Child CPR
Child CPR techniques for ages 1 through puberty. Learn compression depth, rate, rescue breaths, AED use, and certification options.

Child CPR refers to cardiopulmonary resuscitation techniques specifically designed for children typically defined as ages 1 year to puberty. Child CPR differs from both infant CPR which addresses children under 1 year and adult CPR which addresses individuals past puberty. The specific child CPR techniques reflect anatomical and physiological differences between children and other age groups requiring age-appropriate resuscitation approaches. Understanding child CPR helps parents, caregivers, teachers, and various other adults respond appropriately when children experience cardiac arrest or other life-threatening emergencies requiring immediate response.
Child CPR represents critical skill for adults responsible for child supervision. Pediatric cardiac arrest occurs less commonly than adult cardiac arrest though when it does occur, rapid effective response substantially affects survival outcomes. Most pediatric cardiac arrest results from respiratory issues rather than primary cardiac causes producing different presentation patterns than adult cardiac arrest. The age-specific approach combined with this respiratory emphasis affects child CPR technique compared to adult procedures. Building child CPR competency through training and practice supports better emergency response when needed.
This guide explains child CPR comprehensively including specific technique details for children, differences from infant and adult CPR, common causes of pediatric cardiac arrest, recognition of pediatric emergencies requiring CPR, chest compression specifics for children, rescue breath techniques for children, AED use in pediatric patients, training options for child CPR certification, common situations requiring child CPR knowledge, family preparation for pediatric emergencies, and various other aspects affecting child CPR readiness. Whether you are parent, teacher, caregiver, or anyone responsible for child supervision, understanding child CPR supports better emergency preparedness.
Child CPR Key Facts
Child CPR techniques follow systematic approach matching pediatric anatomy and physiology. Recognition of need for CPR includes checking responsiveness through tapping shoulder and shouting child name. Activating emergency response by calling 911 or having someone else call supports rapid professional response. Checking for breathing while feeling for pulse at carotid or femoral artery determines pulse status. Beginning chest compressions if no pulse or signs of circulation provides circulation support. Rescue breaths combined with compressions support oxygenation. Continuing CPR until emergency responders arrive or signs of life return supports sustained intervention.
Chest compression technique for child CPR differs slightly from adult technique. Use heel of one hand or two hands depending on child size on lower half of breastbone. Position hand on lower half of sternum avoiding xiphoid process. Compress chest approximately 2 inches deep or one third of chest depth whichever is less. Allow complete chest recoil between compressions supporting cardiac filling. Maintain compression rate of 100 to 120 per minute matching adult rate. Minimize interruptions in compressions maximizing circulation support. The proper compression technique supports effective circulation during cardiac arrest representing critical CPR component.
Rescue breath technique for child CPR uses head-tilt chin-lift to open airway followed by gentle breaths. Position child on firm flat surface. Tilt head back gently and lift chin opening airway. Pinch nose closed and create seal over child mouth. Give 2 gentle breaths each lasting about 1 second watching for chest rise. Avoid excessive force which can cause complications. After 30 compressions, give 2 rescue breaths repeating compression-breath cycle. The gentle breath approach matches pediatric anatomy avoiding lung injury from excessive ventilation pressure while supporting necessary oxygenation during cardiac arrest situations.
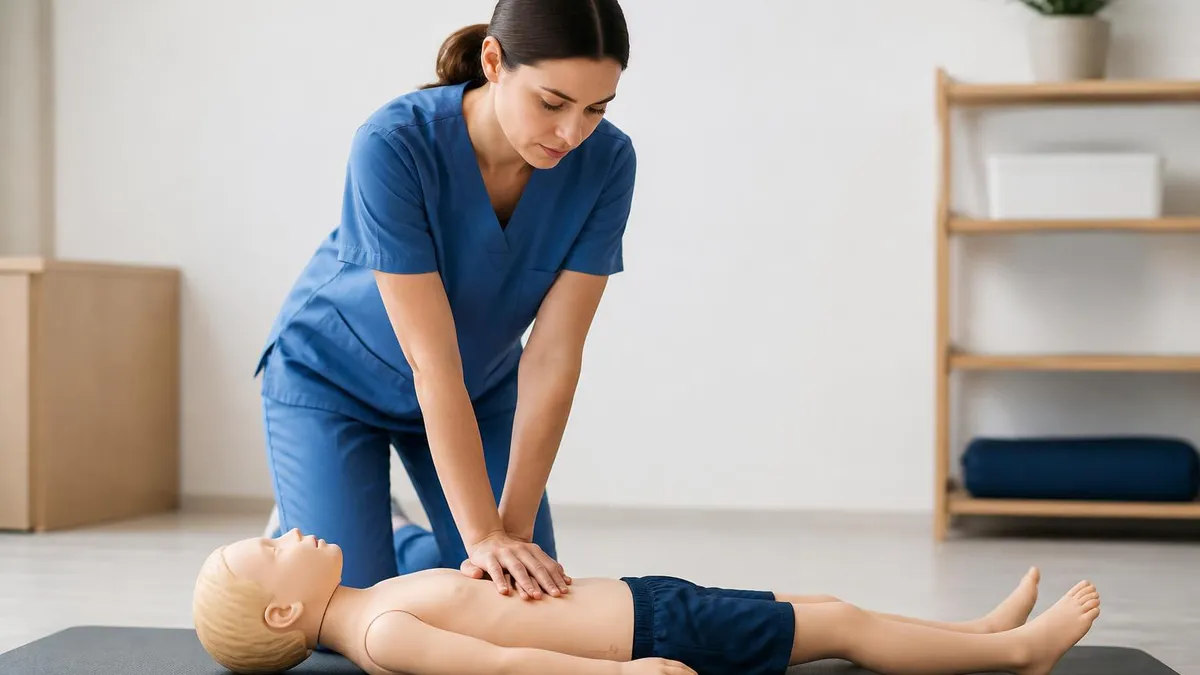
Child CPR differs from adult CPR in several specific ways. Compression depth approximately 2 inches for children versus 2.5 inches for adults reflects smaller chest size. One or two hands may be used for child compressions versus always two hands for adults depending on child size. Rescue breaths use gentler force matching smaller lungs. AED pediatric pads or pediatric dose attenuator preferred when available though adult pads can be used if pediatric not available. Single-rescuer compression-breath ratio remains 30:2 same as adults. Two-rescuer ratio changes to 15:2 for children versus 30:2 maintained for adults reflecting different professional response coordination.
Common causes of pediatric cardiac arrest differ from adult causes substantially. Respiratory failure including drowning, choking, severe asthma, and various other respiratory emergencies represents most common cause. Sudden infant death syndrome SIDS though primarily affecting infants under 1 year can rarely affect older children. Severe trauma from various injuries can produce cardiac arrest. Severe allergic reactions or anaphylaxis can produce circulatory collapse. Congenital heart conditions may produce cardiac events in affected children. Severe electrolyte imbalances from various causes can produce arrhythmias. Understanding common causes helps anticipate situations requiring CPR preparedness and prevention through addressing underlying causes when possible.
Recognition of pediatric emergencies requiring CPR includes various signs and symptoms. Unresponsiveness when checking child should trigger emergency response activation. Absent or abnormal breathing including agonal gasping suggests cardiac arrest. Cyanosis or bluish skin color particularly around lips and fingers suggests inadequate oxygenation. Limp body without normal muscle tone suggests serious illness. Various other signs including pallor, sweating, and altered consciousness may indicate medical emergencies. Rapid recognition supports prompt response which substantially affects outcomes in pediatric emergencies. Adults supervising children benefit from training to recognize and respond to these emergency signs.
AED use in pediatric patients follows specific considerations. AED Automated External Defibrillator can be life-saving when appropriate cardiac rhythm requires defibrillation. Pediatric pads or pediatric dose attenuator preferred when available reducing energy delivered for child-appropriate dose. Adult pads can be used if pediatric not available though placement may need adjustment placing one pad on chest and other on back rather than standard chest placement.
Following AED voice prompts supports correct use even by untrained rescuers. The AED technology has substantially improved pediatric emergency response when defibrillation is needed though not all cardiac arrests respond to defibrillation reflecting respiratory cause prevalence in pediatric arrests.
Child CPR Step-by-Step
Tap child shoulder and shout to determine consciousness. Unresponsive child requires emergency response activation. If responsive but distressed, monitor and provide first aid as appropriate without CPR initiation.
Activate emergency response by calling 911 or having bystander call. Mobile phones simplify rapid help summoning. Speaker mode allows continuing care while communicating with dispatcher who can guide care until responders arrive.
Look for chest rise and feel for breath while checking pulse at carotid or femoral artery for up to 10 seconds. Absent or abnormal breathing combined with no pulse indicates cardiac arrest requiring CPR initiation.
Position heel of hand or two hands on lower sternum. Compress 2 inches deep at rate 100-120 per minute. Allow complete recoil between compressions. Continue for 30 compressions before rescue breaths in single-rescuer scenarios.
After 30 compressions, open airway with head-tilt chin-lift. Pinch nose and seal mouth giving 2 gentle 1-second breaths watching for chest rise. Resume compressions immediately after breaths completing one cycle.
Continue 30:2 cycles until emergency responders arrive, child shows signs of life, or AED instructs to stop. Switch with another trained rescuer if available to prevent fatigue affecting compression quality.
Choking response represents related pediatric emergency frequently encountered. Severe choking in children requires immediate response. For conscious choking child, perform abdominal thrusts Heimlich maneuver from behind the child. Place fist just above navel below ribcage and quickly pull inward and upward. Repeat thrusts until object dislodges or child becomes unconscious. For unconscious choking child, begin CPR with chest compressions which may dislodge obstruction. Check mouth for visible object before rescue breaths removing only if visible. The choking response combined with CPR knowledge supports comprehensive pediatric emergency preparedness.
Drowning represents specific pediatric emergency commonly requiring CPR. Pediatric drowning particularly affects children near pools, bathtubs, and various other water sources. Immediate water rescue followed by CPR if needed represents standard response. Rescue breaths often particularly important in drowning given respiratory cause. Some protocols recommend 5 initial rescue breaths in drowning scenarios before beginning compression-breath cycles. Continuing CPR while waiting for emergency responders supports drowning resuscitation. The pediatric drowning prevention through pool fencing, supervision, and various other safety measures combined with CPR readiness supports better outcomes when drowning emergencies occur.
Training options for child CPR certification include various courses. American Heart Association Heartsaver Pediatric First Aid CPR AED course covers comprehensive pediatric emergency response including CPR. American Red Cross Pediatric CPR courses provide similar training. Various other organizations offer pediatric CPR training. Course length typically 4 to 8 hours. Certification typically valid for 2 years before renewal needed. Online and in-person formats accommodate various scheduling preferences. The widely available training options support community CPR preparedness producing more bystanders trained to respond to pediatric emergencies in homes, schools, and various other settings where children spend time.
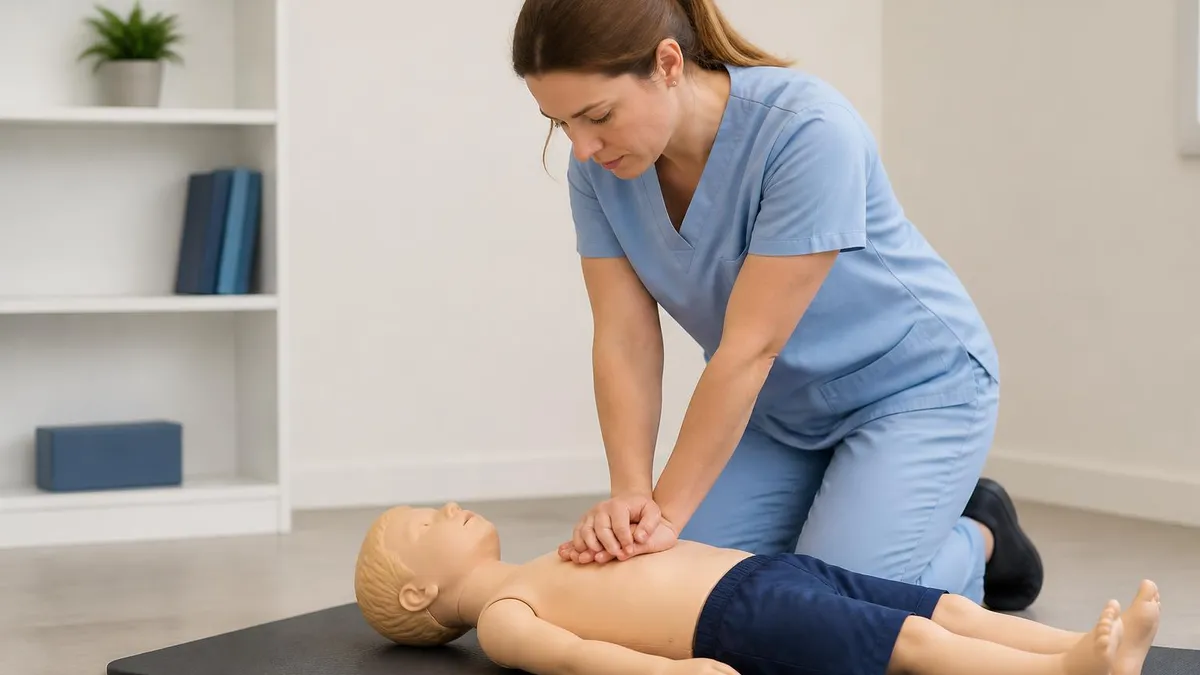
Child CPR Specific Situations
Single rescuer child CPR uses 30:2 compression to breath ratio matching adult ratio. Call 911 then begin CPR if alone with unresponsive child. After approximately 2 minutes or 5 cycles of 30:2, consider AED if available and pediatric pads or attenuator present. Continue CPR until responders arrive. Single rescuer scenarios common when caregiver discovers unresponsive child requiring immediate response without immediate help available. The 30:2 ratio represents standard for both adult and pediatric single rescuer scenarios supporting consistent rescuer approach.
Family preparation for pediatric emergencies supports faster effective response when emergencies occur. Pool safety with proper fencing reduces drowning risk. Choking prevention including age-appropriate food preparation and supervision during eating reduces choking risk. Car seat use protects against motor vehicle injuries. Smoke and carbon monoxide detectors detect environmental hazards. Medication safety storage prevents accidental poisoning. Various other safety measures prevent emergencies. Combined with CPR training, the safety preparation produces comprehensive emergency preparedness through both prevention and response capability matching family responsibility for child safety across various potential emergency situations.
School and childcare CPR considerations affect institutional emergency preparedness. Most states require some level of CPR training for childcare workers and school staff. Specific requirements vary by state and setting. Annual recertification ensures continued competency. Schools and childcare facilities maintain emergency response plans coordinating staff response when emergencies occur. AEDs increasingly available in schools and various other facilities supporting pediatric emergency response. The institutional preparedness supplements family preparedness producing comprehensive community pediatric emergency response capacity beyond individual family preparation alone.
Common mistakes during child CPR affect outcomes negatively. Hesitation to begin CPR fearing harm produces worse outcomes than imperfect CPR. Insufficient compression depth reduces circulation effectiveness. Excessive compression depth can cause injury though appropriate depth rarely causes serious harm. Inadequate chest recoil reduces cardiac filling. Excessive rescue breath pressure can cause lung injury. Interruptions in compressions reduce overall circulation. Avoiding common mistakes through proper training and confidence supports better CPR effectiveness. Training emphasizes building muscle memory supporting effective response despite emergency stress affecting all rescuers.
Imperfect CPR is far better than no CPR. Many bystanders hesitate to perform CPR fearing they will do it wrong or cause harm. Research consistently shows even imperfect CPR substantially improves survival compared to waiting for professional responders. Hands-only chest compressions without rescue breaths still provide circulation supporting brain and heart function. Beginning CPR immediately when needed matters more than perfect technique. Good Samaritan laws in most jurisdictions protect bystanders performing CPR in good faith. The willingness to act represents most important factor in pediatric CPR outcomes regardless of technique perfection.
Hands-only CPR consideration affects bystander response. Hands-only CPR involves continuous chest compressions without rescue breaths simplifying response and reducing barriers to bystander action. Hands-only CPR supports witnessed adult cardiac arrest in some scenarios. For children, traditional CPR with rescue breaths typically preferred given respiratory cause prevalence in pediatric arrest. However hands-only CPR is better than no CPR if rescue breath competency lacking. Recognizing that doing something matters more than doing nothing supports bystander engagement during pediatric emergencies even when full CPR technique not mastered.
Mental health considerations after pediatric resuscitation events affect both rescuers and family members. Even successful resuscitation produces traumatic experience for everyone involved. Stress reactions including anxiety, sleep disturbances, intrusive thoughts, and various other reactions are normal after traumatic events. Professional mental health support helps process traumatic experiences. Support groups for both successful and unsuccessful pediatric emergency outcomes provide peer support. Recognizing emotional impact and seeking support represents important aspect of pediatric emergency response beyond just the technical CPR skills involved during actual emergency situations.
The child CPR represents critical skill for adults responsible for children supporting better emergency outcomes when pediatric emergencies occur. Understanding technique specifics, age-appropriate adaptations, common emergencies requiring response, training options, and various other aspects supports effective preparedness. The investment in child CPR knowledge and training produces value through emergency response capability that could save child life. Whether parent, teacher, caregiver, healthcare worker, or any adult interacting with children, child CPR competency represents foundational emergency preparedness skill matching responsibility for child safety across various life situations.

Child CPR Preparedness Checklist
- ✓Complete child CPR certification through AHA, Red Cross, or other recognized provider
- ✓Renew CPR certification every 2 years maintaining current competency
- ✓Learn choking response specific to children including Heimlich maneuver technique
- ✓Identify nearest AED locations at home, work, schools, and frequent locations
- ✓Verify AED has pediatric pads or dose attenuator available
- ✓Maintain emergency contact information accessible at home and various locations
- ✓Practice CPR technique periodically maintaining muscle memory between certifications
- ✓Teach age-appropriate children about emergency response including how to call 911
- ✓Maintain pool safety measures including fencing if water access nearby
- ✓Prepare emergency response plans for home, school, and various other locations
Recent research on pediatric resuscitation continues informing CPR guidelines. International Liaison Committee on Resuscitation ILCOR reviews evidence periodically updating recommendations. Pediatric Advanced Life Support PALS guidelines incorporate latest evidence into healthcare provider protocols. Basic CPR guidelines for bystanders also evolve based on evidence reviews. Staying current with recommendations through periodic recertification ensures application of best evidence. The continuous evidence-based evolution of CPR guidelines supports better pediatric resuscitation outcomes over time through systematic refinement of resuscitation approaches matching current evidence and clinical experience.
International variations in child CPR guidelines exist though core principles remain consistent. European Resuscitation Council, American Heart Association, and various other regional resuscitation councils may have slight differences in specific recommendations though general approach remains similar. International travelers can apply familiar CPR techniques across countries with high confidence in effectiveness. Training in any major resuscitation council guidelines supports international applicability. The international consistency reflects shared evidence base across resuscitation science globally producing reliable bystander response capability regardless of geographic location.
The child CPR represents essential skill bridging family safety preparation with broader community pediatric emergency response capacity. Understanding child CPR comprehensively including technique, age-specific adaptations, common emergencies, training options, and various other aspects supports informed preparedness. The investment in child CPR knowledge produces value through emergency response capability protecting children when emergencies occur. Whether comprehensive certification or basic familiarity, child CPR understanding supports better outcomes for children experiencing life-threatening emergencies through bystander response complementing emergency medical services arrival across various situations.
Child CPR Knowledge Pros and Cons
- + —
- + —
- + —
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
- − —
Community CPR education extends individual training to broader public benefit. School-based CPR education for older students builds community CPR capacity. Workplace CPR training programs support emergency response in various settings. Public access defibrillation programs combine AED placement with bystander training. The community approach to CPR education produces broader CPR capability supporting better emergency outcomes across communities. Cities and communities with stronger bystander CPR rates show better cardiac arrest survival rates supporting community investment in CPR education through various programs and initiatives.
Technology integration in CPR training continues evolving. Manikin technology provides realistic practice during training. Compression depth and rate feedback devices support proper technique development. Mobile applications support CPR knowledge maintenance between certifications. Online courses combined with practical skills sessions provide flexible certification options. Virtual reality training emerges as innovative training approach. The technology evolution supports more effective CPR training producing better-prepared bystanders for pediatric and adult emergency response. Most CPR training maintains hands-on practical components reflecting CPR fundamentally physical skill requirements beyond just knowledge.
The child CPR represents fundamental life-saving skill every adult responsible for children should master. Understanding the specific techniques, age-appropriate adaptations, emergency recognition, and response approaches supports better preparedness for pediatric emergencies. The investment in CPR training and ongoing skill maintenance produces value through life-saving capability when emergencies occur. Combined with prevention measures, choking response, and various other pediatric emergency skills, child CPR competency represents core component of comprehensive emergency preparedness protecting children across various situations where they may experience life-threatening emergencies throughout daily life and various activities.
CPR Questions and Answers
The child CPR represents critical life-saving skill that all adults responsible for children should master. Understanding age-specific techniques, emergency recognition, training options, and various other aspects supports better preparedness for pediatric emergencies. The investment in proper certification and ongoing skill maintenance produces capability that could save child life. Combined with prevention measures and emergency response planning, child CPR competency represents foundational component of comprehensive child safety preparation across various potential emergency situations affecting children throughout daily activities and various life circumstances.
Building community CPR capacity through individual training combines with various community initiatives produces broader emergency response improvement. School-based education, workplace training, public access defibrillation programs, and various other initiatives expand CPR capability throughout communities. The individual training contribution to community preparedness extends beyond personal capability supporting better outcomes for everyone experiencing emergencies. Encouraging family members, friends, and colleagues to also obtain CPR training multiplies emergency response capacity beyond individual capability alone.
The child CPR landscape continues evolving with ongoing evidence-based refinement of guidelines, training approaches, and various other aspects. Staying current with periodic recertification ensures application of latest evidence. The continuing evolution supports better outcomes over time through systematic improvement in pediatric resuscitation approaches. Whether early-life adult interacting with children or experienced parent or professional, ongoing CPR competency maintenance supports continued effective emergency response capability across the various stages of life involving child interaction and responsibility for child safety.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.