Prostate MRI: Multiparametric Imaging for Prostate Diagnosis
Prostate MRI explained: multiparametric MRI (mpMRI) for cancer detection, PI-RADS scoring, procedure, preparation, and what results mean.
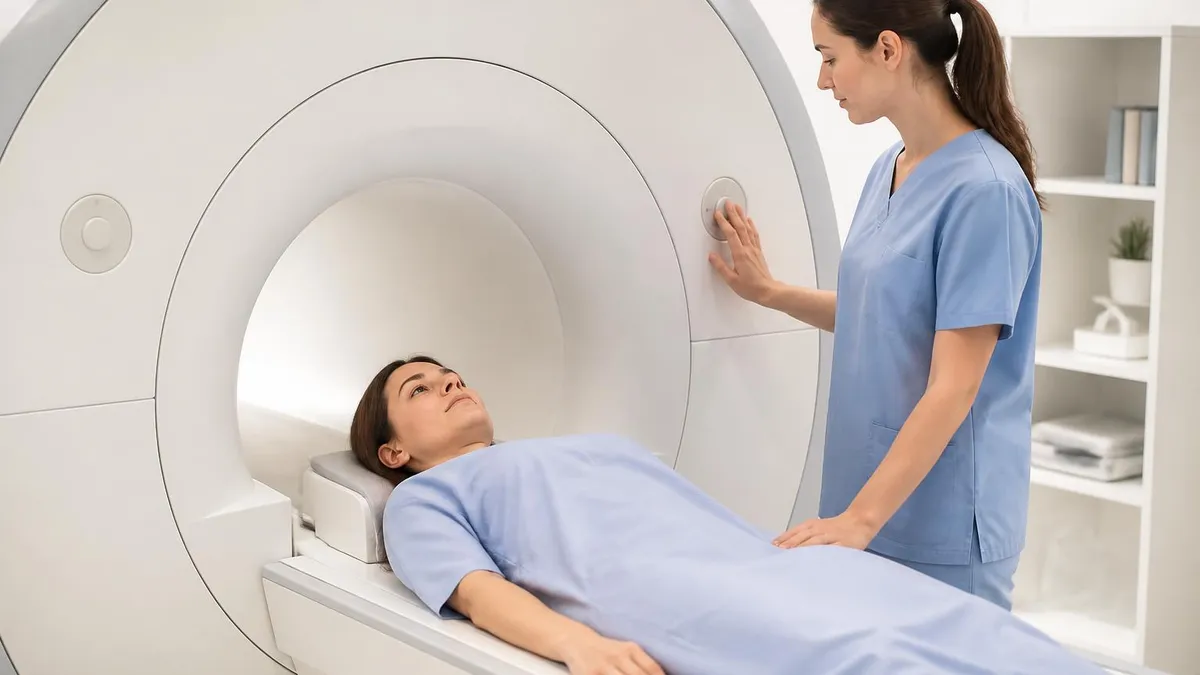
Prostate MRI, particularly multiparametric MRI (mpMRI), has become the standard imaging modality for evaluating prostate cancer suspicion in men. The examination combines multiple MRI sequences providing detailed visualization of prostate anatomy, identification of suspicious lesions, and characterization of lesion features supporting clinical decision-making about biopsy and treatment. Modern prostate MRI substantially improves cancer detection while reducing unnecessary biopsies compared to PSA-based screening alone. Understanding what prostate MRI involves helps patients facing the examination prepare appropriately and understand subsequent results.
Multiparametric prostate MRI typically combines three or more MRI sequences each providing different information. T2-weighted imaging shows detailed prostate anatomy and zonal architecture. Diffusion-weighted imaging (DWI) with apparent diffusion coefficient (ADC) maps highlights areas of restricted water diffusion characteristic of dense cellular tumors. Dynamic contrast-enhanced (DCE) imaging shows tumor blood flow patterns. Some examinations add MR spectroscopy for chemical analysis of suspected tumor areas. The combined sequences enable comprehensive evaluation that single-sequence imaging cannot achieve. Each sequence contributes specific information that radiologists integrate for overall assessment.
Prostate MRI Quick Facts
Type: Multiparametric MRI (mpMRI) combining T2, DWI, and dynamic contrast sequences. Field strength: 3 Tesla preferred; 1.5T acceptable with appropriate technique. Duration: 30-45 minutes scanner time. Cost: $500-$3,500 typical without insurance. Common indications: Elevated PSA, abnormal DRE, family history, post-treatment surveillance, biopsy planning. Scoring: PI-RADS v2.1 standardized scoring system (1-5 scale). Preparation: Bowel preparation common; specific instructions from facility.
Common indications for prostate MRI include elevated prostate-specific antigen (PSA) suggesting possible prostate cancer warranting investigation, abnormal digital rectal examination (DRE) findings suggesting palpable abnormality, family history of prostate cancer affecting risk assessment, prior negative biopsy with continued cancer suspicion, active surveillance monitoring of known low-risk prostate cancer, and pretreatment planning when cancer is confirmed. Each indication has somewhat different examination focus but all use similar mpMRI protocols. The standardization across indications supports radiologist expertise and consistent reporting through standardized scoring systems.
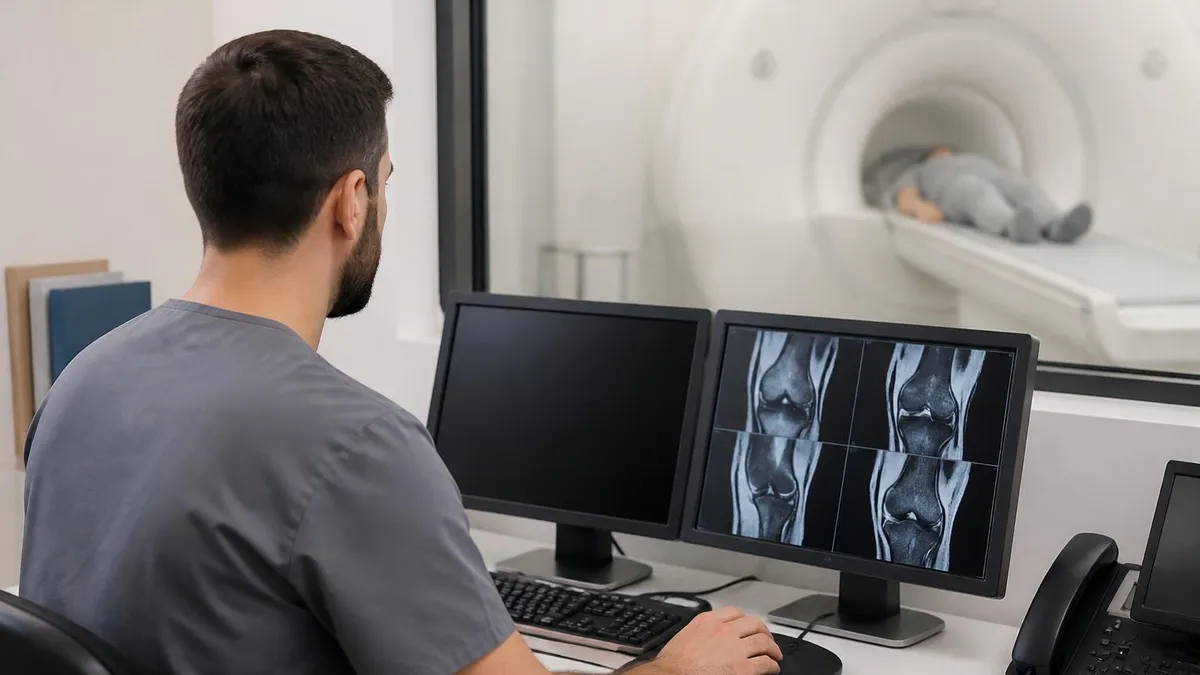
Prostate MRI Components
Shows prostate anatomy and zones. Cancer typically appears as dark areas in normally bright peripheral zone.
Highlights restricted water diffusion in dense tumors. Combined with ADC maps for quantitative assessment.
Shows tumor blood flow patterns through gadolinium contrast injection. Helps characterize suspicious areas.
Chemical analysis of metabolites in suspected tumors. Less commonly used in modern protocols.
Standardized 1-5 scoring assessing cancer suspicion. PI-RADS 4-5 typically prompts biopsy.
Identification and location of suspicious lesions for targeted biopsy if indicated.
The PI-RADS (Prostate Imaging Reporting and Data System) scoring system provides standardized assessment of suspicious lesions identified on prostate MRI. The current version (PI-RADS v2.1) assigns scores 1-5 based on combined assessment of T2, DWI, and DCE findings. PI-RADS 1: very low probability of clinically significant cancer. PI-RADS 2: low probability. PI-RADS 3: intermediate probability requiring clinical correlation.
PI-RADS 4: high probability of clinically significant cancer. PI-RADS 5: very high probability. Higher scores typically prompt targeted biopsy of identified lesions while lower scores may support continued surveillance without immediate biopsy. The standardized scoring supports consistent communication between radiologists and clinicians across different facilities and supports comparison across studies over time.
Targeted biopsy guided by MRI findings has revolutionized prostate cancer diagnosis. Traditional systematic biopsy involves taking 12 core samples from random prostate locations, missing some cancers (particularly anterior prostate cancers difficult to reach with traditional approach) while detecting clinically insignificant cancers that might never cause harm. MRI-targeted biopsy specifically samples PI-RADS 4-5 lesions identified on imaging, improving detection of clinically significant cancers while reducing detection of insignificant disease.
Several biopsy techniques support MRI guidance: cognitive (radiologist views MRI then biopsies general area), MRI-ultrasound fusion (software combines MRI with real-time ultrasound for precise targeting), and in-bore MRI biopsy (biopsy performed within MRI scanner for maximum precision but most expensive and time-consuming). Each approach has advantages and limitations matching different clinical situations.
Modern prostate MRI has substantially impacted clinical practice for prostate cancer evaluation. Pre-biopsy MRI now standard recommendation in many guidelines — performing MRI before biopsy supports targeted biopsy of identified lesions while sometimes avoiding biopsy entirely for low PI-RADS cases. PRECISION trial and similar research demonstrated MRI-guided biopsy detects more clinically significant cancer while detecting fewer insignificant cancers compared to systematic biopsy.
Active surveillance for low-risk prostate cancer increasingly uses periodic MRI to monitor for progression rather than routine repeat biopsies. Treatment planning for confirmed cancer benefits from MRI staging information beyond what biopsy alone provides. Each application reflects MRI's central role in modern prostate cancer care pathway.
Prostate MRI procedure: Arrive 30 minutes early for paperwork, screening, and changing into gown. Some facilities require bowel preparation (enema or laxative) the day of or before exam to reduce gas artifact. IV access established for contrast injection. Patient lies supine on scanner table. Pelvic coil placed over prostate area. Earplugs and headphones provided (scanner is loud). Total scan time 30-45 minutes including various sequences. Contrast injected partway through during dynamic sequences. Stay still during sequences for clear images. Total time at facility 1-2 hours typically.
Patient experience during prostate MRI varies somewhat from other MRI types. Endorectal coil (used in some older protocols, less common modern) creates significant patient discomfort during examination. Modern protocols using only pelvic surface coil are substantially more comfortable. Bowel preparation requirements (enema or laxative) before exam can be inconvenient but improve image quality through reduced rectal gas artifact.
The 30-45 minute scan duration requires staying still for extended period in supine position. Loud scanner noise (similar to other MRI types) protected by earplugs and headphones. IV contrast injection produces brief warm sensation but generally well-tolerated. Anti-anxiety medication available for claustrophobic patients. Most patients tolerate prostate MRI without significant difficulty.
Image quality factors significantly affect prostate MRI value. Modern 3 Tesla (3T) scanners produce sharper images than older 1.5 Tesla (1.5T) scanners through stronger magnetic field, supporting better cancer detection particularly for small lesions. Multi-channel pelvic coils with multiple receiving elements improve signal quality. Patient cooperation through staying still during sequences supports image clarity.
Bowel preparation reducing gas artifact improves images particularly for lesions near rectum. Sequence parameters must follow standardized protocols supporting consistent quality. Quality differences between facilities can substantially affect accuracy — facilities with experienced prostate MRI radiologists, modern equipment, and standardized protocols produce better outcomes than facilities lacking these elements.
Reporting standardization through PI-RADS system improves communication and consistency. Standardized report templates ensure all relevant findings addressed systematically. Lesion location described using sector-based mapping system supporting precise communication. PI-RADS scoring uses standardized criteria reducing subjective interpretation variation. Recommendations for further evaluation follow standard guidelines linking imaging findings to clinical action. The combination of standardization elements supports better clinical decisions through clearer information transfer between radiologists, urologists, and patients across different facilities and treatment teams.
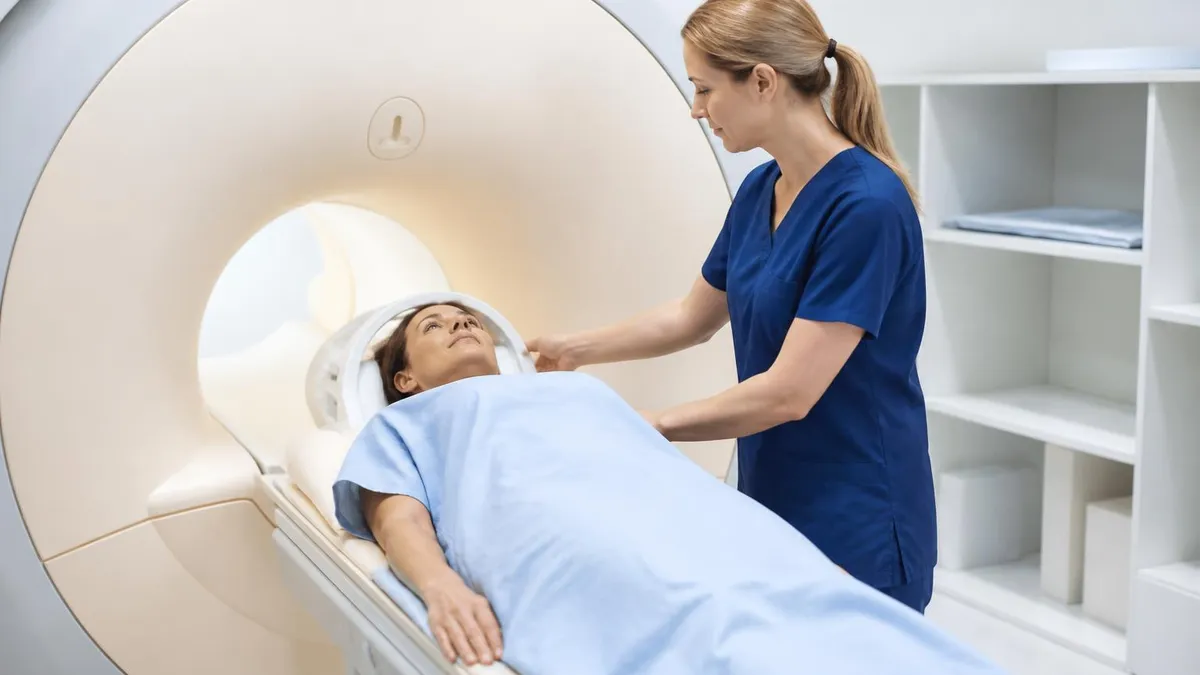
Don't skip preparation requirements — bowel preparation substantially improves image quality. Disclose all metal implants and devices — some prevent MRI examination. Inform about kidney disease — affects gadolinium contrast use. Don't expect immediate results — radiologist interpretation takes 1-3 business days typically. Watch for facility quality differences — experienced prostate MRI facilities produce better outcomes than facilities without specialty experience.
Cost considerations for prostate MRI vary substantially. Without insurance, costs range $500-$3,500 depending on facility and region. Hospital-based MRI typically costs more than outpatient imaging center MRI for equivalent studies. Cash-pay rates at outpatient centers often substantially lower than insurance-billed rates. With insurance, your out-of-pocket cost depends on plan, deductible status, and in-network status. Some insurance plans require pre-authorization for prostate MRI — verify before scheduling. Medicare and most major insurance plans cover prostate MRI for appropriate clinical indications. The investment compares favorably to potential alternative pathways involving multiple unnecessary biopsies.
For men considering prostate MRI based on elevated PSA or other concerns, several factors guide the decision. Discussion with primary care physician or urologist about whether MRI is appropriate for your specific situation. Understanding what MRI can and cannot determine — MRI shows suspicious areas but doesn't definitively diagnose cancer (only biopsy confirms). Considering family history affecting risk assessment. Understanding subsequent decision pathway based on different possible results. Most men with concerning PSA results benefit from prostate MRI before biopsy to support targeted approach if biopsy proves necessary or potentially avoiding biopsy entirely if MRI shows low cancer probability.
For men receiving prostate cancer treatment, MRI plays role in treatment planning and monitoring. Pretreatment staging MRI helps determine cancer extent within prostate and assess for spread beyond prostate to seminal vesicles, lymph nodes, or bones. Treatment planning for radiation therapy uses MRI for precise tumor location supporting focused radiation. Post-treatment surveillance MRI monitors for recurrence after radiation, surgery, or active surveillance. Each application provides valuable clinical information beyond what other modalities provide. The expanding role of MRI throughout prostate cancer care pathway reflects continued improvements in imaging technology and clinical evidence supporting MRI use.
Preparing for Prostate MRI
- ✓Verify with imaging facility about specific preparation requirements
- ✓Complete bowel preparation if instructed
- ✓Disclose all metal implants and surgical history
- ✓Inform about kidney disease affecting contrast use
- ✓Avoid eating immediately before exam
- ✓Bring identification and insurance information
- ✓Wear comfortable easily-removable clothing
- ✓Plan for 1-2 hours total time at facility
Active surveillance for low-risk prostate cancer increasingly uses periodic prostate MRI to monitor for progression. Active surveillance involves close monitoring of low-risk cancer rather than immediate treatment, recognizing that some prostate cancers grow so slowly they never cause harm during patient's lifetime. Traditional active surveillance protocols involved repeated biopsies (every 1-3 years typically) to detect progression.
Newer protocols incorporate MRI as primary monitoring tool, reducing biopsy frequency for stable cases while maintaining ability to detect significant progression. The combination of MRI monitoring plus targeted biopsy for new suspicious findings supports active surveillance with reduced patient burden compared to repeat systematic biopsies.
For radiologists specializing in prostate imaging, ongoing professional development supports expertise. Subspecialty fellowship training in genitourinary radiology develops focused expertise. Society of Abdominal Radiology Disease-Focused Panel on Prostate Cancer publishes guidelines and educational materials. Annual conferences cover prostate imaging advances. Case review with colleagues and second-opinion services support difficult cases. The combination of formal training, continuing education, and ongoing clinical experience supports the substantial expertise prostate MRI interpretation requires. Patients benefit from facilities where radiologists have substantial prostate MRI experience rather than reading occasional studies among general radiology workload.
For urologists working with prostate MRI in clinical practice, integration with overall patient care matters substantially. MRI findings should inform treatment decisions in context of PSA trends, biopsy results, family history, and patient preferences. Regular discussion with imaging colleagues supports best use of MRI in patient care. Multidisciplinary tumor boards reviewing complex cases provide forum for integrated decision-making. Patient education explaining what MRI can and cannot determine supports realistic expectations. The combination of clinical context plus imaging information produces best clinical decisions for individual patients facing prostate cancer concerns or treatment.
For specific patient populations, prostate MRI applications vary somewhat. Men with elevated PSA but no prior biopsy benefit from MRI before biopsy supporting targeted approach. Men with prior negative biopsy but persistent cancer suspicion benefit from MRI identifying possible missed lesions for targeted biopsy. Men on active surveillance benefit from periodic MRI monitoring. Men with confirmed cancer benefit from staging MRI before treatment selection. Each population gets somewhat different MRI emphasis but all use similar fundamental mpMRI approach. Discussion with urologist about appropriate MRI use in your specific situation supports informed decisions about whether and when MRI is appropriate.
Looking forward at prostate MRI evolution, several trends shape future practice. AI-assisted lesion detection helps radiologists identify suspicious areas more reliably. Quantitative biomarkers from MRI may eventually support better cancer characterization beyond qualitative scoring. New contrast agents may improve specific clinical applications. Higher field strength scanners (7T) may eventually provide additional detail though clinical applications remain investigational. Each advance continues improving prostate MRI capability and clinical value. Patients undergoing prostate MRI today benefit from substantial improvements over MRI of even ten years ago, and continued improvement seems likely over coming years supporting better cancer detection and care.
For people considering whether to undergo prostate MRI when ordered, the answer is generally yes for appropriate clinical situations. Modern prostate MRI provides valuable diagnostic information that supports better clinical decisions about biopsy and treatment. The examination is generally well-tolerated with modern protocols not requiring uncomfortable endorectal coils. Cost considerations matter but insurance typically covers MRI for appropriate clinical indications. Quality facilities produce reliable results supporting confident clinical decision-making. The combination of clinical value, reasonable patient experience, and typical insurance coverage makes prostate MRI worthwhile component of modern prostate cancer evaluation pathway.
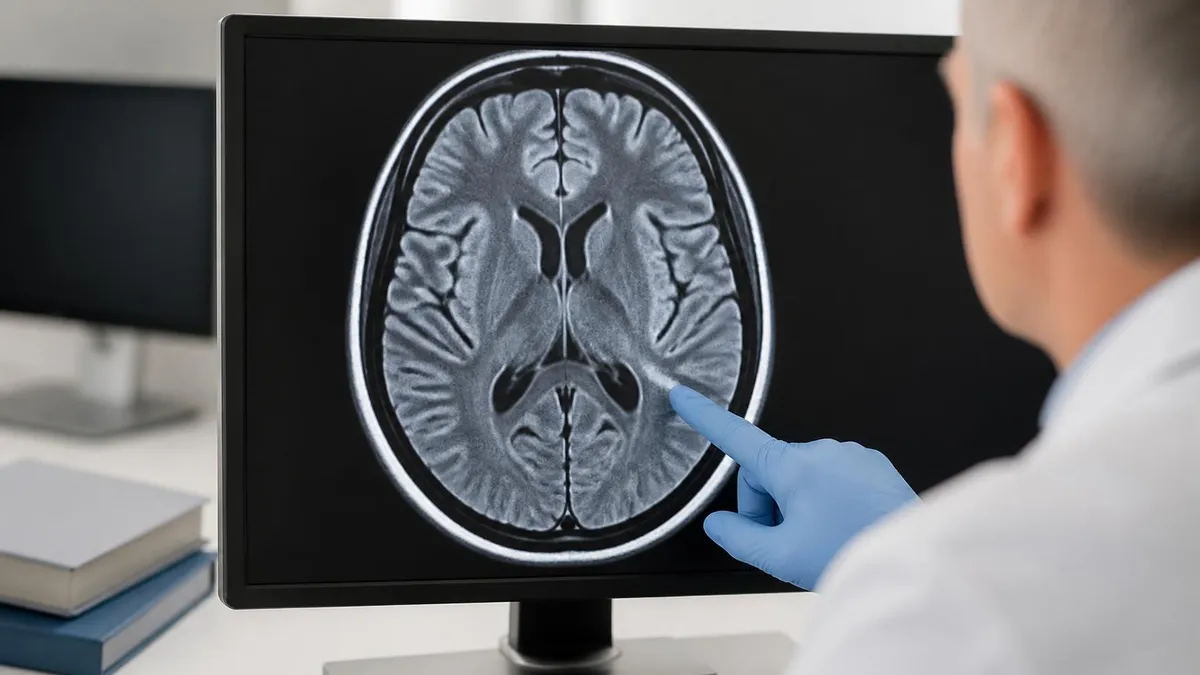
Prostate MRI Quick Stats
PI-RADS Score Implications
Very low probability of clinically significant cancer. Continued surveillance typically appropriate without immediate biopsy.
Low probability of clinically significant cancer. Continued monitoring typically appropriate; biopsy decisions based on other clinical factors.
Intermediate probability. Requires clinical correlation considering PSA trend, family history, prior biopsy results.
High probability of clinically significant cancer. Targeted biopsy of identified lesions typically recommended.
Very high probability of clinically significant cancer. Targeted biopsy strongly recommended.
Highest PI-RADS lesion typically drives clinical decisions. Multiple high-grade lesions warrant comprehensive biopsy approach.
For patients receiving high PI-RADS scores recommending biopsy, several considerations apply. MRI-targeted biopsy more accurately samples concerning lesions than traditional random systematic biopsy. Combined targeted plus systematic biopsy may provide most comprehensive sampling in some situations. Biopsy under local anesthesia typically takes 15-30 minutes with manageable discomfort. Antibiotic prophylaxis prevents infection complications. Most men tolerate biopsy without significant problems. Pathology results typically available within 1-2 weeks. Clear discussion with urologist about biopsy approach, expectations, and follow-up supports informed decision-making and successful procedure experience.
For patients receiving low PI-RADS scores supporting continued surveillance without immediate biopsy, several considerations apply. Continued PSA monitoring detects significant changes. Repeat MRI in 1-2 years (or as clinically indicated) monitors for changes. Discussion with urologist about specific monitoring schedule based on individual risk factors. Lifestyle factors potentially affecting PSA (sexual activity, certain medications, exercise patterns) can be addressed for clearer monitoring trends. The decision to continue surveillance rather than proceed to biopsy involves weighing potential cancer detection benefits against biopsy risks and patient preferences. Quality urological care supports informed decisions through education and ongoing relationship.
For men with family history of prostate cancer, MRI plays particular role in personalized risk assessment. Family history of prostate cancer (particularly in first-degree relatives diagnosed at younger ages) substantially increases personal risk. Genetic testing for BRCA1/BRCA2 mutations and other hereditary cancer predisposition genes affects screening and management decisions. Earlier and more intensive prostate cancer screening including MRI may be appropriate for high-risk men based on family history and genetic testing results. Discussion with primary care physician or urologist about personal risk assessment supports individualized screening approach matching specific risk factors rather than generic population-based recommendations.
For African-American men, prostate cancer represents particular concern given higher incidence and mortality rates compared to other populations. National guidelines recommend earlier screening discussion (starting age 40-45 versus 50 for general population). MRI may have particular value supporting risk-appropriate screening intensity. Cultural and access factors affect appropriate screening implementation requiring culturally-competent care. Discussion with healthcare provider about appropriate screening approach considering individual circumstances and population-specific risks supports best outcomes for higher-risk populations.
For research-minded patients wanting to understand prostate MRI evidence base, several resources support deeper knowledge. PRECISION trial demonstrated MRI-targeted biopsy detects more clinically significant cancer with fewer biopsies than systematic biopsy. PROMIS study established MRI accuracy in prostate cancer detection. Various other research continues building evidence base supporting MRI's central role in prostate cancer evaluation. Patient advocacy organizations including Prostate Cancer Foundation and ZERO provide educational resources about prostate MRI alongside broader prostate cancer information.
Engaged patients bringing knowledge to clinical discussions often achieve better individualized care than passive patients accepting whatever providers recommend without question or critical evaluation of options for their individual prostate cancer evaluation pathway through informed shared decision-making with their healthcare providers and broader treatment team across multiple specialists involved in prostate cancer care.
Prostate MRI: Pros and Cons
- +Improves detection of clinically significant prostate cancer
- +Reduces unnecessary biopsies for low-risk cases
- +Supports targeted biopsy more accurate than systematic
- +Helps distinguish significant from insignificant cancer
- +No ionizing radiation exposure
- +Standardized PI-RADS scoring supports consistent communication
- −Cost ($500-$3,500 without insurance)
- −30-45 minute scan duration in confined space
- −Bowel preparation requirements inconvenient
- −Quality varies across facilities and radiologists
- −Not all suspicious findings represent cancer
- −May miss some cancers despite improved detection
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.