MRI Cost: What You Pay With and Without Insurance in 2026
MRI cost ranges from $400 to $3,500 depending on body part, location, and insurance. Learn what drives MRI prices and how to pay less for your scan.
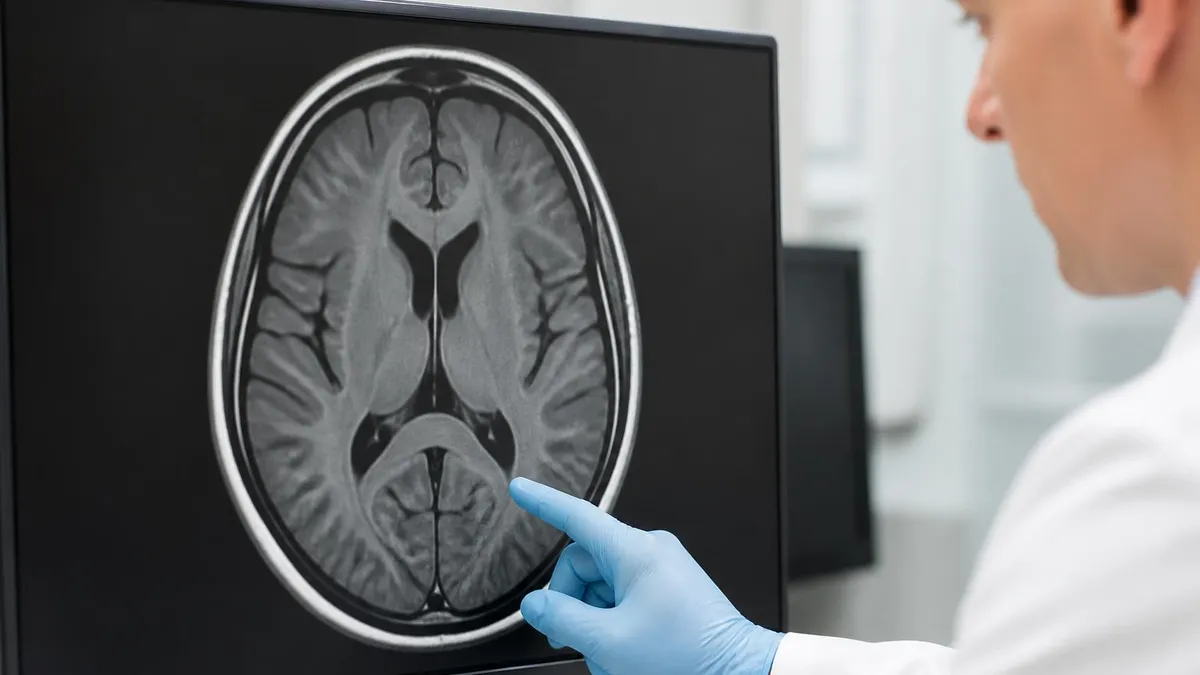
An MRI can cost anywhere from $400 to $3,500 out of pocket depending on where you get it, what body part is scanned, and whether contrast dye is used. With insurance, the patient's share depends on your deductible, copay, and whether the facility is in-network. Understanding what drives MRI pricing helps you make decisions that can save hundreds or even thousands of dollars without compromising on diagnostic quality.
MRI is expensive because the equipment is expensive. A clinical MRI machine costs $1 million to $3 million to purchase, requires dedicated shielded space, consumes substantial electricity, and needs licensed MRI technologists to operate and radiologists to interpret. Facilities amortize these costs across every scan they perform, which is why standalone imaging centers — which have lower overhead than hospitals — consistently charge less for the same scan on comparable equipment.
Hospital outpatient imaging departments routinely charge two to three times the rate of freestanding imaging centers for identical MRI studies. A brain MRI that costs $600 at a standalone radiology center might be billed at $1,500 to $2,000 at a hospital outpatient department. If your insurance requires a referral but does not require a specific facility, asking your physician whether a standalone imaging center is appropriate is worth the conversation. In many cases the answer is yes, and the difference in cost — even after insurance — is significant.
Insurance coverage for MRI is generally good when the scan is ordered by a physician for a medically necessary reason, but prior authorization requirements have expanded significantly. Most commercial insurers require prior authorization for MRI, meaning the ordering physician must submit documentation of medical necessity before the scan is approved.
Failure to obtain prior authorization when required results in the claim being denied even if the MRI was clinically appropriate. Always confirm authorization status with your insurer or physician's office before scheduling. For a broader overview of diagnostic imaging choices and costs, see the mri cost comparison guide that covers when CT versus MRI is more appropriate clinically and financially.
Emergency MRI outside normal business hours carries premium pricing at most facilities, both due to staffing costs and because patients in acute situations have limited ability to comparison shop. Inpatient MRIs (performed while admitted to a hospital) are typically included in the facility's daily room rate or DRG bundled payment rather than billed separately to the patient, which means the cost structure is completely different from outpatient imaging. If you are hospitalized and your physician orders an MRI, the billing will show up as part of the inpatient stay rather than a separate radiology bill in most cases.
Annual growth in the volume of MRI scans performed in the US has continued steadily for two decades as the technology becomes more accessible and clinical guidelines expand its appropriate use cases. This growth has paradoxically contributed to keeping prices higher in some markets by increasing demand faster than new equipment can be deployed. In markets where MRI capacity is constrained, scheduling wait times for non-urgent studies can extend to several weeks, which is worth factoring into your care timing if the clinical situation allows flexibility.
Average MRI Costs in the US
Body part is the primary driver of MRI cost variation. Simple joint scans — knee, ankle, shoulder, wrist — are typically at the lower end because the anatomy is contained and scans run 20 to 30 minutes.
Spinal MRIs vary by region: cervical spine (neck), thoracic spine (mid-back), and lumbar spine (lower back) are usually priced separately, and patients ordered a full spine scan may receive three separate bills or one combined charge depending on how the order is written. Brain MRIs are moderate in cost; cardiac MRIs and full-body scans are at the upper end because of longer scan times and specialized post-processing.
Contrast versus non-contrast significantly affects both clinical utility and cost. Gadolinium-based contrast agents are injected through an IV during the scan to enhance visualization of certain tissues — tumors, blood vessel abnormalities, inflammation, and infection. Contrast studies cost $100 to $400 more than non-contrast depending on the facility.
Not all MRI indications require contrast — a knee MRI for sports injury evaluation is almost always done without contrast, while a brain MRI evaluating for tumor, infection, or multiple sclerosis plaques will typically use contrast. Your ordering physician specifies with or without contrast on the order; if you're uncertain which was ordered, ask before arrival to avoid billing surprises.
Geographic location creates substantial price variation. Major metropolitan markets on the coasts tend to have both higher list prices and more competitive alternatives — freestanding centers compete on price because they're operating in dense markets. Rural areas often have a single facility option, reducing price competition and sometimes inflating costs. States with more MRI capacity per capita (California, New York, Texas) generally have more price competition than states with limited imaging infrastructure. Cash-pay rates can vary from $300 to $800 for the same study between neighboring counties in the same state.
High-field 3T MRI scanners produce sharper images than standard 1.5T scanners for certain applications, and some facilities charge a premium for 3T imaging. For most routine studies — spine, joints, brain — 1.5T is fully adequate and radiologists prefer it to 3T for some applications (1.5T has less artifact in certain body regions). Unless your physician specifically ordered 3T for a clinical reason, there's no advantage to paying a premium for it for standard indications. Our mri cost guide on upright imaging covers how stand-up MRI at lower field strength compares in price and clinical utility to standard-bore scanners.
The professional fee for a radiologist reading your MRI is billed separately from the technical fee charged by the imaging facility in most settings. The technical fee covers the use of the equipment, technologist time, and facility overhead. The professional fee (radiologist interpretation) is a separate line item, often from a different billing entity than the facility.
If you are checking in-network status, you need to confirm that both the facility AND the radiology group reading your scan are in-network. This two-part billing structure is the most common source of surprise out-of-network bills in imaging, and it has become more regulated under federal No Surprises Act protections, but it still occurs in some cases.
Urgent care centers that offer imaging services sometimes provide MRI at prices between standalone centers and hospital outpatient departments. These hybrid facilities are worth including in price comparisons when they exist in your area. Online platforms like Sesame Care, Zocdoc, and facility-specific websites increasingly post imaging prices, making initial research faster than calling each facility individually for a quote.
- Use a freestanding imaging center: Typically 40–60% less than hospital outpatient rates for identical studies
- Ask for the cash/self-pay rate: Many centers discount 30–50% below the standard charge for cash payment
- Compare prices first: Radiology Benefits Management platforms and Healthcare Bluebook show regional pricing
- Check your deductible status: If deductible is met, hospital may cost less than out-of-pocket at standalone center
- Confirm prior authorization before scheduling: Denied claims from missing auth can cost you the full charge
Insurance coverage mechanics significantly affect your out-of-pocket cost for an MRI. If you have a high-deductible health plan (HDHP) and have not met your annual deductible, you'll pay the full contracted rate between your insurer and the imaging facility — which is typically 20 to 40% below the facility's list price but still several hundred dollars.
Once your deductible is met, you pay your plan's co-insurance percentage (often 10 to 20%) until you reach your out-of-pocket maximum. Understanding where you are in your deductible cycle is important when timing an elective MRI — scheduling in December when your deductible is nearly met is very different than scheduling in January when you're starting fresh.
In-network versus out-of-network status changes your cost dramatically. In-network facilities have contracted rates with your insurer; out-of-network facilities can bill any amount and your insurer pays a limited portion. Some plans have no out-of-network coverage at all for imaging. Before scheduling, call your insurer or use their provider search tool to confirm that the specific facility (not just the radiology group that reads the scan) is in-network.
Hospital-based imaging departments are sometimes in-network at the hospital level but the professional component (radiologist reading fee) is billed separately by an out-of-network physician group — this surprise out-of-network billing has led to regulatory reform in many states but still occurs.
Medicare covers medically necessary MRI at 80% of the Medicare-approved amount after the Part B deductible, leaving a 20% co-insurance that can be significant for expensive studies. Medicare Advantage plans vary — some have lower cost-sharing for imaging than traditional Medicare; others have prior authorization requirements that traditional Medicare does not. Medicaid coverage is generally strong for MRI when the scan is physician-ordered, but Medicaid rates are lower than commercial rates, which can limit provider participation in some markets. Federal qualified health centers (FQHCs) and rural health clinics serve Medicaid patients with imaging referral coordination at lower cost.
Medical debt from imaging is one of the more negotiable categories of healthcare billing. Facilities have significant pricing flexibility for patients who are uninsured or underinsured, and hospitals that receive federal funding are required to have charity care programs for patients below income thresholds. If you receive an MRI bill you cannot afford, call the billing department before it goes to collections — most facilities will offer a payment plan, and many will reduce the total bill substantially for patients who request financial assistance.
The full billed charge is almost never what you actually owe; the contractual rate, charity care adjustment, or negotiated settlement is almost always lower. See our mri cost guide on specialized breast imaging for an example of how contrast-enhanced MRI costs are handled in specific clinical contexts.
Telehealth platforms that specialize in imaging referrals have emerged as another cost-reduction pathway. Services like SimonMed's online booking or Lucid Health let patients order certain MRIs directly — bypassing the physician referral in states where direct-access imaging is legal — at published flat-fee rates. These services handle scheduling and results delivery electronically.
For patients who know what imaging they need based on a previous diagnosis or established care relationship, this direct-access pathway can reduce both cost and the administrative friction of getting a referral. Confirm that results will be shared with your treating physician so your care team has the complete clinical picture alongside the cost savings.
MRI Cost by Body Part (Standalone Center)
Without contrast: $400–$700. With contrast: $600–$1,000. With and without (two-pass): $900–$1,500. Most common reasons: headache workup, seizure evaluation, stroke, multiple sclerosis, tumor screening. 30–60 min scan time.
Lumbar (lower back): $600–$1,000. Cervical (neck): $600–$950. Thoracic (mid-back): $600–$900. Full spine (3 regions): $1,500–$2,500. Most commonly ordered for back pain, disc disease, nerve compression. Without contrast is standard unless infection or tumor suspected.
Without contrast: $400–$700. With contrast: rare — usually not needed for sports injuries. Most common reasons: meniscus tear, ACL/MCL/PCL injury, cartilage damage. 20–30 min scan. One of the most commonly ordered MRIs due to sports injuries across all age groups.
Without contrast: $500–$800. MR arthrogram (contrast injected into joint): $800–$1,200. Arthrogram recommended for suspected labral tears (SLAP, Bankart). Standard MRI adequate for rotator cuff evaluation. 20–30 min scan.
Abdomen: $1,000–$1,800 with contrast. Pelvis: $800–$1,500. MRCP (biliary/pancreatic): $1,200–$2,000. Longer scan time (45–90 min) and often requires fasting and breath-hold sequences. Used for liver, kidney, and pelvic organ evaluation when CT or ultrasound is insufficient.
Most expensive: $1,500–$3,500, usually hospital-based. Used for cardiomyopathy evaluation, congenital heart disease, cardiac tumors, and myocardial viability assessment. Requires specialized cardiac MRI protocol and cardiologist oversight. Not widely available at standalone centers.
Shopping for MRI pricing before scheduling is practical and can be done in under 30 minutes. Call the imaging center directly and ask for the self-pay or cash rate for the specific CPT code(s) on your order. If you don't have the CPT codes, ask your doctor's office — they'll be on the ordering form. Price transparency tools like Healthcare Bluebook, Fairhealth Consumer, and hospital charge master databases also provide regional benchmarks. Standalone centers are usually willing to quote prices over the phone; hospital outpatient departments are sometimes reluctant but legally required to provide estimates for scheduled services.
For patients who are uninsured, several national imaging networks offer heavily discounted MRI rates. SimonMed, RadNet, Medovie, and regional alternatives frequently post flat-fee pricing online for common studies — brain, spine, and joint MRIs are often available in the $350 to $550 range at these centers, substantially below what a hospital would charge. These are the same diagnostic quality studies read by board-certified radiologists; the lower price reflects operating model efficiency and volume rather than compromised quality. Images are provided on CD and electronically, and report turnaround is typically 24 to 72 hours for routine studies.
MRI facilities may also offer sliding scale fees based on income, particularly if they are affiliated with academic medical centers or receive any federal funding. Asking about financial assistance programs or charity care at the time of scheduling is appropriate and does not affect the quality of your care. Hospitals are required to have these programs and to make them available to patients who request information.
If you are referred to a hospital facility specifically because of a clinical need — specialized equipment, specific subspecialist radiologist — and the cost is prohibitive, it is worth asking the referring physician whether an equivalent study can be done at a lower-cost setting for your specific indication. The clinical appropriateness conversation and the cost conversation are separate but both legitimate to have. Additional context on managing imaging costs within specific MRI categories is available through the mri cost resource library for MRI technologist and patient education.
Medical billing advocates are an underused resource for patients facing unexpectedly high MRI bills. These professionals — sometimes called patient advocates or medical billing consultants — review your billing, identify errors (which are common), negotiate on your behalf, and help navigate financial assistance applications.
Many work on contingency, taking a percentage of the savings they generate rather than charging upfront fees. For bills above $2,000 where negotiation is clearly warranted, the time savings alone justify using an advocate. State insurance commissioner offices also handle disputes about wrongly denied claims and can facilitate resolution when an insurer incorrectly denies a prior-authorized scan.
Being proactive about insurance coverage before your MRI appointment is far more effective than disputing bills after the fact. The prior authorization process is your single most important protection against large unexpected bills. Getting authorization confirmation in writing (or noting the authorization number and representative name if done by phone) creates documentation that protects you if a claim is later disputed. Keep a record of all communications with your insurer about coverage and authorization for any imaging study. Our mri cost and preparation guide covers the full range of MRI preparation topics for patients and technologist candidates alike.
MRI Cost Checklist Before You Schedule
- ✓Confirm prior authorization status with your insurer or physician's office
- ✓Check whether the facility is in-network for your specific insurance plan
- ✓Ask for the cash/self-pay rate if you are uninsured or paying out-of-pocket
- ✓Compare the in-network rate at a hospital outpatient department vs. a standalone center
- ✓Clarify whether your order is with contrast, without contrast, or both — contrast adds cost
- ✓Ask your physician if a lower-cost facility is clinically appropriate for your specific study
- ✓If on an HDHP, check where you are in your deductible cycle before scheduling
- ✓Ask about financial assistance or charity care programs if cost is a barrier
- ✓Get the CPT codes for your MRI order — you need them to get accurate price quotes
- ✓Confirm that the radiologist reading your scan is also in-network (separate from the facility)
MRI Cost by Insurance Type
Typical structure: Prior authorization required for most MRIs. In-network contracted rate (usually 40–60% below list price). Patient pays: deductible first, then co-insurance (typically 10–20%) until out-of-pocket maximum. Example: $1,200 contracted rate for brain MRI. If deductible is unmet: patient pays $1,200. If deductible met: patient pays 20% co-insurance = $240. Out-of-pocket maximum typically $3,000–$8,000/year depending on plan. Key actions: confirm prior auth, use in-network facility, track deductible status to time elective studies strategically.
Hospital vs. Standalone Imaging Center
- +Hospital: specialists and emergency resources available if complications arise
- +Hospital: may have 3T and specialty scanners (cardiac MRI, intraoperative MRI) not at standalone
- +Hospital: accredited for complex clinical protocols (contrast monitoring, sedation)
- +Standalone: significantly lower cost — typically 40–60% of hospital outpatient rates
- +Standalone: often shorter wait times and faster scheduling for routine studies
- −Hospital: higher cost even after insurance; surprise out-of-network physician bills more common
- −Hospital: longer wait times for non-urgent scheduling
- −Standalone: not appropriate for unstable patients or those requiring clinical monitoring
- −Standalone: limited specialty protocols (cardiac MRI, pediatric sedation) at most centers
- −Standalone: may have fewer same-day or emergency appointment slots for urgent studies
MRI Cost Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.