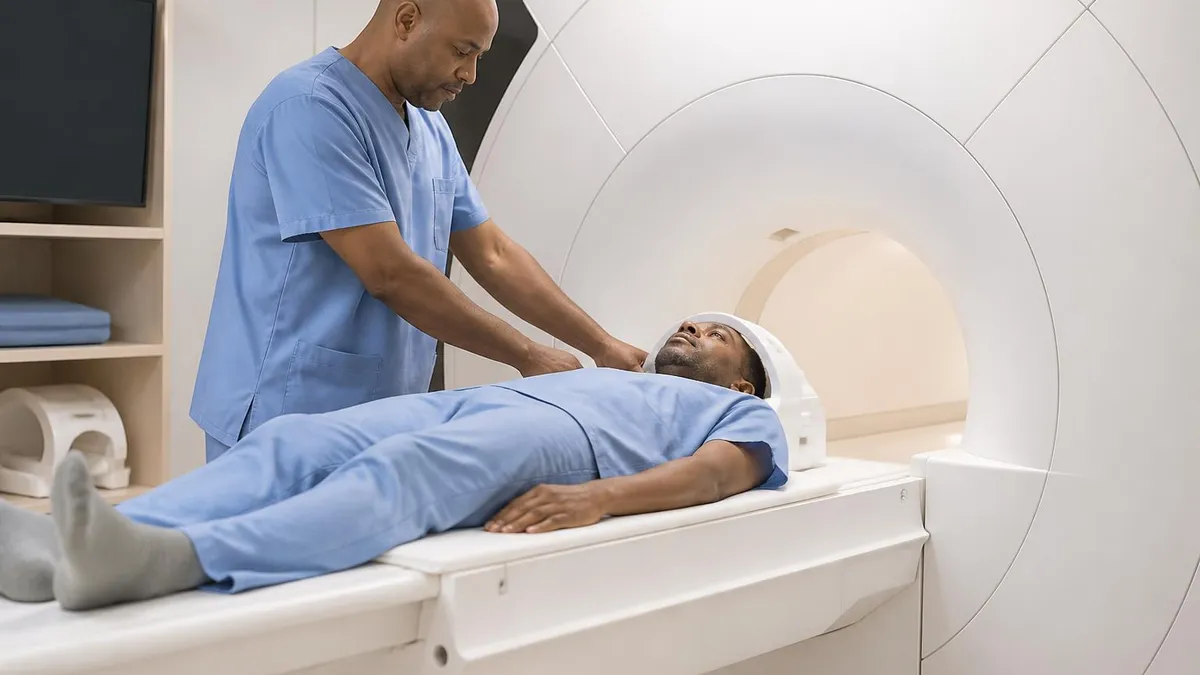
Which Scan Is Preferred by Condition
MRI preferred — superior soft tissue contrast, no radiation, multiplanar capability. CT used in emergencies or when MRI is contraindicated.
CT preferred — speed is critical. Full-body trauma CT in under 60 seconds. MRI too slow for acute emergency assessment.
MRI preferred — shows disc herniation, cord compression, and nerve root involvement with detail CT cannot match without myelography.
CT preferred (low-dose non-contrast) — detects stones as small as 1mm anywhere in the urinary tract with near-100% sensitivity.
MRI preferred — shows tendons, ligaments, cartilage, and menisci in detail. CT shows bone well but misses soft tissue injuries.
CT preferred — lung tissue creates natural contrast. Low-dose CT is the recommended annual screening method for high-risk patients.
MRI dominates for brain and spinal cord imaging in non-emergency settings. The soft tissue contrast MRI provides is dramatically better than CT for identifying tumors, demyelinating disease (like multiple sclerosis), small strokes in follow-up, and subtle abnormalities in the brain's white and gray matter. A neurologist evaluating a patient for MS or unexplained cognitive changes will almost always order MRI, not CT.
The spine is another MRI stronghold. A brain MRI of the cervical, thoracic, or lumbar spine shows the spinal cord, nerve roots, and intervertebral discs in a level of detail that CT cannot replicate without injecting contrast directly into the spinal canal. For back pain patients being evaluated for herniated discs, spinal stenosis, or nerve compression, MRI is the standard imaging choice before surgical or interventional treatment planning.
Musculoskeletal imaging for sports injuries and joint pain almost always means MRI. Torn ACLs, rotator cuff tears, meniscus damage, cartilage defects, and tendon pathology all show clearly on MRI while remaining invisible or poorly defined on CT. Orthopedic surgeons rely on MRI for pre-operative planning for these injuries because it tells them exactly which structures are damaged and how severely.
Prostate, uterine, and rectal cancer staging benefit significantly from MRI. The pelvic organs are surrounded by fat that provides excellent natural contrast on MRI, allowing radiologists to define tumor margins and assess whether cancer has spread to adjacent structures. CT is used for these cancers too — particularly to check lymph nodes and distant spread to the liver and lungs — but MRI provides the local staging detail that guides surgical and radiation planning.
For pediatric patients, MRI is strongly preferred whenever the clinical question can wait for the longer scan time. Children's tissues are more sensitive to radiation than adults', and cumulative exposure through a childhood of CT scans adds meaningful risk. Pediatric hospitals have developed MRI protocols specifically designed to minimize anesthesia requirements for young children who can't remain still.
Functional MRI (fMRI) is a specialized MRI technique that measures blood flow changes associated with brain activity. Neurosurgeons use fMRI before brain tumor surgery to map eloquent cortex — the brain regions responsible for speech, motor function, and language — to minimize the risk of post-surgical deficits. Research applications of fMRI have fundamentally changed our understanding of how the brain processes information and responds to disease. This capability doesn't exist in CT, which is structurally informative but cannot directly map brain function.
Diffusion-weighted MRI (DWI) is a sequence that detects the movement of water molecules in tissue. Restricted diffusion — where water can't move freely — appears bright on DWI and indicates early ischemic stroke (as early as minutes after symptom onset), abscess formation, and certain tumor types. DWI has transformed acute stroke imaging, allowing physicians to identify the volume of infarcted brain tissue before it becomes visible on standard MRI or CT. This early identification directly guides decisions about aggressive reperfusion therapy in stroke centers.
Whole-body MRI is an emerging technique for cancer staging, particularly for multiple myeloma and certain metastatic cancers. Rather than multiple separate scans, whole-body MRI captures the entire skeleton and soft tissues in a single session. For conditions that spread throughout bone marrow — which CT often underestimates — whole-body MRI provides superior staging accuracy and is increasingly recommended in international guidelines over traditional CT-bone scan combinations.
Questions to Ask Before Your Scan
- ✓Why was this scan type chosen over the alternative?
- ✓Will contrast be used, and what are the risks given my kidney function?
- ✓Do I have any metal implants that need to be reviewed before an MRI?
- ✓How long will the scan take, and will I need to hold still throughout?
- ✓Will I receive the images and report, or only a summary?
- ✓Is this scan covered by my insurance, and what is my estimated out-of-pocket cost?
- ✓Are there lower-radiation alternatives if a CT is ordered for a non-emergency?
- ✓If I'm claustrophobic, is an open MRI or sedation an option?
CT vs MRI: Detailed Comparison
Uses ionizing X-ray radiation. Scan time 5–10 minutes. Best for bone, calcifications, bleeding, lung, kidneys, and emergency trauma. Contrast uses iodine-based dye. More widely available than MRI, including in smaller hospitals and urgent care facilities. Lower cost on average. Not suitable for pregnant women in non-emergencies due to radiation. Loud machine hum but no confinement issues for most patients.
CT Scan vs MRI: Tradeoffs
- +CT is faster — critical advantage in emergencies and trauma
- +CT is more available — more facilities own CT scanners than MRI machines
- +CT is lower cost on average across most body regions
- +CT handles large body areas efficiently in a single scan
- +MRI delivers superior soft tissue detail with zero radiation exposure
- +MRI is preferred for pediatric imaging to avoid cumulative radiation
- −CT delivers ionizing radiation — concern for repeated scans and children
- −CT has lower soft tissue contrast than MRI for brain, spine, and joints
- −MRI takes 3–6 times longer than CT — not suitable for uncooperative patients
- −MRI is contraindicated for some metal implants and devices
- −MRI causes claustrophobia issues in some patients
- −MRI is typically more expensive than CT for comparable body regions
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.