ACLS Practice Test PDF 2026: Free Advanced Cardiovascular Life Support Questions
Download free ACLS practice test PDF 2026. Study AHA exam questions, algorithms, drug dosing, and rhythms. Pass with 84%+ on your first attempt.
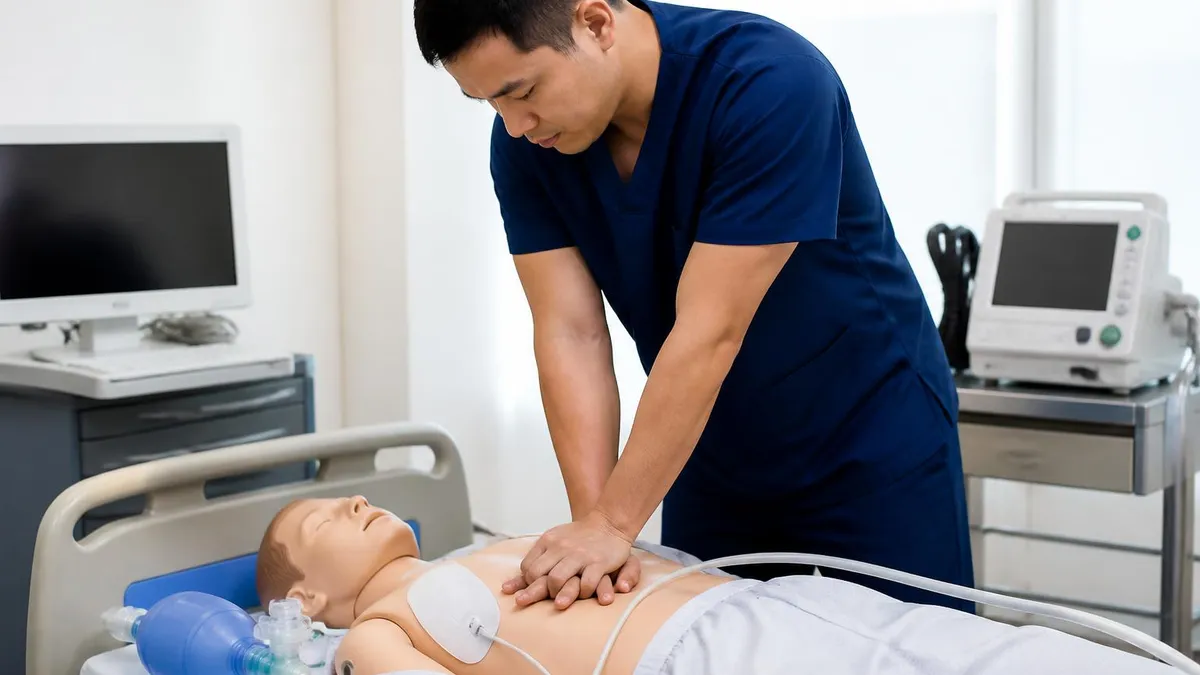
If you're preparing for ACLS certification, you already know the stakes are high. The American Heart Association's Advanced Cardiovascular Life Support course tests your ability to manage life-threatening emergencies — cardiac arrest, stroke, acute coronary syndrome, and dangerous arrhythmias. Downloading an ACLS practice test PDF lets you study anywhere, drill rhythms without an internet connection, and build the pattern recognition you need before exam day.
This page walks you through everything: what the ACLS written exam actually covers, the format you'll face, passing score requirements, key algorithms, and drug dosing you must know cold. Use the free PDF below as your offline reference.
What the ACLS Exam Tests
ACLS certification has two components. The written (cognitive) exam and the megacode skill station. Both matter, but the written test is where most candidates stumble — not because the content is obscure, but because exam questions assume fast, confident recall under pressure.
The written test covers:
- Rhythm recognition — VF, pVT, asystole, PEA, sinus bradycardia, SVT, wide-complex tachycardia, atrial fibrillation, heart blocks
- BLS integration — high-quality CPR, compression-to-ventilation ratios, minimizing interruptions
- ACLS algorithms — the exact decision trees the AHA wants you to follow for each emergency
- Pharmacology — drugs, doses, routes, timing, and contraindications
- Post-cardiac arrest care — targeted temperature management, hemodynamic optimization
- Team dynamics — closed-loop communication, defined roles, mutual respect in a resuscitation team
The megacode skill station tests your ability to lead or participate in a simulated resuscitation. You'll be evaluated on rhythm recognition, correct algorithm application, drug choices, and communication. Both sections must be passed to earn certification.
Exam Format and Passing Score
The AHA written exam consists of 50 multiple-choice questions. You need to score 84% or higher — that's 42 out of 50 correct — to pass. Questions are scenario-based: you're given a clinical situation, a rhythm strip or 12-lead ECG, and asked what to do next.
Time pressure is real. You have roughly 60 minutes. That's just over a minute per question. If you hesitate on rhythms or second-guess drug doses, the clock works against you. This is why offline practice with a PDF matters. You can pause, annotate, and review at your own pace — something a timed online simulator doesn't allow.
Initial ACLS certification is valid for two years. After that, you renew through an ACLS recertification course, which is shorter but still requires passing the written and megacode components.
Who Needs ACLS Certification
ACLS is required or strongly recommended for a wide range of healthcare professionals:
- Registered nurses working in ICU, ED, step-down, or telemetry units
- Paramedics and advanced EMTs
- Physicians in emergency medicine, internal medicine, anesthesiology, and surgery
- Respiratory therapists involved in airway management
- Nurse practitioners and physician assistants in acute care settings
- Flight nurses and transport team members
- Surgical technologists assisting in procedures with cardiac risk
Some employers require ACLS before your first shift. Others give you 90 days to obtain it after hire. Either way, you don't want to show up unprepared. The written test is passable on the first attempt if you've studied the right material — and a thorough practice PDF is the most efficient tool for that.
Key ACLS Algorithms You Must Know
The AHA publishes specific algorithms for each emergency scenario. These aren't optional suggestions — they're the framework examiners use to evaluate your responses. Know these five cold before your exam.
Cardiac Arrest Algorithm (VF/pVT and Non-Shockable)
Confirm cardiac arrest. Start high-quality CPR immediately. Attach the defibrillator. For VF or pulseless VT: deliver a shock, resume CPR for 2 minutes, check rhythm. Give epinephrine 1 mg IV/IO every 3–5 minutes. After the second shock, consider amiodarone (300 mg IV, then 150 mg). For PEA and asystole: CPR plus epinephrine, treat reversible causes (the Hs and Ts). Don't stop for rhythm checks more often than every 2 minutes.
Bradycardia Algorithm
Identify unstable signs: hypotension, altered mental status, ischemic chest pain, acute heart failure. If unstable, give atropine 0.5 mg IV (up to 3 mg total). If atropine fails or bradycardia is high-degree block, use transcutaneous pacing. Dopamine and epinephrine infusions are second-line options while preparing for pacing or transvenous pacing consult.
Tachycardia Algorithm
If the patient is unstable (hypotension, acute chest pain, signs of shock, decreased consciousness), go straight to synchronized cardioversion. If stable, determine if the QRS is narrow or wide. Narrow QRS with regular rhythm: try vagal maneuvers first, then adenosine 6 mg IV rapid push (can repeat with 12 mg). Wide QRS regular rhythm: adenosine if you suspect SVT with aberrancy; otherwise amiodarone infusion.
Acute Coronary Syndrome Algorithm
MONA isn't a mnemonic anymore — the AHA removed routine oxygen, and morphine use is now cautious. Start with aspirin 325 mg chewed, obtain 12-lead ECG within 10 minutes, assess for STEMI vs. NSTEMI/UA. STEMI: activate the cath lab immediately, target door-to-balloon time under 90 minutes. Antiplatelet therapy, anticoagulation, and early PCI are cornerstones.
Stroke Algorithm
Cincinnati Prehospital Stroke Scale: facial droop, arm drift, abnormal speech. Time is brain — call a stroke alert, get non-contrast CT within 25 minutes of arrival. If ischemic stroke and within 3–4.5 hours of symptom onset (and no contraindications): tPA 0.9 mg/kg IV. Monitor BP closely; avoid aggressive hypertension correction unless >220/120 in non-tPA candidates.
Drug Dosing Reference
ACLS pharmacology questions are some of the most specific on the exam. These are the doses you'll be tested on most frequently:
- Epinephrine — 1 mg IV/IO every 3–5 minutes during cardiac arrest (no upper limit per current guidelines, but give it early)
- Amiodarone — 300 mg IV/IO first dose for VF/pVT; 150 mg IV/IO second dose. Infusion: 150 mg over 10 min for stable VT, then 1 mg/min for 6 hours.
- Atropine — 0.5 mg IV for bradycardia; maximum cumulative dose 3 mg. Doses under 0.5 mg can paradoxically worsen bradycardia.
- Adenosine — 6 mg rapid IV push for SVT; flush immediately with saline. Second dose 12 mg if no conversion. Give as close to the IV site as possible.
- Lidocaine — 1–1.5 mg/kg IV for VF/pVT as an alternative to amiodarone. Maintenance infusion: 1–4 mg/min.
- Dopamine infusion — 2–20 mcg/kg/min for bradycardia unresponsive to atropine or symptomatic hypotension.
- Norepinephrine — 0.1–0.5 mcg/kg/min for post-arrest hypotension with adequate fluid resuscitation.
A PDF study guide lets you tab to this drug table during an offline session and quiz yourself without toggling between browser tabs. Many candidates print it and annotate the margins — underlining the gotchas like the atropine minimum dose and amiodarone first vs. second dose amounts.
Why Use an ACLS Practice Test PDF
Online simulators have their place. But a PDF does things a website can't. You can study during a shift break without relying on hospital Wi-Fi. You can print it and take notes directly on the page. You can share it with a study group without everyone needing account logins.
More importantly, rhythm recognition improves with repetition away from distractions. Sitting with a printed strip and making yourself name the rhythm and state the treatment — without clicking a hint button — builds the fast-twitch recall the megacode demands.
For complete ACLS study resources, algorithm diagrams, and practice quizzes sorted by topic, visit the ACLS Advanced Cardiovascular Life Support masterpage. It covers certification pathways, course options, and topic-specific practice sets for every algorithm category.
Renewing Your ACLS Certification
ACLS expires every two years. The renewal course assumes you already know the foundations — it focuses on updates to the guidelines, difficult airway scenarios, and high-performance team dynamics. You still take a written exam and complete a megacode, but the course is shorter than initial certification.
Don't wait until the last minute to renew. Many hospitals flag providers whose ACLS expires mid-year, which can affect scheduling and credentialing. Set a calendar reminder 3 months before expiration and use the PDF to do a quick refresher — algorithms change between AHA guideline cycles (most recently 2020, with the next major update expected around 2025–2026).
ACLS Written Exam Fast Facts
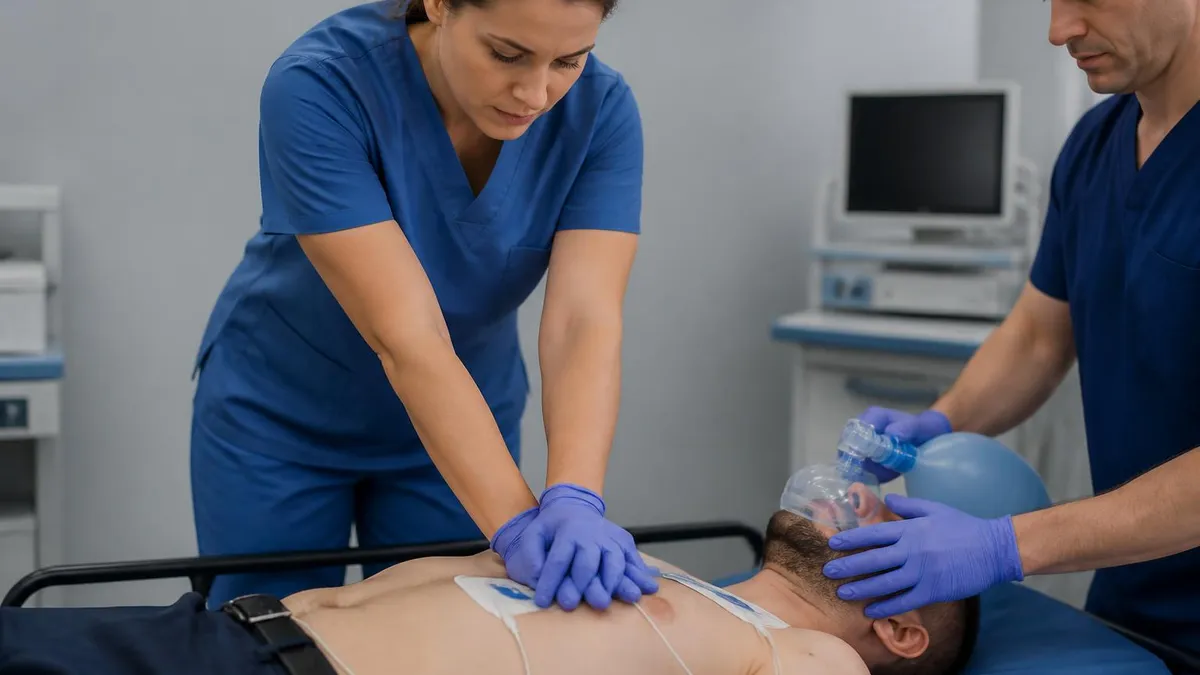
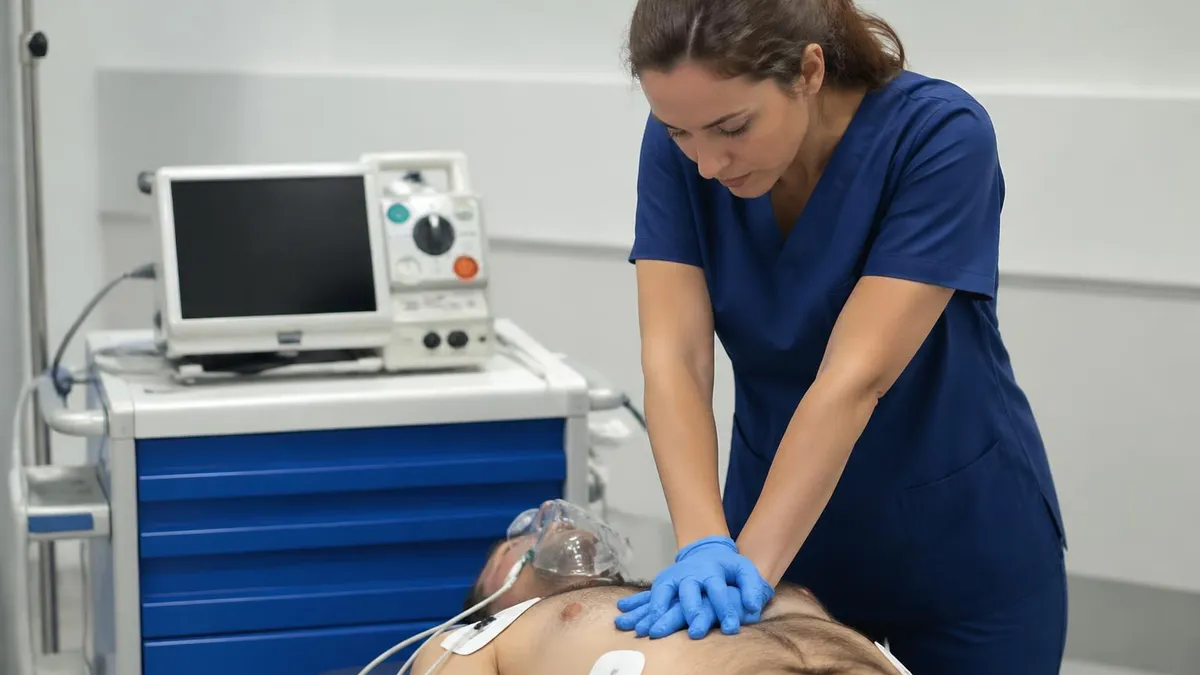
Common Exam Mistakes to Avoid
How to Use the ACLS PDF Effectively
Don't just read it once and feel ready. Here's a study method that works:
Pass 1 — Read through: Go through all questions without stopping. Mark anything you're unsure about.
Pass 2 — Algorithm focus: For every question you missed, trace it back to the correct algorithm. Don't memorize the answer — understand the decision point.
Pass 3 — Timed drill: Set a timer. Give yourself 60 seconds per question. This simulates exam pressure and exposes gaps in recall speed.
The day before your exam, review the drug dosing table one more time. Exam questions often hinge on a single number — the 0.5 mg atropine minimum, the 300 mg amiodarone first dose, the 84% passing threshold itself. A quick final pass over the PDF the night before locks in those details.
Ready to Test Your Knowledge?