ACLS Recertification: Full Renewal Process, Cost, and What To Do If Your Card Expired
ACLS recertification guide: 5-6 hr renewal class, HeartCode, RQI, cost $150-$345, no grace period — what to do if your ACLS card expired.
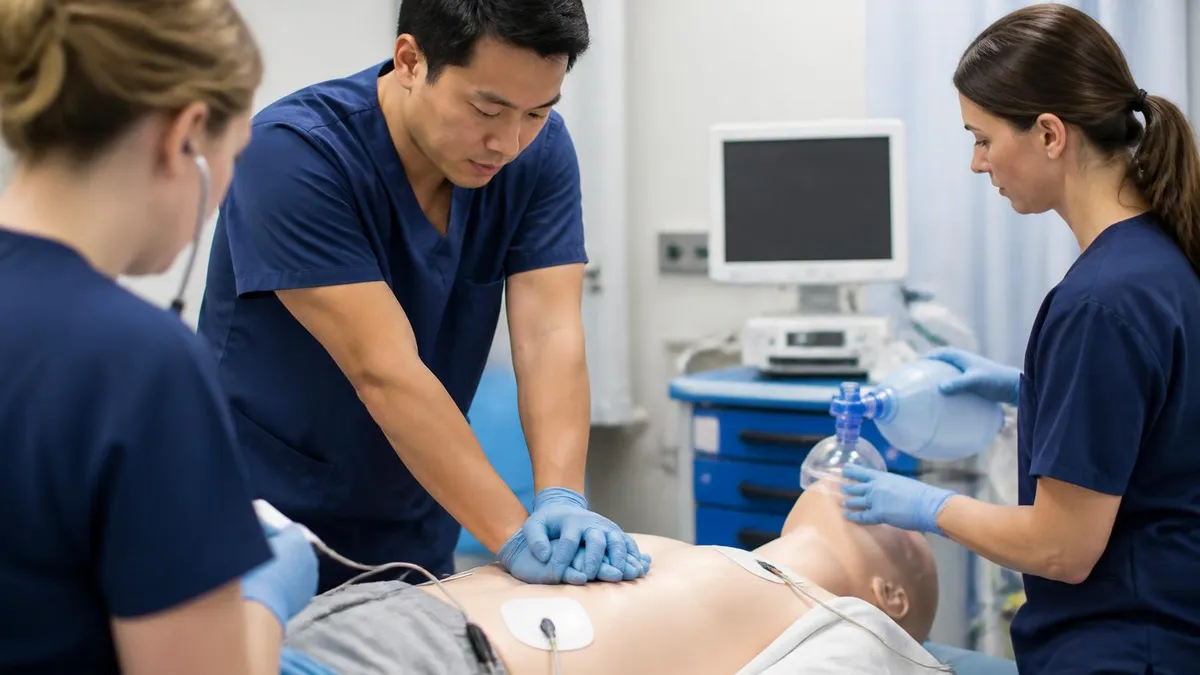
You looked at your ACLS certification card last week and the expiration date finally registered. It lapses in 60 days, or worse, last month.
Now you are trying to figure out whether you need the full initial course again, whether the online HeartCode option counts, what it costs, and how fast you can be back on the on-call list. ACLS recertification is its own animal: shorter than the initial provider course, cheaper, but ruthlessly time-sensitive.
Miss the window and you do not get a discount or a grace period. You are back to the full 12 to 14 hour initial class at full price.
This guide walks through the entire ACLS renewal process in detail. It covers the three legitimate pathways nurses and physicians use to keep their card current, exactly what shows up on the megacode skills check, what to bring on class day, and a 60-day countdown timeline you can paste into your calendar today.
Whether you trained in a hospital classroom, a Saturday-morning weekend class, or a HeartCode hybrid, the rules under the current AHA guidelines apply the same way to all of us. The good news? Most providers who plan ahead breeze through recert in a single day and walk out with a fresh eCard before dinner.
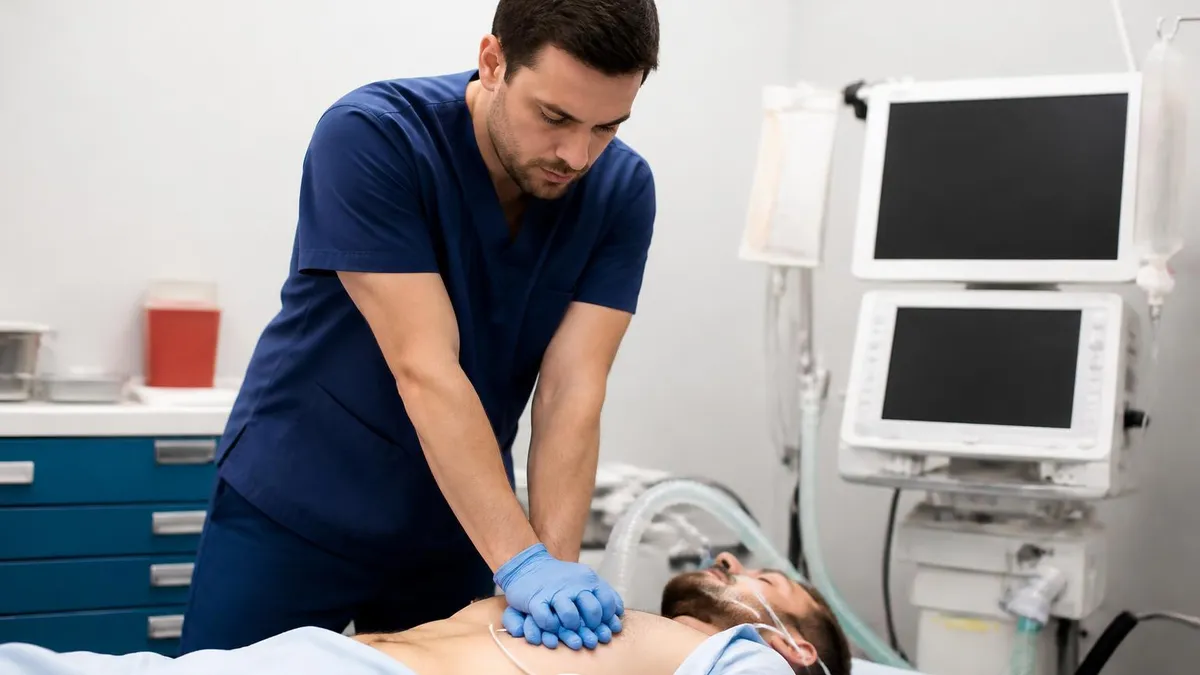
The American Heart Association does not offer a grace period on ACLS cards. The moment your expiration date passes, your card becomes invalid — even by one day. You are no longer eligible for the standard 5 to 6 hour renewal course and must complete the full initial provider course (12 to 14 hours, $250 to $350). Some hospital systems allow 30 to 60 days of administrative leeway for scheduling, but your AHA eCard is technically expired, which can affect on-call privileges, pay differential, and payroll classification. Set a calendar reminder at 60 days, 30 days, and 7 days before expiration. Book your renewal class no later than 21 days before expiration so you have a buffer if life intervenes.
The 4 ACLS Recertification Pathways Compared
The traditional in-person renewal course runs 5 to 6 hours in a single classroom session, typically scheduled for a Saturday or weekday morning. You arrive, sign in, get your ACLS Provider Manual updates, sit through condensed lecture and instructor demos covering the cardiac arrest, bradycardia, tachycardia, and acute coronary syndrome algorithms, then rotate through skills stations and megacode practice. The written test (50 questions, pass mark 84%) and a megacode scenario close the day. Cost runs $150 to $250 depending on city and training center. Pros: most reliable, instructor present for hands-on coaching, you walk out with a paper card same day. Cons: a full Saturday gone and you cannot pause to look things up.
The 3 Legitimate ACLS Recert Pathways
Best for hands-on learners who want one focused Saturday and a paper card same day. 5-6 hours, $150-$250, classroom format, instructor demonstrations, skills stations, megacode, written test all in one sitting.
- ▸5-6 hours single day
- ▸$150-$250 cost
- ▸Same-day card issuance
- ▸Best for tactile learners
Best for self-paced learners and shift workers who cannot block a full Saturday. 8-12 hours online + 1-2 hour in-person skills session, $295-$345 total, retake modules, pause anytime, two separate sign-ups.
- ▸8-12 hrs online + 1-2 hr skills
- ▸$295-$345 total
- ▸Self-paced cognitive portion
- ▸Two appointments to book
Best for hospital-employed providers whose institution subscribes. Quarterly 10-15 minute simulator sessions on the unit, no traditional renewal class, continuous quality feedback, only available through institutional contracts.
- ▸Quarterly 10-15 min sessions
- ▸$50-$100/yr institutional
- ▸No traditional class
- ▸Hospital contract required
Most providers default to the in-person renewal class because the AHA Training Center network is dense. Even mid-sized cities have 3 to 8 sites listed on the official Course Finder.
You can find ACLS classes near me by entering your ZIP code and filtering for Renewal (not Initial) on heart.org. Class sizes are typically 6 to 12 students, which means more megacode reps and less queueing at the skills stations.
Hospital-employed nurses often have their renewal scheduled and paid for by their education department. Agency, travel, and independent contractors usually pay out of pocket and submit receipts later.
HeartCode is overtaking traditional renewal among shift workers, night-shift ICU nurses, and anyone who works rotating 12-hour shifts. The cognitive portion runs as a series of branching simulated patient cases.
The AHA platform shows you a deteriorating patient. You click through assessment, intervention, and reassessment, and the system gives you feedback at each branch point. Pause mid-case, take a break, and resume hours or days later.
The downside? The platform sometimes lags on older browsers, and you cannot get the eCard until the in-person skills session is signed off by an Instructor. Plan your skills session for the week after you finish the online portion — that scheduling gap catches a lot of HeartCode students.
RQI is the newest and most disruptive option. Hospitals that subscribe install a small cart on each unit (a manikin, CPR feedback puck, and tablet running the AHA modules). Every 90 days, a notification pings your phone and you spend 10 to 15 minutes at the cart running a scenario. After four quarters, you are recertified. No Saturday gone, no precourse self-assessment, no megacode anxiety. The catch: you cannot sign up as an individual, and your renewal status is tied to that specific hospital's contract.
ACLS Recertification Cost by Pathway
Hidden cost surprises catch a lot of recertifying nurses off guard. The provider manual is the biggest one. Some Training Centers bundle it into tuition; others charge $45 to $50 separately on top of the course fee.
The 2020 edition is the current one as of this writing. The AHA refreshes guidelines roughly every 5 years, so a 2025 update is expected to roll out gradually through Training Centers.
If you have last cycle's manual on your shelf, check the edition on the inside cover. An out-of-date manual will not get you into class. The algorithms may be the same broad strokes, but the dosing tables, evidence ratings, and post-arrest targets have all shifted.
Other line items creep up. Parking at hospital training centers runs $10 to $25. Travel matters if you live rural. Then there is the cost of replacing your BLS card if it also expired at the same time (BLS is a prerequisite for ACLS in nearly all programs — $50 to $80 for a renewal). Add CE credit submission fees if your state board requires CEs reported separately from the AHA card.
Plan for roughly $300 all-in for an in-person renewal, $400 all-in for HeartCode, and budget closer to $500 if your card has already expired and you are paying for the initial course out of pocket.
One more consideration: the ACLS course retake policy. If you fail the megacode or the written test, most Training Centers offer one free retest the same day after brief remediation. If you fail the retest, you typically pay a reduced fee ($75 to $125) to re-attend the next available class, but some Training Centers charge full price. Confirm the retest policy when you book.
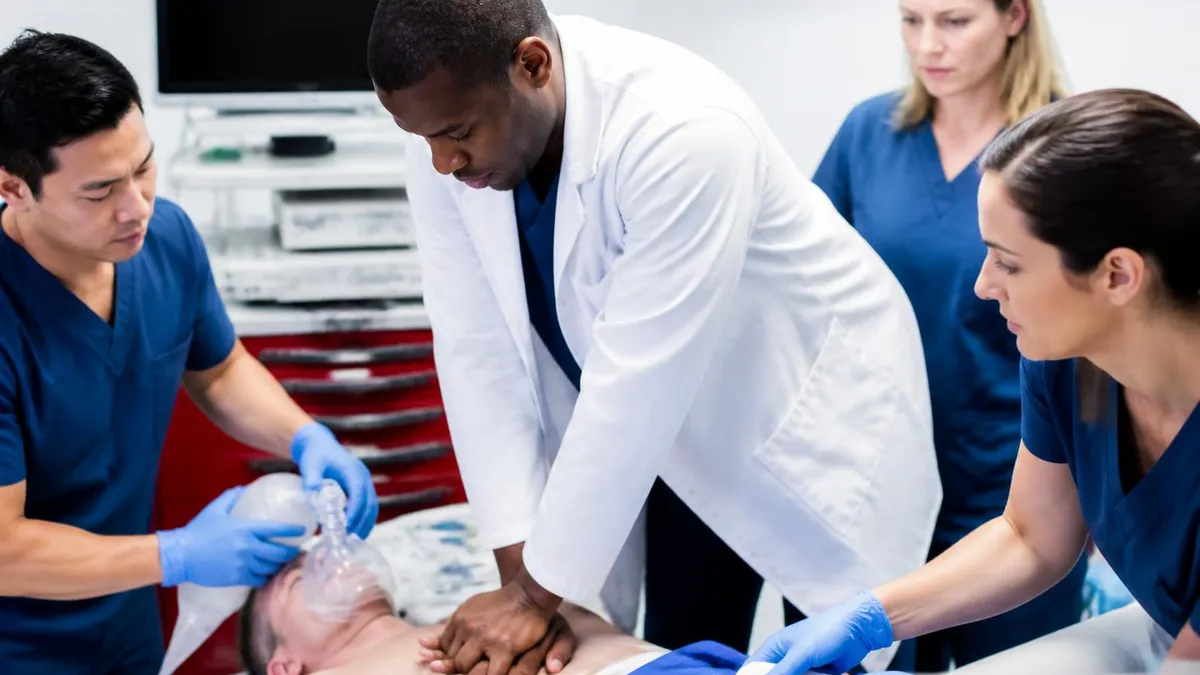
60-Day ACLS Recert Prep Timeline
Day -60: Set the Deadline
Day -50: Pick Pathway and Book
Day -35: Order Manual
Day -21: Start Precourse Self-Assessment
Day -14: Review Algorithms and Drug Doses
Day -7: Megacode Mental Rehearsal
Day 0: Class Day
The ACLS precourse self-assessment is the gatekeeper you cannot skip. AHA policy requires you to bring evidence of completion (84% or higher) to class.
Many Training Centers will not let you sign in without the printed certificate. The assessment runs about 50 multiple choice questions covering rhythm recognition, pharmacology, and BLS basics.
You can retake it as many times as needed, and the questions rotate so you do not see the same set twice. Plan 60 to 90 minutes for the first attempt, and 30 minutes for any retake. Score 84% the first time and you save yourself an evening.
Rhythm strip recognition is where most recertifying nurses lose points. You will see V-fib, V-tach (monomorphic and polymorphic), asystole, PEA (organized rhythm + pulseless), sinus bradycardia, sinus tachycardia, atrial fibrillation, atrial flutter, supraventricular tachycardia, and several AV block patterns.
The AV blocks specifically: first-degree AV block, second-degree Mobitz I (Wenckebach) and Mobitz II, third-degree (complete) heart block, and idioventricular rhythm. If any of those make you hesitate, spend 30 minutes with a free rhythm strip app or the strips in the manual.
The megacode evaluators will not wait for you to flip pages. Quick rhythm identification (under 5 seconds) is the difference between a smooth scenario and one where the timer runs out while you are still trying to decide if you are looking at PEA or fine V-fib.
ACLS Recertification Day Checklist
- ✓Current ACLS card (or expired card for records, plus your driver's license)
- ✓Photo ID — driver's license or hospital badge with photo
- ✓Current BLS card (prerequisite for ACLS — no card, no class)
- ✓ACLS Provider Manual current edition (digital eBook or paper)
- ✓Printed precourse self-assessment certificate showing 84%+ score
- ✓Comfortable scrubs, gym pants, or athletic clothes for skills check
- ✓Closed-toe shoes (no sandals, flip-flops, or open-back clogs)
- ✓Pen, highlighter, blank paper or printed algorithm cards
- ✓Snacks and water bottle — most classes have a 30 min break
- ✓Reading glasses if you wear them — fine print on rhythm strips
- ✓Phone on silent (you will not need it during megacode)
- ✓$0-$50 cash for parking, manual purchase, or unexpected fees
ACLS Recert by the Numbers
One question comes up often: do you really need to study, or can you wing it on day-of? Plenty of nurses who run codes weekly assume the cardiac arrest algorithm is muscle memory by now. That assumption gets a lot of people stuck on rhythm recognition under pressure.
The megacode is not testing whether you can recognize V-fib on a real patient with a real defibrillator in your hand. It is testing whether you can read a small printed strip, in a simulated bay, while an evaluator stares at you, and call out the correct dose for the correct drug at the correct timing. Those skills atrophy faster than algorithm knowledge.
The other study trap is over-focusing on the cardiac arrest algorithm at the expense of the peri-arrest scenarios. ACS, stroke, post-arrest care, and toxicological arrests all appear on the written exam and rotate through the megacode. The bradycardia and tachycardia algorithms are arguably the highest-yield review topics because they appear in every single megacode rotation.
Practice doses out loud the week before class. Saying "epi 1 milligram" silently in your head is not the same as saying it crisply in front of an evaluator with a stopwatch.
Drill the doses on your drive to work, in the shower, while making dinner. The verbal recall is what gets graded. Bonus tip: record yourself running through a megacode out loud on your phone, then listen back. You will catch hesitations and mumbled doses you would never notice in real time. Most providers tighten their callouts by 30 to 40 percent after one self-review.
If you have access to a colleague who also needs to recertify, run mock megacodes for each other over coffee. Trading turns as team leader and recorder is the closest thing to in-class practice you can get for free. Bring printed rhythm strips, time each scenario to 6 minutes, and grade each other on dose accuracy and reassessment loops. Two 30-minute sessions usually beats two hours of solo study.
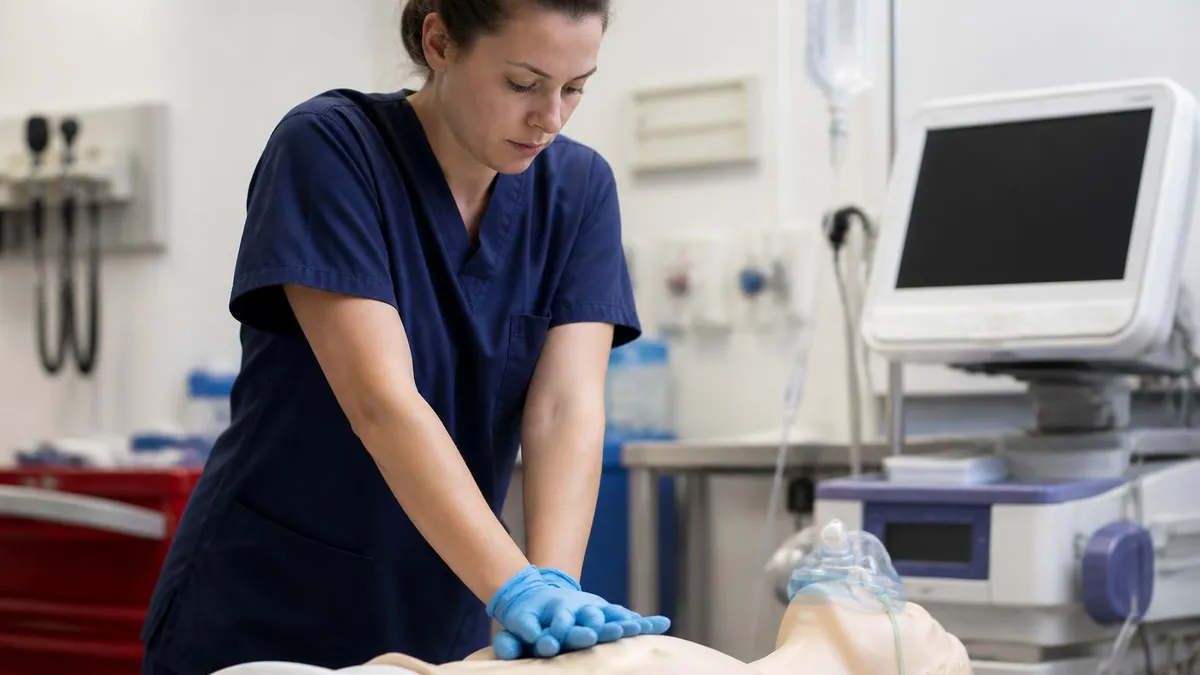
Always say it out loud. The evaluator cannot read your mind. If you call for epi but the team hears "prep epi," they wait. Say "Push epi 1 milligram IV now" — verb, drug, dose, route, timing.
Loop on reassessment. Every 2 minutes you must call for a rhythm check, a pulse check, and a CPR quality check. Build that loop into your verbal pattern from the first scenario in practice.
Designate roles early. Within the first 15 seconds, point at team members and assign compressions, airway, IV access, recorder, and code-cart manager. Evaluators score you on team leadership, not just clinical accuracy.
The megacode is the moment everything snaps into focus. You are placed at the head of a manikin in a small simulated bay.
The instructor reads you a brief scenario — a 67 year old woman with chest pain and a heart rate of 38, for example — and you have 5 to 10 minutes to lead the resuscitation as team leader. You delegate compressions, intubation, IV access, monitor placement, drug pushes, and rhythm checks.
You must verbalize your differential, your assessment, your treatment, and your reassessment loop. The instructor injects rhythm changes mid-scenario. Bradycardia deteriorates to a polymorphic V-tach. The monitor flatlines. The patient regains pulses then re-arrests.
You handle each transition by name, dose, and timing. Closed-loop communication is graded: "Push epi 1 milligram IV" — "Epi 1 milligram IV, confirmed and pushed."
Scenarios that come up reliably across megacode rotations include pulseless V-fib (defib, epi, amiodarone), PEA (search for H's and T's), asystole (epi, identify and treat reversible causes), and symptomatic bradycardia (atropine, transcutaneous pacing, dopamine or epi infusion).
Also expect unstable tachycardia (synchronized cardioversion), stable wide-complex tachycardia (amiodarone or procainamide), ACS with STEMI (aspirin, nitro, morphine, cath lab), suspected stroke (FAST, time of last known well, CT, tPA criteria), post-cardiac arrest hypothermia management (targeted temperature 32-36C), and toxicological arrest with specific antidotes.
Review the ACLS bradycardia and tachycardia algorithms the week before. They show up in nearly every megacode rotation, and dose recall on atropine, dopamine, and epi infusions is where confidence either holds or cracks under pressure.
Renew On Time vs Let It Expire
- +Renewal class is 5-6 hours vs 12-14 hours for initial
- +Renewal cost is $150-$250 vs $250-$350 for initial
- +Your AHA eCard stays continuously valid — no gap in privileges
- +On-call list, pay differential, and code-team membership uninterrupted
- +Skills decay is minimized — you are still sharp from last cycle
- +Hospital education department typically covers timely renewal
- −Have to plan 60 days ahead and block a Saturday or evening
- −Cost still applies even when nothing else has changed in your practice
- −Provider manual may need replacing if AHA guidelines updated
- −Precourse self-assessment is an extra 60-90 minute commitment
- −If you let it expire, you lose ACLS privileges instantly — even by 1 day
- −Expired card means initial course required, doubling time and cost
The financial argument for renewing on time is straightforward. The privileges argument is what stings hospital employees.
The moment your AHA eCard expires, hospital credentialing systems flag your file. In many large hospital systems, this triggers an automatic removal from the code-team roster, the rapid-response team, and sometimes the on-call rotation.
Charge nurses get a notification. The staffing coordinator gets a notification. You may find yourself paired with someone covering your scope until you renew.
Some union contracts also tie a small pay differential to active ACLS certification — losing the card means losing $0.50 to $1.50 an hour until you fix it. For a full-time nurse, that is $80 to $250 a month of lost pay just for letting the card lapse.
Retired nurses returning to bedside practice are a special case. If your last ACLS card has been expired for more than 2 years, AHA policy treats you as a brand-new provider.
You must complete the full initial course regardless of how many cycles you renewed before retirement. The same applies to clinicians switching specialties — an outpatient nurse returning to the ICU after 5 years, for example. There is no "reactivation" pathway between the initial course and the current cycle.
Over-reliance on the algorithm cheat sheet during megacode. The pocket cards are a study aid, not a crutch — evaluators expect you to verbalize doses and timings without flipping cards mid-resuscitation.
Forgetting drug doses under pressure. Memorize epi 1mg q3-5min, amiodarone 300mg first dose then 150mg, atropine 1mg q3-5min, adenosine 6mg then 12mg, and the dopamine and epi drip ranges.
Missing rhythm transitions. The instructor will switch the monitor from PEA to V-fib mid-scenario; if you keep treating PEA, you fail the scenario.
Weak team communication. Closed-loop callouts ("Epi 1mg IV push, confirmed?" — "Confirmed, epi 1mg IV push given.") are graded.
Skipping the precourse self-assessment. Showing up without the 84% certificate gets you turned away at sign-in.
Online-only ACLS is not the same as HeartCode ACLS, and the difference matters. Several non-AHA vendors sell "100% online ACLS recertification" for $99 to $149.
You complete an online cognitive portion, take a multiple choice test, and they mail you a card. These programs are not AHA-affiliated and the card they issue is not an AHA eCard.
Most US hospitals, EMS agencies, and state nursing boards require an AHA ACLS card specifically. The issuer must be a recognized AHA Training Center and the card must come through the AHA Atlas system.
Always confirm with your employer's education department before paying for an online-only program. If in doubt, stick with the heart.org Course Finder.
State and territory variations exist but are limited. Most states accept any AHA-recognized ACLS card without additional requirements.
A few state nursing boards (notably some in the Northeast) require CE credits to be submitted separately to the state board, in addition to holding the AHA card. EMS providers should double-check their state EMS office's continuing education rules.
Paramedic ACLS recertification can include additional state-specific requirements like local protocol updates. For nurses, the AHA card is almost always sufficient as long as your employer accepts it and your state license is current.
Tracking your card has been easier since 2017, when AHA rolled out the eCard system. After you pass class, your Instructor enters your name and email into the AHA Atlas portal.
You receive an email link and create a free account to download your card. The eCard contains a unique QR code that employers can scan to verify authenticity — no more wallet-card forgery worries, and no more lost paper cards.
Take screenshots, save the PDF to cloud storage, and forward a copy to your HR or credentialing office. The eCard is recognized everywhere a paper card was accepted, and most hospital systems now require the eCard URL during credentialing rather than a photocopy.
If you trained before 2017 and still have a paper card on file with your employer, you do not need to retroactively convert. Your current card is valid until its expiration date.
But your next renewal will issue as an eCard regardless of pathway — in-person renewal, HeartCode, or RQI. Many providers keep both: the printable PDF for personal records and the verified link for employer verification.
The Atlas portal also stores your renewal history, which is handy for tracking when your next 2-year cycle expires. Set a calendar reminder the day you receive the new eCard — block out a Saturday 24 months out and your future self will thank you.
ACLS Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.