What Is CPR? Definition, Steps & When to Use It
What is CPR? Learn what cardiopulmonary resuscitation is, how it works, the steps to perform it, and when hands-only CPR is appropriate.
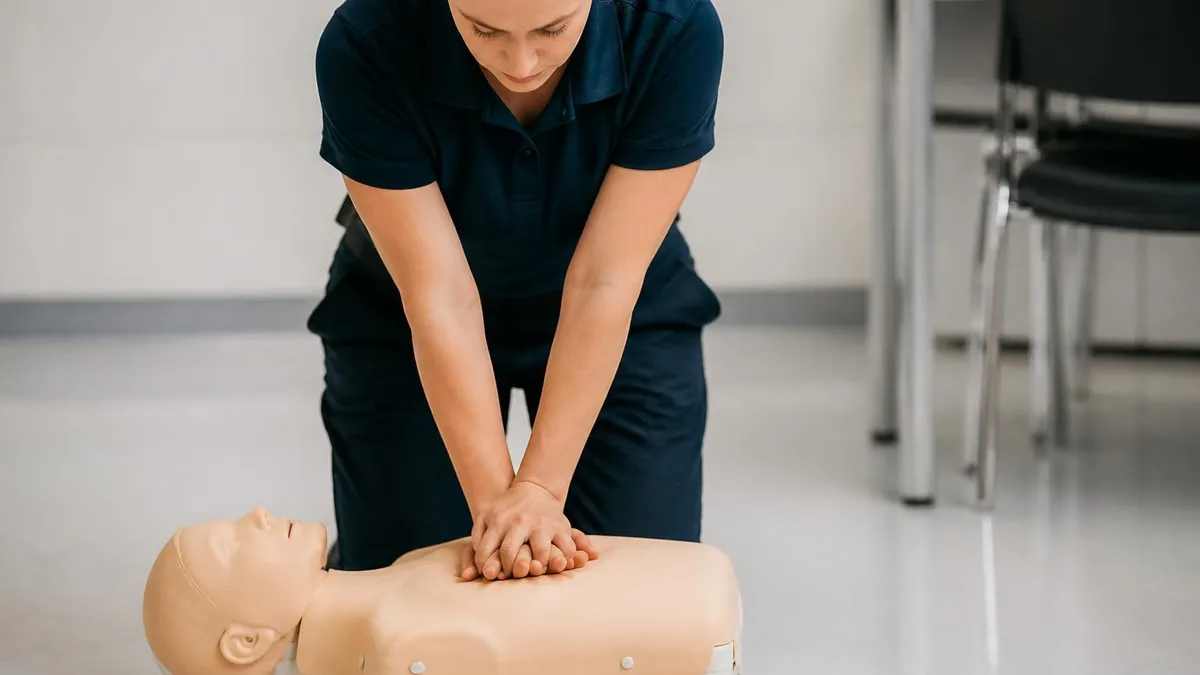
What is CPR? CPR stands for Cardiopulmonary Resuscitation — a life-saving emergency technique that manually pumps blood to the brain and vital organs when the heart stops beating. Bystander CPR can double or triple a cardiac arrest victim's chance of survival. You don't need to be a healthcare professional to save a life.
Every year, about 350,000 cardiac arrests happen outside of hospitals in the United States. Most of them — roughly 70% — occur at home, in front of family members or friends who may feel completely helpless. CPR changes that. It gives ordinary people the power to keep someone alive until paramedics arrive.
So what is CPR, exactly? CPR stands for Cardiopulmonary Resuscitation. Break that down: "cardio" refers to the heart, "pulmonary" refers to the lungs, and "resuscitation" means reviving someone from unconsciousness or apparent death. When you perform CPR, you're manually stepping in for the heart and lungs — keeping blood and oxygen circulating until the heart can be restarted.
Without CPR, the brain begins to suffer permanent damage within 4 to 6 minutes of cardiac arrest. Emergency responders typically take 8 to 12 minutes to arrive. That gap is where bystander CPR becomes the difference between life and death. The skills aren't complicated. They don't require medical training. They require knowledge, practice, and the willingness to act.
What Does CPR Do?
When someone goes into cardiac arrest, their heart stops pumping blood effectively. Without a steady supply of oxygenated blood, the brain and other vital organs begin to shut down — fast. CPR manually takes over that pumping action, buying time until definitive treatment arrives.
Chest compressions physically squeeze the heart between the breastbone and the spine, forcing blood out into the circulatory system. Rescue breaths (when used) push oxygen into the lungs, which the blood then carries to the brain and organs. Together, these actions create a temporary artificial circulation — not perfect, but enough to buy critical time. Quality compressions can maintain 25 to 30% of normal cardiac output — sufficient to preserve brain function during those precious minutes before defibrillation.
CPR doesn't typically restart the heart on its own. What it does is keep oxygen-rich blood moving to the brain, preventing or slowing brain damage until a defibrillator (or advanced medical care) can restore a normal heart rhythm. Think of CPR as a bridge — it keeps the person viable until more powerful help arrives.
People often confuse cardiac arrest with a heart attack. A heart attack happens when blood flow to part of the heart muscle is blocked — the person is usually conscious and in pain. Cardiac arrest is when the heart's electrical system fails and the heart stops beating altogether. The person collapses, becomes unresponsive, and stops breathing normally. Cardiac arrest requires immediate CPR. A heart attack may or may not — but if you're unsure which it is, calling 911 first is always the right move.

The CPR Steps: C-A-B
The American Heart Association updated the CPR sequence to C-A-B: Compressions, Airway, Breathing. This replaced the older A-B-C order because getting compressions started immediately is the most critical step — every second counts.
Before you start, make sure the scene is safe. Then: check responsiveness by tapping shoulders and shouting; call 911 immediately (or have someone else call while you begin CPR); check breathing for no more than 10 seconds — occasional gasping is NOT normal breathing. Then begin compressions.
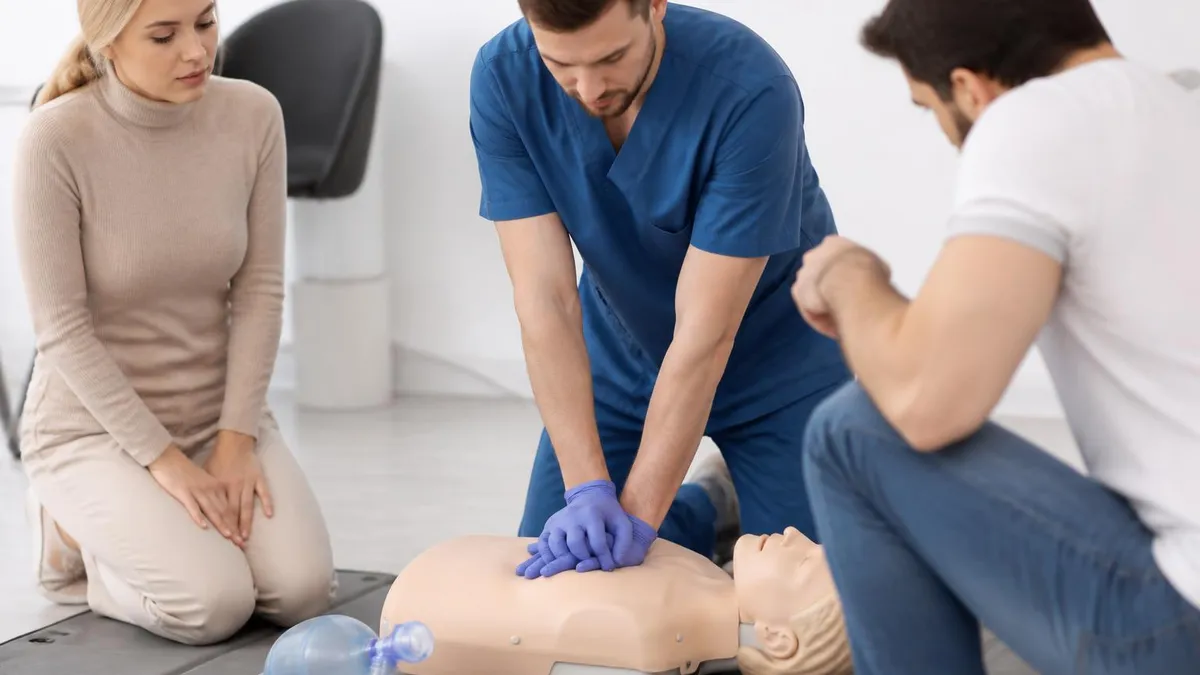
For compressions, place the heel of one hand on the center of the chest (lower half of the breastbone), place your other hand on top, and interlock your fingers. Keep your arms straight and compress hard and fast. Allow the chest to fully recoil between compressions — don't lean on the chest between pushes.
If you're trained and comfortable giving rescue breaths: after 30 compressions, tilt the head back, lift the chin, pinch the nose, create a seal over the mouth, and give 2 breaths of about 1 second each. Watch for chest rise. Then return immediately to compressions. Continue until EMS arrives, an AED is available, the person recovers, or you can no longer continue. If a second trained person is present, switch every 2 minutes to maintain compression quality.
Once you're comfortable with the basics, formal training helps enormously. Finding red cross cpr classes near me puts you in a hands-on environment with mannequins and real-time instructor feedback — the kind of practice that makes the difference when it counts.
CPR Technique by the Details
- Hand placement: Heel of hand on center of chest, second hand on top, fingers interlocked
- Body position: Kneel beside the person, arms straight, shoulders directly over your hands
- Depth: Push down at least 2 inches (2–2.4 inches for adults) — don't be afraid to push hard
- Rate: 100–120 compressions per minute — roughly the beat of "Stayin' Alive" by the Bee Gees
- Full recoil: Let the chest fully rise between each compression — don't lean on the chest
- Minimize interruptions: Pauses in compressions should be less than 10 seconds
Hands-Only CPR vs. Traditional CPR
Not all CPR situations call for the same approach. The two main options are hands-only CPR (compression-only) and traditional CPR (compressions plus rescue breaths). Understanding the difference helps you respond correctly — and confidently.
Hands-only CPR skips the rescue breaths and delivers continuous chest compressions. The AHA recommends it for untrained bystanders witnessing sudden cardiac arrest in adults. It works because — immediately after sudden cardiac arrest — there's still oxygen in the blood and lungs. Compressions keep it circulating. It also removes the hesitation many people feel about mouth-to-mouth contact, meaning more bystanders actually act when it matters most.
Traditional CPR with rescue breaths is recommended when oxygen delivery is critical: for children and infants (whose cardiac arrest is more often caused by respiratory failure), drowning victims (already oxygen-depleted before cardiac arrest), drug overdose cases, and any trained rescuer who can perform rescue breaths correctly and confidently.
If you're unsure which approach to use, hands-only CPR is far better than no CPR. A 911 dispatcher can guide you in real time. When you want to be prepared for both scenarios, knowing cpr classes how long they run helps you plan — most adult courses take just a few hours and cover both techniques with mannequin practice.

Hands-Only CPR: Pros and Cons
- +Easier for untrained bystanders to perform correctly under pressure
- +No hesitation about mouth-to-mouth — more bystanders actually act
- +Effective for witnessed sudden cardiac arrest in adults
- +911 dispatcher can guide you through it step by step over the phone
- +Maintains compression quality with no interruptions for rescue breaths
- −Less effective for children, drowning victims, or drug overdose cases
- −Blood oxygen levels drop after several minutes without rescue breaths
- −Not the best choice for trained rescuers — traditional CPR produces better outcomes when done correctly
- −Compressor fatigue sets in faster without natural rest breaks from breath-giving
- −No airway management without the rescue breath component
When to Perform CPR
Knowing when to start CPR is just as important as knowing how. The signs of cardiac arrest are distinct — and you need to recognize them fast.
Start CPR immediately if someone is unresponsive and doesn't react to shouting or a firm tap on the shoulders, and if they're not breathing normally — no breathing at all, or only occasional gasps (called agonal breathing). You don't need to confirm a pulse. Checking for a pulse is difficult even for medical professionals, and the delay costs precious seconds. If the person is unresponsive and not breathing normally, start CPR.
Don't wait for certainty. If you're not sure whether someone is in cardiac arrest, err on the side of action. Starting CPR on someone who doesn't need it carries minimal risk — failing to start it on someone who does can be fatal. The consequences of inaction are irreversible. The consequences of acting wrongly are usually manageable.
There are situations where CPR isn't appropriate: if the person is conscious and breathing normally; if there are obvious signs of biological death; if a valid Do Not Resuscitate order is present; or if the scene is unsafe and you can't protect yourself. In every other scenario, act immediately. Call 911 first (or have someone else call while you begin), then start CPR. Dispatch operators are trained to assess the situation with you and guide you through every step. You don't need to be certain — you just need to start.
CPR and AED: A Powerful Combination
CPR is most effective when paired with an Automated External Defibrillator (AED). These portable devices are found in airports, malls, gyms, schools, and many workplaces — designed to be used by anyone, not just medical professionals. Many people walk past them every day without knowing what they are.
An AED analyzes the heart's electrical activity and delivers a controlled shock to restore normal rhythm. CPR alone rarely restarts the heart. What CPR does is keep the person viable — maintaining blood flow to the brain — while the AED corrects the underlying electrical problem causing the arrest.
When an AED is available, use it as soon as possible. Don't stop CPR to go looking for one unless someone else can retrieve it. When it arrives, turn it on — voice prompts guide every step. Attach pads as shown (upper right chest below the collarbone; lower left side below the armpit), stand clear during analysis, follow prompts for shock delivery, then resume CPR immediately after the shock. The AED re-analyzes every 2 minutes and continues guiding you through the sequence.
You cannot accidentally shock someone who doesn't need it — the device won't allow it. CPR training courses typically cover AED use alongside compressions and rescue breaths. If you're planning your certification, checking how long is cpr certification good for beforehand helps you schedule renewals — most certifications are valid for 2 years.
AED Quick Reference
Place Pad 1 on the upper right chest below the collarbone. Place Pad 2 on the lower left side below the armpit. For children under 8, use pediatric pads if available. Keep pads at least 1 inch away from any pacemaker or implanted device. On a hairy chest, press firmly and peel to remove hair, or shave quickly if a razor is available.
"Analyzing rhythm" — stop CPR, ensure no one is touching the patient. "Shock advised" — clear the patient, press the shock button. "No shock advised" — resume CPR immediately. "Resume CPR" — begin 30 compressions then 2 breaths, or continuous hands-only compressions. The AED re-analyzes every 2 minutes and guides you through each cycle.
Continue CPR without interruption. Send someone to locate the nearest AED — most public buildings are required to have one. If you're alone, call 911 first, then start CPR. Do not leave the victim to search for an AED yourself. Quality bystander CPR alone significantly improves survival odds until a defibrillator arrives.
Who Should Learn CPR?
Short answer: everyone. But some people are especially positioned to save lives and should make CPR training a genuine priority.
Parents and caregivers carry an obvious responsibility. Children can choke, drown, or experience sudden medical emergencies. Knowing pediatric CPR — which uses slightly different technique for infants and young children — can mean everything in those terrifying moments. If you have kids at home, CPR certification isn't optional. Neither is knowing where your nearest AED is.
Teachers, coaches, and school staff spend hours each day with kids who push themselves physically, eat too fast, or have undiagnosed heart conditions. A coach who knows CPR can respond before the ambulance even dispatches. Many school districts now require it, and for good reason. Athletic fields and gymnasiums are high-risk environments.
Gym members and fitness instructors should recognize that high-intensity exercise raises cardiac risk, especially for older adults or those with undetected conditions. Most gyms have AEDs on site. Knowing how to locate and use one matters far more than knowing where the water fountain is.
Healthcare workers — nurses, EMTs, medical assistants, doctors — need CPR certification as a job requirement. Understanding how long does cpr certification last is essential for staying compliant with employer and licensing requirements without letting credentials lapse unexpectedly.
Everyday people don't need a professional reason to learn. If you live with someone who has heart disease, if you're regularly around elderly relatives, or if you simply want to be prepared — that's reason enough. Searching for heart association cpr classes gives you access to AHA-certified courses in every state, with both in-person and blended learning options available.
CPR Readiness Checklist
- ✓Take a hands-on CPR course (Red Cross or AHA) — not just a video
- ✓Practice on a mannequin to get compression depth and rate right
- ✓Locate AEDs in your workplace, gym, and frequently visited public spaces
- ✓Recertify every 2 years to stay current with updated guidelines
- ✓Teach family members the basics of hands-only CPR
- ✓Save your local emergency number and know how to describe your location clearly
CPR Success Rates and What the Research Shows
The numbers around CPR are both sobering and encouraging. Without any bystander intervention, survival for out-of-hospital cardiac arrest runs roughly 5 to 10%. When bystander CPR is performed promptly, that rate doubles or triples. Combined with early AED use and rapid EMS response, survival rates can reach 40 to 50%.
For every minute without CPR, the chance of survival drops by about 7 to 10%. A 5-minute delay — roughly the time it might take someone to hesitate and then decide to act — could cut survival odds in half. The math is stark. Hesitation costs lives. It's a sobering calculation that makes the case for bystander action more powerfully than any training slogan ever could.
Hands-only CPR has been shown as effective as traditional CPR for adult witnessed cardiac arrest in the first several minutes. A landmark study in the New England Journal of Medicine found no significant difference in survival to hospital discharge between the two approaches for adults in out-of-hospital cardiac arrest. That research drove the AHA's recommendation for untrained bystanders to use hands-only CPR — removing the barrier of discomfort around rescue breaths and making it more likely that someone nearby will actually act.
When defibrillation occurs within 3 to 5 minutes of collapse, survival rates can exceed 50%. Yet only about 2.7% of cardiac arrest victims receive bystander defibrillation before EMS arrives. More trained bystanders means more lives saved. It really is that direct. The technology exists, the evidence is clear, and the limiting factor is simply the number of people who know what to do.
CPR Questions and Answers
Getting Trained: Your Next Step
Reading about CPR is a start — but it's not enough. The muscle memory for correct compression depth and rate only develops through practice on a mannequin. Without that tactile feedback, you won't really know if you're pushing hard enough when the moment comes. Videos and articles explain the concept. A mannequin teaches your hands what 2 inches of compression depth actually feels like — and that difference is everything.
Fortunately, getting trained has never been easier. The American Red Cross and AHA offer courses in virtually every city, with flexible scheduling and multiple formats — in-person, blended (online knowledge plus in-person skills check), and even workplace group training. A basic adult CPR course typically takes 2 to 3 hours. A full Heartsaver or Basic Life Support course covers adult, child, and infant CPR plus AED use and may take a half day. Neither will eat your entire weekend.
Most certifications are valid for 2 years, after which a renewal course — usually shorter than the original — brings you current on any guideline changes. If you want to verify timelines before signing up, check how long is cpr certification good for at the certifying organization's site. Some people prefer to do a free online review before their in-person class — you'll spend more time practicing compressions rather than reviewing concepts, which is the best use of your time.
CPR is one of those skills you hope you never need — but if you do, you'll be profoundly glad you have it. And so will the person whose life you save.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.
Join the Discussion
Connect with other students preparing for this exam. Share tips, ask questions, and get advice from people who have been there.
View discussion (2 replies)