MRI Radiation: Complete Guide to Magnetic Resonance Imaging Safety
Complete guide to MRI radiation covering whether MRI uses ionizing radiation, magnetic field safety, contrast agent considerations, and comparison with CT...
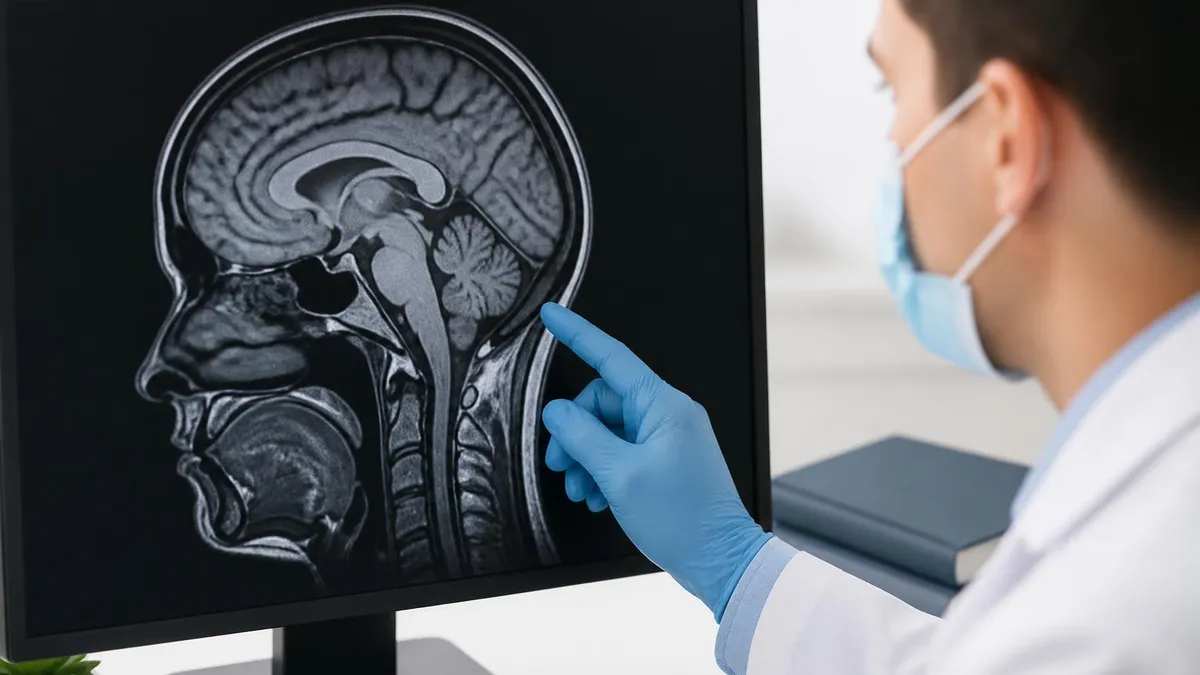
MRI does not use ionizing radiation unlike X-rays or CT scans making it among the safest medical imaging technologies for radiation exposure concerns. Magnetic Resonance Imaging uses strong magnetic fields and radio waves producing detailed images of body interior without the ionizing radiation that other imaging technologies require. Understanding MRI radiation differs from common imaging assumptions supports informed patient decisions about imaging choices when multiple imaging options exist for specific medical questions.
Ionizing radiation refers to high-energy electromagnetic radiation including X-rays, gamma rays, and various other forms that can damage DNA potentially causing cancer with sufficient cumulative exposure. CT scans, traditional X-rays, mammography, and various other imaging technologies use ionizing radiation. PET scans combine ionizing radiation with metabolic imaging through injected radioactive tracers. Nuclear medicine studies use various radioactive substances. The various ionizing radiation imaging technologies provide valuable diagnostic information while requiring careful management of cumulative radiation exposure across patient lifetimes.
Non-ionizing radiation including magnetic fields and radio waves used in MRI does not damage DNA in same way as ionizing radiation. The fundamental physical difference between non-ionizing and ionizing radiation reflects different energy levels with non-ionizing being substantially lower energy than ionizing. While substantial magnetic field exposure can cause specific safety concerns particularly with metal implants, the magnetic fields do not produce cancer risks from cumulative exposure in same way as ionizing radiation. The radiation safety distinction makes MRI substantially safer than ionizing radiation imaging for most patients.
Historical context for MRI development reflects Nobel Prize winning research. Felix Bloch and Edward Purcell received 1952 Nobel Prize in Physics for nuclear magnetic resonance work providing physical foundation for MRI. Paul Lauterbur and Peter Mansfield received 2003 Nobel Prize in Medicine for MRI imaging development. The substantial scientific recognition reflects MRI fundamental importance to medical imaging. Continuing technological advancement has produced increasingly capable MRI systems while maintaining the radiation safety advantages of the underlying physics.
Cancer screening considerations affect imaging modality choices including MRI and CT options. Breast MRI supports high-risk patient screening alongside mammography. Whole body MRI screening exists in some contexts though not universally recommended. The radiation safety advantages of MRI for screening contexts particularly matters since screening involves repeated imaging of healthy individuals where any cancer risk from imaging itself must be minimized. The screening applications of MRI continue evolving as research clarifies optimal screening approaches.
Insurance coverage variations affect MRI accessibility across patient populations. Most major insurance plans cover medically necessary MRI scans though specific authorization requirements may apply. Some plans require step-up approaches trying less expensive imaging before authorizing MRI. Out-of-pocket costs for MRI scans without insurance can range from 400 to 3,500 dollars depending on body region and facility. Insurance variations affect specific patient experiences with MRI scheduling and costs.
MRI does not use ionizing radiation unlike CT scans, X-rays, and mammography. MRI uses magnetic fields and radio waves producing detailed images without DNA damage risks from ionizing radiation. MRI safety concerns relate to metal implants and very loud noise rather than radiation exposure. Comparison with CT scans shows MRI as safer imaging choice when both options provide equivalent diagnostic information.
MRI offers substantial diagnostic capability without ionizing radiation exposure supporting both patient safety and excellent clinical imaging across diverse medical applications.
Magnetic field strength in MRI systems typically ranges from 1.5 Tesla to 3 Tesla for clinical use with some research systems operating at 7 Tesla or higher. The strong magnetic field attracts ferromagnetic materials potentially causing serious injuries if metal objects enter the MRI room. Pacemakers, certain surgical implants, metallic foreign bodies, and various other ferrous materials may exclude patients from MRI scanning. Modern MRI-safe implants increasingly support patient access to MRI imaging though specific implant verification before scanning prevents potentially serious incidents.
Radio frequency exposure during MRI produces minor heating in body tissues from absorbed radio wave energy. The specific absorption rate is carefully managed during MRI scans staying within established safety limits. Most patients experience no perceptible heating effects from MRI scanning. Some patients with specific medical conditions or implants may have specific radio frequency considerations during scanning. The carefully managed radio frequency exposure produces no demonstrated health risks for typical patients in routine clinical MRI scanning.
MRI technical principles involve hydrogen atom nuclei alignment with magnetic field. Radio frequency pulses temporarily disrupt this alignment. Returning to magnetic alignment produces detectable radio signals creating images. The fundamental physics avoids ionizing radiation while providing detailed imaging capability. Understanding basic principles helps patients appreciate why MRI differs from ionizing radiation imaging supporting informed patient discussions during medical care.
Quality variation across MRI facilities affects examination results. Hospital-based MRI departments typically have substantial expertise and equipment. Outpatient imaging centers may offer more convenient scheduling and lower costs. Mobile MRI services support smaller communities without permanent MRI facilities. Each setting has specific characteristics affecting patient experience. Quality factors include radiologist expertise interpreting scans, MRI equipment quality, technologist experience, and various other factors affecting overall examination quality.
MRI vs Other Imaging
No ionizing radiation. Uses magnetic fields and radio waves. Excellent for soft tissue imaging. Long scan times. Loud noise. Metal implant concerns. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Uses ionizing radiation typically 100-1000 times more than chest X-ray. Fast scanning. Excellent for bone and acute imaging. Cumulative radiation exposure concerns. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Uses ionizing radiation in low doses. Quick imaging. Limited soft tissue detail. Common for bone fractures and chest imaging. Cumulative exposure tracking matters. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
No ionizing radiation. Uses sound waves. Real-time imaging. Limited tissue penetration. Operator-dependent quality. Excellent for various soft tissue conditions. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Combines ionizing radiation with metabolic imaging through radioactive tracer injection. Substantial radiation exposure. Excellent for cancer and metabolic studies. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Various studies using radioactive substances. Specific radiation exposure depending on study type. Specialized functional imaging beyond just anatomical structure. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Contrast agents used in MRI typically include gadolinium-based contrast media supporting enhanced visualization of certain tissues. Gadolinium contrast does not contain ionizing radiation though has specific safety considerations including rare but serious nephrogenic systemic fibrosis risk in patients with severe kidney disease. Most patients tolerate gadolinium contrast well without adverse effects. Specific kidney function evaluation before contrast administration supports identifying patients at risk for adverse reactions to gadolinium contrast administration.
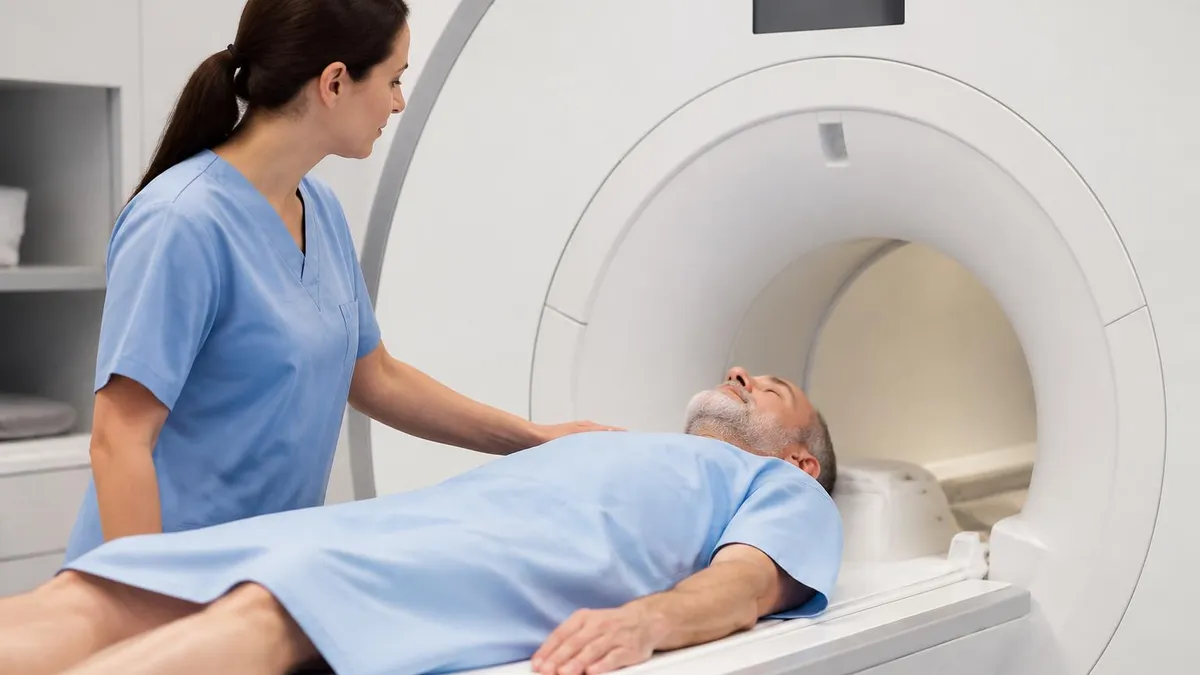
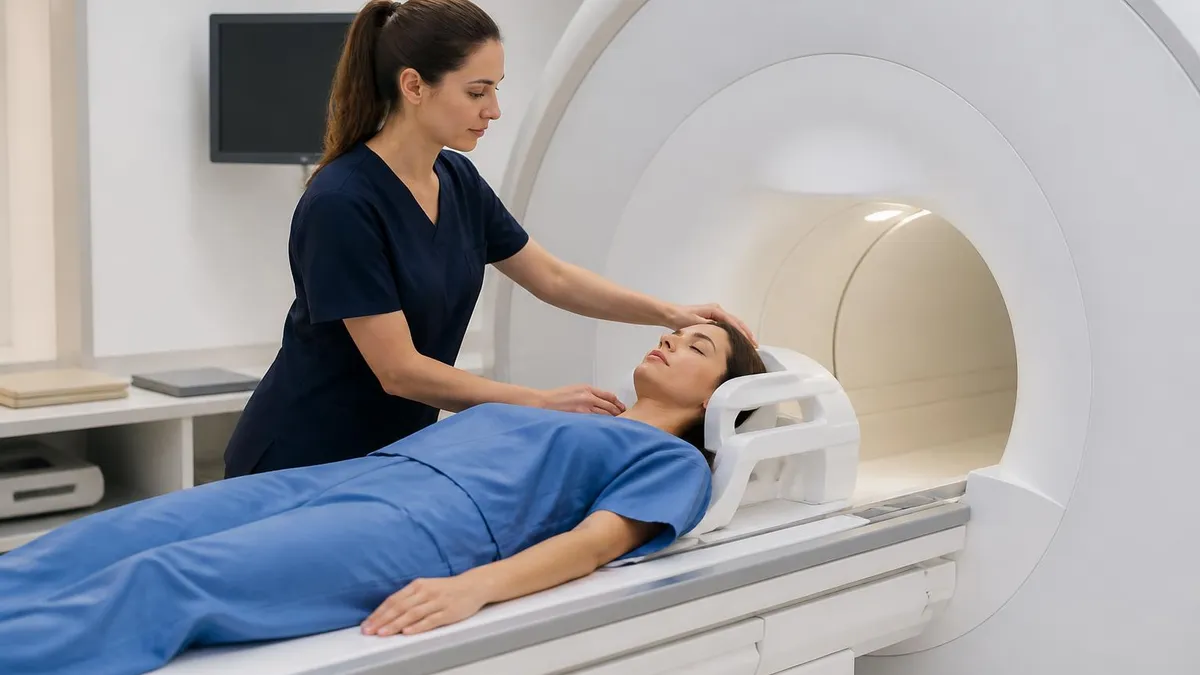
Patient experience during MRI differs substantially from CT or X-ray imaging. MRI scans typically take 20 to 60 minutes longer than CT or X-ray. Patients lie still in narrow tube enclosure with loud knocking and buzzing noises from MRI scanner. Some patients experience claustrophobia during scans. Hearing protection through earplugs or headphones reduces noise exposure. Open MRI systems support patients with claustrophobia through more open scanner design though may have lower image quality than closed systems. The patient experience considerations affect specific MRI scheduling decisions.
MRI sequence variety supports diverse clinical applications. T1-weighted sequences provide anatomical detail. T2-weighted sequences highlight pathological conditions. FLAIR sequences support specific neurological applications. Various other specialized sequences address specific clinical needs. The substantial sequence variety supports comprehensive evaluation through single MRI examination producing rich diagnostic information beyond what single imaging approach could provide alone.
Comparison with other non-radiation imaging including ultrasound shows complementary roles. Ultrasound provides real-time imaging with portable equipment supporting various applications particularly obstetric imaging. MRI provides detailed static images with substantial equipment supporting various other applications. Both technologies avoid ionizing radiation though through different physical principles. The complementary nature supports both technologies coexisting in modern medical imaging rather than competing for same applications.
MRI Safety Considerations
MRI uses magnetic fields and radio waves without ionizing radiation. This represents major safety advantage over CT scans and other ionizing radiation imaging. Patients can undergo multiple MRI scans without cumulative radiation exposure concerns. MRI is preferred for repeat imaging when both MRI and CT could provide equivalent diagnostic information. The radiation safety supports broad MRI use across various patient populations including pregnant women and children where radiation exposure concerns matter substantially.
Each safety consideration affects specific patient situations supporting informed discussions with healthcare providers about MRI as imaging option.
Pregnancy considerations for MRI differ from other imaging due to absence of ionizing radiation. MRI scanning during pregnancy is generally considered safe particularly after first trimester. The lack of ionizing radiation makes MRI preferred imaging modality when imaging needed during pregnancy. Specific recommendations may apply for first trimester scans with risk-benefit consideration for each specific clinical scenario. Contrast agent use during pregnancy requires careful consideration with most providers avoiding gadolinium contrast during pregnancy except in specific clinical circumstances.
Pediatric MRI considerations include radiation safety advantage over CT plus specific challenges with patient cooperation during long scans. Young children may require sedation or general anesthesia to remain still during MRI. Open MRI systems support pediatric scanning when claustrophobia is concern. The radiation safety advantage particularly matters for pediatric patients given longer expected lifetimes during which radiation exposure could potentially cause cancer. MRI use in pediatric imaging continues expanding as protocols develop addressing pediatric-specific scanning challenges.
Open MRI systems address claustrophobia concerns through more open scanner design. Traditional closed MRI requires patients to lie inside narrow tube. Open MRI systems provide more open space accommodating claustrophobic patients. However open MRI typically operates at lower field strength affecting image quality. The trade-off between patient comfort and image quality affects specific scanning decisions. Some facilities offer both closed and open MRI supporting patient choice based on individual needs and clinical considerations.
Future developments may continue advancing MRI capabilities. Higher field strength systems support better image quality. Faster scanning techniques reduce examination times. Specialized contrast agents support new applications. Artificial intelligence applications support image acquisition and interpretation. The continuing advancement maintains MRI relevance while preserving fundamental radiation safety advantages over ionizing radiation imaging technologies across various clinical applications throughout medical practice.
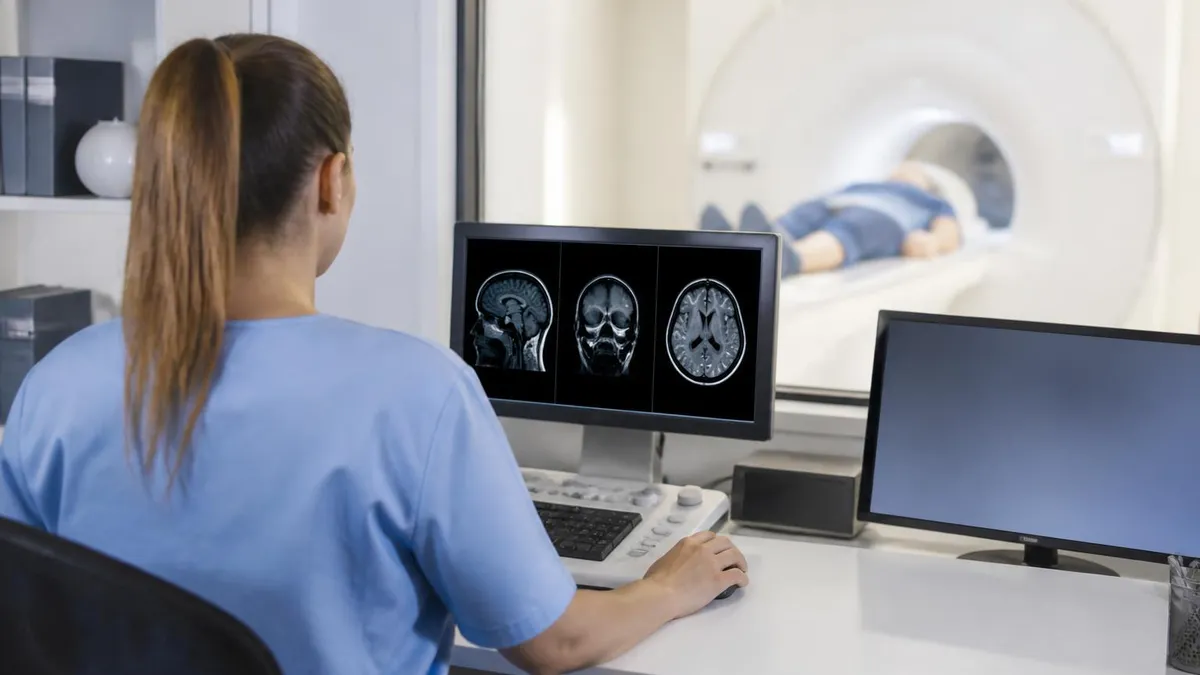
Despite MRI not using ionizing radiation, MRI has specific safety considerations including metal implants, claustrophobia, and contrast agent reactions. Complete MRI safety screening before scanning identifies potential issues. Disclose all surgical implants, medical devices, metallic foreign bodies, kidney problems, and allergies to MRI staff before scanning supporting safe examination.
MRI safety screening represents critical step before any scan. Disclose all implants, devices, allergies, and medical conditions to MRI staff before scanning supporting safe examination outcomes.
Common patient concerns about MRI radiation reflect general public confusion about different imaging types. Many patients assume all medical imaging involves radiation similar to CT or X-ray. Understanding MRI uses different technology without ionizing radiation supports informed patient discussions with healthcare providers. The educational opportunity during MRI scheduling supports patient comfort and informed consent for procedures. Healthcare providers increasingly emphasize this distinction when discussing imaging options with patients facing imaging decisions.
Cumulative radiation exposure concerns affect patients undergoing multiple imaging studies over time. Patients with chronic conditions requiring frequent imaging may face substantial cumulative radiation from CT scans. MRI alternative when clinically appropriate avoids the cumulative radiation concerns. Some patients specifically request MRI over CT when both options are available though clinical considerations beyond just radiation should guide imaging choices. The cumulative exposure consideration represents legitimate concern affecting various patient situations.
Wide bore MRI represents middle ground between standard closed MRI and open MRI. Wide bore systems use closed tube design with larger diameter than standard MRI accommodating claustrophobic patients somewhat better. Most wide bore systems operate at full clinical field strength preserving image quality. The wide bore option provides patient comfort improvement without quality sacrifice though may not fully address severe claustrophobia like open MRI systems would.
MRI Preparation
- ✓Complete MRI safety screening form identifying any implants, devices, or other concerns
- ✓Disclose all surgical implants and medical devices to MRI staff before scanning
- ✓Remove all metallic objects including jewelry, watches, and various other metal items
- ✓Inform staff about claustrophobia concerns supporting potential open MRI scheduling or sedation
- ✓Discuss kidney problems if MRI will use gadolinium contrast for enhanced imaging
- ✓Bring list of current medications and known allergies for MRI staff review
- ✓Plan for hour-long appointment supporting full scan completion without rushing
- ✓Wear comfortable clothing without metallic decorations or hardware for scanning convenience
- ✓Arrange transportation if sedation will be used during scanning preventing self-driving home
Functional MRI represents specialized MRI application studying brain activity through blood oxygenation level dependent imaging. fMRI uses standard MRI technology without ionizing radiation while providing functional information about brain activity beyond just anatomical structure. The specialized application supports neuroscience research and various clinical applications. Functional MRI maintains the radiation safety advantages of standard MRI while providing additional functional information beyond anatomical imaging alone supporting diverse research and clinical applications.
Diffusion MRI represents another specialized MRI application studying water molecule movement in tissues. The technique supports stroke diagnosis, white matter pathway visualization, and various other applications. Like all MRI applications, diffusion MRI uses no ionizing radiation. The continuing development of specialized MRI techniques expands diagnostic capabilities while maintaining the radiation safety advantages over CT and other ionizing radiation imaging technologies producing safer comprehensive imaging across diverse clinical needs.
Pediatric MRI considerations include several specific factors. Young children may require sedation or general anesthesia to remain still during long scans. Specialized pediatric MRI staff support child comfort during scanning. Pediatric protocols adapt scanning to pediatric anatomy and clinical questions. The radiation safety advantage particularly matters for pediatric patients given their longer expected lifetimes. MRI in pediatric imaging continues expanding as protocols develop addressing pediatric-specific challenges.
Cost considerations for MRI typically exceed CT scan costs due to longer scan times and more expensive equipment. Insurance coverage typically supports MRI when medically necessary though specific insurance considerations may affect specific cases. Some insurance plans require preauthorization for MRI scans particularly when CT scan alternatives could provide similar information. The cost consideration affects healthcare resource allocation though radiation safety advantages of MRI support its use when clinically appropriate despite higher costs than alternative imaging.
Comparison with ultrasound shows both technologies avoid ionizing radiation though through different physical principles. Ultrasound uses sound waves providing real-time imaging with portable equipment supporting bedside use. MRI uses magnetic fields producing detailed anatomical images requiring substantial equipment. Each technology has specific strengths with ultrasound preferred for obstetric imaging and various other applications while MRI excels for detailed anatomical visualization of various body regions and tissues.
Common clinical MRI applications include brain imaging for various neurological conditions, spine imaging for back pain evaluation, joint imaging for orthopedic conditions, abdominal imaging for various organ conditions, breast imaging for cancer evaluation, and cardiac imaging for heart conditions. Each application uses specific protocols matching clinical questions. The diverse applications reflect MRI versatility across virtually all body regions and medical specialties supporting comprehensive medical imaging needs without ionizing radiation exposure across these various clinical contexts.
MRI vs Imaging Comparison
MRI Strengths
Exceptional soft tissue contrast and detail compared to other imaging modalities. Preferred for many neurological, musculoskeletal, and abdominal imaging applications. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Zero ionizing radiation exposure makes MRI safer than CT scans for repeated imaging needs and pediatric or pregnant patients. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Direct imaging in any plane without repositioning patient. Multiple imaging sequences during single examination supporting comprehensive evaluation. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Functional MRI variants support brain activity imaging, diffusion studies, and various other functional applications beyond just anatomical structure. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
High sensitivity for various tissue characteristics including inflammation, hemorrhage, and various pathological conditions beyond just structural abnormalities. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
MR angiography supports vascular imaging without ionizing radiation alternative to CT angiography for various vascular conditions. Specific clinical considerations support choosing appropriate imaging modality for individual patient situations.
Future MRI developments continue expanding capabilities while maintaining radiation safety. Higher field strength systems support better image quality. Faster scanning techniques reduce examination times. New contrast agents support specialized imaging applications. Artificial intelligence applications support image interpretation and acquisition optimization. The continuing technological advancement maintains MRI relevance as essential medical imaging technology while preserving its fundamental advantage of using non-ionizing radiation for diagnostic imaging across diverse clinical applications.
Patient advocacy through informed imaging decisions includes understanding when MRI provides appropriate alternative to CT scanning. Patients facing imaging recommendations can ask whether MRI alternative would provide equivalent diagnostic information without radiation exposure. Healthcare providers typically consider radiation exposure in imaging recommendations though patient preferences may affect specific choices. The informed patient discussion supports both better clinical decisions and patient comfort about imaging procedures across various medical situations.
Patient empowerment through understanding imaging options supports informed healthcare decisions. Asking healthcare providers about MRI alternatives to CT scans when appropriate represents legitimate patient advocacy. Understanding the fundamental difference between MRI and ionizing radiation imaging supports informed discussions about imaging choices. Patients facing imaging recommendations benefit from understanding what radiation exposure their specific imaging would involve when considering recommended procedures across various medical situations.
Continued advancement in MRI technology and clinical applications supports ongoing improvement in medical imaging capabilities while maintaining the fundamental radiation safety advantage that distinguishes MRI from ionizing radiation alternatives across diverse clinical contexts and patient populations.
Healthcare providers increasingly emphasize the radiation safety advantages of MRI when discussing imaging options with patients facing various medical questions affecting their treatment decisions.
The clinical role of MRI continues expanding across medical specialties supporting diverse diagnostic needs.
MRI technology continues benefiting patients across medical practice.
MRI Imaging Considerations
- + —
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
- − —
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.