AHA ACLS: American Heart Association Advanced Cardiovascular Life Support Guide
Complete AHA ACLS guide: certification process, course content, exam preparation, and renewal requirements for healthcare providers.
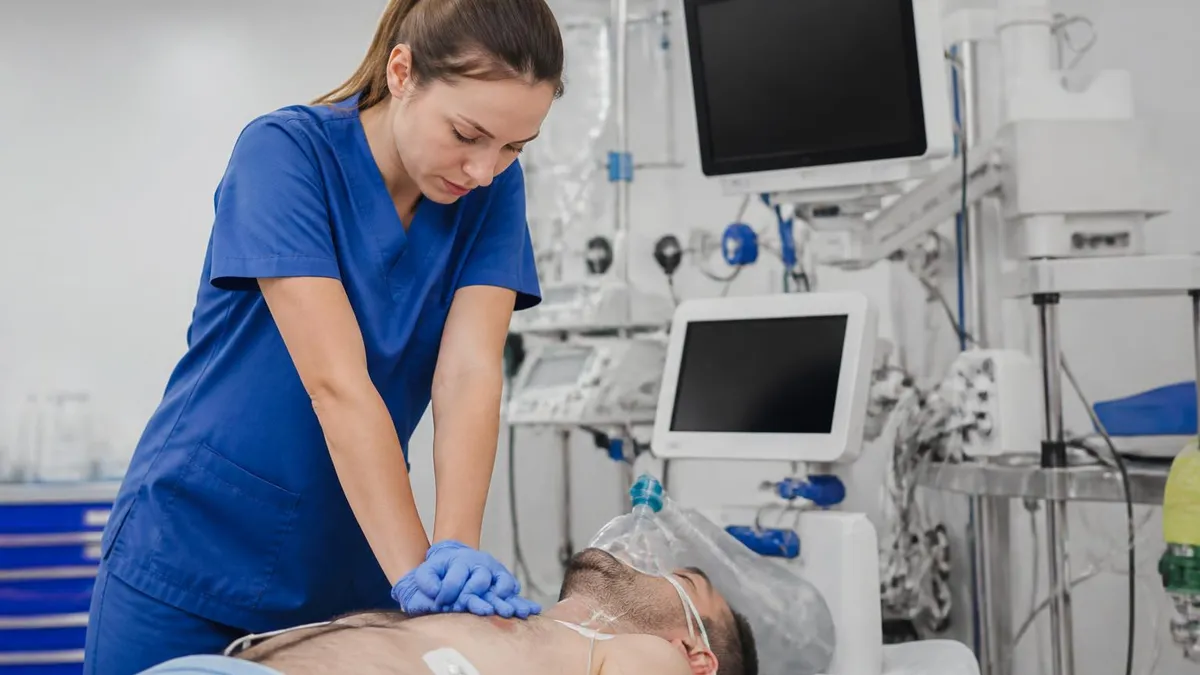
AHA ACLS — American Heart Association Advanced Cardiovascular Life Support — is the gold standard certification for healthcare providers responding to cardiovascular emergencies. Whether you're a nurse, physician, paramedic, respiratory therapist, or other healthcare professional whose work involves emergency response, ACLS certification provides the knowledge and skills to manage cardiac arrest, post-cardiac arrest care, acute coronary syndrome, stroke, and bradyarrhythmia/tachyarrhythmia situations. The certification is widely required across hospital and pre-hospital settings, making it one of the most important credentials for emergency-capable healthcare workers.
The American Heart Association (AHA) publishes the ACLS algorithms and guidelines that are revised every 5 years based on updated resuscitation science. The most recent comprehensive guidelines were released in 2020 with subsequent annual updates incorporating new research findings. ACLS algorithms cover cardiac arrest (VF/pulseless VT, PEA, asystole), bradycardia, stable and unstable tachycardia, post-cardiac arrest care, acute coronary syndromes, suspected stroke, and special situations like cardiac arrest in pregnancy or due to specific reversible causes.
ACLS courses combine online learning, hands-on skills practice, and exam testing to certify providers. Most candidates complete the AHA-developed Provider Course, typically a 1-2 day classroom course (or hybrid blended-learning format with online portion completed before in-person practice). The course teaches algorithm application through simulated megacode scenarios — providers respond to mock cardiac emergencies as they would in actual clinical practice. Successful completion includes both a written exam and demonstration of competence in megacode scenarios.
This guide covers AHA ACLS comprehensively: certification requirements, course content, study strategies, megacode preparation, exam tips, and renewal expectations. Whether you're pursuing initial ACLS certification or renewing existing credentials, you'll find practical information to support your preparation and success.
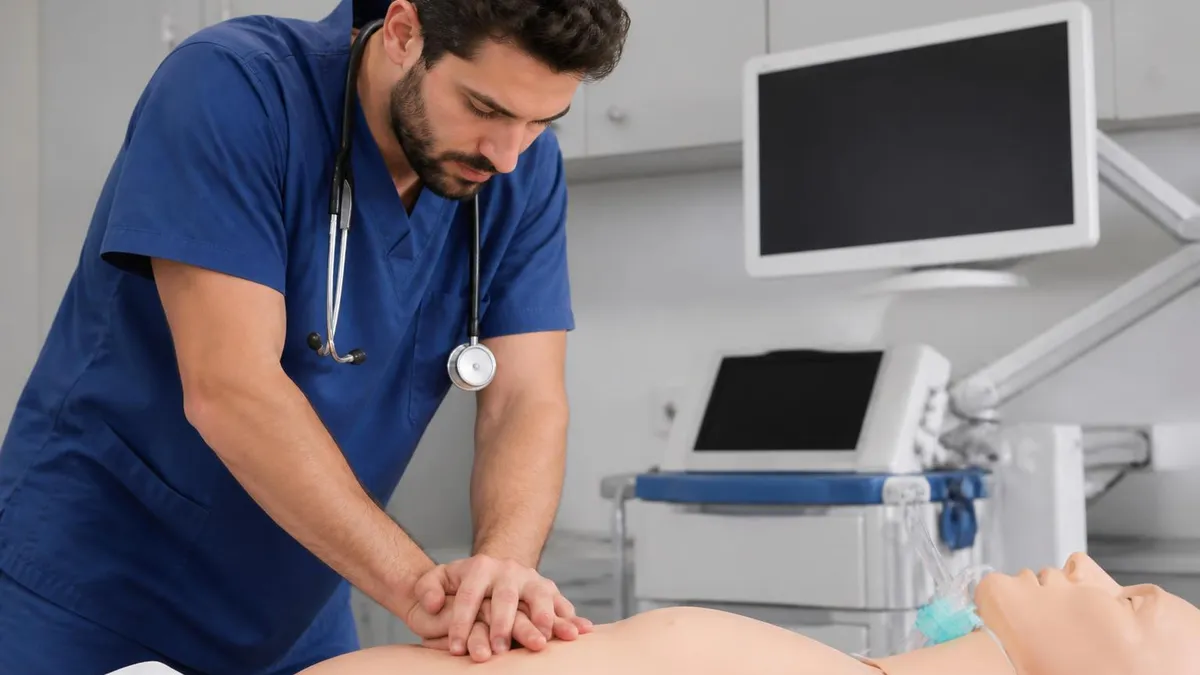
The role of CPR quality is heavily emphasized in current ACLS guidelines. High-quality CPR — adequate compression depth (2-2.4 inches in adults), rate (100-120 per minute), full chest recoil between compressions, minimizing interruptions — improves resuscitation outcomes substantially. ACLS providers learn to monitor and improve CPR quality during resuscitations through metrics, feedback devices, and effective team communication. The team leader's role includes ensuring continuous high-quality CPR throughout the code, switching compressors regularly to prevent fatigue.
Issuing organization: American Heart Association
Course format: Provider Course (initial); Renewal Course (every 2 years for current providers)
Length: 1-2 days for full course; renewal often shorter
Components: Online or classroom didactic, hands-on skills, megacode simulations, written exam
Validity: 2 years from completion date
The ACLS Provider Course covers all major cardiovascular emergency scenarios. Cardiac arrest management is central — recognizing and managing ventricular fibrillation/pulseless ventricular tachycardia (VF/pVT) with defibrillation and CPR, pulseless electrical activity (PEA) and asystole with CPR and reversible cause identification, and post-cardiac arrest care emphasizing organ-protective measures. Each algorithm has specific medication doses, timing intervals, and decision points that providers must recall and apply during simulated and actual scenarios.
Bradycardia and tachycardia algorithms address rhythm disturbances that may or may not progress to cardiac arrest. Symptomatic bradycardia management involves atropine, transcutaneous pacing, and dopamine or epinephrine infusions. Stable tachycardia management uses adenosine, beta-blockers, or calcium channel blockers depending on rhythm type. Unstable tachycardia requires synchronized cardioversion. Each algorithm has decision trees that providers learn to apply systematically based on patient assessment findings. The ACLS algorithm resources cover these specific algorithms in detail.
Acute coronary syndrome (ACS) management focuses on rapid assessment, ECG interpretation, and time-sensitive treatment decisions. Identifying STEMI (ST-elevation myocardial infarction) versus other coronary syndromes drives different treatment approaches — STEMI requires emergent reperfusion via primary PCI or fibrinolysis. Time targets matter critically: door-to-balloon time goals of 90 minutes for primary PCI; door-to-needle time of 30 minutes for fibrinolysis. ACLS providers participate in the systems that meet these targets through prompt recognition, communication, and appropriate immediate care.
Stroke management emphasizes rapid recognition, prompt activation of stroke protocols, and time-sensitive interventions. Eligibility for IV thrombolytics (tPA) depends on time from symptom onset, eligibility criteria including absence of contraindications. Mechanical thrombectomy for large vessel occlusion has expanded treatment windows in recent years. ACLS providers contribute to the chain of recognition, transport, and immediate care that enables these time-sensitive treatments. The ACLS certification programs build the broader cardiovascular emergency competence around these specific scenarios.
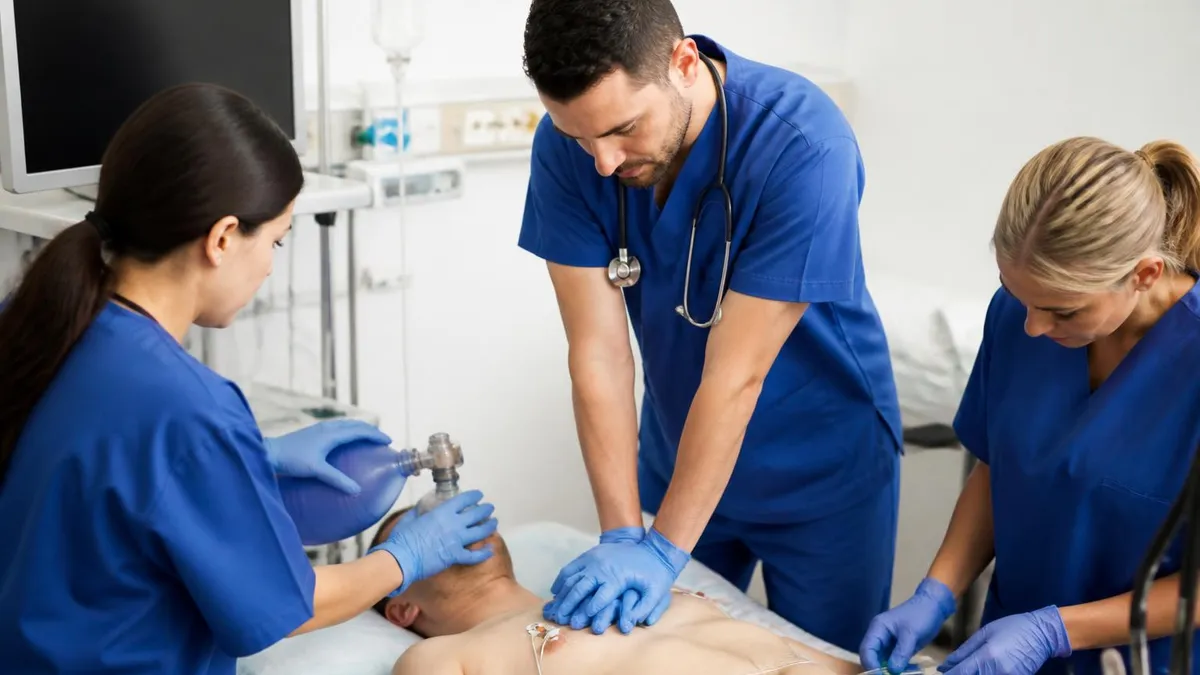
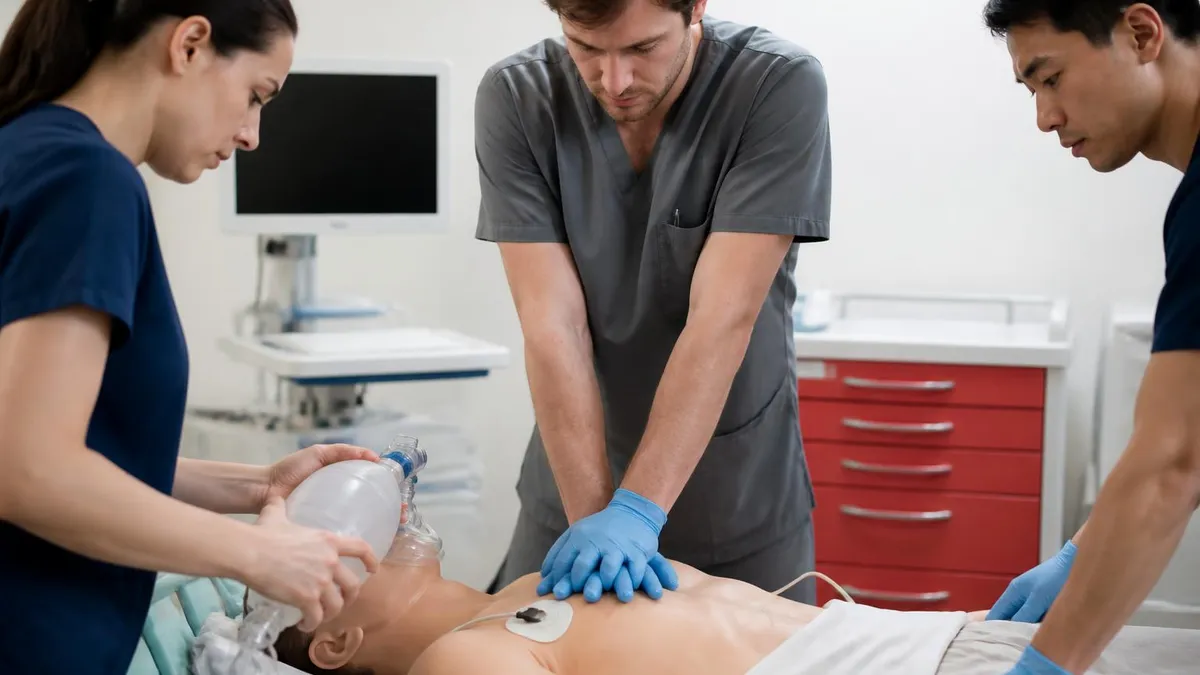
Megacode scenarios test integrated application of all algorithms in realistic simulations. Candidates lead a team responding to a complex evolving scenario — perhaps starting with an unstable patient that arrests, requires multiple algorithm applications during resuscitation, and continues into post-arrest care. Skills tested include team leadership, clear closed-loop communication, accurate algorithm application, appropriate medication administration, and effective team dynamics. The megacode is often the most stressful part of the course but also where the most learning happens through pressure-tested application of integrated knowledge.
Defibrillation timing matters greatly. For shockable rhythms (VF/pVT), early defibrillation is the single most effective intervention — survival decreases approximately 7-10% per minute of delay. Public access defibrillation through AEDs in many community locations enables defibrillation before EMS arrival. In hospital settings, immediate defibrillation when shockable rhythms are identified is the priority. ACLS providers practice rapid recognition, charge timing, and safe defibrillation that doesn't delay subsequent compressions during the resuscitation.
Major ACLS Algorithm Categories
Adult cardiac arrest algorithm with branches for shockable (VF/pVT) and non-shockable (PEA, asystole) rhythms. CPR, defibrillation, epinephrine, antiarrhythmics, reversible cause assessment (Hs and Ts). Most heavily tested area in ACLS courses and exams. Foundation for all other ACLS scenarios.
Algorithm for symptomatic bradycardia: atropine 1 mg IV, transcutaneous pacing, dopamine or epinephrine infusion. Decision points based on symptoms, hemodynamic stability, and response to interventions. Important to distinguish symptomatic from asymptomatic bradycardia — only the former needs intervention.
Stable tachycardia management with adenosine for SVT, beta-blockers/CCB for stable AF/atrial flutter. Unstable tachycardia management with synchronized cardioversion. Wide-complex versus narrow-complex tachycardias have different management approaches based on stability and rhythm characteristics.
Care after return of spontaneous circulation (ROSC): targeted temperature management, hemodynamic optimization, ventilation strategy, treatment of reversible causes. Critical phase for neurological outcome — proper post-arrest care substantially affects whether resuscitated patients survive with good function.
Effective ACLS preparation typically requires 20-40 hours of study before the course, depending on your starting familiarity. Healthcare providers with frequent cardiac code experience may need only review; those returning to ACLS after time away from clinical practice may need substantial preparation. Pre-course preparation includes reading the AHA Provider Manual, taking practice tests, and reviewing common algorithm details until they're committed to memory.
The AHA-published Provider Manual is the authoritative reference. Read it cover-to-cover at least once before your course. The manual covers all algorithms, drug pharmacology, ECG rhythm recognition, and integrated case scenarios. Annotating the manual with your own notes helps retention. The manual is structured around the algorithms, making it useful as both initial study material and ongoing reference.
The AHA ACLS Precourse Self-Assessment is required completion before attending the course. The assessment tests baseline ECG and pharmacology knowledge through online questions. Failing the precourse means the in-class course won't be productive — you need to address the knowledge gaps first. Most candidates pass the precourse without difficulty, but completing it conscientiously helps identify weak areas to target during in-course preparation. The ACLS precourse self-assessment answers resources help candidates work through this preparation effectively.
Practice tests for ACLS exams are essential study tools. Multiple commercial sources provide ACLS practice tests at varying quality levels. The ACLS practice test resources from quality sources help identify content areas needing more study. Take practice tests under timed conditions to build pacing similar to the actual exam. Review every missed question to understand both the correct answer and why other options are incorrect. Repeated practice testing produces better results than passive content review.
Megacode preparation deserves dedicated attention because it's where many candidates feel most stressed. Visualize the algorithm steps. Practice closed-loop communication: when calling for medications, specify dose, route, and request confirmation when given. Practice team leadership without being authoritarian — clear communication and quick decisions matter. Some candidates find practicing megacode scenarios with study partners helpful — taking turns leading and observing. Several megacode practice videos are available on YouTube showing both ideal and suboptimal approaches.
Capnography monitoring during cardiac arrest provides real-time information about CPR quality and resuscitation progress. End-tidal CO2 (ETCO2) values reflect both ventilation and pulmonary blood flow. Sustained ETCO2 below 10 mmHg suggests inadequate CPR or futile resuscitation; values above 10 mmHg with rising trend suggest ROSC may be imminent. ACLS guidelines incorporate capnography as a key adjunct to traditional rhythm and pulse-based resuscitation monitoring, providing objective real-time feedback that improves resuscitation decisions.
ACLS Course Components
Required completion before attending the course:
- AHA ACLS Precourse Self-Assessment: online assessment of baseline ECG and pharmacology knowledge
- Provider Manual reading: 200+ page comprehensive reference
- Algorithm memorization: cardiac arrest, bradycardia, tachycardia, post-arrest care
- Drug pharmacology review: doses, indications, contraindications, side effects
- Practice tests: identify and address knowledge gaps before course
ACLS certification is valid for 2 years from completion date. Renewal courses are shorter than initial courses (typically 1 day or less) since renewal candidates are presumed to have foundational knowledge from the initial certification. Renewal courses focus on algorithm updates, refreshing skills, and confirming continued competence through megacode and written exam. The 2-year cycle ensures providers stay current with periodic updates to algorithms and best practices.
For healthcare providers whose ACLS expired more than the renewal grace period (typically 30 days), full re-certification through the Provider Course is required. Letting certification lapse beyond the grace period creates more work and cost than timely renewal. Setting calendar reminders 6 months before expiration provides adequate time to schedule renewal during convenient periods. Many employers provide ACLS courses on-site or cover course fees as part of professional development; checking with your employer's nursing education department or equivalent identifies these resources.
Cost of ACLS courses varies. Initial Provider Course typically runs $200-$300 at training centers and online providers. Renewal Course is typically $150-$250. AHA-affiliated training centers and approved blended learning providers offer the official AHA ACLS course; check the AHA's training center locator for options near you. Some online providers offer ACLS training that may not be AHA-issued — verify the certificate type before purchasing if your employer requires AHA-specific certification.
For candidates who fail the course, most training centers allow remediation through additional practice sessions and re-attempts at the megacode and written exam. The specific policies vary by training center; some allow retest within a few weeks while others require waiting longer or paying additional fees for retests. Don't be discouraged by needing remediation — many competent providers fail their first ACLS attempt and pass on retake with focused additional preparation. The ACLS training programs resources cover course options and what to expect from various providers.
Beyond ACLS, related certifications complement comprehensive emergency response capability. BLS (Basic Life Support) is the foundation course covering basic CPR and AED use — required prerequisite for ACLS at most centers. PALS (Pediatric Advanced Life Support) covers pediatric resuscitation. NRP (Neonatal Resuscitation Program) covers newborn resuscitation. Each addresses specific patient populations or care contexts. Healthcare providers in roles requiring multiple certifications often complete them sequentially, starting with BLS and adding ACLS plus pediatric or neonatal certifications based on their practice area.
Some online ACLS courses issue certificates that aren't from the American Heart Association — these may not satisfy hospital or employer requirements that specify AHA ACLS. Before purchasing any ACLS course, verify it's an AHA-authorized course issuing AHA cards. The AHA training center locator at heart.org lists authorized training providers. Non-AHA courses can be cheaper and more convenient but may not be accepted by employers, requiring you to retake an AHA course at additional cost. Save money in the long run by getting AHA-issued certification from the start.
Career relevance of ACLS varies by role. ICU nurses, emergency department staff, anesthesia providers, cath lab personnel, and rapid response team members typically need ACLS as a job requirement. Med-surg nurses, primary care providers, and ambulatory care nurses may or may not need ACLS depending on employer requirements. Knowing whether your specific role requires ACLS — and verifying with your employer — ensures you maintain appropriate certifications without unnecessary effort or expense.
For students entering nursing or other healthcare careers, ACLS is typically pursued after graduating and securing employment that requires it. Some nursing programs include ACLS during clinical training; others don't. Healthcare employers often provide initial ACLS certification as part of new-hire training or shortly thereafter. Pursuing ACLS independently before employment can be valuable for some career paths but isn't strictly necessary for entry-level positions in most cases. Discussing ACLS expectations with prospective employers during job searches clarifies what's needed when.
For working healthcare providers, maintaining current ACLS demonstrates professional commitment to emergency response capability. Even providers in roles where cardiac emergencies are rare benefit from periodic ACLS renewal because emergencies do occasionally arise unexpectedly. The structured review during renewal courses keeps skills sharp despite limited daily application. Building habits of consistent ACLS renewal throughout your career produces sustained competence that you may rely on when needed.
The relationship between ACLS knowledge and actual cardiac emergency response involves practical considerations beyond just knowing algorithms. Real codes are chaotic — managing teams of various experience levels, working with limited information, making decisions with incomplete data, and dealing with the emotional intensity of life-threatening emergencies. Course training provides foundation; clinical experience builds the practical skills that turn algorithm knowledge into effective emergency leadership. Both elements contribute to the comprehensive capability that ACLS certification represents.
Looking forward, ACLS algorithms continue evolving as resuscitation science advances. The 5-year cycle of major updates incorporates research on chest compression depth and rate, ventilation strategies, medication efficacy, post-cardiac arrest care, and various other topics. Annual focused updates address specific findings between major cycles. Staying engaged with current best practices through your organization's resuscitation committees, professional society publications, and continuing education maintains practical knowledge that may exceed what's covered in periodic ACLS courses alone.
For nurses pursuing ACLS, the certification often unlocks opportunities for higher-acuity positions including critical care, emergency department, post-anesthesia care, and other specialty units. Combining ACLS with PALS (Pediatric Advanced Life Support) is common for pediatric ICU nurses and emergency department nurses who care for both adults and children. Some certifications like CCRN (Critical Care Registered Nurse) build on ACLS foundation alongside specialized critical care knowledge for further professional advancement.
For physicians, ACLS is part of broader emergency response capability that physicians develop through residency training. Most physicians complete ACLS during residency or shortly thereafter; many maintain certification throughout their careers as part of professional credentialing requirements at hospitals where they practice. Subspecialty physicians (cardiology, emergency medicine, anesthesiology, intensive care) build advanced expertise beyond ACLS but use ACLS framework as foundational vocabulary for emergency response.
For paramedics and other prehospital providers, ACLS skills apply directly to field cardiac emergencies. The complexity of pre-hospital settings — limited resources, varied environments, complex patient situations — adds challenges that hospital-based ACLS scenarios don't typically include. Paramedic education includes ACLS-equivalent content as part of their broader scope of practice. Maintaining ACLS certification in addition to paramedic licensing demonstrates ongoing commitment to evidence-based emergency response.
AHA ACLS Quick Facts
ACLS Course Format Choices
- +Traditional classroom: full instructor-led training, hands-on practice, supportive learning environment
- +Blended learning: online portion at your own pace plus in-person skills/megacode
- +Renewal courses: shorter than initial certification for current providers
- +Multiple training centers: choose convenient location and schedule
- +Most healthcare employers cover course costs as professional development
- −Course intensity: 1-2 days of focused training can be exhausting
- −Megacode pressure: simulating emergencies under observation creates stress for many candidates
- −Cost without employer coverage: $200-$300 for initial certification
- −Time commitment: pre-course preparation plus course attendance plus exam
- −Updates between renewals: keeping current with algorithm changes between certification cycles
ACLS Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.