Basic Life Support: BLS Skills, Training, and Certification
Basic Life Support (BLS): core skills (CPR, AED, choking), certification through AHA or Red Cross, healthcare provider requirements, and renewal.

Basic Life Support (BLS) is the foundational set of emergency response skills healthcare providers use to maintain circulation and breathing in patients experiencing cardiac arrest or respiratory failure. BLS training and certification are essentially mandatory for clinical healthcare workers — nurses, doctors, paramedics, dental staff, respiratory therapists, athletic trainers, and many other roles requiring competence in immediate life-saving response.
The BLS skill set includes high-quality cardiopulmonary resuscitation (CPR) for adults, children, and infants; automated external defibrillator (AED) operation; choking response across all age groups; team-based resuscitation in healthcare settings; and integration with broader emergency response. Quality BLS training prepares healthcare providers for the critical first minutes of cardiac arrest response that substantially affect patient survival.
BLS certification differs from lay rescuer CPR (Heartsaver) in several meaningful ways. BLS Provider courses cover same fundamental CPR skills but add healthcare-specific elements including team-based response with role assignment, bag-valve-mask ventilation technique, integration with code response in clinical settings, transition from BLS to advanced cardiac life support (ACLS) care, and various scenarios common in healthcare environments. The healthcare-focused content makes BLS appropriate for clinical work; lay rescuer courses don't include these elements making them inappropriate for healthcare provider requirements. Most clinical employers specifically require BLS Provider certification for clinical staff rather than accepting lay rescuer alternatives.
Basic Life Support Quick Facts
Major certifying bodies: American Heart Association (AHA BLS Provider) most widely accepted; American Red Cross BLS for Healthcare Providers; ASHI and HSI also offer BLS courses. Course duration: 4-5 hours initial; 3-4 hours renewal. Cost: $50-$130 typical. Format: Classroom or hybrid (HeartCode online + in-person skills). Validity: 2 years. Required for: Most clinical healthcare positions. Renewal: Schedule before expiration to avoid full re-certification.
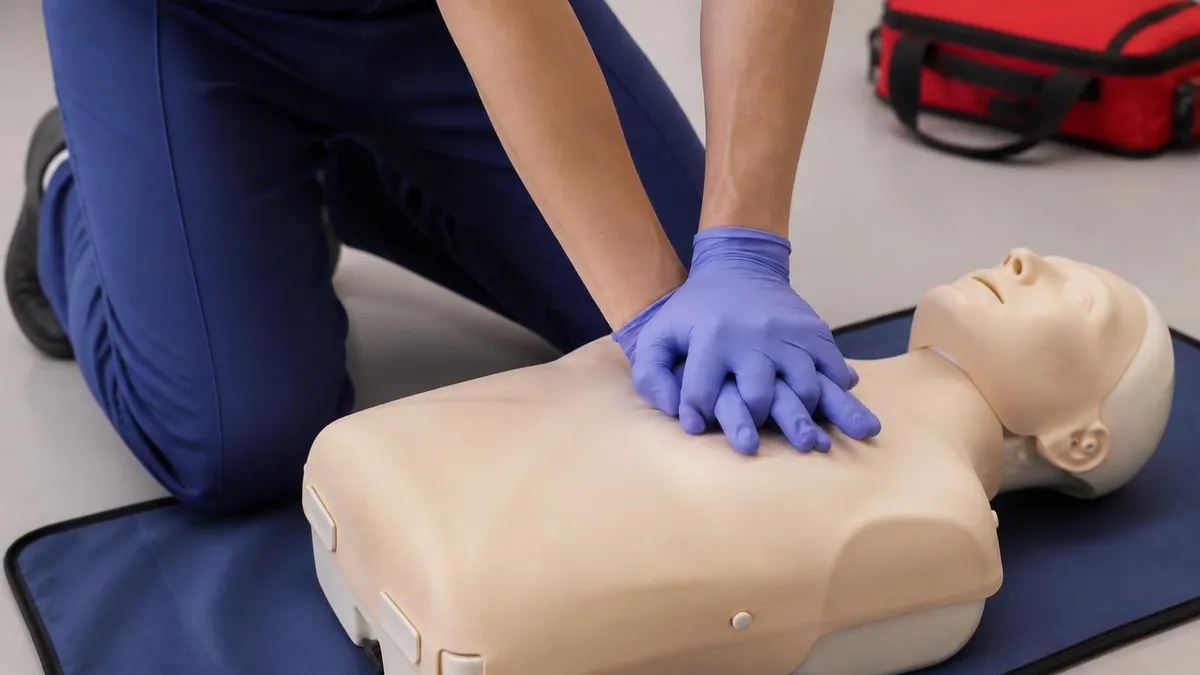
The fundamental BLS skill set begins with high-quality CPR. Compression depth at least 2 inches (2-2.4 inches optimal) for adults, about 2 inches for children, about 1.5 inches for infants. Compression rate 100-120 per minute consistently. Complete chest recoil between compressions allowing heart to refill before next compression.
Minimal interruptions in compressions — particularly important for survival outcomes per research. Proper hand placement on lower half of sternum for adults and children, two-finger or two-thumb technique for infants. Each element matters substantially for effective CPR. Modern manikins with feedback devices help students develop proper compression technique through real-time feedback during practice.

BLS Skill Components
Compression depth, rate, recoil, and minimal interruptions for adults, children, and infants.
Recognizing shockable rhythms, applying pads correctly, delivering shocks, integrating with CPR.
Recognition of mild vs severe airway obstruction, abdominal thrusts, response when victim becomes unconscious.
Effective ventilation using BVM device, proper seal, appropriate volume and rate.
Role assignment during resuscitation, clear communication, coordinated team response in healthcare settings.
Drowning, opioid overdose, pregnancy, hypothermia, electrical injury — modifications to standard BLS.
AED operation forms essential component of modern BLS. Automated external defibrillators analyze heart rhythm identifying shockable rhythms (ventricular fibrillation, pulseless ventricular tachycardia) and automatically deliver shocks when appropriate. BLS providers must learn proper pad placement (one upper right chest, one lower left side; alternative anterior-posterior placement in some situations), shock delivery while ensuring no contact with patient, and seamless integration with CPR (resume compressions immediately after shock). Modern AEDs provide voice prompts guiding rescuers through process.
Quality BLS training includes hands-on AED practice with training units (not actual AEDs) supporting genuine competence with the equipment. AEDs are increasingly available in public spaces (gyms, schools, airports, shopping centers) supporting bystander defibrillation that substantially improves survival when paired with quality CPR.
Choking response within BLS curriculum addresses airway obstruction across age groups. For conscious adults and children with severe obstruction, abdominal thrusts (Heimlich maneuver) attempt to expel obstructing object. For infants, alternating back blows and chest thrusts work better than abdominal thrusts. For pregnant women or obese individuals where abdominal thrusts impractical, chest thrusts substitute.
Recognition of mild versus severe obstruction is critical — mild obstruction (effective coughing) requires only encouragement to keep coughing; severe obstruction (no airflow) requires immediate intervention. When choking victim becomes unconscious, transition to CPR with airway check before each rescue breath looking for visible obstruction to remove. Each variation requires specific technique that BLS training develops.
Team-based resuscitation distinguishes healthcare BLS from lay rescuer CPR. In healthcare settings, multiple responders work together with assigned roles — compressor (rotating every 2 minutes to maintain quality), airway manager (BVM ventilation), AED/monitor manager, IV access (in some settings), team leader coordinating overall response, and recorder documenting events and timing. Clear closed-loop communication ensures roles are assigned and tasks completed. Quality team dynamics dramatically improve resuscitation outcomes compared to single-rescuer or uncoordinated multi-rescuer response. BLS courses include team scenario practice developing the coordination skills healthcare providers need for actual code responses.
Adult CPR sequence: Recognize cardiac arrest (unresponsive, no normal breathing). Activate emergency response (call 911 or code team). Get AED if available. Begin CPR — 30 compressions then 2 breaths if rescue breaths included; continuous compressions if compression-only. Compression depth 2-2.4 inches at 100-120/minute with complete recoil. Use AED when available. Continue cycles until advanced help arrives or patient shows signs of life. Switch compressors every 2 minutes to maintain compression quality.
Special situations require modifications to standard BLS approach. Drowning victims often have respiratory arrest preceding cardiac arrest — start with 5 rescue breaths before chest compressions in some protocols, since hypoxia caused the arrest. Opioid overdose victims may have respiratory arrest with intact pulse — naloxone (Narcan) administration alongside ventilation can rapidly reverse opioid effects.
Pregnant women in cardiac arrest receive standard CPR with manual left uterine displacement to relieve aortic compression by gravid uterus. Hypothermia victims may have very slow weak pulse — assess for longer period before starting CPR; continue resuscitation longer than for normothermic victims. Each special situation has specific modifications BLS training covers through scenario practice supporting appropriate response across diverse arrest causes.
BLS guidelines update periodically based on resuscitation science research. International Liaison Committee on Resuscitation (ILCOR) reviews evidence and publishes consensus recommendations. American Heart Association then publishes updated guidelines (every 5 years typically — 2010, 2015, 2020, 2025). Each update may modify specific protocols based on new evidence about what improves outcomes. Recent updates have emphasized continuous chest compressions with minimal interruption, expanded scope of opioid overdose response with naloxone, refinements in pediatric protocols, and post-cardiac arrest care considerations. BLS providers should renew certification before expiration to learn current guidelines rather than working from outdated protocols.
BLS certification through American Heart Association is most widely recognized and required by major hospital systems. AHA BLS Provider course covers comprehensive healthcare BLS curriculum through classroom or hybrid HeartCode format. Cost typically $50-$130 depending on training center and format. Total time 4-5 hours for initial certification. Renewal courses are slightly shorter at 3-4 hours. American Red Cross also offers BLS for Healthcare Providers covering equivalent content with somewhat different pedagogical approach. ASHI and HSI offer BLS courses primarily for workplace and community certification rather than pure healthcare provider use. Verify your specific employer's accepted certifying organizations before pursuing certification.

Don't confuse BLS Provider with Heartsaver — BLS is for healthcare; Heartsaver for lay rescuers. Don't let certification expire — full re-certification required versus shorter renewal. Don't accept online-only certification — major organizations require hands-on skills verification. Verify employer's preferred certifying organization — most accept multiple but some specifically require AHA. Maintain skills between certifications — research shows skill decay within months without practice.
Skills retention between certifications represents real challenge. Research consistently shows CPR skills decay substantially within months without practice — by 6-12 months without reinforcement, skills approach pre-training levels. This decay matters substantially because cardiac arrest emergencies happen unpredictably regardless of when training occurred.
Various approaches address skill maintenance including periodic mock code drills in healthcare workplaces, brief refresher training between formal certifications, practice manikins available in some workplaces for self-directed practice, and online refresher modules. Healthcare workers serious about CPR competence engage in skill maintenance beyond just biennial certification — most clinical settings include periodic mock codes that support skill maintenance alongside meeting formal certification requirements.
Hospital code response systems integrate BLS as foundation for broader emergency care. When patient experiences cardiac arrest, code response activates with team assembling for coordinated resuscitation. BLS skills sustain patient through initial response while ACLS-trained providers (typically physicians and ACLS-certified nurses) arrive to provide advanced interventions including defibrillation with manual settings, advanced airway management, IV/IO medications, and various other advanced techniques. The BLS-to-ACLS transition is seamless because ACLS builds on BLS foundation. Quality BLS skills among hospital staff substantially affect outcomes during the critical minutes between arrest recognition and arrival of advanced response.
For healthcare educators, BLS instruction represents fundamental teaching responsibility. AHA BLS Instructor certification supports nurses and other clinical staff teaching BLS to colleagues. Some organizations have internal training centers staffed by BLS instructors providing continuous certification training to organizational staff. Other organizations contract with external Training Centers for BLS programming. Quality BLS instruction substantially affects subsequent BLS performance — well-taught students develop genuine competence; poorly taught students may pass certification while lacking real skill. Investment in quality instruction supports actual patient care quality beyond just regulatory compliance with certification requirements.
Maintaining BLS Competence
- ✓Complete initial BLS certification through recognized organization
- ✓Renew before expiration to avoid full re-certification requirement
- ✓Participate in workplace mock code drills
- ✓Use practice manikins between certifications when available
- ✓Stay current with guideline updates through professional resources
- ✓Engage actively during certification training rather than passive attendance
- ✓Build personal protocols supporting skill maintenance
- ✓Understand differences between certification organizations if working across employers
For new healthcare professionals entering clinical practice, BLS certification timing matters. Most healthcare employers require BLS certification before starting clinical work. Some require certification before hiring; others schedule certification during initial orientation. New nurses, doctors, and other healthcare workers typically obtain certification during education (most healthcare programs include BLS in curriculum) or shortly after graduation through employer-arranged training. Career-spanning BLS certification continues through multiple renewal cycles supporting ongoing healthcare practice. Many healthcare workers maintain BLS certification continuously for entire careers spanning decades.
For healthcare workers transitioning between employers, BLS certification typically transfers between settings. Standard AHA BLS Provider certification works across most US healthcare settings. Verify accepting organizations through employer or licensure board. Some specialty settings (specific hospitals, particular nursing departments) may require specific certification organizations or have specific renewal preferences — verify before assuming any certification suffices. Most transitions work smoothly with current valid certification regardless of which organization issued it as long as recognized organization (AHA, Red Cross, ASHI, HSI) was used.
Beyond traditional clinical settings, various other professional roles benefit from BLS certification. Athletic trainers managing player emergencies. Lifeguards in healthcare-adjacent contexts. School nurses serving student populations. Occupational health staff in industrial settings. Emergency response volunteers in various community contexts. Each setting has somewhat different application of BLS skills but core skill set remains consistent. The portable foundational skills support diverse roles requiring competence in immediate life-saving response across various contexts beyond just traditional clinical employment.
The relationship between BLS and Advanced Cardiac Life Support (ACLS) represents progression in resuscitation capability. BLS covers fundamental skills available to all healthcare providers. ACLS adds advanced interventions including manual defibrillation, advanced airway management, IV/IO medications, and complex arrhythmia management. Most healthcare workers in ICU, emergency medicine, cardiology, anesthesia, and various other critical care areas hold both BLS and ACLS certifications.
ACLS requires BLS as foundation — the advanced skills build on rather than replace fundamental capabilities. PALS (Pediatric Advanced Life Support) similarly builds on BLS for pediatric scenarios. NRP (Neonatal Resuscitation Program) builds on BLS for newborn-specific scenarios. Each advanced certification extends BLS foundation for specific clinical contexts.
For research-minded healthcare workers, understanding BLS evidence base supports thoughtful practice. Decades of resuscitation research have refined BLS protocols based on what actually improves survival outcomes. Continuous chest compressions with minimal interruption improve neurologic outcomes. Bystander CPR substantially improves out-of-hospital cardiac arrest survival. Public-access defibrillation through widely-deployed AEDs adds further improvement. Each evidence-based refinement reflects better understanding of resuscitation physiology and outcomes. BLS providers serious about practice quality benefit from understanding why protocols are designed as they are rather than just memorizing protocols mechanically.
Looking forward at BLS evolution, several trends shape future practice. Continued emphasis on bystander CPR and public-access defibrillation expanding survival outcomes for out-of-hospital arrests. Technology integration including manikin feedback devices, virtual reality training scenarios, and AI-supported diagnostics. Quality measurement and improvement focus through cardiac arrest registries supporting outcome tracking. International harmonization through ILCOR continuing improving consistency across countries. Each trend supports continued improvement in resuscitation outcomes through both better training and better immediate response. Healthcare providers entering BLS-required careers today face evolving practice with continued investment in supporting skill development and patient care quality.
BLS Quick Stats
BLS Across Patient Populations
Compression 2-2.4 inches, 100-120/min, 30:2 ratio single rescuer. Standard protocol for ages 8+.
Compression about 2 inches (one-third chest depth). One or two hands depending on size. 30:2 single rescuer; 15:2 two rescuers.
Compression 1.5 inches. Two-finger or two-thumb technique. 30:2 single rescuer; 15:2 two rescuers.
Modified protocol with initial breaths before compressions in some guidelines, due to hypoxic etiology.
Naloxone (Narcan) alongside ventilation can rapidly reverse opioid-induced respiratory arrest.
Standard CPR with manual left uterine displacement to relieve aortic compression.
For people considering whether to pursue BLS certification beyond required uses, several factors support voluntary certification. Personal preparedness for family emergencies — many cardiac arrests happen at home where bystander BLS can be lifesaving. Community contribution through being trained responder available in public emergencies. Professional development supporting potential healthcare career transitions. Personal confidence and reduced anxiety about emergencies. Insurance benefits at some homeowner or auto insurers offering modest discounts for certified safety training. Each motivation supports voluntary investment in certification even when not required for current employment.
For employers requiring BLS certification across staff, organized training programs typically work better than individual employee responsibility. Group training arrangements through Training Centers provide volume pricing and convenient scheduling. Internal training centers (for larger organizations) provide ongoing certification capability. Tuition reimbursement programs cover individual certification costs in exchange for employment commitments. Each arrangement supports systematic certification across workforce. Documentation supporting both regulatory compliance and individual employment requirements should be maintained centrally for HR records and individually for employee benefit.
The cardiac chain of survival represents the framework BLS supports. Early recognition and call for help (recognizing cardiac arrest and activating emergency response). Early CPR (immediate quality compressions and ventilation). Early defibrillation (rapid AED use for shockable rhythms). Early advanced life support (ACLS interventions when available). Integrated post-cardiac arrest care (specialized care after return of spontaneous circulation). Each link in the chain affects survival outcomes substantially. BLS providers handle the first three links — the most time-critical interventions before advanced help arrives. Quality BLS performance during these critical minutes substantially affects whether patients survive cardiac arrest with good neurologic outcomes.
Compression-only CPR for adult cardiac arrest is increasingly emphasized as alternative to traditional CPR with rescue breaths. Research shows compression-only CPR by bystanders produces equivalent survival outcomes for adult witnessed cardiac arrest compared to traditional CPR with breaths. The simpler approach removes barriers to bystander response (mouth-to-mouth concerns) that prevented some bystanders from acting. AHA Hands-Only CPR campaign promotes compression-only CPR for untrained or undertrained bystanders responding to adult cardiac arrest in public settings. For healthcare providers, traditional CPR with breaths remains standard given the team-based context and BVM availability. Understanding both approaches supports appropriate response in different contexts.
For people considering BLS as personal preparedness investment beyond healthcare employment, the certification provides genuine capability for emergencies that could happen in family, community, or workplace contexts. The investment of one afternoon every two years for renewal certification produces career-spanning capability that may literally save lives. Few personal investments offer comparable potential value for the modest time and cost commitment involved in maintaining current BLS certification across many years of personal preparedness benefit beyond just employment requirements.
BLS Certification: Pros and Cons
- +Required for most clinical healthcare positions
- +Foundation for advanced certifications (ACLS, PALS)
- +Genuine life-saving capability beyond regulatory compliance
- +Reasonable certification cost ($50-$130 typical)
- +Multiple format options (classroom, hybrid)
- +Career-spanning skill supporting healthcare work
- −Renewal every 2 years required for healthcare positions
- −Skill decay between certifications affects practical readiness
- −Quality varies across instructors and Training Centers
- −Time investment for initial and renewal certifications
- −Hospital-specific preferences may limit accepted certifications
- −Online-only options not legitimate for healthcare BLS
BLS Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.