Full Body MRI: What It Scans, How Long It Takes, Cost, and What to Expect
Full body MRI: what it scans, cost, how long it takes, what it detects, pros and cons vs targeted MRI, and who should get one.
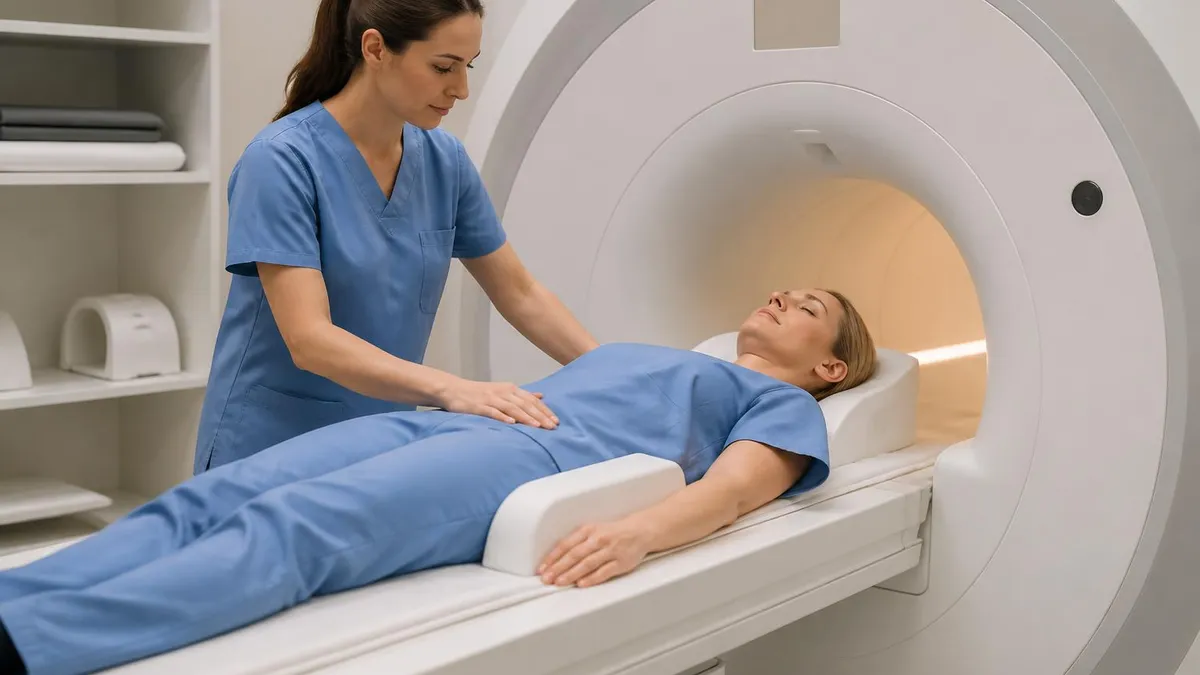
A full body MRI is a head-to-toe imaging study that uses powerful magnetic fields and radio waves to create detailed pictures of your organs, tissues, and bones — all in a single session. Unlike a standard MRI scan that focuses on one region, a whole-body MRI covers your brain, spine, chest, abdomen, pelvis, and musculoskeletal system without exposing you to any ionizing radiation.
It sounds like the ultimate health checkup, and in some ways it is. But it's also expensive, time-consuming, and not always covered by insurance. Whether you're exploring it for peace of mind or a doctor has mentioned it, this guide breaks down everything you need to know before you book one.
The appeal of a full body MRI is easy to understand. You get one appointment, one machine, one set of results — and a radiologist reviews images of nearly every major organ system in your body. For people with strong family histories of cancer, or those who've never had a comprehensive imaging study, the idea of a single comprehensive screen is genuinely compelling. The challenge is that medicine doesn't always work that neatly. Imaging is a tool, not a guarantee, and the question of whether a whole-body scan adds clinical value depends on who's asking and why.
Quick Facts: Full Body MRI
- Scan duration: 45–90 minutes depending on protocol and contrast use
- Cost range: $1,000–$5,000 (often out-of-pocket)
- No ionizing radiation — safe for most adults
- Can detect tumors, vascular abnormalities, organ disease, and bone marrow problems
- Common in executive health screenings and cancer surveillance programs
To understand what makes a full body MRI different, it helps to know how the technology works. The MRI machine generates a strong magnetic field that temporarily aligns the hydrogen atoms in your body. When radio waves pulse through, those atoms emit signals that the scanner converts into cross-sectional images — called slices — that radiologists read to spot abnormalities.
A targeted MRI looks at just one body part, say your knee or your brain. A full body MRI runs through multiple imaging sequences, one region at a time, to produce a comprehensive picture. It's the same physics, just applied on a much larger scale.
The sequences used for each region differ. Brain imaging relies heavily on T1-weighted images for anatomy and T2/FLAIR sequences for detecting white matter changes and edema. Abdominal imaging adds fat-suppression techniques to separate organ tissue from surrounding fat. Cardiac MRI uses ECG gating to synchronize image acquisition with the heartbeat. Each protocol is purpose-built for the tissue it's examining, and a skilled radiologist will choose different sequences depending on what they're looking for. A good full body protocol doesn't just run one sequence — it layers several for each region to maximize diagnostic sensitivity.
Field strength matters too. Most clinical MRI scanners operate at 1.5 Tesla or 3 Tesla. Higher field strength generally means better signal-to-noise ratio and sharper images, though it also means more acoustic noise during the scan and higher sensitivity to metal artifacts. For whole-body screening, 3T scanners are increasingly preferred, particularly for detecting small lesions in soft tissues. If you're comparing facilities, it's worth asking what magnet strength they use.
One important nuance: there's no single universal full body MRI protocol. Different imaging centers use different sequences and field strengths. A 3-Tesla scanner at a major academic hospital will produce sharper images than a 1.5T scanner at a community center. When you're comparing prices or centers, ask exactly which body regions are included and what magnet strength they use.
That said, most comprehensive programs cover the same core territory: brain, cervical and lumbar spine, chest (including heart and lungs), abdomen (liver, kidneys, pancreas, spleen), pelvis, and major joints. Some add vascular imaging of the aorta and major arteries as well.
Gadolinium contrast is another variable. Some full body protocols use intravenous gadolinium — a contrast agent that causes abnormal tissues to light up on certain sequences — while others are deliberately designed to be contrast-free. Contrast improves lesion characterization, especially in the liver and brain, but it adds cost, requires IV access, and is contraindicated in patients with severe kidney disease. Ask in advance whether contrast is part of the protocol you're being offered and whether you have any conditions that would make it inadvisable.
The brain portion screens for tumors, white matter lesions, early signs of dementia, aneurysms, and structural abnormalities. Spine imaging covers disc herniations, spinal cord compression, and vertebral fractures. Together, these sequences often take 15–25 minutes of the total scan time.
- Detects: gliomas, meningiomas, pituitary adenomas, cervical stenosis
- Clinical use: neurological symptoms, headache workups, cancer surveillance
- Sequences used: T1, T2, FLAIR, DWI
Now you know what it covers — but how does a full body MRI compare to ordering separate targeted scans? The answer isn't as straightforward as it might seem. Understanding the MRI vs CT scan tradeoffs is one piece of the puzzle, but the full body vs targeted MRI question is its own conversation.
A targeted MRI is ordered when a clinician has a specific clinical question — you've got knee pain, or a breast lump, or a neurological symptom. The radiologist knows what to look for and tailors the protocol accordingly. With a full body scan, the radiologist is looking at everything, which means they might catch something clinically insignificant and flag it anyway.
Think about it this way: if you have lower back pain, your doctor orders a lumbar spine MRI. The radiologist focuses entirely on the lumbar vertebrae, discs, and surrounding soft tissue. They apply sequences optimized for that region, and the resulting images are higher resolution than what a full body scan would produce for the same area. A targeted scan is a clinical tool; a full body scan is more of a screening tool. Both have value — but they answer different questions.
There's also a practical imaging quality consideration. Whole-body protocols inevitably involve tradeoffs. To cover head-to-toe anatomy in under 90 minutes, some sequences have to be shortened or simplified. A dedicated brain MRI for epilepsy might use thin-slice sequences that catch tiny cortical lesions missed on a faster whole-body brain protocol. If you have a known condition, a targeted scan is almost always the better choice for that specific area — and a full body scan can supplement it, not replace it.
- Scope: Head to toe — brain, spine, chest, abdomen, pelvis, MSK
- Duration: 45–90 minutes
- Cost: $1,000–$5,000 out-of-pocket
- Insurance: Rarely covered unless medically ordered
- Best for: Preventive screening, cancer surveillance, executive health
- Limitation: Higher incidental finding rate, longer scan time
- Scope: Single body region (brain, knee, abdomen, etc.)
- Duration: 20–45 minutes
- Cost: $400–$1,500 (often partially insured)
- Insurance: Covered when medically indicated
- Best for: Diagnosing specific symptoms, follow-up imaging
- Limitation: Misses pathology outside the imaged region
One underappreciated issue with full body MRI is the incidental finding problem. Studies suggest that up to 30% of asymptomatic adults who undergo whole-body screening have at least one incidental finding that requires follow-up. Most turn out to be benign — a cyst on the kidney, a small thyroid nodule, a liver hemangioma — but each one triggers anxiety, additional imaging, and sometimes invasive procedures.
That's not an argument against full body MRI across the board. But it's a reason to think carefully before you book one without a clinical rationale. The scan itself is safe; the downstream effect of an unexpected finding can be stressful and costly.
The medical community uses the term "cascade effect" to describe what happens after incidental findings: one scan leads to a follow-up scan, which leads to a biopsy, which leads to a minor procedure — each step adding cost and risk, even when the original finding was harmless. This is particularly common with small adrenal masses (adrenal incidentalomas), indeterminate liver lesions, and subcentimeter lung nodules. Radiologists use standardized reporting systems like Lung-RADS and LI-RADS to help manage these findings, but not every facility applies them consistently to whole-body screening results.
- +No ionizing radiation — safe to repeat over time unlike CT scans
- +Comprehensive coverage catches pathology you didn't know to look for
- +Excellent soft-tissue contrast, especially for abdominal organs and bone marrow
- +Useful for cancer surveillance in high-risk populations (BRCA carriers, Lynch syndrome, family history)
- +Can replace multiple separate targeted scans in certain clinical scenarios
- +Non-invasive — no surgical risk, no recovery time
- −High out-of-pocket cost, typically $1,000–$5,000, often not covered by insurance
- −Incidental findings in ~30% of scans lead to further workup, anxiety, and added expense
- −Long scan time (45–90 minutes) is challenging for claustrophobic patients
- −Less sensitive than CT for small pulmonary nodules and calcifications
- −Not appropriate for patients with certain metal implants or pacemakers
- −Clinical evidence for routine screening in average-risk adults is limited
So who should actually get a full body MRI? The clearest use cases are clinical: known cancer patients undergoing surveillance, people with genetic syndromes that significantly raise cancer risk, and patients with unexplained symptoms spanning multiple systems. In these situations, a doctor orders the scan, insurance often covers it, and the radiologist has a clinical context that sharpens interpretation.
The more debated use case is healthy adults seeking preventive reassurance — the "executive health screening" market. High-end health concierge programs offer full body MRI as part of comprehensive packages, sometimes alongside a battery of labs and cardiac tests. If you can afford it and go in with realistic expectations, it's not unreasonable. Just don't expect a clean scan to guarantee good health, and be prepared for the possibility of follow-up testing.
It's also worth knowing about MRI safety considerations before booking. Most people are fine, but if you have a pacemaker, cochlear implant, certain aneurysm clips, or embedded metal fragments, you may not be eligible. Always disclose your full implant history to the imaging center before your appointment.
- ✓Inform the center of all metal implants, surgical hardware, or embedded devices
- ✓Ask whether gadolinium contrast will be used and discuss any kidney disease history
- ✓Fast for 4–6 hours if contrast or abdominal imaging is included
- ✓Remove all jewelry, piercings, and metal accessories before the scan
- ✓Wear comfortable, metal-free clothing (or change into a gown at the facility)
- ✓Take any prescribed anti-anxiety medication beforehand if you have claustrophobia
- ✓Ask for earplugs or headphones — MRI machines are loud (up to 110 dB)
- ✓Plan for 2–3 hours total including prep, scan, and recovery
- ✓Arrange a driver if sedation or contrast is used
- ✓Ask how long results take and who will discuss them with you
Here's what the experience actually looks like on the day of your scan. You'll check in, complete safety screening paperwork, and change into a gown if needed. A technologist will confirm your history, remove any remaining metal, and position you on the scanner table. If contrast is used, a nurse places an IV line in your arm.
The table slides into the bore of the magnet — a large cylindrical tube, typically 60–70 cm in diameter. You'll hear rhythmic banging and buzzing sounds as the imaging sequences run. These sounds are completely normal; they come from the gradient coils switching magnetic fields rapidly. Earplugs or headphones are standard.
You'll need to stay still during each sequence. The technologist may ask you to hold your breath briefly for chest and abdominal scans. Full body protocols often reposition you or adjust the table between regions. The total time inside the scanner ranges from 45 minutes for a streamlined protocol to 90 minutes for a comprehensive one with contrast.
The technologist communicates with you throughout the scan via an intercom. You'll have a squeeze bulb or button to signal if you need to stop — use it without hesitation if you feel unwell or panicked. Most facilities play music through the headphones to make the time pass more comfortably. Some offer mirror setups or angled mirrors so you can see out of the magnet bore, which helps reduce the closed-in feeling significantly.
Temperature can also be a factor. The scanner room is often kept cool for equipment reasons, and lying still for an hour can make you feel chilly. Ask for a blanket before you go in. It sounds like a small thing, but comfort matters when you're trying to stay still for 90 minutes straight.
Check-in and Safety Screening
Positioning and Prep
Brain and Spine Sequences
Chest and Cardiac Imaging
Abdomen and Pelvis
Musculoskeletal and Wrap-Up
After the scan, most people feel completely normal and can drive home and resume their day immediately — unless they received sedation. If contrast was used, staying well hydrated helps your kidneys clear the gadolinium. Results typically take 24–72 hours; a radiologist reads all the images and sends a report to your ordering physician, who discusses findings with you.
Understanding what an MRI is at a fundamental level — and what distinguishes it from other imaging — helps you ask better questions. If you want a deeper foundation, read our guide on what is an MRI, which covers the physics, history, and clinical applications of magnetic resonance imaging in plain language.
Insurance Note: Most insurers consider full body MRI experimental or not medically necessary for asymptomatic patients. If your doctor orders one for a specific clinical reason — such as cancer staging or genetic syndrome surveillance — coverage is much more likely. Always call your insurer before booking to confirm whether a referral or prior authorization is required.
Cost is one of the biggest barriers to full body MRI. Prices vary dramatically by geography, facility type, and whether contrast is included. A direct-pay imaging center in a mid-size city might charge $1,200–$1,800 for a comprehensive whole-body scan. A hospital-based scan with contrast can run $3,000–$5,000 before insurance adjustments. Some high-end concierge health programs bundle the scan into annual memberships ranging from $3,000 to $10,000.
The good news: direct-pay pricing has become far more transparent and competitive in recent years. Companies like Ezra and Prenuvo have entered the consumer full body MRI market with streamlined protocols and fixed pricing around $1,000–$2,500. Their scans typically cover fewer sequences than a full clinical protocol, but they're standardized, interpreted by board-certified radiologists, and read specifically for screening purposes.
If cost is a concern and you're in reasonable health, discuss with your primary care physician whether a full body scan is the right choice versus targeted screening tests (mammogram, colonoscopy, PSA, coronary calcium score) that are evidence-backed, less expensive, and typically covered by insurance.
It's also worth asking whether your employer's health plan or flexible spending account (FSA/HSA) allows you to use pre-tax dollars for the scan. Many direct-pay imaging companies provide itemized receipts that qualify for FSA/HSA reimbursement, effectively giving you a 20–30% discount depending on your tax bracket. That won't make a $2,500 scan cheap — but it's a meaningful reduction if you've already decided the scan is right for you.
One more financial consideration: the cost of acting on findings. If your scan finds something ambiguous, plan for additional imaging costs that aren't included in your original quote. A whole-body MRI is the beginning of a diagnostic process, not necessarily the end. Budgeting only for the scan without accounting for potential follow-up can lead to unexpected expenses down the line.
Full Body MRI Questions and Answers
The bottom line is that a full body MRI is a powerful but imperfect tool. It's the most comprehensive single imaging study available to healthy adults, covering more anatomy in one session than any other non-invasive test. But comprehensive doesn't mean complete — it won't catch everything, it's not infallible, and the incidental findings it generates require careful management.
If you're in a high-risk category for cancer or cardiovascular disease, talk to your doctor about whether a whole-body protocol belongs in your surveillance plan. If you're a generally healthy adult seeking reassurance, weigh the cost, the probability of incidental findings, and whether evidence-based targeted screening tests might give you more actionable information for less money.
Whatever you decide, going in informed makes the experience less stressful and the results easier to interpret. The technology is extraordinary — knowing how to use it well is what makes the difference.
Medical imaging has advanced remarkably over the past two decades. What once required days of hospital admission and multiple separate appointments can now be accomplished in a single outpatient session. Full body MRI sits at the leading edge of that evolution — offering something genuinely unprecedented in preventive medicine. Your job as a patient is to decide whether that capability addresses a real need in your specific situation, and to work with your physician to make the most of whatever the results show.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.