Does MRI Cause Cancer
Can MRI cause cancer? MRI uses no ionizing radiation eliminating cancer risk from imaging. Learn the facts about MRI safety profile.
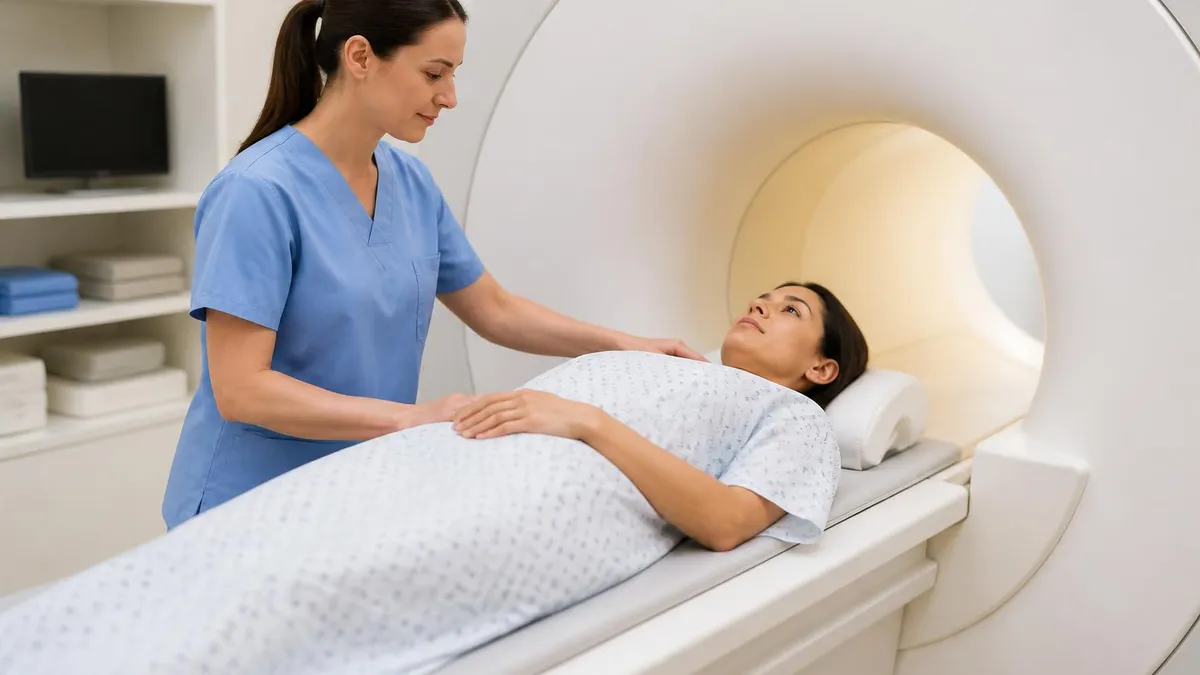
The question of whether MRI scanning causes cancer represents common concern for patients undergoing or considering MRI imaging. MRI scanners use strong magnetic fields and radiofrequency waves to produce diagnostic images without ionizing radiation. Unlike X-rays, CT scans, and nuclear medicine imaging that use ionizing radiation potentially associated with cancer risk, MRI does not use ionizing radiation eliminating direct cancer risk from radiation exposure during scanning. The basic physics of MRI imaging produces no ionizing radiation supporting safety profile that does not include cancer risk from radiation exposure.
Understanding MRI safety helps patients make informed decisions about imaging options. Many patients confuse different imaging types thinking MRI uses radiation similar to X-rays or CT scans. The confusion produces unnecessary anxiety about cancer risk from MRI. Learning the actual physics of MRI imaging supports informed decisions matching the actual safety profile of MRI versus radiation-based imaging. The MRI safety advantage compared to radiation imaging makes MRI preferred option for many clinical situations particularly for patients requiring multiple imaging studies or younger patients with longer life expectancy supporting cumulative imaging considerations.
This guide explains MRI safety regarding cancer risk, the physics of MRI imaging, comparison with radiation-based imaging including X-rays and CT scans, gadolinium contrast considerations, specific patient situations affecting MRI decisions, comparison with alternative imaging options, and various other aspects affecting MRI safety understanding. Whether you are considering single MRI or multiple MRI scans for ongoing care, understanding MRI safety regarding cancer risk supports informed decisions matching evidence-based assessment of MRI versus alternative imaging options across various clinical situations requiring diagnostic imaging.
MRI Safety Key Statistics
MRI imaging physics differs fundamentally from radiation-based imaging. Magnetic resonance imaging uses strong static magnetic fields, gradient magnetic fields, and radiofrequency waves to manipulate hydrogen atoms in body tissues producing diagnostic images. The radiofrequency waves used in MRI fall in the radio wave portion of electromagnetic spectrum operating at energy levels far below ionizing radiation threshold. These non-ionizing radiofrequency waves do not have enough energy to damage DNA or produce cellular changes potentially leading to cancer development. The fundamental physics of MRI eliminates cancer risk from imaging process itself.
Ionizing radiation refers to electromagnetic waves or particles with enough energy to remove electrons from atoms producing ions in tissues. X-rays, gamma rays, and certain particle radiation have enough energy to damage DNA potentially producing cellular changes that may lead to cancer over time. CT scans, nuclear medicine, fluoroscopy, and various other imaging types use ionizing radiation producing measurable cancer risk that increases with cumulative radiation dose. The radiation-based imaging types require careful consideration of risk versus diagnostic benefit particularly for younger patients and those requiring multiple imaging studies.
The non-ionizing nature of MRI radiofrequency waves and magnetic fields produces no measurable cancer risk from imaging exposure. Decades of research and clinical experience support MRI safety regarding cancer development. Large studies including population studies and animal research have found no association between MRI exposure and cancer risk. The accumulated evidence supports MRI as safe imaging option from cancer risk perspective. Patients can undergo multiple MRI scans throughout life without cumulative cancer risk concerns associated with radiation-based imaging types affecting alternative diagnostic approaches.

MRI uses non-ionizing radiofrequency waves and magnetic fields producing zero direct cancer risk from imaging process. X-rays use ionizing radiation with measurable but typically very small cancer risk increase. CT scans use higher ionizing radiation doses than X-rays producing slightly higher cancer risk consideration. Nuclear medicine scans use radioactive tracers producing internal radiation exposure with cancer risk considerations. PET scans combine CT and nuclear medicine radiation. Mammography uses low-dose X-rays with controlled radiation exposure. The radiation imaging types have specific cancer risk considerations balanced against diagnostic benefits for specific clinical situations affecting imaging selection decisions across various patient circumstances and medical needs.
Gadolinium contrast agents used in some MRI scans represent separate safety consideration distinct from radiation cancer risk. Gadolinium-based contrast agents enhance specific MRI images supporting better diagnosis of various conditions. The gadolinium contrast is administered intravenously when needed for specific imaging questions. Safety considerations include allergic reactions, kidney function affecting contrast clearance, and rarely nephrogenic systemic fibrosis in patients with severe kidney disease. The gadolinium safety considerations are distinct from cancer risk and managed through screening protocols matching individual patient circumstances.
Gadolinium retention in body tissues represents area of ongoing research without established cancer connection. Recent research has shown that some gadolinium contrast may be retained in brain tissues, bone, and other body areas following contrast administration. The clinical significance of gadolinium retention remains unclear. Long-term studies have not established cancer association with gadolinium retention. Different gadolinium contrast formulations have different retention profiles affecting specific agent selection decisions. The retention research has supported updated guidelines for gadolinium use but has not changed MRI cancer risk assessment from imaging exposure perspective.
The strong magnetic fields of MRI scanners do not produce cancer risk. The static magnetic field strength of 1.5 to 3 Tesla used in clinical MRI is much stronger than Earth magnetic field though produces no ionizing effects. The gradient magnetic fields that change during scanning produce minor effects including peripheral nerve stimulation feelings in some patients though produce no cancer risk. The combined magnetic field exposure during MRI has been extensively studied without finding cancer association. The magnetic field safety supports MRI as preferred option from cancer risk perspective compared to radiation-based imaging.
Imaging Types and Cancer Risk Comparison
Uses non-ionizing radiofrequency and magnetic fields with zero ionizing radiation exposure. No measurable cancer risk from imaging process. Preferred for multiple scan situations and younger patients due to safety profile.
Uses ionizing radiation in controlled doses with very small cancer risk per scan. Different body parts require different radiation doses. Standard chest X-ray exposure equivalent to background radiation over several days exposure.
Uses higher ionizing radiation doses than X-rays producing slightly increased cancer risk. CT chest equivalent to several years background radiation. Risk balanced against diagnostic benefit for specific clinical situations.
Uses radioactive tracers producing internal radiation exposure. Different scans have different radiation doses. Risk considerations balanced against unique diagnostic information from nuclear medicine techniques unavailable from other imaging.
Uses sound waves with no ionizing radiation producing zero cancer risk from imaging. Limited tissue penetration affects specific applications. Often combined with MRI for comprehensive imaging without radiation exposure.
Uses low-dose X-rays with controlled radiation exposure. Screening mammography balances small radiation cancer risk against breast cancer detection benefits. Specific schedule recommendations match individual risk profiles.
Pediatric imaging benefits substantially from MRI safety profile regarding radiation exposure. Children have longer life expectancy supporting more time for radiation-induced cancer development. Pediatric tissues may be more sensitive to radiation effects than adult tissues affecting cancer risk considerations. The MRI absence of ionizing radiation makes MRI preferred option for many pediatric imaging needs when MRI provides adequate diagnostic information. The pediatric MRI preference reduces cumulative radiation exposure during childhood supporting better long-term safety profile across imaging needs throughout pediatric care.
Cancer surveillance imaging often involves multiple imaging studies over years affecting cumulative radiation exposure considerations. Patients with cancer history requiring surveillance imaging benefit from MRI preference when MRI provides adequate diagnostic information for surveillance purposes. The cumulative radiation exposure from repeated CT scans for surveillance produces meaningful cancer risk consideration over time. MRI surveillance avoids the cumulative radiation issue supporting better long-term safety profile for ongoing cancer surveillance imaging needs across various cancer types requiring imaging follow-up.
Pregnancy considerations affect imaging decisions substantially. MRI without contrast generally considered safe during pregnancy though typically avoided in first trimester due to limited specific safety data. The MRI absence of ionizing radiation supports MRI preference over CT scanning during pregnancy when imaging needed. Gadolinium contrast typically avoided during pregnancy due to placental transfer considerations. The MRI safety advantage during pregnancy makes MRI valuable option for diagnostic imaging when needed during pregnancy supporting both maternal and fetal safety considerations across various clinical situations requiring imaging during pregnancy.
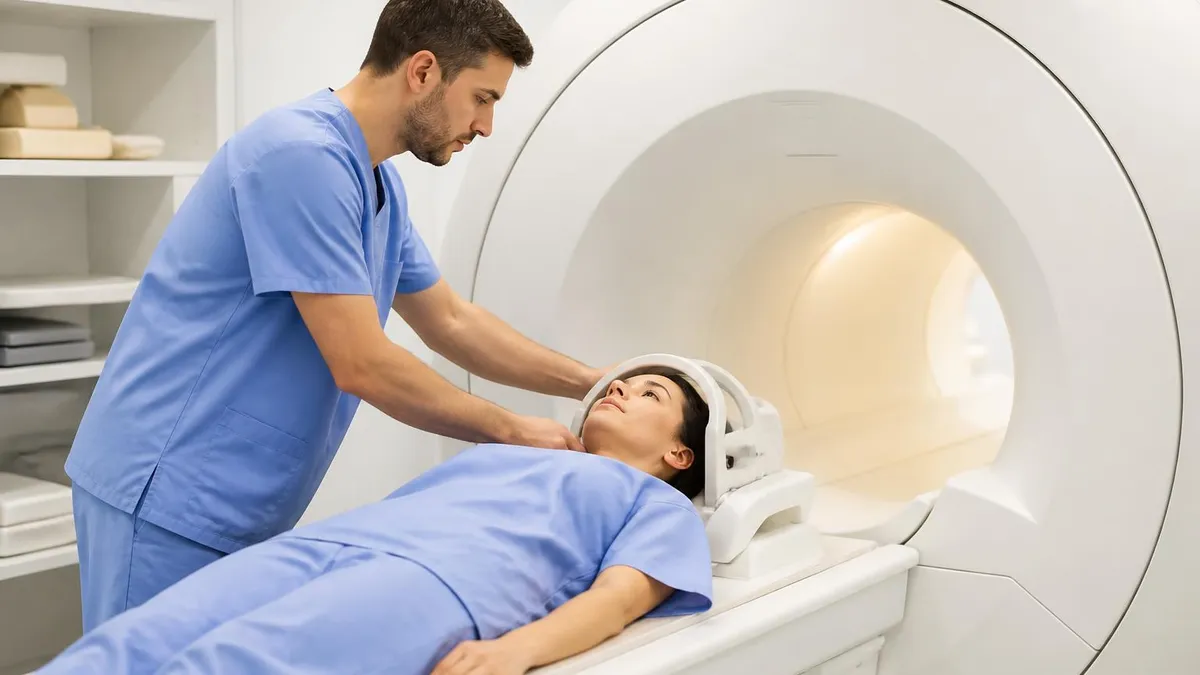
MRI Safety Aspects
Strong magnetic fields used in MRI do not produce cancer risk. The static field strength of 1.5 to 3 Tesla used clinically has been extensively studied without finding cancer association. Magnetic field safety considerations focus on metal objects, implanted devices, and specific medical conditions rather than cancer risk. The magnetic field safety profile supports MRI as safe imaging from cancer perspective while requiring specific safety screening for other considerations affecting MRI eligibility for individual patients.
Long-term MRI safety data supports continued confidence in MRI as low cancer risk imaging option. Over 40 years of clinical MRI use has produced extensive safety data without finding cancer associations from MRI exposure. Population studies including large cohort studies have not found increased cancer rates among patients with MRI exposure history. Animal research has not shown cancer development from MRI-equivalent exposures. The accumulated long-term evidence supports MRI safety regarding cancer risk across various exposure patterns including single scans, multiple scans, and very high cumulative exposure in specific patient situations.
Comparison with background radiation provides context for understanding imaging radiation risks. Background radiation from natural sources including cosmic rays, radon, and natural radioactivity in environment produces small ongoing radiation exposure for everyone. Annual background radiation exposure varies by location with some areas having higher natural radiation than others. CT scan radiation exposure equivalent to several months to years of background radiation. MRI exposure has no radiation component making MRI radiation exposure equivalent to zero background radiation supporting fundamental safety advantage compared to radiation-based imaging from cumulative exposure perspective.
Specific tissue cancer risk considerations affect imaging decisions for various clinical situations. Thyroid cancer risk from radiation exposure to neck region affects imaging decisions for neck and chest imaging particularly in younger patients. Breast cancer risk from radiation exposure affects imaging decisions in women particularly mammography schedules. Leukemia risk from various radiation exposures affects cumulative exposure considerations. The MRI absence of radiation eliminates these tissue-specific radiation cancer considerations supporting MRI preference when MRI provides adequate diagnostic information for specific clinical questions affecting individual patient situations.
Although MRI does not cause cancer through radiation exposure, MRI is not appropriate for all clinical situations. Some conditions require CT scanning, X-ray imaging, or other modalities for adequate diagnosis. The imaging selection should match clinical question with appropriate modality. Avoiding MRI when clinically inappropriate due to misconception about radiation can delay diagnosis affecting patient outcomes. Discussing imaging options with healthcare providers supports informed decisions matching clinical needs with appropriate imaging modality balancing all considerations including radiation, image quality, availability, cost, and individual patient circumstances affecting imaging decisions.
Common misconceptions about MRI safety include various incorrect beliefs that affect patient decisions. The belief that MRI uses radiation like X-rays represents most common misconception affecting patient anxiety. The actual physics of MRI imaging differs fundamentally from radiation-based imaging eliminating radiation cancer concern. Other misconceptions include beliefs about magnetic field cancer risk despite absence of evidence supporting magnetic field cancer association. Beliefs about radiofrequency cancer risk despite extensive safety data. Educating patients about actual MRI physics and safety profile supports informed decisions matching evidence rather than misconception affecting imaging choices.
Multiple MRI scans throughout life do not produce cumulative cancer risk from imaging exposure. Patients with conditions requiring multiple MRI scans for monitoring, diagnosis, or treatment planning can undergo numerous MRI scans without cancer risk concerns from cumulative radiation exposure. The radiation-free nature of MRI supports unlimited MRI use from radiation cancer perspective. Other safety considerations including contrast agents may have specific considerations though radiation cumulative exposure is not concern for MRI imaging. The unlimited MRI use advantage supports MRI as imaging option for chronic conditions requiring ongoing monitoring throughout life.
Cancer screening with MRI involves specific considerations for various cancer types. Breast MRI provides additional screening for high-risk women complementing mammography. Prostate MRI provides specific information about prostate cancer assessment. Liver MRI provides screening for liver cancer in high-risk patients. The MRI screening applications use the same radiation-free imaging providing diagnostic information without radiation cancer concerns. The MRI screening role continues expanding as technology improves supporting cancer detection without cumulative radiation exposure across various screening applications and patient populations.
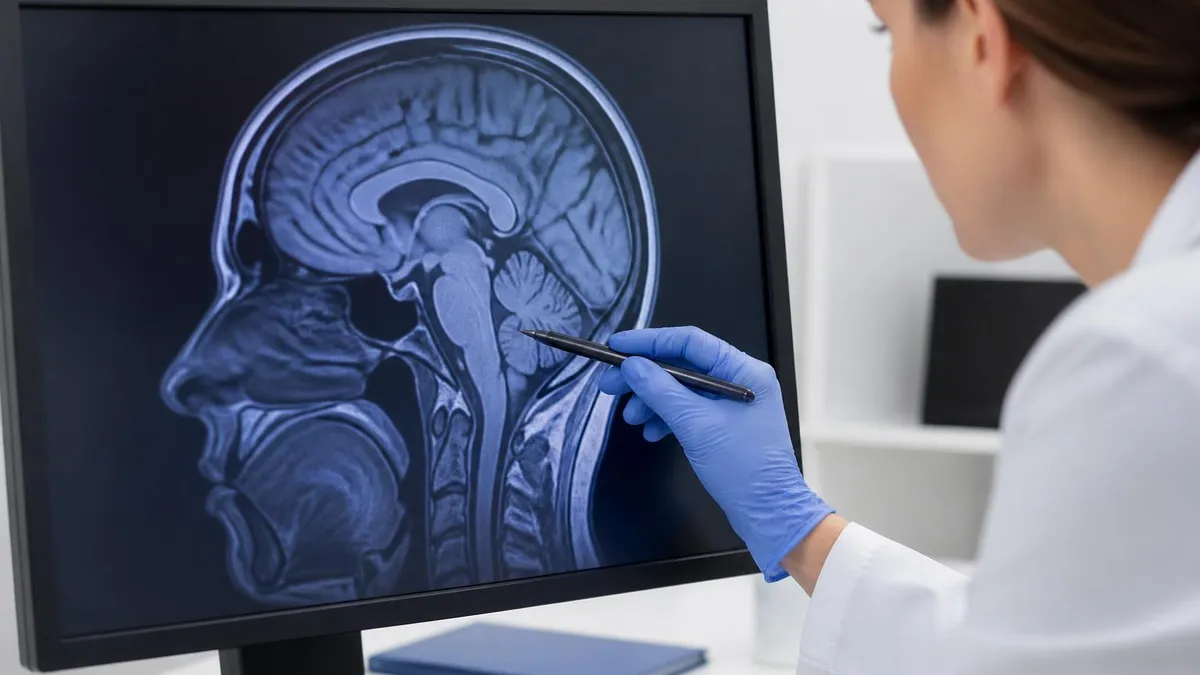
MRI Cancer Risk Assessment Checklist
- ✓Understand MRI uses non-ionizing radiofrequency waves and magnetic fields without ionizing radiation
- ✓Recognize MRI does not produce cancer risk from imaging exposure unlike X-rays and CT scans
- ✓Differentiate MRI from CT scanning which uses ionizing radiation with measurable cancer risk
- ✓Consider MRI preference for pediatric patients due to longer life expectancy and radiation sensitivity
- ✓Evaluate MRI preference for cancer surveillance avoiding cumulative radiation exposure
- ✓Understand gadolinium contrast safety considerations are distinct from cancer risk
- ✓Recognize MRI safety during pregnancy compared to radiation-based imaging options
- ✓Consider MRI for multiple scan situations where radiation exposure would accumulate
- ✓Discuss imaging modality selection with healthcare providers matching clinical needs
- ✓Avoid MRI anxiety based on radiation misconceptions that do not apply to MRI physics
Healthcare provider discussions about imaging safety help patients make informed decisions matching individual circumstances. Healthcare providers can explain specific imaging modality risks and benefits for individual clinical situations. The discussions support informed consent for imaging procedures and address patient concerns including cancer risk questions. Discussing imaging options with healthcare providers helps patients understand why specific modality recommended for specific clinical question. The provider discussions support better patient understanding and reduce anxiety about imaging procedures including MRI scanning supporting better imaging experience and decisions matching individual needs.
Imaging center education about MRI safety supports patient understanding before scanning. Many imaging centers provide educational materials, videos, or staff discussions explaining MRI safety profile. The pre-scan education addresses common questions and concerns including cancer risk questions. The education investment supports better patient experience through informed understanding rather than anxiety from misconceptions. Many patients arrive for MRI with concerns that pre-scan education effectively addresses producing better scanning experience supported by informed understanding of MRI safety profile across various concerns including cancer risk considerations.
Research continues investigating MRI safety across various aspects supporting evidence-based safety assessment. Ongoing research investigates gadolinium retention significance, specific population safety considerations, and various technical safety aspects. The continuing research supports updated safety guidelines and protocols matching current evidence. Healthcare providers and imaging centers update protocols based on emerging research supporting best practice MRI safety. The continuing safety research supports patient confidence in MRI imaging knowing that safety evaluation is ongoing process supported by extensive existing evidence and continuing investigation across various MRI safety aspects.
MRI Safety Pros and Cons
- + —
- + —
- + —
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
- − —
Insurance coverage considerations may affect imaging selection independent of safety profile. Some insurance plans require step-up approaches preferring less expensive imaging before MRI authorization. The insurance considerations may produce situations where CT or other imaging used before MRI even when MRI would be preferred from safety perspective. Patient advocacy for MRI preference when clinically appropriate supports better safety profile matching evidence-based imaging selection. Discussing insurance considerations with healthcare providers supports informed advocacy for appropriate imaging matching clinical needs and safety considerations affecting individual patient situations and insurance circumstances.
Access to MRI affects imaging selection particularly in some geographic areas. Urban areas typically have multiple MRI options supporting MRI preference when clinically appropriate. Rural areas may have limited MRI access affecting imaging decisions. Emergency situations may favor CT imaging due to faster scan times and broader availability even when MRI would provide equivalent diagnostic information. The access considerations affect specific imaging decisions in specific situations. The access advantages of other imaging types must be balanced against MRI safety advantages in specific situations affecting individual imaging decisions.
The MRI absence of cancer risk from imaging exposure represents important safety advantage compared to radiation-based imaging types. The MRI safety profile supports MRI as preferred option for many clinical situations particularly multiple scan needs, pediatric imaging, pregnancy imaging, and cancer surveillance imaging. The accumulated decades of safety evidence supports confident MRI use without cancer risk concerns from imaging exposure. Discussing imaging options with healthcare providers supports informed decisions matching clinical needs with appropriate safety considerations balancing all relevant factors including radiation exposure, image quality, availability, and individual circumstances affecting imaging decisions for specific patient situations.
MRI Questions and Answers
Patient empowerment through MRI safety understanding supports better imaging decisions and reduced anxiety about MRI procedures. Patients who understand actual MRI physics make better informed decisions matching evidence-based safety assessment. The empowerment reduces unnecessary anxiety about MRI while supporting informed consent and active participation in imaging decisions. The investment in MRI safety understanding produces better patient experience through informed engagement with healthcare providers and imaging centers about specific imaging needs and considerations affecting individual circumstances and clinical situations.
Future MRI technology continues improving while maintaining favorable safety profile. New scanning sequences provide better diagnostic information without changing fundamental safety profile. Faster scanning reduces time inside scanner improving patient experience. Quieter scanning reduces acoustic considerations. New contrast agents continue improving with evolving safety profiles. The continuing technological advancement supports continuing MRI advantages including the fundamental safety advantage of non-ionizing imaging. Patients can confidently expect ongoing MRI advances while maintaining the cancer safety profile that characterizes MRI imaging compared to radiation-based alternatives.
The fundamental answer to whether MRI causes cancer is no. MRI does not use ionizing radiation eliminating the primary mechanism of imaging-induced cancer risk. Over 40 years of clinical experience supports MRI safety regarding cancer development. The MRI safety profile makes MRI preferred imaging option for many clinical situations particularly those requiring multiple scans, pediatric imaging, pregnancy imaging, and cancer surveillance. Understanding actual MRI physics and safety profile supports informed decisions matching evidence-based assessment of imaging options. The investment in MRI safety understanding produces better imaging experience through informed engagement with healthcare across various health situations requiring diagnostic imaging.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.