MRI Accident: Causes, Risks & How Facilities Prevent Them
Learn what causes MRI accidents, the most common types of safety incidents, and how MRI facilities use screening protocols to keep patients safe.
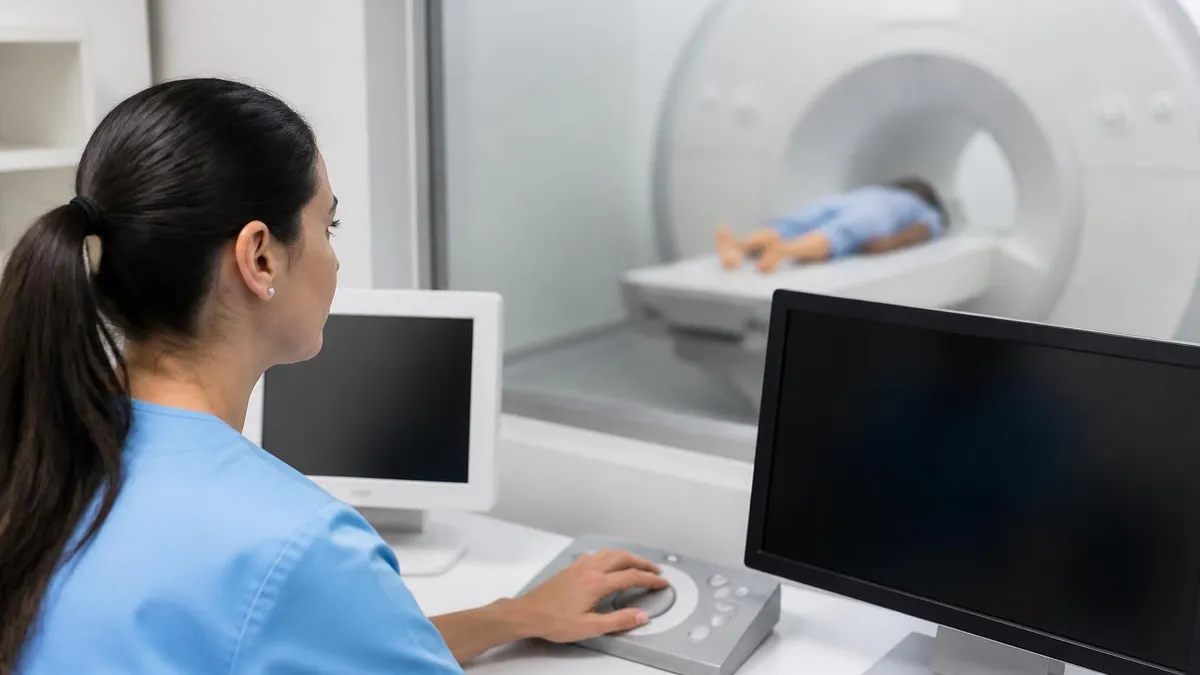
MRI accidents are rare — but when they happen, they can be dramatic and, in some cases, life-threatening. Every year, a small number of serious incidents occur in MRI suites around the world, almost all of them preventable. Understanding what causes these accidents, who's at risk, and how modern facilities work to stop them is essential — whether you're a patient preparing for a scan, a healthcare professional, or someone studying for an MRI safety certification.
An MRI scan uses an extraordinarily powerful magnetic field — far stronger than anything in ordinary daily life — to produce detailed images of the body's internal structures. That same power is also what makes the MRI environment uniquely hazardous. Get the safety protocols wrong, and objects that seem harmless in any other room can become dangerous projectiles in seconds.
This guide walks you through everything you need to know: the physics behind MRI accidents, documented incident types, who faces elevated risk, and the layered safety systems that responsible facilities use to protect patients and staff. We'll keep it factual and calm — because the goal isn't to frighten anyone, it's to inform.
- Projectile effect: Ferromagnetic objects — oxygen tanks, scissors, IV poles, even small tools — can be yanked into the MRI bore at high speed.
- Implant heating: Metal implants, tattoos with metallic inks, and conductive jewelry can heat dangerously during a scan.
- Pacemaker interference: Active implanted devices may malfunction or be reprogrammed by the magnetic field.
- Contrast reactions: Gadolinium-based contrast agents carry a small risk of allergic reaction, including rare cases of anaphylaxis.
- Hearing damage: The loud acoustic noise of MRI can cause temporary or, rarely, permanent hearing threshold shifts without proper ear protection.
Before we go deeper, it helps to understand what MRI meaning actually involves on a physical level. MRI stands for Magnetic Resonance Imaging. The scanner generates a magnetic field measured in Tesla — most clinical MRI machines operate at 1.5T or 3T, though research systems can reach 7T or beyond. For reference, the Earth's magnetic field is roughly 0.00005T. That staggering difference explains why the MRI room is treated as a controlled zone requiring strict access protocols.
The most fundamental hazard in any MRI suite is the magnetic field itself — and it's always on. Unlike X-ray machines or CT scanners, superconducting MRI magnets can't simply be switched off between patients. The field is continuously active, even when no scan is in progress. That's a fact that surprises many people, including some healthcare workers who haven't received formal MRI safety training.
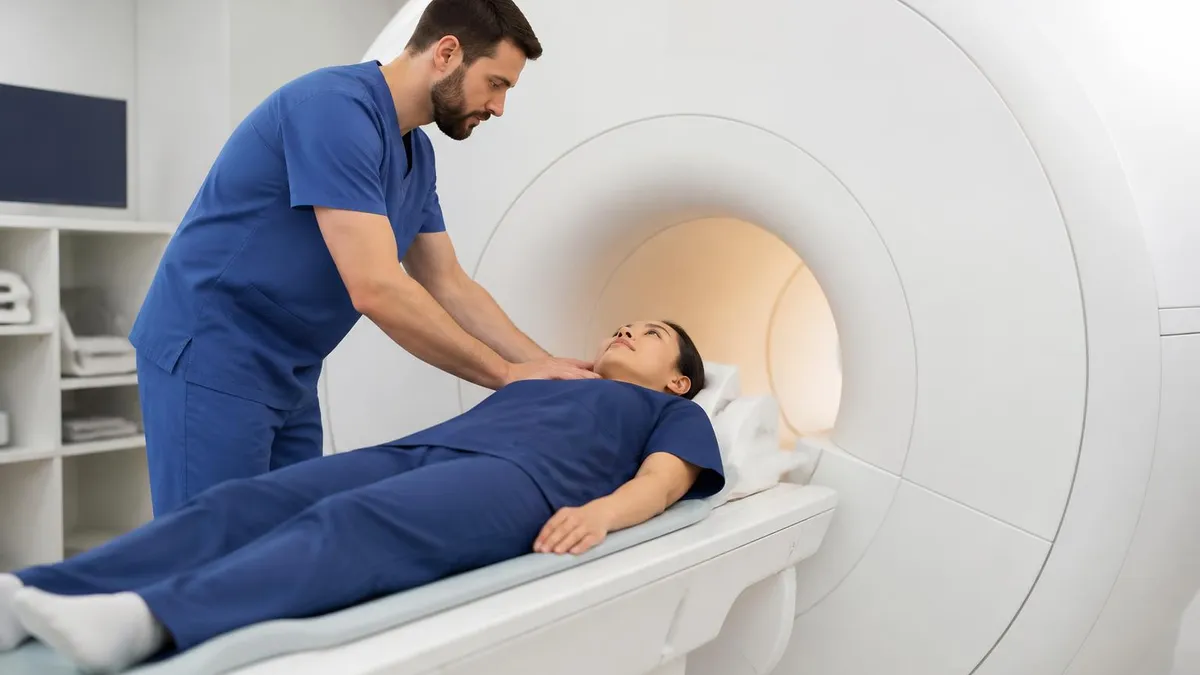
What Causes MRI Accidents: The Projectile Effect
The single biggest cause of MRI accidents is the projectile effect — sometimes called the missile effect. When a ferromagnetic object enters the MRI room, the magnetic field exerts an attractive force on it. The closer the object gets to the magnet bore, the stronger that force becomes. Objects can accelerate from a gentle pull to a high-speed projectile in a fraction of a second.
Think about it this way: a full oxygen cylinder weighing around 10 kg, pulled into a 1.5T magnet, can reach speeds comparable to a car accident. The force follows an inverse-square relationship with distance — which means doubling your proximity to the bore quadruples the pull. Objects that seem manageable to hold at the room entrance can become uncontrollable at the scanning table.
The force doesn't care whether the object belongs to a patient or a member of staff. Inexperienced personnel entering the room without proper checks, or emergency responders rushing in without MRI safety awareness, are common factors in reported accidents.
Common Objects Involved in Projectile Accidents
- ✓Oxygen tanks and gas cylinders
- ✓IV poles and infusion pumps
- ✓Scissors, clamps, and surgical instruments
- ✓Mop buckets and cleaning equipment
- ✓Chairs and wheelchairs with metal components
- ✓Gurneys and patient transport equipment
- ✓Personal items: keys, phones, belt buckles
- ✓Medical equipment brought in during emergencies
- ✓Service weapons carried by security or police personnel
Famous Documented MRI Accidents
Several well-documented accidents have shaped how the medical community approaches MRI safety protocols. Without identifying any victims by name, the pattern across these incidents is remarkably consistent.
One of the most widely cited accidents involved a young child undergoing sedation for an MRI. An oxygen tank was brought into the scan room by an attendant who was unfamiliar with the magnetic hazard. The tank was pulled from the attendant's grip and struck the child inside the bore — resulting in fatal head trauma. This incident triggered major reviews of MRI safety standards across the United States and helped drive adoption of mandatory ferromagnetic screening.
In another documented case, a patient with a previously unidentified metal fragment in their eye experienced severe eye movement and hemorrhaging during a scan. Metal fragments — particularly from industrial work like grinding or welding — are invisible on standard visual inspection. Only targeted imaging or screening can detect them. The lesson: occupational history matters during pre-scan screening.
Other documented incidents include a cleaning worker entering the bore room with a metal mop bucket that struck the magnet housing, and a patient with an outdated pacemaker whose device was reprogrammed by the magnetic field causing a dangerous cardiac arrhythmia. Each of these events has a common thread: a breakdown in the screening and access control system that's supposed to prevent exactly this kind of incident. They're not evidence that MRI is inherently dangerous — they're evidence that safety protocols work, and skipping them doesn't.
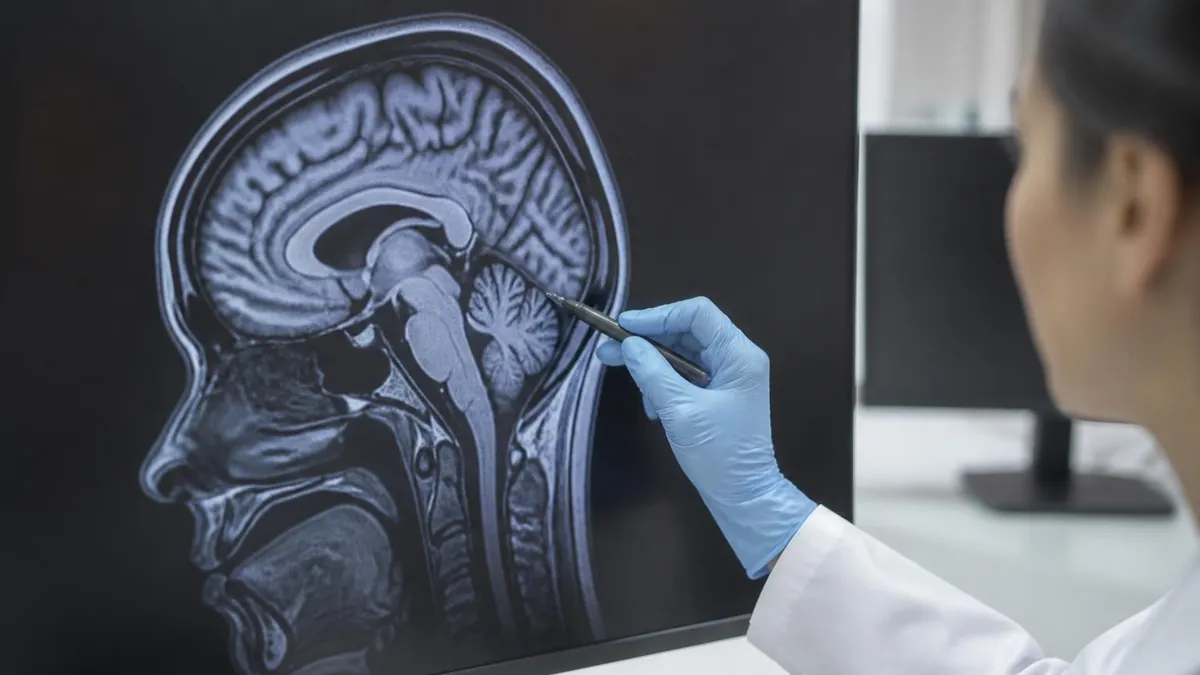
ACR MRI Safety Zone Classifications
The American College of Radiology (ACR) defines four MRI safety zones to control access and reduce accident risk:
- Zone I: General public areas outside the MRI environment — waiting rooms, hallways.
- Zone II: Interface between Zone I and the controlled MRI environment — reception, screening area. Patients are interviewed and screened here before proceeding further.
- Zone III: Restricted area where the fringe field exists — only screened individuals allowed. MRI personnel control all access.
- Zone IV: The MRI scanner room itself — the highest-risk area. Only fully screened, trained personnel and patients may enter.
Breaches of Zone III or IV access are a primary cause of projectile accidents.
Types of MRI Safety Incidents
Projectile events get the most attention, but they're not the only category of MRI accident. Understanding the full spectrum helps you recognize what protective measures are relevant for different patients and situations.
Burns from Conductive Materials
Burns are one of the more underreported MRI hazards. They occur when conductive materials — metallic implants, tattoo inks containing iron oxide pigments, EEG electrodes, or even certain clothing dyes — form loops in the RF (radiofrequency) field and generate heat. The RF field used to excite hydrogen atoms during imaging can induce electrical currents in any closed conductive loop in contact with the patient's skin.
Most burns are first- or second-degree and affect small skin areas — painful but not life-threatening. However, internal heating from deeply placed implants is harder to detect and potentially more serious. Items associated with burns include monitoring cables looped on the skin surface, metallic tattoo inks (particularly older dark pigments), retained surgical clips or staples, poorly positioned surface coils touching skin, and transdermal medication patches with metallic backings.
Hearing Damage
MRI machines are loud. The acoustic noise comes from the gradient coils — rapidly switching magnetic fields that vibrate the coil housing during image acquisition. Peak noise levels in some sequences can exceed 130 dB SPL, comparable to a jet engine at close range. Exposure without hearing protection can cause temporary threshold shift (TTS) — a temporary reduction in hearing sensitivity — and rarely, permanent noise-induced hearing loss (NIHL). Foam earplugs or MRI-compatible headphones reduce noise exposure by 15–30 dB.
Contrast Agent Reactions
Gadolinium-based contrast agents (GBCAs) are used in a significant proportion of MRI scans to enhance visualization of soft tissues, tumors, and vascular structures. Most patients tolerate GBCAs without any reaction. But a small percentage experience adverse events ranging from mild (nausea, headache, transient warmth) to severe (anaphylaxis — rare but potentially fatal). A separate concern is nephrogenic systemic fibrosis (NSF) — a serious condition affecting patients with severe kidney disease exposed to older GBCA formulations. Modern macrocyclic GBCAs have dramatically reduced this risk.
Claustrophobia-Related Incidents
Not every MRI incident involves physics. Claustrophobia affects an estimated 5–10% of patients undergoing MRI, and severe anxiety during a scan can lead to sudden movement, panic attacks, or falls during the post-scan process. Open MRI systems and sedation protocols address many claustrophobia cases — but the psychological component of MRI safety is genuinely underappreciated compared to the magnetic hazards.
Who Is at Risk in an MRI Environment
Risk in the MRI suite isn't equally distributed. Certain patient populations require heightened scrutiny during screening — and in some cases, MRI may be contraindicated entirely or require specialist consultation before proceeding. The challenge is that many risk factors aren't immediately visible. You can't tell by looking at someone whether they have a cochlear implant magnet, a retained orbital fragment, or a pacemaker with no MRI clearance. That's exactly why verbal and written screening has to be thorough every time — not just for new patients, but for returning ones too.
Pacemaker and ICD patients face some of the highest risks. Older devices are often MRI-unsafe. Even MR-conditional devices require specific scan parameters and cardiac monitoring. The magnetic field can reprogram device settings, inhibit pacing, or in worst cases cause device malfunction during critical cardiac moments. This is one area where the stakes are highest and the margin for error is smallest.
Cochlear implant recipients are another high-risk group. Most cochlear implants contain ferromagnetic components and are typically MRI-unsafe unless a specific protocol is followed. The magnet in the implant can flip or displace, causing severe pain and requiring surgical repositioning. Some newer implant models are designed with removable or fixed magnets specifically to facilitate MRI access — but that still requires verification beforehand.
Patients with intracranial aneurysm clips face risks tied to clip material. Older clips may be ferromagnetic — the torque exerted by the MRI field on a clip near a cerebral artery is a potential catastrophe. Pre-scan verification of clip manufacturer and model is essential, not optional. When records are unavailable, imaging with CT or plain X-ray may help characterize the clip before an MRI decision is made.
Industrial workers and military veterans may carry retained metal fragments from prior injuries. Orbital foreign bodies are particularly dangerous — even a tiny metallic fragment near the optic nerve can move enough to cause vision loss. Standard X-ray orbital imaging is used to screen high-risk patients before any MRI. Don't skip this step just because a patient reports no known injury history — many metallic eye injuries go unnoticed at the time.
Staff risk is often overlooked. MRI technologists, radiologists, nurses, and ancillary staff who work in or near Zone III/IV are occupationally exposed to the static magnetic field. While chronic low-level field exposure isn't known to cause harm at clinical strengths, safety discipline matters for another reason: complacency.
Staff who work in the MRI environment daily can develop familiarity bias — forgetting to screen a personal item, holding a door open for an unscreened colleague, or assuming a piece of equipment is MRI-safe without checking. Never bringing ferromagnetic items into the controlled zone is critical for everyone who works near an MRI machine.
MRI Incident Types at a Glance
The projectile (missile) effect is the most dramatic MRI hazard. Ferromagnetic objects are pulled toward the bore with force that increases sharply the closer they get. An oxygen cylinder can accelerate to dangerous speeds in under a second. Even small objects — scissors, pens, badges — can cause injury when traveling at high velocity inside a confined bore room. Prevention relies on strict Zone IV access control and ferromagnetic detection before any object enters the room.
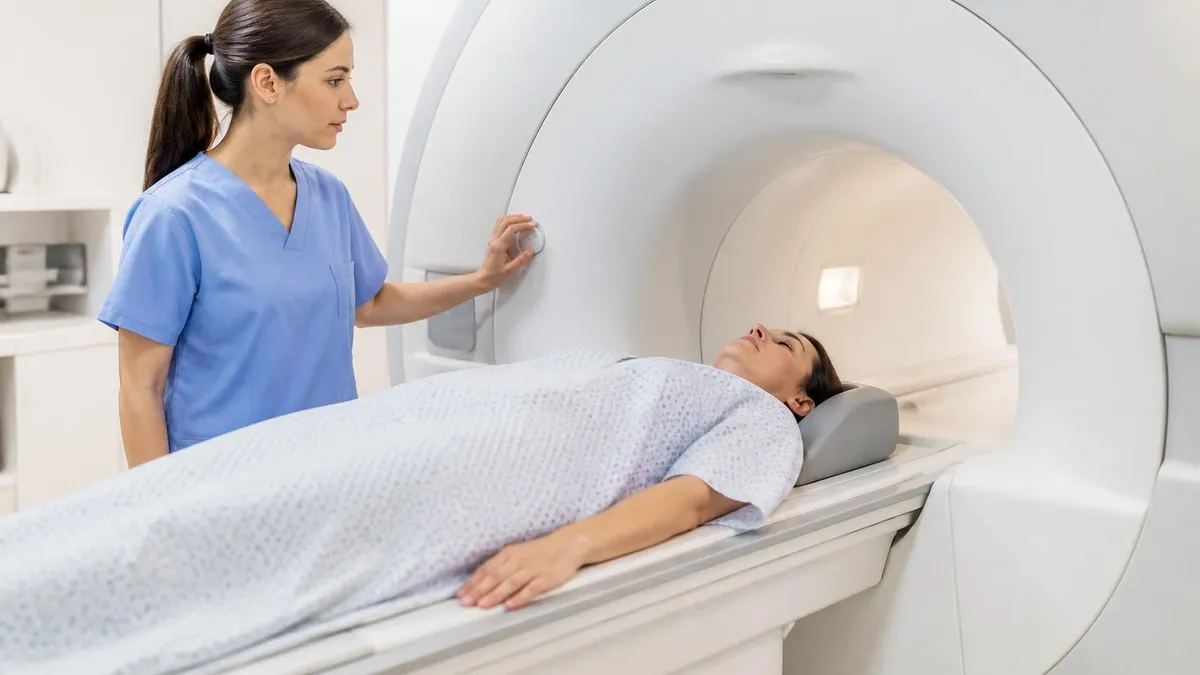
MRI Safety: Benefits vs. Limitations
- +MRI provides unparalleled soft tissue contrast with no ionizing radiation
- +Modern ferromagnetic detection systems catch most metallic objects before Zone IV
- +MR-conditional implant classifications allow many device patients to be scanned safely
- +Standardized ACR zone system and mandatory staff training have significantly reduced accident rates
- +Open MRI and 3T wide-bore systems reduce claustrophobia-related incidents
- −The magnetic field is always on — there is no safe idle state for the MRI room
- −Many implant safety classifications are device-specific and require time-consuming verification
- −Emergency response in the MRI suite is complicated by the need to screen all responders
- −Hearing protection compliance is imperfect, particularly in pediatric or sedated patients
- −Older MRI machines may lack modern safety features like RF monitoring or ferromagnetic detectors
How MRI Facilities Prevent Accidents
Modern MRI facilities use a layered approach to safety — no single measure is sufficient on its own, but together they create a system where accidents become very unlikely. Understanding this system is central to any MRI safety certification curriculum.
Patient and Staff Screening
Screening is the first and most important line of defense. Before entering any restricted zone, every patient and accompanying staff member completes a standardized MRI safety questionnaire. It covers all surgical implants, devices, and prior procedures; history of metal-related injuries or occupational exposure; pregnancy status; tattoos, permanent makeup, or body piercings; and medication patches and external devices.
The questionnaire should be reviewed by a qualified MRI safety professional — not delegated to administrative staff or handled as a checkbox formality. Critically, verbal confirmation isn't enough. Patients under sedation, cognitive impairment, or language barriers may not be able to provide accurate histories.
Ferromagnetic Detection Systems
Handheld and walk-through ferromagnetic detection systems (FDS) are now widely used as a secondary screen before Zone IV entry. These devices detect ferromagnetic materials that questionnaires might miss — forgotten keys, a hair clip, or a recently placed implant the patient didn't think to mention. The ACR recommends FDS use particularly for high-throughput facilities.
Physical Access Controls and Staff Training
Zone III and Zone IV areas require controlled entry — keypad locks, swipe card access, or intercom entry — to prevent unauthorized personnel from walking into the scan room. Emergency responders must be briefed on MRI hazards before any potential response scenario. MRI technologists in the United States are typically certified through the ARRT, and the American Board of Magnetic Resonance Safety (ABMRS) offers specialist credentials for MR Safety Officers (MRSO) and MR Medical Directors (MRMD).
Emergency Quench Procedures
Every superconducting MRI magnet has an emergency quench capability — a controlled rapid de-energization that collapses the magnetic field in minutes by venting the supercoolant. Quenching is used as a last resort when someone is pinned by a projectile object and the field must be eliminated immediately. It's not casual — quenching damages the magnet and recovery is expensive — but it's lifesaving when needed.
What to Do If You're Worried About MRI Safety
- ✓Disclose every implant, surgery, injury, and metallic foreign body — let the MRI team decide what matters
- ✓Bring manufacturer documentation for any implanted device: model numbers determine MRI compatibility
- ✓Remove all jewelry and piercings before the scan, including less visible body piercings
- ✓Ask about sedation options if claustrophobia is a concern — mild anxiolytics are commonly available
- ✓Ask the technologist to explain what you'll hear — the loud banging is normal, not a malfunction
- ✓Advocate for yourself if screening feels rushed — reputable facilities welcome safety questions
- ✓Mention any recent surgeries even if you think the hardware used is 'non-magnetic' — verify don't assume
MRI Accident Legal Considerations
When MRI accidents do occur — particularly projectile injuries, implant-related burns, or contrast reactions — they frequently result in medical malpractice or negligence claims. The legal standard centers on whether the facility followed the accepted standard of care. Plaintiffs typically argue that inadequate screening, failure to verify implant compatibility, or improper access controls constituted negligence. Damages sought can include medical expenses, pain and suffering, and in catastrophic cases, wrongful death claims.
Courts have found liability in cases where facilities failed to maintain proper zone controls, where staff brought ferromagnetic objects into the scan room without screening, and where known contraindications were overlooked under scheduling pressure. The existence of published ACR and Joint Commission guidelines is double-edged: it establishes what best practice looks like, making deviation from it easier to characterize as negligence. Facilities that cannot demonstrate documented screening protocols are in a particularly difficult position in litigation.
If you experienced an injury during an MRI procedure, document everything you remember about the pre-scan screening process — or the lack thereof. Keep all medical records and imaging reports. Consult a healthcare attorney who specializes in medical device or imaging-related cases. Causation in these cases is complex, and expert radiological testimony is typically required to establish the connection between a protocol failure and the patient's specific harm. Don't delay — statutes of limitations for medical malpractice vary by state and some are as short as two years from the date of injury.
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.