MRI Scanner: How It Works, Types, Components and Cost
MRI scanner guide — how it works, magnet strengths (1.5T, 3T, 7T), scanner types, components, top manufacturers, cost, and how it differs from CT.
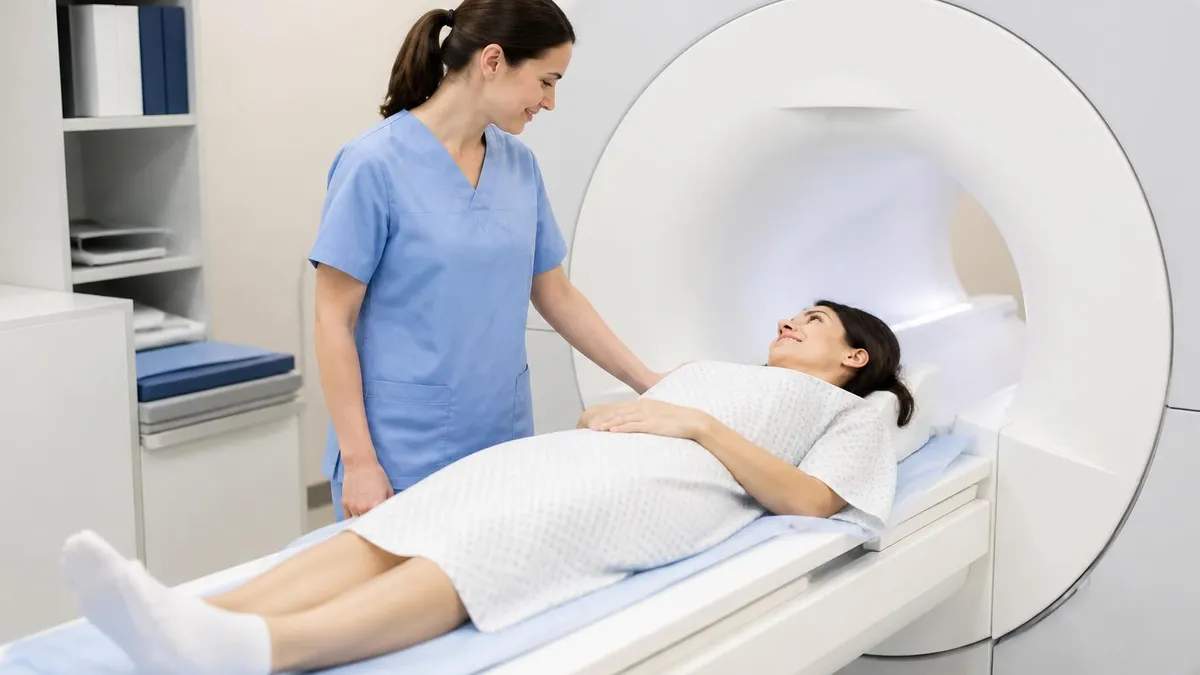
An MRI scanner is the medical imaging machine that uses a powerful magnetic field and radio waves to produce detailed cross-sectional images of the inside of the body. Where CT scanners use ionizing X-rays and ultrasound machines use sound waves, MRI uses no radiation at all — the imaging signal comes from the protons inside hydrogen atoms in the patient's tissues, which respond to the scanner's magnetic field and radiofrequency pulses. The resulting images show soft tissue, organs, brain, spine, joints and blood vessels in a detail no other imaging modality can match.
The scanner itself is a complex assembly of high-tech components. At the core sits a superconducting magnet kept at -269°C by liquid helium, generating a static magnetic field 30,000 to 60,000 times stronger than the earth's magnetic field. Surrounding the static magnet are three gradient coils that switch on and off rapidly to encode position information, plus radiofrequency coils that transmit and receive the imaging signal. A separate computer system processes the raw data into the images displayed on the radiologist's workstation.
MRI scanners come in several configurations. Closed-bore scanners with a 60 cm tube are the standard hospital workhorse, available at every major imaging center. Wide-bore scanners (70 cm) feel less confining for claustrophobic patients and accommodate larger body sizes. Open MRI scanners with C-arm or vertical-field designs trade some image quality for an open feel that suits very claustrophobic or pediatric patients. Field strengths range from low-field 0.3T machines for limb imaging up to 7T research scanners that produce extraordinary resolution for neuroscience research.
This guide explains how an MRI scanner works at the physical level, the components that make it function, the different magnet strengths and scanner types you may encounter, the major manufacturers (Siemens Healthineers, GE HealthCare, Philips, Canon Medical), realistic cost figures, and how MRI compares to other imaging modalities. The goal is to make the technology behind every MRI scan less mysterious so you understand what you are looking at when you walk into the imaging suite.
MRI scanner in 30 seconds
An MRI scanner uses a superconducting magnet (cooled by liquid helium to -269°C), gradient coils for spatial encoding and radiofrequency coils for signal transmission and reception. Standard clinical scanners are 1.5T or 3T magnetic field strength. Closed-bore (60 cm) is standard; wide-bore (70 cm) and open MRI options exist for claustrophobic or larger patients. New scanner cost ranges from about $1 million for low-field to $3 million+ for 3T systems, with 7T research scanners exceeding $7 million.
The physics of MRI starts with the abundance of hydrogen atoms in the human body — water, fat and other tissues all contain large quantities of hydrogen, which is just a proton with one electron. Protons have a quantum property called spin, which gives them a tiny magnetic moment. In the absence of an external magnetic field, the protons in your body are randomly oriented and produce no net magnetic signal. Place the body in a strong magnetic field, however, and the protons align with that field, producing a small but detectable net magnetization.
The scanner then transmits a radiofrequency pulse tuned to the specific frequency at which the aligned protons resonate (the Larmor frequency, which depends on the field strength). This pulse tips the proton magnetization away from alignment with the static field. When the pulse stops, the protons relax back to alignment, releasing energy as a radio signal. The receiver coils pick up that signal, the gradient coils encode the position information, and the computer reconstructs the data into images.
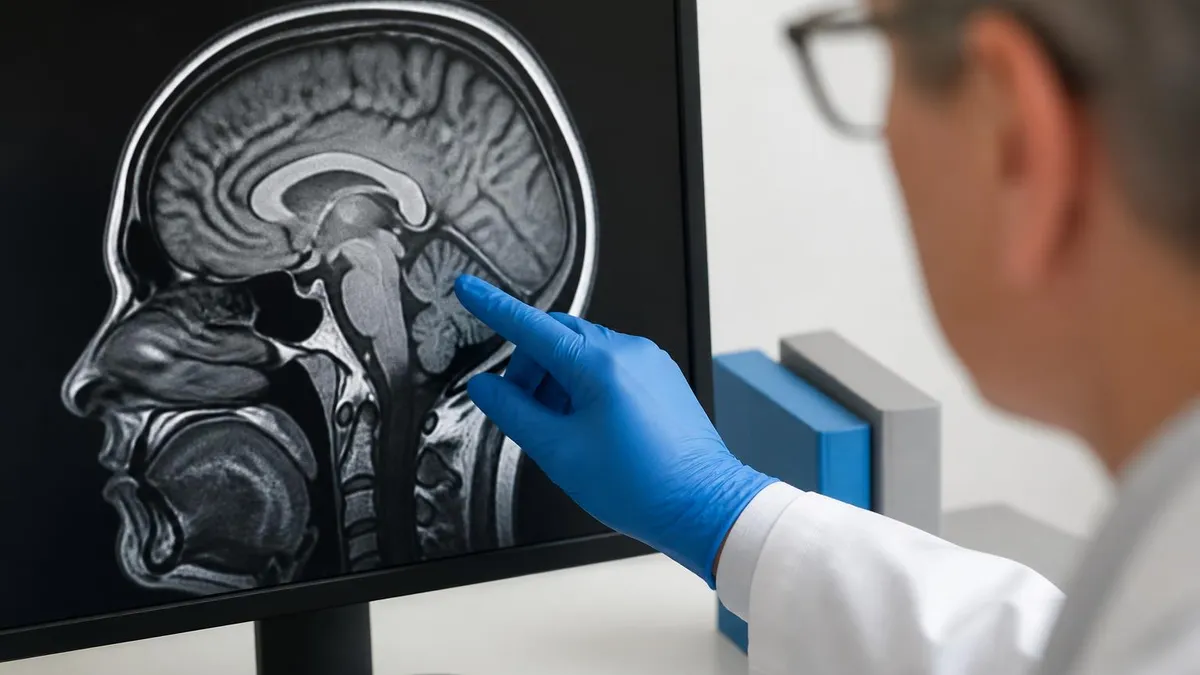
Different tissues have different relaxation properties — fat relaxes differently from muscle, which relaxes differently from cerebrospinal fluid. By varying the timing of the radiofrequency pulses and the relaxation measurements, the scanner produces different image contrasts emphasizing different tissue types. T1-weighted images are typically the anatomical reference. T2-weighted images emphasize water content. Dozens of specialty sequences exist, each tuned to highlight specific findings — diffusion-weighted imaging for stroke, susceptibility-weighted imaging for blood products, MR spectroscopy for tumor characterization.
The main static magnet is the largest, most expensive and most sensitive component of the scanner. Modern 1.5T and 3T scanners use superconducting magnets — niobium-titanium wire coils cooled to nearly absolute zero by liquid helium, where electrical resistance disappears entirely and the current flows essentially forever once started. The magnet is energized once at installation and remains on continuously for the life of the scanner, only quenched (deliberately discharged) for major service or emergencies.
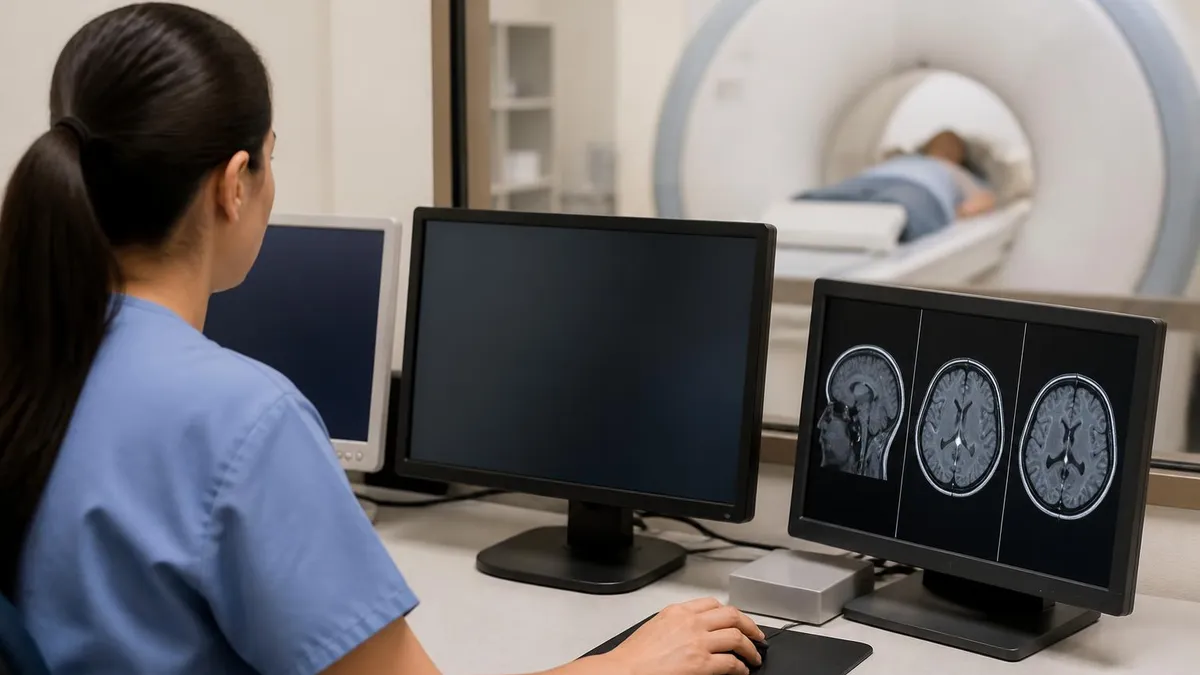
Major MRI scanner components
The heart of the scanner. Niobium-titanium wire coils carrying massive current, cooled to -269°C by liquid helium. Produces the static magnetic field (1.5T, 3T or higher) that aligns the body's hydrogen protons. Operates continuously for years with periodic helium top-ups; quench-only emergency discharge.
Three sets of coils (X, Y, Z axes) that switch on and off rapidly during scanning to encode spatial position into the signal. Gradient switching produces the loud knocking sounds patients hear during MRI. Higher gradient strength enables faster scans and finer resolution. Typical specifications: 80 mT/m strength, 200 T/m/s slew rate.
Transmit RF pulses at the Larmor frequency to perturb the proton magnetization, then receive the returning signal. Body, head, knee, breast, shoulder and other anatomy-specific coils plug into the scanner for each exam. Newer multi-channel array coils (32-channel and beyond) accelerate scans and improve image quality substantially.
Processes the raw signal data through Fourier transforms and reconstruction algorithms into the final cross-sectional images. Modern scanners use GPU acceleration for real-time reconstruction, supporting advanced techniques like compressed sensing and AI-based denoising. The control console runs the scanner, monitors patient safety and stores the resulting images.
Magnet field strength is measured in Tesla (T), named after Nikola Tesla. Earth's magnetic field is about 0.00005 Tesla. Refrigerator magnets are about 0.001 Tesla. A standard clinical MRI scanner is 1.5T or 3T — meaning 30,000 to 60,000 times stronger than the planet's magnetic field. The unit is named for the inventor who first systematically described electromagnetic resonance phenomena in the 19th century, although the MRI application of his theoretical foundations only emerged in the 1970s.
Field strength matters because higher field produces a stronger MRI signal, which can be traded for faster scans, higher resolution or thinner image slices. A 3T scanner produces about twice the signal of a 1.5T scanner of the same age and design. The trade-offs are higher equipment cost, slightly higher artifact rates from metal in the body, and more challenging engineering for shielding and homogeneity. For most clinical applications 1.5T is excellent and 3T is preferred; for research applications 7T provides extraordinary resolution but is rare.
Low-field scanners (0.3T to 1.0T) still exist for specific niches. Some musculoskeletal-only scanners image just hands, knees, feet, elbows or shoulders at low field. The patient sits or lies in a comfortable position with only the limb in the magnet, which avoids claustrophobia entirely. Image quality is lower than full-body 1.5T or 3T but adequate for most extremity questions. Recent low-field general-body scanners (Hyperfine, others) at 0.064T are emerging for portable bedside imaging in ICUs and rural settings.
The 7T scanners are research instruments at major academic centers — about a hundred installed worldwide. They produce neuroimaging detail far beyond clinical capability, allowing visualization of individual cortical layers and small structures invisible at 3T. The FDA approved 7T systems for clinical use in 2017, but the high cost ($7 million+), strict siting requirements (specialized magnetic shielding, extensive cooling infrastructure) and challenging artifact profile keep them mostly in research. Wider clinical 7T adoption is decades away.
MRI scanner types compared
The classic 60 cm bore tube scanner found in most hospitals. 1.5T or 3T field strength. Excellent image quality for nearly every clinical exam. Best signal-to-noise ratio. Confined feel may trigger claustrophobia in 5 to 10% of patients. Manufacturer examples include Siemens Magnetom Aera (1.5T), GE Signa Architect (3T), Philips Ingenia (1.5T or 3T).
The room around the scanner is engineered to support its operation. The MRI suite must be shielded from external radiofrequency interference, typically with a Faraday cage built into the room walls — a continuous metallic shield that blocks outside RF noise from reaching the scanner. The doors include RF gaskets that maintain shielding integrity when closed. Specialized grounding, filtered electrical penetrations and copper lining around windows complete the shielding system. Without proper shielding, ambient radio signals would corrupt the imaging data.
Cryogen handling adds further infrastructure. The liquid helium that cools the magnet boils off slowly (about 0.05% per day in modern zero-boil-off systems) and must be replenished every 1 to 5 years depending on the scanner generation. The boil-off vapor is vented through a quench pipe to the building exterior. In an emergency quench scenario, all the helium boils off at once into the room, which would displace breathable air — emergency ventilation systems handle this risk. Cryogen costs are a substantial line item in scanner operating budgets.
The patient table is more sophisticated than it appears. Inside the table run electrical connections for the radiofrequency coils placed over the patient, the patient call button, the panic squeeze ball, and the patient comfort accessories. The table positioning is computerized and indexed precisely for each scan. The bore opening accepts the table for imaging and retracts it between sequences. Modern tables include weight capacity sensors, table-side controls for technologists and emergency stop systems.
The control console is in the adjacent technologist's room, separated from the scanner room by a window with RF shielding and a door. The technologist runs the scan from the console while watching the patient through the window and communicating via intercom. A second monitor displays vital signs from the patient's pulse oximetry and ECG monitoring, particularly important for sedated patients or those undergoing contrast-enhanced exams. Emergency stop buttons and intercom links are within arm's reach throughout the procedure.
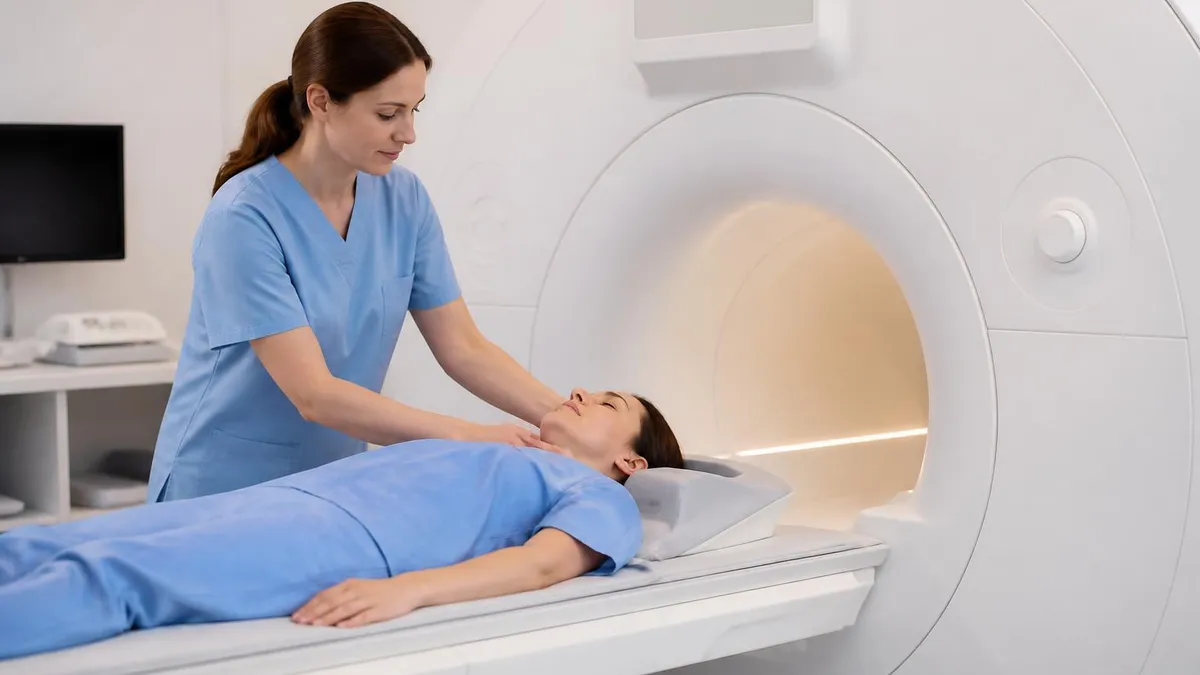
MRI suites use a four-zone safety model. Zone I is the public area outside the suite — no MRI risks. Zone II is the patient intake and screening area where ID and history are reviewed. Zone III includes the technologist control room and ancillary spaces, restricted to screened personnel. Zone IV is the magnet room itself, where the magnetic field is always on. Anyone entering Zone IV must be screened for ferromagnetic objects and implants. Free-flying ferromagnetic items become deadly projectiles in this zone.
The four major MRI manufacturers globally are Siemens Healthineers, GE HealthCare, Philips and Canon Medical Systems (formerly Toshiba Medical). Together they account for the vast majority of installed MRI base. Each maintains a full lineup from 1.5T through 3T, with their flagship systems differentiated by software features, gradient performance, coil technology and AI-enabled reconstruction. The four-vendor competition keeps innovation moving rapidly across the industry.
Siemens Healthineers' MRI lineup includes the Magnetom family — Magnetom Aera (1.5T), Magnetom Vida (3T) and Magnetom Cima.X (3T flagship). Siemens emphasizes BioMatrix sensor technology that adapts the scan to each patient and Deep Resolve AI image reconstruction. GE HealthCare's Signa lineup includes Signa Architect (3T), Signa Premier (3T) and Signa Hero (3T flagship), with strong AIR Recon DL deep learning reconstruction. Philips Ingenia and Canon Vantage round out the major options.
Pricing varies enormously by configuration. New 1.5T scanners run $1 million to $1.7 million depending on bore size, gradient performance, coil package and software. New 3T scanners run $2 million to $3.2 million in similar configurations. 7T research scanners exceed $7 million. Used scanners (typically 5 to 10 years old) trade at 30 to 50% of new prices and remain workhorses at smaller imaging centers and outpatient clinics. Total cost of ownership over 10 years runs roughly twice the purchase price when service contracts, cryogen, electricity and replacement parts are included.
For the patient using the scanner, the manufacturer choice is mostly invisible. Image quality differences between vendors at the same field strength are subtle and require expert review. The choice of scanner brand at a given imaging center is driven by purchase economics, service relationships, training history and integration with the existing PACS (picture archiving and communication system). What matters most for image quality is the field strength, the age of the scanner generation, the coil package available and the experience of the radiologist reading the images.
Choosing an MRI facility checklist
- ✓Confirm field strength: 1.5T standard, 3T preferred for fine detail
- ✓Confirm bore size: 70 cm wide-bore for claustrophobia or larger body habitus
- ✓Confirm scanner age: under 8 years generally produces best images
- ✓Verify ACR (American College of Radiology) accreditation
- ✓Ask about appropriate coil for your specific exam
- ✓Verify board-certified radiologist reads the studies
- ✓Confirm subspecialty radiologist for neuro, MSK, cardiac etc.
- ✓Ask about prior MRI image upload for comparison
- ✓Confirm exam protocol matches your clinical question
The differences between MRI and other imaging modalities are concrete. CT scanners use ionizing X-rays rotating around the patient to produce cross-sectional images; the test is fast (under 2 minutes for a head scan), excellent for bone and acute hemorrhage, and uses a relatively low radiation dose. CT is the test of choice for trauma triage, acute stroke screening and many lung and abdominal questions where speed matters. CT cannot match MRI's soft-tissue detail, however, particularly for the brain, spine, joints and pelvic organs.
X-ray (radiography) is the simplest imaging modality, using a single-shot ionizing X-ray to produce a 2D image. It is extremely fast and inexpensive, which makes it the standard first-line test for fractures, chest infections, foreign bodies and many orthopedic questions. X-ray has no soft-tissue resolution to speak of and shows nothing inside the brain or spinal cord beyond the bony framework. It complements MRI rather than competing with it.
Ultrasound uses high-frequency sound waves and a handheld probe to produce real-time images. It uses no radiation, is portable and inexpensive, and is the imaging method of choice in obstetrics, in critical care for procedural guidance, in cardiac assessment, and in many abdominal and vascular applications. Ultrasound's limitations include operator dependence, poor penetration through bone and gas, and limited deep-tissue imaging in obese patients. It is complementary to MRI rather than a competitor.
PET (positron emission tomography) uses injected radioactive tracers to image metabolic activity rather than anatomy. It is the standard test for whole-body cancer staging, for some neurological diseases, and for cardiac viability assessment. Modern PET scanners are usually paired with CT (PET/CT) or MRI (PET/MRI) to combine functional and anatomical imaging in a single exam. PET-MRI hybrid scanners exist but are rare because of the engineering challenge of combining the two technologies safely.
For patients curious about the noise of MRI, the explanation lies in the gradient coils. When the gradients switch on and off rapidly during a scan, the changing magnetic fields exert mechanical force on the coil wires inside the scanner. The vibration produces sound at frequencies the human ear hears as loud knocking, clicking or buzzing. Noise levels reach 100 dB or higher inside the bore — louder than a chainsaw — which is why hearing protection is mandatory and music is offered through MRI-safe headphones during the scan.
Active noise cancellation technology, similar to consumer headphones, has begun appearing on premium scanners. The technique uses microphones inside the bore to capture the gradient noise, then plays an inverted waveform through the headphones to cancel it. The result is a substantial reduction in perceived noise — sometimes to under 70 dB inside the headphones during the loudest sequences. Most existing scanners do not have this capability, but new installations increasingly include it as a comfort feature.
MRI scanner quick numbers
Top MRI manufacturers
German manufacturer with the Magnetom MRI lineup. Aera (1.5T), Vida (3T), Cima.X (3T flagship) and 7T research systems. Strong on BioMatrix patient adaptation technology and Deep Resolve AI image reconstruction. Largest installed base globally; particularly dominant in European and Asian markets.
American manufacturer with the Signa MRI lineup. Architect (3T), Premier (3T) and Hero (3T flagship). Strong on AIR Recon DL deep learning reconstruction technology and a wide coil portfolio. Particularly strong in North American hospital systems and integrated with the GE PACS and clinical workflow platforms.
Dutch manufacturer with the Ingenia MRI lineup. Ingenia (1.5T or 3T), Ingenia Elition (3T flagship). Strong on Compressed SENSE acceleration technology and helium-free magnet designs (Ingenia Ambition). Significant European market share with growing installations across emerging markets.
Japanese manufacturer (formerly Toshiba Medical) with the Vantage MRI lineup. Vantage Galan (1.5T or 3T), Vantage Centurian (3T flagship). Strong on quiet scan technology (mWave for noise reduction) and AI-enhanced reconstruction. Particularly strong in Japanese and Asian markets with growing North American footprint.
The future of MRI scanners is moving in several directions simultaneously. AI-based image reconstruction is dramatically reducing scan times — sequences that took 6 minutes on older scanners now complete in 90 seconds with similar image quality on systems with deep learning reconstruction. The result is shorter exams, less patient discomfort and higher throughput for the imaging center. Most major manufacturers now ship AI reconstruction as a standard or upgrade feature.
Helium-free and reduced-helium magnet designs are another active area. Liquid helium is a finite global resource with rising prices and supply concerns; new scanner designs use sealed helium systems that need no top-ups, or in some cases use only a few liters of helium with ongoing recovery. Philips Ingenia Ambition was an early entrant in this category. Long-term, the goal is sealed scanners that operate for the full 15-year life without any helium replenishment, dramatically simplifying logistics and reducing total cost of ownership.
MRI scanner: strengths and limits
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.