Spine MRI: Complete Imaging Guide
Spine MRI evaluates disc herniation, stenosis, nerve compression, and tumors. Learn protocols, regional differences, contrast use, and what to expect.

Spine MRI represents standard imaging procedure evaluating spinal anatomy and pathology across various spine conditions. The procedure uses powerful magnetic fields and radio waves to generate detailed images of vertebrae, intervertebral discs, spinal cord, nerve roots, and surrounding soft tissues. Spine MRI supports diagnosis and management of various conditions including back pain, herniated discs, spinal stenosis, nerve compression, tumors, infections, and various other spinal pathologies. Understanding spine MRI helps patients prepare for examination while supporting clinical decision-making across various spinal conditions requiring imaging evaluation.
Spine MRI typically divided into three regional examinations matching specific spine areas. Cervical spine MRI evaluates neck region from skull base to thoracic spine. Thoracic spine MRI evaluates middle back from thoracic to lumbar transition. Lumbar spine MRI evaluates lower back from thoracic transition to sacrum. Sacral and coccygeal MRI when needed evaluates lowest spine region. Some clinical situations require multi-regional spine MRI evaluating multiple areas in single examination session. Understanding regional approach supports appropriate imaging order matching specific clinical question and patient presentation.
This guide explains spine MRI comprehensively including clinical indications, imaging protocols, contrast considerations, procedural expectations, regional differences, common findings, normal anatomy review, conditions diagnosed, comparison with other imaging modalities, post-procedure considerations, and various other aspects affecting spine MRI procedures. Whether you are patient scheduled for spine MRI, family member supporting patient, considering spine imaging for various symptoms, comprehensive understanding supports informed approach to this important diagnostic procedure across various spine conditions and clinical scenarios.
Spine MRI Facts
Clinical indications for spine MRI span various medical conditions affecting spine function or anatomy. Persistent back pain not responding to conservative treatment requires imaging evaluation. Sciatica or radiating leg pain suggesting nerve root compression. Numbness, weakness, or various neurological symptoms suggesting spinal cord or nerve involvement. Suspected herniated disc, spinal stenosis, tumor, or various other spine pathology. Trauma evaluation when spine injury suspected. Cancer staging and metastasis evaluation. Post-surgical evaluation for various spine procedures. Understanding indications supports appropriate imaging utilization matching specific clinical questions.
Imaging protocols for spine MRI optimize visualization of specific regional anatomy. Sagittal images provide longitudinal view showing spine alignment, disc spaces, and various anatomical relationships. Axial images provide cross-sectional view showing individual vertebrae, discs, spinal canal, and surrounding structures. T1 weighted images show fat as bright supporting fat-containing structure visualization. T2 weighted images show water as bright supporting fluid and pathology visualization. Various other sequences including STIR, gradient echo, and contrast-enhanced sequences support specific clinical questions. The systematic protocol approach produces comprehensive spine imaging.
Contrast considerations for spine MRI involve selective gadolinium use based on clinical question. Non-contrast spine MRI provides excellent anatomy and pathology visualization for many conditions including herniated discs, spinal stenosis, and various other common conditions. Contrast use indicated for tumor evaluation, infection assessment, post-operative imaging distinguishing scar tissue from recurrent pathology, and various other specific situations. Kidney function evaluation before contrast use through serum creatinine. Allergy considerations affect contrast use decisions. The selective contrast use balances diagnostic capability with contrast considerations across various spine MRI applications.
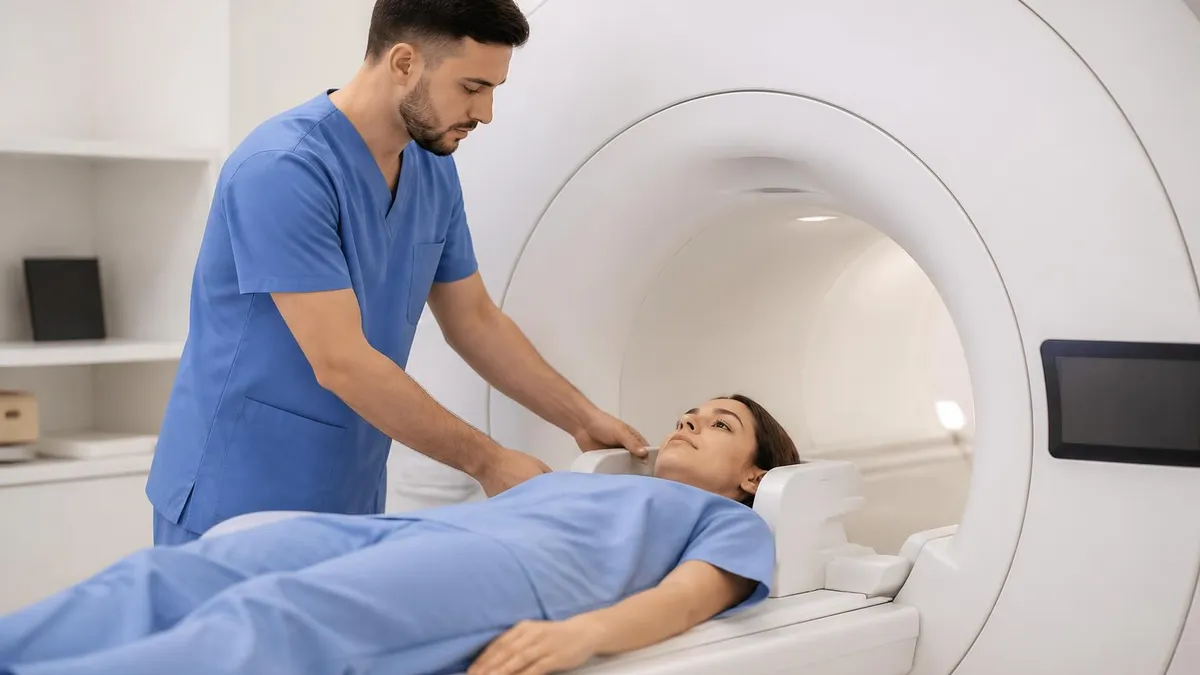
Spine MRI offers substantial advantages over other spine imaging modalities. X-ray provides bone visualization with limited soft tissue detail and uses ionizing radiation. CT scan provides excellent bone detail and reasonable soft tissue detail though uses ionizing radiation. MRI provides superior soft tissue contrast including spinal cord, discs, and nerve roots without radiation exposure. Specific clinical situations may favor specific imaging modalities with MRI typically preferred for soft tissue evaluation while CT preferred for bone detail or emergency situations. The imaging modality selection matches specific clinical question with appropriate capability for diagnostic needs across various spine evaluation scenarios.
Regional differences in spine MRI reflect specific anatomy and common pathologies. Cervical spine MRI evaluates neck region with focus on spinal cord, nerve roots, and disc pathology causing neck pain and arm symptoms. Thoracic spine MRI evaluates less commonly imaged middle back region with focus on trauma, tumor, and various pathology. Lumbar spine MRI most commonly performed evaluating lower back pain, sciatica, and various lumbar conditions including herniated discs and spinal stenosis. Each regional examination uses similar core protocols with regional adaptation supporting specific anatomy visualization and common pathology identification.
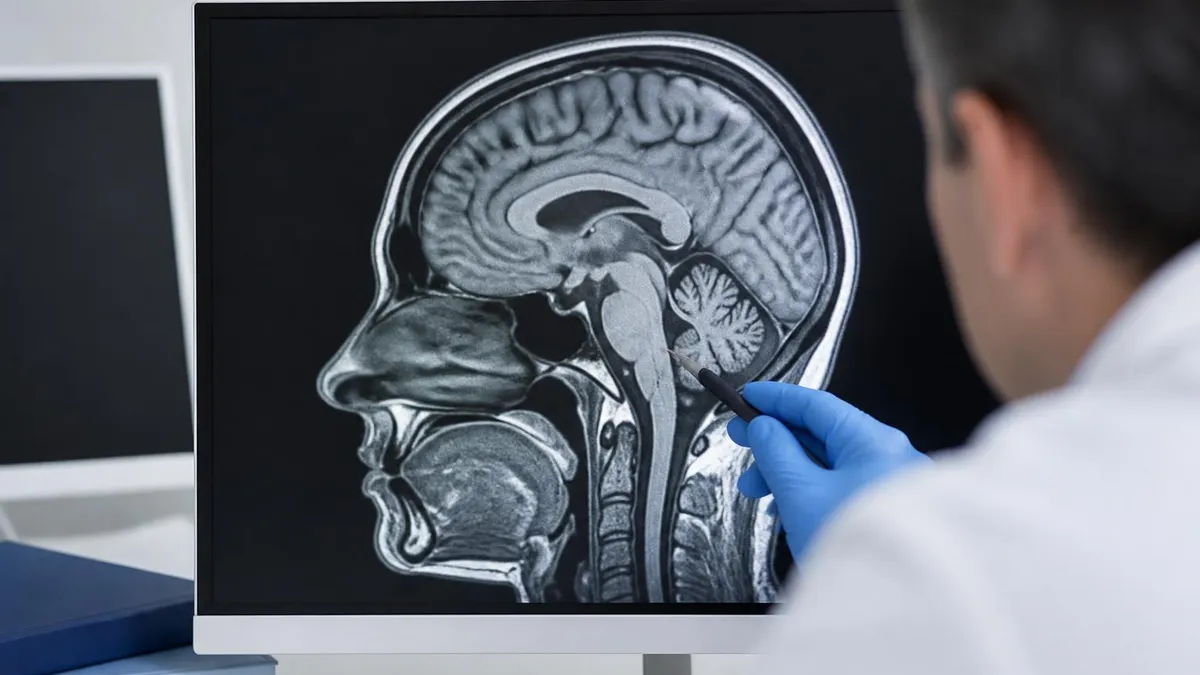
Normal spine anatomy on MRI provides foundation for pathology identification. Vertebrae appear as cubic bones with cortical edges and medullary marrow content. Intervertebral discs sit between vertebrae with nucleus pulposus center and annulus fibrosus periphery. Spinal canal contains spinal cord and cerebrospinal fluid. Nerve roots exit spine through foramina between adjacent vertebrae. Ligaments support spinal alignment. Muscles surround spine providing movement and stability. Understanding normal anatomy supports recognizing pathological changes affecting various spinal structures across different spine regions and conditions.
Common conditions diagnosed through spine MRI include various pathological findings affecting clinical management. Herniated disc represents most common finding with disc material extending beyond normal disc boundaries potentially compressing nerves. Spinal stenosis involves narrowing of spinal canal compressing spinal cord or nerve roots. Degenerative disc disease shows disc dehydration and various changes. Spondylolisthesis involves vertebrae slippage. Tumors including metastases and various other lesions identified through MRI. Infections including discitis and osteomyelitis. Trauma effects including fractures and ligament injuries. Each finding requires correlation with clinical symptoms for appropriate management.
Common Spine MRI Findings
Most common spine MRI finding with disc material extending beyond normal disc boundaries. May compress nerve roots or spinal cord causing various symptoms. Severity ranges from disc bulge to severe extrusion. Most resolve with conservative treatment though some require surgical intervention. MRI characterizes herniation location, size, and structural impact supporting clinical decisions about treatment approach.
Narrowing of spinal canal compressing spinal cord or nerve roots. Most common in lumbar and cervical spine. May cause leg pain with walking lumbar or arm symptoms cervical. Often combined with degenerative disc disease. Treatment depends on symptom severity including conservative management or surgical decompression. MRI shows stenosis extent and structural causes supporting treatment planning.
Age-related disc changes with disc dehydration, height loss, and various structural changes. Common with aging affecting most adults to some degree. May or may not cause symptoms depending on specific changes and nerve involvement. Treatment focuses on symptom management through various conservative approaches. MRI shows disc changes supporting clinical correlation with patient symptoms.
Various pathologies affecting spinal cord including tumors, demyelinating disease, infections, vascular abnormalities, and various other conditions. MRI provides excellent spinal cord visualization supporting diagnosis. May cause significant neurological symptoms requiring specific treatment. Specialized neurology evaluation typically required for spinal cord pathology supporting comprehensive diagnostic and treatment planning.
Compression of exiting nerve roots through various causes including herniated disc, foraminal stenosis, tumor, and various other conditions. Causes radiating pain following specific nerve distribution. Treatment depends on specific cause and symptom severity. MRI identifies compression location and cause supporting targeted treatment planning across various nerve compression scenarios.
Various injuries from trauma including fractures, ligament injuries, disc damage, and various other traumatic findings. MRI provides comprehensive trauma evaluation when soft tissue injury suspected. Often combined with CT for bone detail. Treatment depends on specific injuries and stability assessment. Emergency MRI may support trauma evaluation in various clinical scenarios requiring urgent imaging.
Procedural expectations for spine MRI similar to other MRI procedures with regional considerations. Patient arrives at imaging center, completes screening forms removing metallic objects. Hospital gown for examination supports comfort and metal-free imaging. Intravenous line placement if contrast planned. Patient positioned supine on MRI table with positioning matching specific region being imaged. Procedure typically 30 to 45 minutes for non-contrast examinations and 45 to 60 minutes with contrast. Communication with technologist through intercom supports comfort during procedure. The systematic procedure approach supports efficient spine imaging while maintaining patient comfort and procedure quality.
Patient preparation for spine MRI includes several considerations. Most spine MRI does not require specific dietary preparation unlike some other imaging studies. Continuing current medications typically appropriate. Removing all metallic objects supports safe MRI environment. Wearing comfortable clothing without metal accessories supports procedure. Identifying any implants or devices through screening. Discussing pregnancy status when applicable. Anti-anxiety medication consideration for patients with claustrophobia. The preparation supports safe and effective MRI examination matching specific patient circumstances and clinical considerations across various spine MRI applications.
Common patient concerns about spine MRI include various worries affecting procedure experience. Claustrophobia represents common concern with enclosed scanner producing anxiety for some patients. Scanner noise loud requiring earplugs or headphones with music. Procedure duration may be uncomfortable particularly for patients with back pain. Position requirements may exacerbate symptoms for some patients. Anti-anxiety medication, communication during scan, and various other approaches support patient comfort. Understanding common concerns supports informed patient approach to spine MRI procedure across various individual circumstances and concerns.
Spine MRI Topics
Cervical spine MRI evaluates neck region from skull base to thoracic transition. Common indications include neck pain, arm symptoms, suspected disc herniation, spinal stenosis, and various other cervical conditions. Imaging shows vertebrae C1 to C7 with corresponding discs and surrounding structures. Spinal cord visualization important given cervical cord vulnerability to compression. Nerve roots evaluated for compression causing arm symptoms. Specific positioning supports neck imaging with neutral alignment supporting optimal visualization across various cervical spine conditions.
Post-procedure considerations include return to normal activities and follow-up planning. Most patients return to normal activities immediately after spine MRI without restrictions. Contrast received patients should hydrate adequately supporting kidney clearance. Allergic reactions to contrast rare but require monitoring. Results typically available within days to weeks depending on facility and clinical urgency. Follow-up with referring physician for results discussion typically scheduled. The post-procedure considerations represent minimal impact for most patients supporting routine spine imaging without significant lifestyle interruption beyond examination day itself.
Results interpretation involves correlation of imaging findings with clinical and physical examination information. Radiologist interprets imaging providing detailed report. Treating physician correlates imaging with patient symptoms and examination for treatment decisions. Multi-disciplinary discussion between radiologist, neurosurgeon, orthopedist, neurologist may support complex cases. Patient discussion with treating physician explains findings and management implications. The collaborative interpretation supports comprehensive spine care across various specialty contributions affecting clinical decisions and patient management planning throughout spine condition treatment.
Surgical planning support represents important spine MRI application for patients requiring surgical intervention. Detailed anatomical visualization supports surgical approach selection. Pathology characterization including location, size, and structural impact informs procedure planning. Adjacent structure relationships affect surgical approach decisions. Pre-operative MRI provides baseline for post-operative comparison. The detailed pre-operative imaging supports informed surgical planning matching specific patient anatomy and pathology across various spine surgery scenarios and procedures requiring detailed anatomical information for optimal outcomes.
Spine MRI safety considerations include various factors affecting procedure suitability. Pacemakers, cochlear implants, certain aneurysm clips, and various other implants may contraindicate MRI. Spinal cord stimulators and other spine-related implants require specific evaluation for MRI compatibility. Recent surgery with various surgical implants requires verification. Pregnancy considerations particularly with gadolinium contrast. Severe claustrophobia may prevent procedure completion without sedation. Discussing safety considerations with referring physician and imaging facility supports informed procedure decisions. Most patients safely undergo spine MRI with appropriate screening and considerations.
Special spine MRI techniques support specific clinical questions beyond standard protocols. MR myelography provides cerebrospinal fluid imaging supporting evaluation of fluid-filled structures and pathology. Diffusion-weighted imaging supports tumor and infection characterization. MR spectroscopy provides chemical information supporting tumor and metabolic evaluation. Functional MRI techniques support specific applications. Specialized sequences for specific conditions including multiple sclerosis, syringomyelia, and various other conditions provide targeted information. The specialized techniques expand spine MRI capability beyond standard protocols supporting comprehensive spine evaluation across diverse clinical scenarios.
Multi-disciplinary care coordination supports comprehensive spine condition management. Primary care physicians often initiate spine evaluation and coordinate care. Specialists including neurosurgeons, orthopedists, neurologists, and pain management physicians provide specialized care. Physical therapists support conservative treatment and rehabilitation. Radiologists support diagnostic imaging interpretation. Multi-disciplinary teams discuss complex cases supporting coordinated treatment planning. The collaborative care approach supports comprehensive spine condition management across various specialty contributions affecting patient outcomes throughout spine treatment timeline.
The spine MRI procedure represents valuable diagnostic tool supporting accurate diagnosis of various spine conditions affecting many patients each year. Understanding the procedure comprehensively including indications, protocols, expectations, regional considerations, and follow-up supports informed patient approach. The detailed spine imaging supports clinical decisions across various spine conditions producing important diagnostic information affecting treatment decisions and patient outcomes. Most spine MRI procedures proceed smoothly with valuable diagnostic information supporting optimal clinical care across diverse spine medical scenarios and individual patient circumstances throughout evaluation and treatment processes.
Spine MRI Preparation
- ✓Confirm specific spine region examination with referring physician
- ✓Complete screening forms for MRI safety
- ✓Disclose all implants, devices, and metal in body
- ✓Remove all metallic objects before scanner entry
- ✓Confirm pregnancy status if applicable
- ✓Provide complete medication and allergy history
- ✓Discuss kidney function status for contrast considerations
- ✓Address claustrophobia or anxiety concerns before scan
- ✓Plan transportation if anti-anxiety medication used
- ✓Follow up with referring physician for results discussion
Quality considerations for spine MRI include various factors affecting diagnostic value. Field strength typically 1.5 or 3 Tesla with higher field strength supporting improved image quality. Coil selection affects image quality with dedicated spine coils supporting optimal regional imaging. Protocol optimization for specific clinical questions improves diagnostic capability. Technologist expertise affects positioning and image quality. Radiologist interpretation expertise supports accurate diagnosis. The quality factors affect diagnostic outcomes with quality imaging supporting better clinical decisions across various spine MRI applications and individual patient clinical scenarios requiring optimal imaging support.
Comparison with non-spine MRI applications reveals spine-specific considerations. Brain MRI uses different protocols and coils than spine MRI. Joint MRI uses joint-specific positioning and coils. Abdominal and pelvic MRI uses different protocols. Each anatomical region has specific imaging optimization. Spine MRI specifically addresses spine anatomy and pathology through dedicated protocols. The regional specialization within MRI supports optimal imaging for various clinical questions matching specific anatomical considerations across diverse MRI applications and clinical needs.
The spine MRI procedure provides essential diagnostic capability across various spine conditions supporting accurate diagnosis and effective treatment planning. Understanding the procedure comprehensively including indications, protocols, expectations, common findings, and various other aspects supports informed patient approach to important diagnostic procedure. Whether for back pain evaluation, nerve compression assessment, tumor evaluation, or various other clinical questions, spine MRI provides detailed information supporting clinical decisions throughout spine condition management across diverse patient circumstances and specific clinical scenarios.
Spine MRI
- + —
- + —
- + —
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
- − —
Pediatric spine MRI considerations include various factors affecting children specifically. Younger children may require sedation or anesthesia for examination tolerance. Specific pediatric protocols optimize imaging for smaller patients. Pediatric radiologists with specific expertise support image interpretation. Parental presence policies vary across facilities. Understanding pediatric considerations supports family preparation for children's spine MRI when needed. Most pediatric spine MRI procedures proceed safely with appropriate considerations supporting accurate diagnosis for pediatric spine conditions across various clinical scenarios requiring spine evaluation in pediatric population.
Special clinical situations including post-operative imaging present specific challenges. Post-surgical scar tissue may complicate interpretation distinguishing scar from recurrent pathology. Contrast enhancement supports differentiation. Metal implant artifacts may affect image quality though techniques exist for artifact reduction. Specific protocols for post-operative spine optimize imaging. Understanding post-operative considerations supports appropriate post-surgical imaging when needed across various spine surgery scenarios and post-operative complication evaluations requiring continued imaging for clinical management.
The spine MRI represents critical diagnostic tool supporting accurate diagnosis and treatment planning for diverse spine conditions affecting patient health and quality of life. Understanding the procedure comprehensively supports informed patient approach to important diagnostic procedure. Whether for initial diagnosis, treatment planning, or post-treatment monitoring, spine MRI provides essential information supporting clinical decisions throughout spine condition management. The systematic understanding helps patients navigate spine evaluation with appropriate context and informed participation in their healthcare decisions across various spine clinical scenarios.
MRI Questions and Answers
Cost considerations for spine MRI vary across geographic regions and healthcare systems. Insurance coverage typically supports medically indicated spine MRI though preauthorization may be required. Out-of-pocket costs vary substantially depending on insurance coverage and specific facility pricing. Some patients face significant costs requiring financial planning for procedure. High-deductible plans may produce substantial patient responsibility before insurance coverage activates. Discussing costs with provider and insurance before procedure supports informed financial planning across various healthcare contexts and patient circumstances affecting spine MRI access.
Continuing advances in MRI technology support evolving spine imaging capabilities. Higher field strength scanners, improved coil technology, advanced imaging sequences, faster imaging protocols, and various other developments improve diagnostic capability while potentially reducing procedure duration. Artificial intelligence applications support image interpretation and quality optimization. The evolving technology base continues improving spine imaging supporting better patient care over time across various clinical scenarios requiring spine evaluation throughout ongoing medical practice and patient management.
Final considerations for spine MRI emphasize collaborative care between patient and healthcare team for optimal outcomes. Discussion with referring physician about clinical question and expected imaging value supports informed approach. Understanding general procedure expectations supports preparation. Asking questions throughout process supports informed participation. Following up with appropriate specialists supports comprehensive care. The collaborative approach combining patient knowledge with professional expertise produces best outcomes across diverse spine medical scenarios throughout spine condition diagnosis and management across various individual patient circumstances.
Quality healthcare communication throughout spine MRI process supports better patient experience and informed decision-making. Discussing examination purpose, expected findings considerations, and follow-up plans before procedure supports informed patient participation. Asking questions about specific concerns supports anxiety reduction and procedure understanding. The communication investment supports better outcomes across various spine MRI scenarios and patient circumstances.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.