MRI Without Contrast: What It Shows, When It Is Used, and What to Expect
MRI without contrast explained: what it shows, when it is the right choice, accuracy versus contrast MRI, prep steps, scan time, and what radiologists look for.
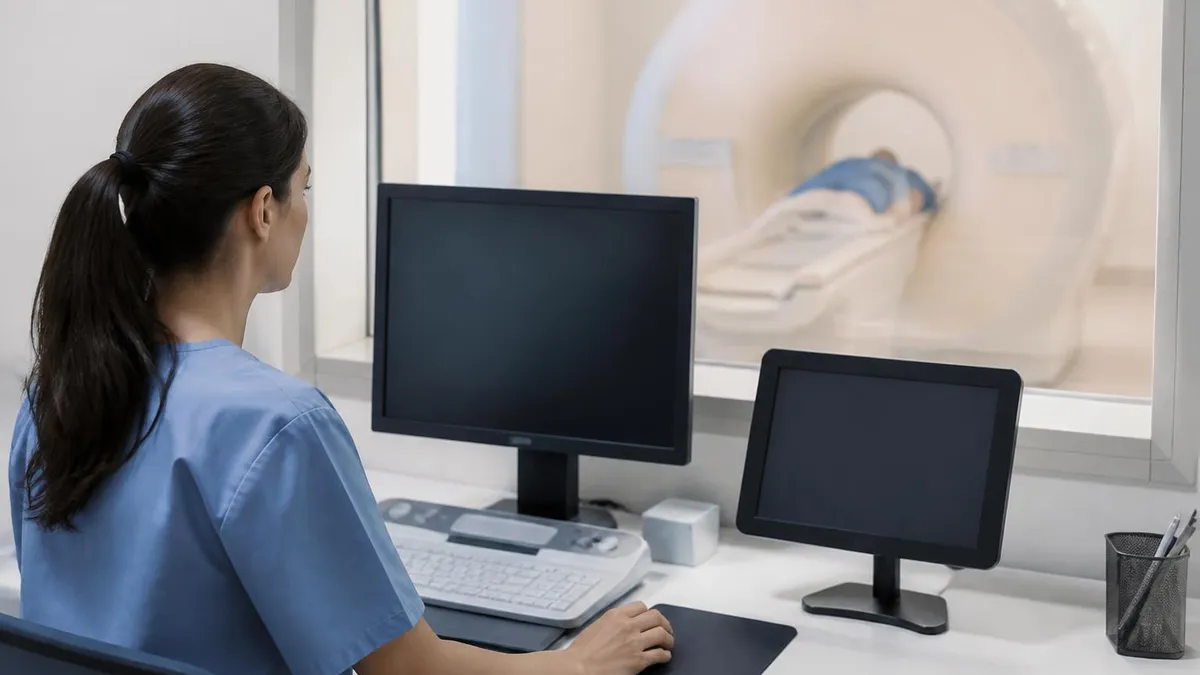
The first question patients ask when they walk into an imaging center holding a referral is usually some version of the same one. "Do I need the dye?" An MRI without contrast means exactly what it sounds like, a magnetic resonance scan performed with no gadolinium injection, and for many indications it is the right test, the safer test, and the test the radiologist actually ordered. Not every MRI needs contrast, and assuming you do can lead to unnecessary IVs, longer scan times, and the small but real risks that come with gadolinium-based agents.
If your doctor wrote "MRI without contrast" on the order, that wording was deliberate. It tells the technologist not to start an IV, signals the radiologist that the answer to the clinical question lives in the native tissue contrast, and usually shortens your appointment by 15 to 25 minutes. But patients still get blindsided at check-in when they learn they will not get the injection they were braced for, or worse, when they discover after the fact that their scan was the no-contrast version and they wonder whether anything was missed.
This guide walks through what an MRI without contrast actually shows, where it shines, where it falls short, when contrast genuinely adds information, and how to prepare for the scan itself. We will also cover what radiologists look for in a non-contrast study, the accuracy compared to contrast-enhanced versions, and the practical questions about cost, scan time, and follow-up imaging that come up in nearly every appointment.
MRI works by aligning protons in the body inside a strong magnetic field, then knocking them out of alignment with radio pulses and listening to how they relax back. Different tissues relax at different rates, which is what produces the contrast you see in the final images. This is called intrinsic or native tissue contrast, and it is the foundation of every scan, with or without gadolinium. When a radiologist orders an MRI without contrast, they are saying that the intrinsic differences between tissues are enough to answer the clinical question.
Most musculoskeletal imaging is non-contrast. A knee MRI for a meniscal tear, a lumbar spine MRI for disc herniation, a shoulder MRI for rotator cuff disease, a wrist MRI for ligament injury, almost all of these are non-contrast studies. The same is true for routine brain MRI screening, stroke imaging in the acute phase, follow-up of known stable findings, and a long list of other indications. Contrast becomes useful when you need to see vascularity, inflammation, infection, breakdown of the blood brain barrier, or tumor enhancement, but those are specific scenarios, not the default.
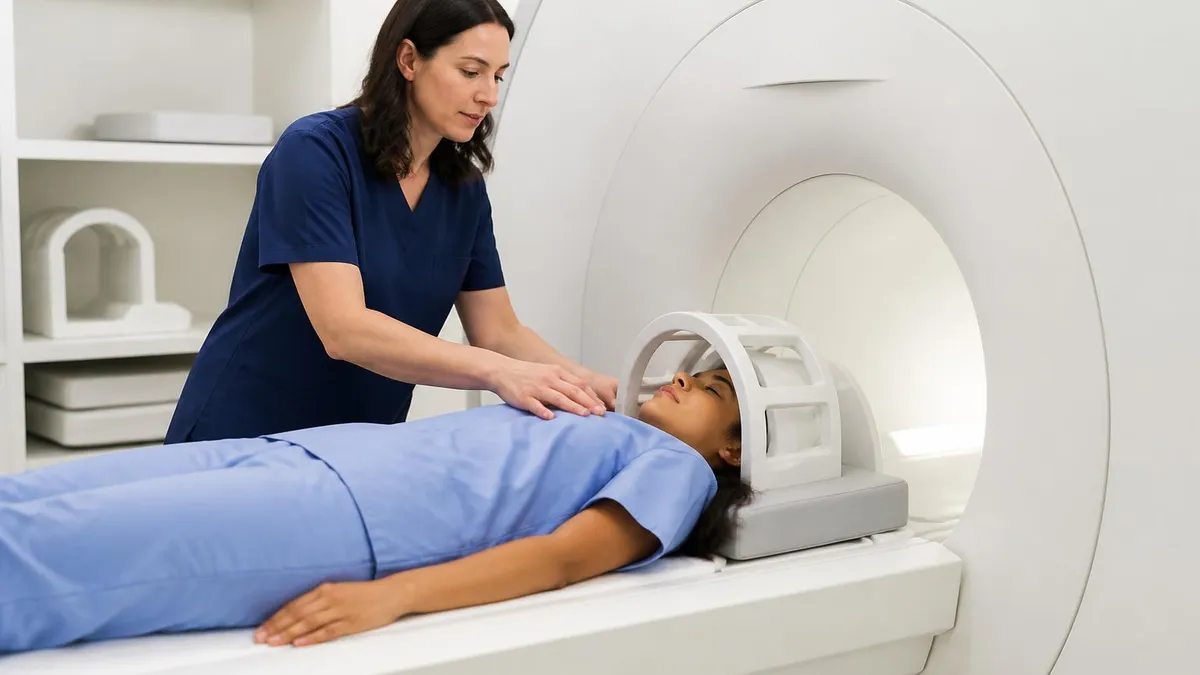
Musculoskeletal injury — Meniscal tears, ligament injuries, rotator cuff disease, labral tears, stress fractures, tendinopathy. Intrinsic tissue contrast is excellent for these.
Routine spine imaging — Disc herniation, degenerative disc disease, spinal stenosis, nerve root impingement without prior surgery. Contrast is generally added only for post-surgical evaluation or suspected infection.
Acute stroke evaluation — Diffusion-weighted imaging in the first hours after symptom onset works without contrast and is the gold standard for early ischemic stroke detection.
Routine brain screening — Headache workup in low-risk patients, follow-up of stable lesions, white matter disease assessment. Contrast is added when tumor, infection, or active inflammation is suspected.
The sequences a radiologist uses on a non-contrast study are the workhorses of MRI. T1-weighted images show fat as bright and water as dark, making them excellent for anatomy, marrow signal, and subacute hemorrhage. T2-weighted images reverse that pattern, with water appearing bright, which is why fluid collections, edema, cysts, and inflammation light up on T2 sequences. Proton density imaging sits between T1 and T2 and is particularly useful for cartilage and ligament evaluation. Fat-saturated sequences suppress the signal from fat so that bone marrow edema, joint effusions, and soft tissue swelling become much more obvious.
Specialized sequences expand what a non-contrast scan can show. Diffusion-weighted imaging picks up restricted water motion, which happens in acute ischemia, abscess, and some tumors. FLAIR sequences null the signal from cerebrospinal fluid so that periventricular and cortical lesions become visible. Susceptibility-weighted imaging detects blood products and calcifications with extreme sensitivity. Time-of-flight MR angiography images blood vessels without needing any injected contrast at all, just relying on the inflow of unsaturated spins into the imaging plane.
Together these sequences cover a huge range of pathology without any need for gadolinium. A skilled radiologist reading a well-acquired non-contrast study can often answer the clinical question definitively. The decision to add contrast is not about getting a better picture in general, it is about answering a specific question that intrinsic contrast cannot reach.
What MRI without contrast can show
Meniscal tears, ACL and PCL injuries, labral tears in the shoulder and hip, rotator cuff tears, Achilles tendon tears, plantar fasciitis, muscle strains, and ligament sprains. Fluid-sensitive sequences make most of these obvious without any contrast.
Disc herniation, disc desiccation, facet arthropathy, spinal stenosis, nerve root compression, and most cases of cord compression. Non-contrast MRI is the first-line study for back and neck pain in patients without prior surgery.
Stress fractures, occult fractures, avascular necrosis, bone bruises, and marrow edema patterns that are invisible on X-ray and CT. Fat-saturated T2 imaging is exquisitely sensitive to marrow changes.
Acute stroke on diffusion imaging, hemorrhage on susceptibility imaging, white matter lesions on FLAIR, and structural abnormalities on T1 and T2. Many emergency brain MRIs are performed without contrast.
MR angiography of the brain, neck, and renal arteries can be performed without any contrast using time-of-flight techniques, which is especially important for patients with kidney disease who cannot receive gadolinium safely.
Initial evaluation of ovarian cysts, uterine fibroids, simple liver cysts, and renal cysts can often be done without contrast. Contrast is added when characterization of a solid mass is required.
The flip side is just as important. There are clinical questions an MRI without contrast cannot answer reliably, and ordering the wrong study wastes time and money. Suspected tumor characterization almost always requires contrast because the pattern of enhancement helps distinguish benign from malignant lesions and identifies the most aggressive part of a tumor for biopsy planning. Suspected infection or abscess often requires contrast to differentiate phlegmon from drainable fluid collections. Multiple sclerosis active disease assessment relies on contrast to identify enhancing lesions, which mark active inflammation versus old plaques.
Post-surgical spine imaging is another classic case where contrast adds critical information. After lumbar discectomy, scar tissue and recurrent disc herniation can look nearly identical on T1 and T2 images. Scar enhances brightly with gadolinium because it is vascularized, while recurrent disc material does not. Without contrast, the radiologist may not be able to tell the surgeon what they need to know. The same principle applies to evaluating possible tumor recurrence after surgery or radiation in any part of the body.
Pituitary microadenomas, small acoustic neuromas, perineural tumor spread, leptomeningeal disease, and early stages of certain infections also benefit substantially from contrast. If your clinical question falls into one of these categories, the radiologist may recommend adding contrast even if the original order was non-contrast, or recommend a follow-up scan with contrast if findings on the non-contrast study are suspicious.
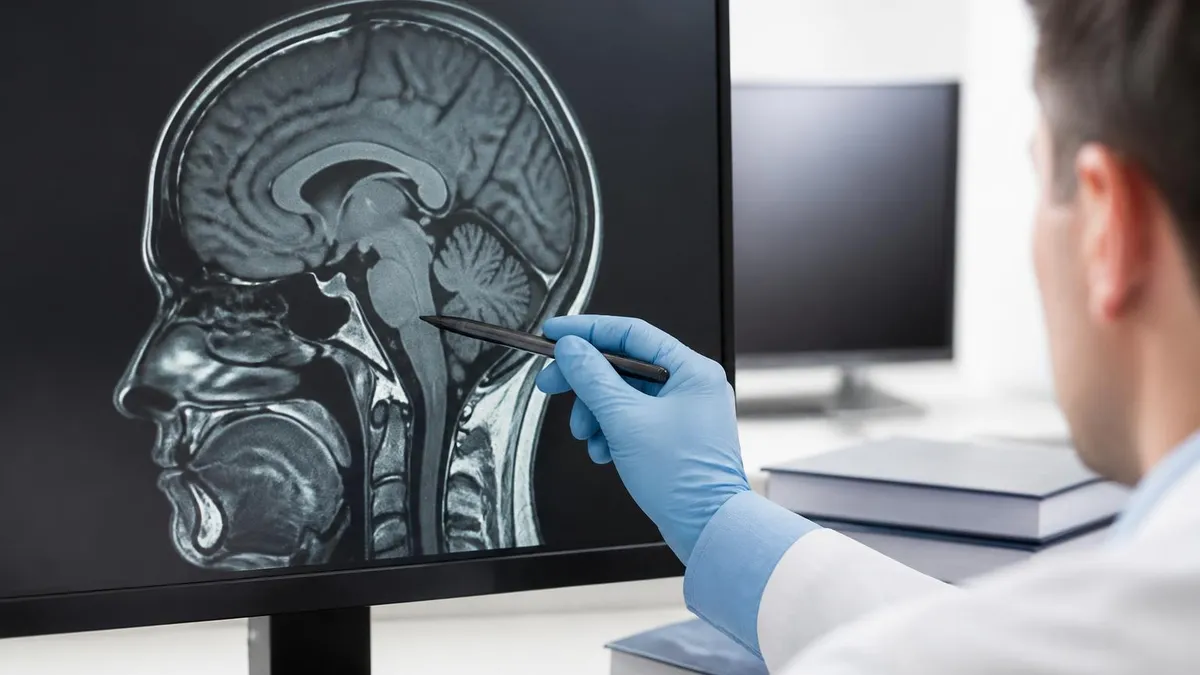
Non-contrast brain MRI is the standard for acute stroke evaluation, headache workup in low-risk patients, follow-up of stable lesions, white matter disease assessment, and screening for structural abnormalities. Contrast is typically added when tumor, abscess, encephalitis, active multiple sclerosis, or leptomeningeal disease is suspected. If the radiologist sees something unexpected on a non-contrast study, they may call to recommend contrast.
Preparing for an MRI without contrast is generally easier than preparing for a contrast study. You do not need an IV, you do not need to confirm normal kidney function, and you do not need a pre-scan blood test in most cases. The basics of MRI safety still apply. You will be asked about any metal implants, surgical clips, pacemakers, cochlear implants, drug delivery pumps, neurostimulators, retained shrapnel, prior eye injuries with metal foreign bodies, and any prior MRI complications. Most modern orthopedic implants are MRI compatible, but the technologist will verify before bringing you to the scanner room.
You will change into a gown or scrubs and remove anything metallic, including jewelry, glasses, watches, hearing aids, dental retainers, hairpins, and underwire bras. Tattoos with metallic ink rarely cause issues but you should mention them. Make-up and certain cosmetics can also contain metallic particles. You may be asked to leave wallets and electronics outside the scanner room because the magnetic field will damage credit cards and wipe magnetic strips.
For body MRIs, you may be asked to fast for four to six hours before the scan if you are getting an abdominal study, but this is more about reducing bowel motion than anything to do with contrast. For brain, spine, and joint imaging, you can eat and drink normally. Take your regular medications unless told otherwise. If you are claustrophobic, your ordering physician can prescribe a mild sedative such as lorazepam to take 30 minutes before the appointment. Wide-bore scanners are also available at most centers and dramatically reduce the closed-in feeling.
Unexpected mass or enhancing-appearing lesion. If a non-contrast study reveals a suspicious mass, the radiologist may recommend completing the study with contrast before you leave the scanner.
Atypical signal characteristics. Some lesions are easy to characterize with intrinsic contrast, others are not. Indeterminate findings often prompt a contrast follow-up.
Clinical change during scan. Rarely, the clinical picture shifts and the radiologist decides additional sequences with contrast are warranted.
Post-operative considerations. If imaging reveals possible recurrent disease or unclear post-surgical findings, contrast helps differentiate scar from active disease.
One of the most common patient questions is whether a non-contrast MRI is somehow less accurate or lower quality than a contrast study. The honest answer is that accuracy depends entirely on what question is being asked. For meniscal tears, the sensitivity and specificity of non-contrast knee MRI are both over 90 percent, far better than any other imaging test.
For acute ischemic stroke, diffusion-weighted imaging without contrast detects infarction within minutes of symptom onset and is far more sensitive than CT. For routine disc herniation in the lumbar spine, non-contrast MRI is the gold standard, and adding contrast would not change diagnosis or management.
On the other hand, for primary brain tumor characterization, contrast adds substantial diagnostic value because the pattern of enhancement helps differentiate glioblastoma from lower-grade gliomas, and identifies the most metabolically active areas. For breast MRI, contrast is essential and a non-contrast breast MRI provides limited information. For evaluating multiple sclerosis activity, contrast distinguishes acute from chronic lesions, which guides treatment decisions.
What this means in practice is that ordering doctors and radiologists choose the right protocol for the right question. If you were scheduled for a non-contrast study, the team has determined that the answer your doctor needs lives in tissue properties that show up without injection. Asking the technologist whether you need contrast just because someone else got contrast for a similar-sounding scan is a fair question, but the answer is almost always that the protocol was tailored to your specific indication.
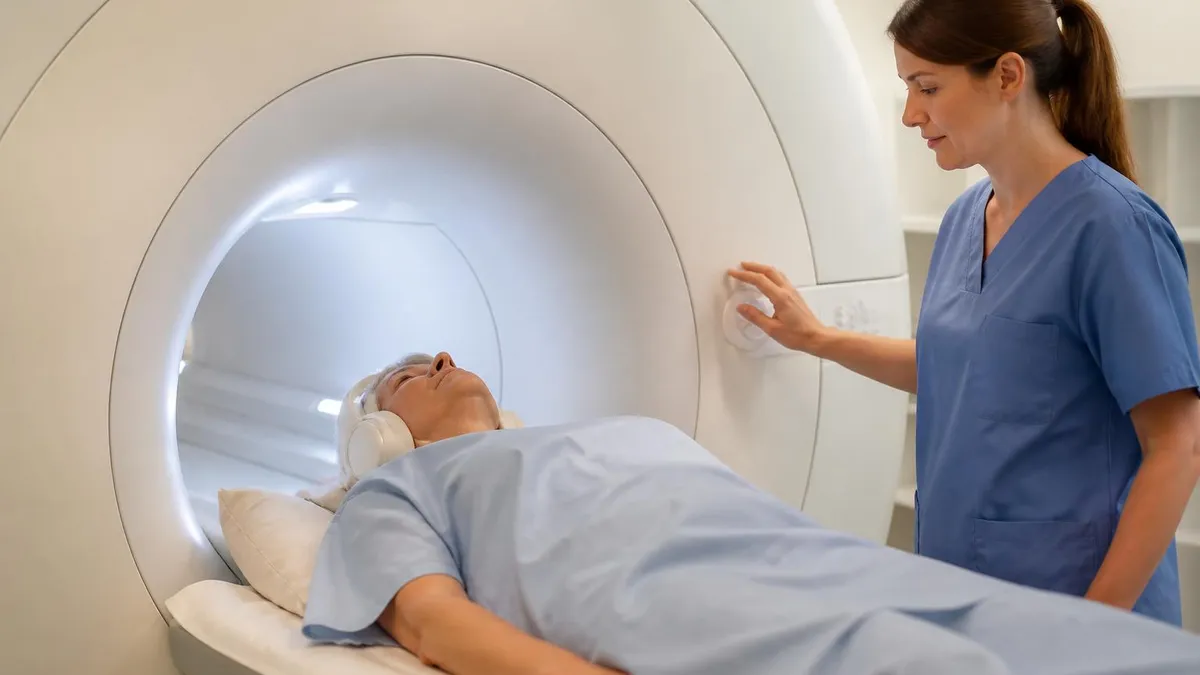
Before your MRI without contrast appointment
- ✓Bring the order or referral with the exact indication clearly written
- ✓List all metal implants, surgical clips, pacemakers, and neurostimulators
- ✓Mention any prior eye injury involving metal fragments
- ✓Remove jewelry, watches, glasses, hearing aids, and dental retainers
- ✓Wear comfortable clothing without metal zippers, snaps, or underwire
- ✓Take your regular medications unless told otherwise
- ✓Discuss claustrophobia with your ordering provider in advance
- ✓Plan to arrive 15-20 minutes early for paperwork and screening
- ✓Bring a list of prior imaging studies for comparison
- ✓Eat normally for brain, spine, and joint scans unless told to fast
What happens during a non-contrast scan looks similar to a contrast scan from the outside, just shorter. You lie on the scanner table, the technologist positions a coil over the body part being imaged, and you are slid into the bore of the magnet. The scan itself runs in a series of acquisition blocks called sequences, each lasting two to seven minutes.
The scanner makes loud knocking, buzzing, and beeping noises during each sequence, which is why you are given earplugs or headphones. Between sequences there is a brief pause where the technologist may check in, then the next acquisition starts.
For a knee MRI without contrast, expect 25 to 35 minutes in the magnet. A lumbar spine MRI takes 30 to 40 minutes. A brain MRI without contrast typically runs 20 to 30 minutes. Abdominal and pelvic scans are usually longer because they involve breath-holding and motion correction. The shorter scan time compared to contrast studies happens because the contrast portion of a scan typically adds 10 to 20 minutes for the injection, the post-contrast sequences, and the brief observation period afterward.
You may be asked to hold still, hold your breath for short intervals, or signal the technologist if you feel unwell. The technologist watches you continuously through a window and can communicate through an intercom. If you need to stop the scan, squeeze the call ball placed in your hand and the technologist will pause the acquisition and check on you. Stopping mid-scan does not damage anything but may require restarting the affected sequence.
After the scan you can leave immediately and resume normal activities. There are no post-scan restrictions for non-contrast studies. Your images are reviewed by a radiologist, who dictates a report that is sent to your ordering physician usually within 24 to 48 hours. Results are not typically given by the imaging center directly because the radiologist's report needs interpretation in the context of your full clinical picture.
MRI without contrast: trade-offs
- +No IV insertion required, faster check-in and check-out
- +Shorter total scan time, typically 20-45 minutes
- +No risk of gadolinium-related reactions or retention
- +Safe for patients with kidney disease
- +Lower cost than contrast-enhanced studies in most regions
- +Excellent diagnostic accuracy for musculoskeletal and most spine indications
- +Time-of-flight angiography can image vessels without any injection
- +Pregnant patients can be imaged when MRI is necessary
- −Cannot characterize most enhancing tumors definitively
- −Limited for detecting active multiple sclerosis lesions
- −Cannot reliably distinguish scar from recurrent disc after spine surgery
- −Less sensitive for small acoustic neuromas and pituitary microadenomas
- −Abscess versus cellulitis or phlegmon characterization is reduced
- −Some perineural and leptomeningeal disease can be missed
- −Vascular characterization is limited compared to dynamic contrast techniques
- −Indeterminate findings may require a follow-up scan with contrast
The cost of an MRI without contrast varies enormously depending on geography, facility type, insurance coverage, and the body part being imaged. In the United States, hospital-based MRI without contrast typically lists at $1,500 to $3,500 before insurance adjustments, with negotiated rates dropping that to $400 to $1,500 in most cases. Outpatient imaging centers, particularly independent radiology groups, often charge significantly less than hospital outpatient departments for the same exam. If you are paying out of pocket or your deductible is high, calling several centers for a cash price quote can save several hundred dollars on the same scan.
Insurance pre-authorization is required for almost all MRI scans, contrast or not. The ordering physician submits the indication to the insurer, who reviews it against medical necessity criteria and approves a specific CPT code. If your scan is denied, your doctor can submit additional clinical information or request a peer-to-peer review. Self-pay patients should ask about prompt pay discounts, which can reduce the bill by 30 to 50 percent at some facilities.
Cost differences between contrast and non-contrast scans usually run $200 to $500 because the contrast media itself, the IV setup, and the additional scan time all add to the facility charge. If your insurance is approving a non-contrast study but you or your physician believe contrast is warranted, that conversation needs to happen before the scan, not after, because adding contrast at the appointment without authorization can result in unexpected bills.
MRI Questions and Answers
The simplest framing for understanding when an MRI without contrast is the right choice is this. The scan answers questions about anatomy, tissue water content, fat distribution, marrow signal, vascular flow patterns, and acute changes in water diffusion. It does not answer questions about vascularity at the level of small enhancing lesions, the active inflammatory state of plaques, or the degree of breakdown of biological barriers like the blood-brain barrier. For the first set of questions, non-contrast MRI is excellent. For the second set, contrast is essential.
Most patients who get an MRI scan in their lifetime will have at least one non-contrast study, and many will never need a contrast scan at all. The fact that your scan was ordered without contrast is not a sign that anything was skipped or shortchanged. It is a sign that your ordering team chose the test that fits your clinical situation, and a sign that the radiologist will have the information they need to answer the question on the order.
If you have specific concerns about whether a contrast scan might be warranted in your case, the conversation to have is with your ordering physician before the scan, not at the appointment. The technologist and the radiologist follow the protocol on the order, and adding contrast at the last minute introduces logistical, insurance, and clinical complications. A good rule of thumb is that if you are unsure, ask your doctor to walk you through why a non-contrast study answers their question. Most of the time, the explanation makes intuitive sense.
And if your scan finds something unexpected that does need contrast for full characterization, the radiology team will reach out and arrange the follow-up. The two-step approach, a non-contrast screening first and a targeted contrast study only if needed, is often the most efficient and patient-friendly use of imaging resources. It avoids unnecessary IVs and contrast exposure for the majority of patients while preserving the ability to drill down on cases that need it.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.