What Does an MRI Show? Brain, Spine, and Soft Tissue Guide
MRI scans reveal soft tissue, brain structures, spinal discs, and torn ligaments. Learn exactly what MRI imaging shows by body part and when doctors order it.
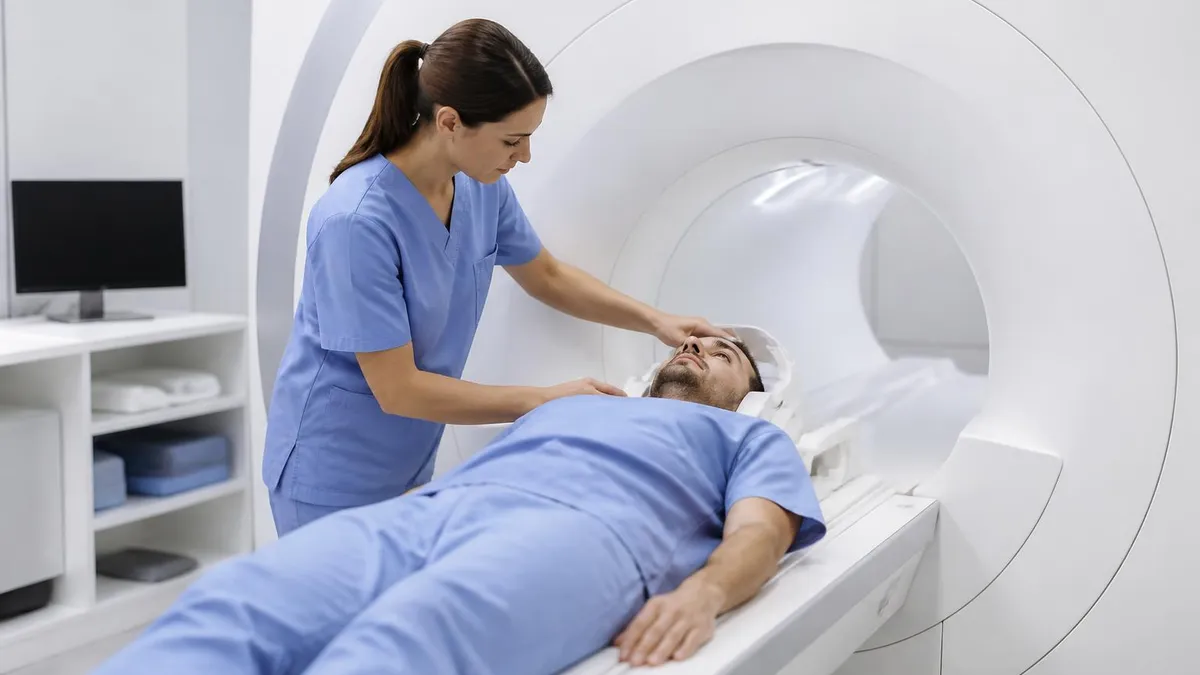
What Does an MRI Show?
An MRI (magnetic resonance imaging) scan uses powerful magnetic fields and radio waves to produce detailed images of the body's internal structures. Unlike X-rays and CT scans, which use ionising radiation and excel at imaging dense tissue like bone, MRI is uniquely suited to visualising soft tissue — the structures that X-rays largely pass through without capturing. This makes MRI the imaging modality of choice for diagnosing conditions affecting the brain, spinal cord, nerves, muscles, tendons, ligaments, and organs.
What an MRI shows depends almost entirely on where the scan is focused and what the ordering physician is looking for. An MRI of the brain looks for very different things than an MRI of the knee — the technology is the same, but the structures under examination, the relevant pathologies, and the scan protocols all change by body region. When your doctor orders an MRI, they specify both the body part and often the specific protocol (with or without contrast, specific sequences) based on the clinical question they're trying to answer.
Understanding what an MRI can and can't show helps you make sense of your radiologist's report, ask better questions during follow-up appointments, and understand why your doctor ordered this specific test rather than an alternative. MRI is not the right tool for every diagnostic question — sometimes CT, X-ray, or ultrasound is more appropriate — and knowing the difference reduces anxiety about the testing process and helps you engage meaningfully with your care team.
- Best at: Soft tissue — brain, spinal cord, nerves, muscles, tendons, ligaments, cartilage, organs (especially liver, prostate, uterus)
- Good at: Detecting inflammation, infection, tumours, bleeding, and structural abnormalities in most body regions
- Weaker at: Fine bone detail (CT is better), lung tissue (CT is better), rapidly changing processes requiring speed
- With contrast: Gadolinium contrast enhances blood vessels and active lesions — useful for detecting tumours, active inflammation, and infection
- Without contrast: Still highly detailed — contrast is added only when specific information is needed, not routinely for all scans
- No radiation: MRI uses magnetic fields and radio waves, not X-rays — making it preferable for repeated imaging and for populations sensitive to radiation
How Doctors Interpret MRI Results
Radiologist reviews the images
The radiologist writes a report
Your ordering doctor interprets the report in clinical context
Follow-up decisions are made
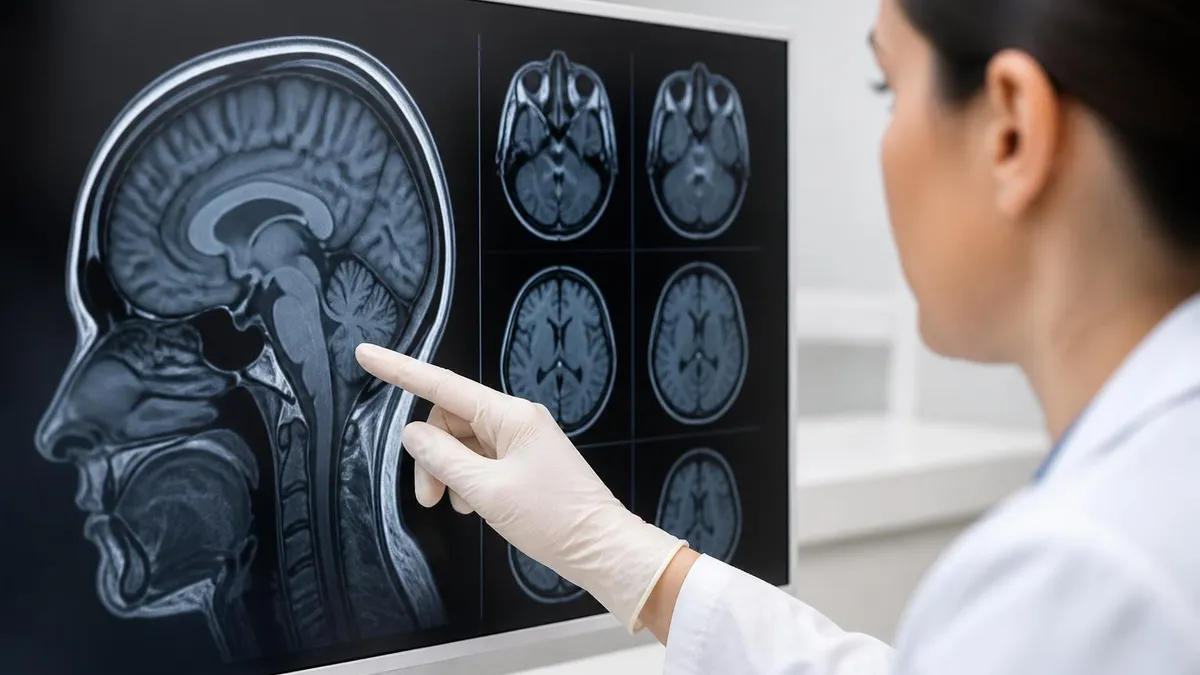
What Does an MRI of the Brain Show?
Brain MRI is one of the most frequently ordered MRI examinations, and it can reveal a wide range of structural and pathological findings. The brain's complex architecture — grey matter, white matter, ventricles, cerebellum, brainstem, blood vessels — is visualised in high detail because of MRI's sensitivity to the subtle differences in water content and tissue composition that distinguish these structures.
Tumours and masses. Brain MRI can detect primary brain tumours (gliomas, meningiomas, acoustic neuromas) and metastatic tumours that have spread from cancer elsewhere in the body. Contrast-enhanced MRI is particularly useful here — gadolinium contrast highlights areas where the blood-brain barrier is disrupted, which is a hallmark of most tumours. The size, location, and enhancement pattern of a mass helps radiologists distinguish between tumour types and guide biopsy or treatment planning.
Stroke and ischaemia. MRI — specifically diffusion-weighted imaging (DWI) sequences — can detect acute ischaemic stroke within minutes of onset. DWI identifies areas where water diffusion is restricted, which occurs when brain cells begin to die from lack of oxygen. This makes brain MRI critical in the acute stroke setting. Older strokes (areas of prior infarction) appear as bright spots on certain MRI sequences and help clinicians understand the history of cerebrovascular events even without prior imaging.
White matter disease and demyelination. Conditions like multiple sclerosis (MS) cause characteristic lesions in the white matter — the myelin-rich areas that connect different brain regions. These appear as bright spots on T2-weighted MRI sequences and follow specific patterns that help neurologists diagnose MS, differentiate it from similar conditions, and monitor disease progression over time. Brain MRI is the primary tool for tracking MS activity and response to treatment.
Bleeding and haemorrhage. Different types of intracranial bleeding — subdural haematoma, epidural haematoma, subarachnoid haemorrhage, intracerebral haemorrhage — have distinctive appearances on MRI depending on how old the blood is. MRI can detect bleeding that occurred days to weeks earlier, whereas very acute bleeding (within the first few hours) is sometimes more clearly shown on CT, which is why CT is typically the first-line scan in head trauma emergencies.
Brain atrophy and structural changes. MRI provides detailed views of brain volume, which allows clinicians to assess age-related atrophy, identify patterns associated with specific dementias (Alzheimer's disease shows characteristic hippocampal atrophy), and monitor changes over time. Structural brain MRI is a key component of workups for memory problems, dementia, and neuropsychiatric conditions.
MRI by Body Region: Key Findings
Shows intervertebral disc herniations, spinal cord compression, nerve root impingement, vertebral fractures, infections (discitis/osteomyelitis), tumours involving the vertebrae or spinal cord, and degenerative changes including stenosis. Essential for diagnosing the cause of back pain, radiculopathy (shooting pain down arms or legs), and numbness or weakness that suggests nerve involvement.
Reveals tears in the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial and lateral menisci, and collateral ligaments. Also shows articular cartilage damage, bone bruising (bone marrow oedema), and effusions. The standard pre-surgical imaging for knee injuries in athletes and patients considering arthroscopic repair.
Identifies rotator cuff tears (partial and full thickness), labral tears (SLAP tears, Bankart lesions), biceps tendon pathology, bursitis, and AC joint problems. Shoulder MRI with contrast injected directly into the joint (MR arthrography) provides superior visualisation of labral tears compared to standard MRI.
Shows liver lesions (distinguishing benign cysts from tumours), biliary system abnormalities, pancreatic conditions, adrenal masses, kidney lesions, uterine fibroids, ovarian masses, and prostate cancer staging. Frequently used when CT findings are ambiguous or when radiation exposure needs to be minimised for repeated imaging.
MRI With vs Without Contrast
Most MRI scans are performed without contrast as the first-line approach. Non-contrast MRI provides excellent detail for:
- Structural anatomy: Brain structure, spinal cord, disc herniations, ligament and tendon tears, cartilage damage — all clearly visible without contrast
- Diffusion-weighted imaging (DWI): Acute stroke detection does not require contrast
- FLAIR sequences: White matter lesions, perivascular spaces, and cortical abnormalities visible without contrast
- Musculoskeletal imaging: Most joint and soft tissue injuries are adequately assessed without contrast
- Patients with kidney disease: Gadolinium contrast is contraindicated in severe renal impairment due to risk of nephrogenic systemic fibrosis — non-contrast MRI is the standard for these patients
- Cost and time: Non-contrast studies are shorter and less expensive than contrast-enhanced studies
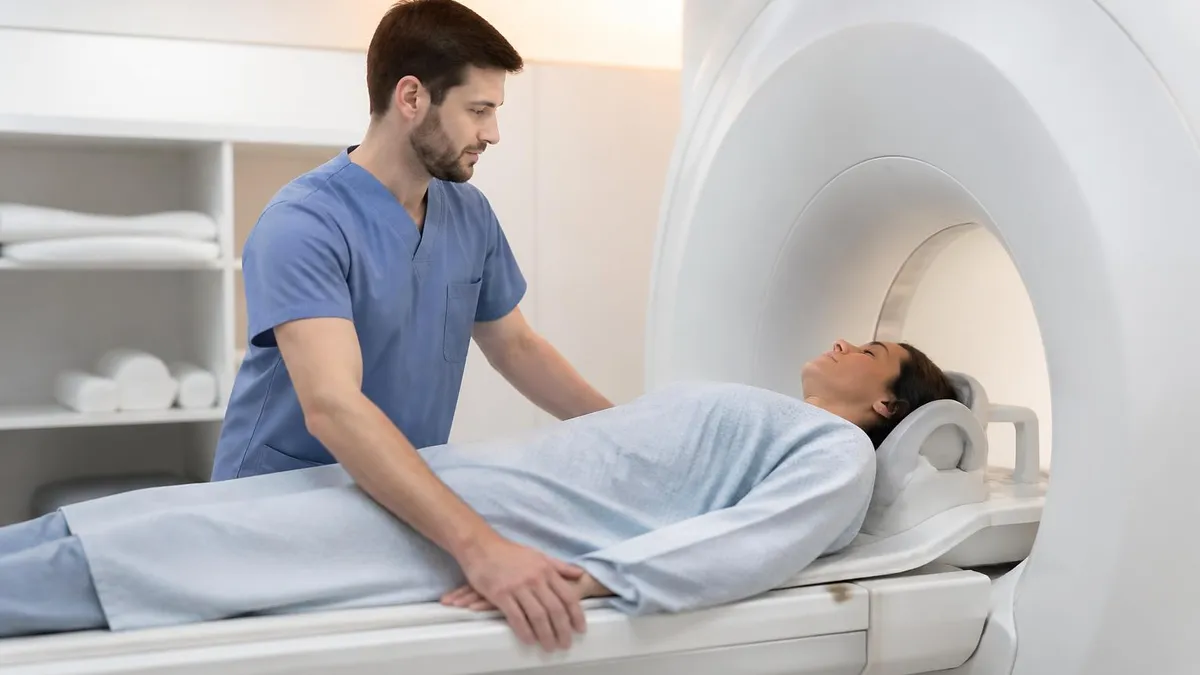
What Does an MRI of the Spine Show?
Spinal MRI is one of the most commonly ordered imaging studies for musculoskeletal and neurological complaints. The spine is a complex structure — vertebrae, intervertebral discs, the spinal cord itself, nerve roots exiting at each level, and the surrounding soft tissue — and MRI can evaluate all of these components in a single examination.
Disc herniations and degeneration. A herniated disc occurs when the inner portion (nucleus pulposus) of an intervertebral disc bulges or ruptures through the outer ring (annulus fibrosus) and impinges on a nerve root or the spinal cord. MRI shows the exact location and severity of herniations — distinguishing between a minor bulge, a moderate protrusion, and a large extrusion that's compressing neural structures. This distinction directly guides treatment decisions: mild herniations may respond to physical therapy, while severe compressions may require surgical consideration.
Spinal stenosis. Stenosis refers to narrowing of the spinal canal or the lateral recesses through which nerve roots exit. MRI provides direct visualisation of the degree of narrowing and whether neural structures are being compressed. Lumbar spinal stenosis — a common condition in older adults — typically causes leg pain and weakness with walking (neurogenic claudication), and MRI findings guide both non-surgical and surgical management.
Spinal cord pathology. For patients with symptoms suggesting spinal cord involvement — weakness, loss of coordination, bladder/bowel dysfunction — MRI is essential for evaluating the cord itself. Multiple sclerosis lesions within the spinal cord, cord compression from a large disc herniation or tumour, syrinxes (fluid-filled cavities within the cord), and inflammatory conditions like transverse myelitis all require spinal cord MRI for diagnosis and monitoring.
Infection and malignancy. Discitis (infection of the disc space) and osteomyelitis (infection of the vertebral bone) cause characteristic signal changes on MRI that appear before bone changes are visible on X-ray. Spinal metastases — vertebral involvement from cancers including lung, breast, prostate, and kidney — can cause vertebral collapse and cord compression that MRI identifies early enough to guide preventive treatment.
When Doctors Order MRI: Common Clinical Indications
- ✓Neurological symptoms — numbness, weakness, tingling in extremities suggesting nerve root or spinal cord involvement
- ✓Back or neck pain with radiculopathy (pain radiating into the arm or leg) that hasn't responded to conservative treatment
- ✓Suspected brain tumour, stroke, or other intracranial pathology based on symptoms or neurological examination findings
- ✓Multiple sclerosis diagnosis or disease monitoring — MRI is the primary tool for tracking MS lesion burden
- ✓Musculoskeletal injury — ACL tear, meniscal tear, rotator cuff tear, other soft tissue injuries in athletes or trauma patients
- ✓Cancer staging or monitoring — detecting metastases, assessing tumour response to treatment, evaluating post-treatment changes
- ✓Abdominal or pelvic organ evaluation when CT findings are inconclusive or when radiation minimisation is important
- ✓Evaluation of unexplained symptoms (seizures, headaches, vision changes, balance problems) requiring intracranial assessment
MRI vs CT Scan: Which Is Better?
- +MRI excels at soft tissue contrast — brain, nerves, muscles, tendons, cartilage, and solid organs are imaged with superior detail compared to CT
- +No ionising radiation — MRI is preferable for repeated imaging, for younger patients, and in clinical situations where cumulative radiation dose matters
- +Multi-planar imaging — MRI produces high-quality images in any plane (axial, coronal, sagittal) without repositioning the patient or increasing dose
- +Functional information — advanced MRI sequences (functional MRI, diffusion tensor imaging) provide information about brain activity and white matter connectivity not available with CT
- −CT is faster — a chest CT takes seconds; a brain MRI takes 20–45 minutes. For acute emergencies (stroke, trauma, PE), CT is often the first-line study because speed matters
- −CT shows bone better — fine cortical bone detail, fracture lines, and calcifications are more clearly depicted on CT than on standard MRI sequences
- −MRI contraindications — patients with certain implanted metal devices (older pacemakers, cochlear implants, some surgical clips) cannot safely undergo MRI; CT has no such limitation
- −MRI is more expensive and less widely available than CT in many settings, particularly in emergency and rural environments
Understanding Your MRI Report
MRI reports are written for ordering physicians, not patients — the terminology is technical, the descriptions assume anatomical knowledge, and findings are reported in a standardised format that can feel clinical and impersonal. Understanding the basic structure and terminology of an MRI report helps you engage more productively with your doctor and reduces the anxiety that comes from reading findings without context.
The technique section describes how the scan was performed: the field strength of the magnet (typically 1.5 Tesla or 3 Tesla — stronger magnets provide higher resolution), which body parts were scanned, what sequences were used, and whether contrast was given. This section tells you the quality and scope of the information available for interpretation.
The findings section is the core of the report. The radiologist describes each structure they examined — often systematically working through the anatomy. They note size, signal characteristics, and anything that deviates from expected normal appearances. Terms like 'hyperintense' (brighter than surrounding tissue on a specific sequence), 'hypointense' (darker), 'enhancing' (takes up contrast), and 'unremarkable' (appears normal) are standard radiological vocabulary. 'Incidental finding' refers to something noted that wasn't the reason for the scan and may or may not require clinical attention.
The impression section summarises the radiologist's conclusions — this is the section your doctor focuses on most. If significant pathology was identified, it's characterised here with differential diagnoses and recommendations. 'No acute intracranial abnormality' or 'no significant interval change' are common reassuring conclusions when the scan was ordered to rule out concerning pathology.
A key concept for patients reading their own reports is that radiologists describe everything they see — including anatomical variants, age-related changes, and minor findings that may have no clinical significance. A report with multiple findings does not necessarily mean multiple problems. Your ordering physician knows which findings are clinically relevant to your symptoms and which are incidental background findings that don't require action. Always discuss your results with your doctor rather than interpreting the radiologist's report in isolation.
Incidental findings deserve specific mention because they cause disproportionate patient anxiety. An incidental finding is something the radiologist noticed that wasn't the reason for the scan — a small cyst in the liver, a slightly enlarged lymph node, a benign-appearing lesion in bone. These are common in any large imaging study; one analysis found that roughly 40% of body MRI studies contain at least one incidental finding.
The vast majority require no intervention — the radiologist will typically characterise them as 'likely benign' or 'no suspicious features' and recommend routine follow-up imaging if they're large enough to warrant monitoring. Receiving a report with incidental findings doesn't mean something is seriously wrong; it means the scan was thorough enough to capture the full picture of your anatomy at that moment in time.
MRI by the Numbers
What MRI Cannot Show
MRI is a powerful diagnostic tool, but it has real limitations that affect when and why doctors choose alternative imaging modalities. Understanding what MRI doesn't show well helps explain why you might be sent for a CT scan, X-ray, or ultrasound rather than — or in addition to — an MRI.
Fine bone detail. MRI shows bone marrow, bone oedema (bruising), and large structural abnormalities well, but the fine cortical detail of fracture lines, small bone chips, and calcifications within soft tissues is better captured by CT. In trauma settings, CT is typically the first study for evaluating complex fractures of the skull, spine, pelvis, or extremities because of its speed, accuracy for bony injury, and the ability to reformat images in any plane.
Lung parenchyma. The lungs are mostly air, and air produces very little MRI signal — making MRI poorly suited for detecting lung nodules, consolidation, or other pulmonary pathology. CT is the gold standard for chest imaging, able to detect nodules as small as 1–2mm with high sensitivity. MRI is occasionally used for specific lung applications (cardiac MRI includes views of the adjacent lung bases) but is not used for routine pulmonary evaluation.
Calcium and calcification. Calcifications in soft tissue — phleboliths in blood vessels, calcified lymph nodes, calcium deposits in tendon pathology — appear as dark areas on MRI, making them easy to overlook or mischaracterise. CT and X-ray both show calcium clearly as bright, dense structures. When characterising calcifications is clinically important (such as distinguishing benign from malignant calcifications in the breast), X-ray mammography or CT is preferred.
Implanted metal and pacemakers. Ferromagnetic metals can be moved by MRI's magnetic field, heating can occur in conductive metal implants, and device function can be disrupted — making standard MRI contraindicated for patients with older pacemakers, cochlear implants, and some surgical clips and joint prostheses. MRI-conditional devices (designed to be compatible with MRI under specific conditions) are increasingly common, and many patients with newer implants can be safely scanned under specific protocols. But when implant compatibility is uncertain, CT provides the clinical information without the safety concerns.
Before every MRI, you must disclose all metal implants, devices, and prior surgeries — even if you've had MRI before. This includes pacemakers and cardiac rhythm devices, cochlear implants, neurostimulators, surgical clips (especially intracranial aneurysm clips), joint replacements and orthopaedic hardware, shrapnel or metal fragments from work or military service, and intrauterine devices (most are MRI-safe but should be disclosed). Some older implants are contraindicated for MRI; many newer ones are MRI-conditional and can be scanned under specific protocols. Tattoos with metallic pigments and permanent makeup can cause skin irritation during MRI. Pregnancy (especially first trimester) is a relative consideration — MRI is generally avoided unless the clinical benefit outweighs theoretical risk. Always complete the safety screening form honestly and completely, and tell the technologist about any implants even if they're not on the form.
Most MRI scans require you to remove all metal before entering the scanner room — jewellery, piercings, hearing aids, hairpins, and glasses. You'll change into a hospital gown if your clothing has any metal hardware (zips, underwire). Secure lockers are provided for valuables. For abdominal and pelvic MRI, you may be asked to fast for four to six hours beforehand to improve image quality by reducing bowel motion — your imaging facility will send specific preparation instructions if fasting is needed.
During the scan, you'll lie on a table that slides into the MRI machine — a large cylindrical magnet. The machine produces loud knocking and banging sounds as the magnetic gradients switch on and off — earplugs or headphones are provided. You'll be given a hand-held squeeze bulb to signal the technologist if you need to stop. The key requirement is to remain as still as possible throughout the scan; movement blurs MRI images significantly, which can necessitate repeating sequences and extending the total scan time.
Claustrophobia is a real concern for some patients, particularly in closed-bore (traditional tunnel-style) MRI machines. Strategies that help include requesting a mild sedative from your ordering doctor before the appointment, choosing an open MRI scanner (lower field strength but no enclosed tunnel), or asking the technologist to position you feet-first rather than head-first when the area being scanned allows it. Communication with your imaging facility before the appointment is the most effective way to ensure a manageable experience if you have anxiety about enclosed spaces.
After the scan, you can resume normal activities immediately — MRI has no recovery period and no radiation-related precautions. If contrast was given, staying well-hydrated for the rest of the day helps your kidneys clear the gadolinium efficiently. The technologist cannot tell you what the images show — result communication is the responsibility of your ordering physician.
If your doctor's office hasn't contacted you within the expected timeframe, calling to follow up is appropriate; results occasionally fall through communication gaps in busy practices. Accessing your results through a patient portal before speaking with your doctor is common now, but reading an MRI report without clinical context can cause unnecessary worry — try to wait for your physician's interpretation before drawing conclusions about what the findings mean for your health.
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.