Therapeutic Phlebotomy: What It Is, Conditions Treated & Process
Learn what therapeutic phlebotomy is, which conditions it treats (hemochromatosis, polycythemia), the procedure, and how often it's needed.
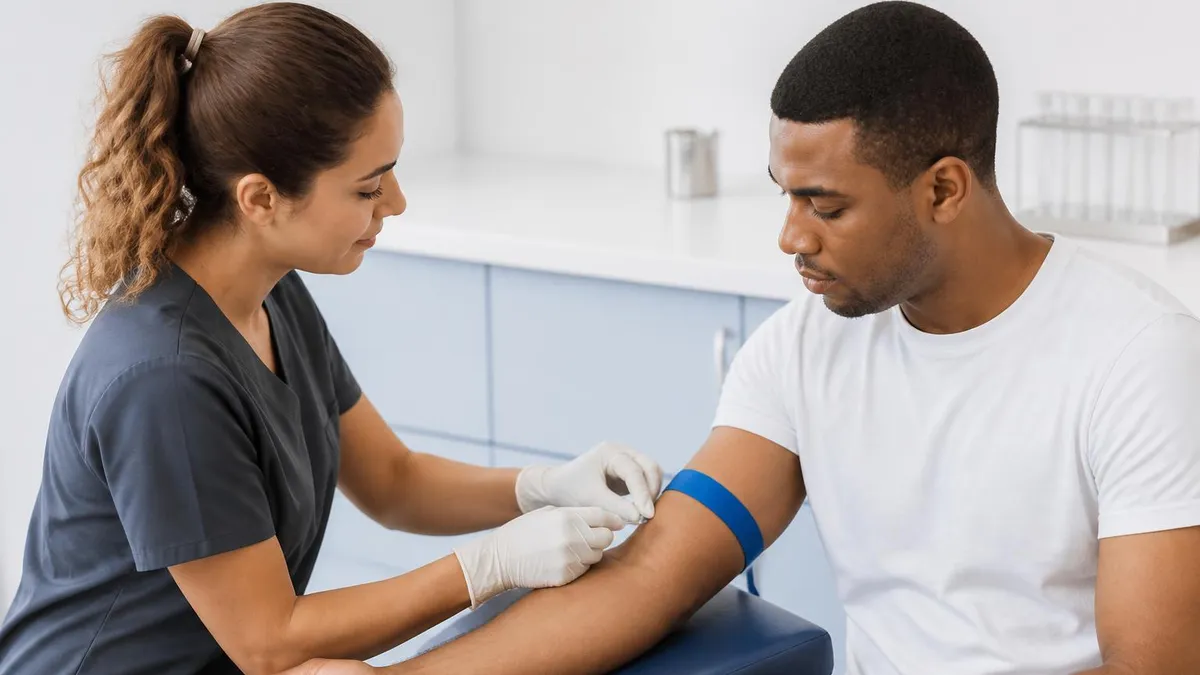
Therapeutic phlebotomy is a medical procedure that removes blood from a patient as a treatment, not just as a diagnostic sample. Unlike a routine blood draw for testing — which collects a small amount in a tube — therapeutic phlebotomy removes a larger volume (typically 350 to 500 mL, similar to a blood donation) to reduce iron overload, lower red blood cell counts, or treat specific medical conditions.
The procedure has been used in some form for thousands of years, but modern therapeutic phlebotomy is a precise, evidence-based treatment for specific diagnosed conditions rather than the indiscriminate "bloodletting" of historical medicine.
Two conditions account for most therapeutic phlebotomy treatments today: hereditary hemochromatosis and polycythemia vera. Hemochromatosis is a genetic disorder where the body absorbs and stores too much iron, leading to iron deposits in the liver, heart, pancreas, and other organs. Polycythemia vera is a blood cancer that produces too many red blood cells, increasing blood thickness and clot risk. Both conditions are managed long-term through scheduled phlebotomy sessions that maintain safe blood and iron levels — typically continuing throughout the patient's life with adjusted frequency based on response.
The procedure itself resembles blood donation in many ways. A trained phlebotomist or nurse inserts a large-bore needle into a vein (usually in the inner elbow), allows blood to flow into a collection bag, and removes a measured volume over 15 to 30 minutes. Saline is sometimes infused during or after to maintain blood volume. The patient is monitored for lightheadedness or other adverse reactions throughout. Most patients tolerate sessions well, though the first few sessions may cause mild fatigue while the body adjusts to the change.
This guide covers therapeutic phlebotomy in detail: the conditions it treats, how the procedure works, what to expect during and after sessions, scheduling considerations, comparison to blood donation, and the role of phlebotomists and nurses in administering the treatment. Whether you've recently been diagnosed with a condition requiring phlebotomy or you're a healthcare professional learning the procedure, you'll find clear practical information here.
The terminology around therapeutic phlebotomy can be confusing because the same procedure is sometimes called "venesection," "bloodletting," or simply "phlebotomy" depending on regional medical practice and the era of the source you're reading. Modern medical literature has largely standardized on "therapeutic phlebotomy," but you may encounter the older terms in patient communications, especially when family members or older clinicians use phrases that have stuck from earlier decades. They all refer to the same evidence-based procedure when used in current clinical contexts.
What it is: Removing 350-500 mL blood as treatment for specific conditions
Common conditions: Hereditary hemochromatosis, polycythemia vera, porphyria cutanea tarda
Frequency: Initially weekly to bi-weekly; maintenance every 2-4 months once stable
Session length: 30-60 minutes including check-in, draw, and recovery
Long-term: Usually a lifelong treatment with periodic adjustments based on lab results
Hereditary hemochromatosis affects about 1 in 200 people of Northern European descent, making it one of the most common genetic disorders. The condition causes excessive intestinal iron absorption, leading to iron levels that gradually accumulate in tissues over decades. Without treatment, this iron overload damages the liver (cirrhosis, liver cancer), heart (cardiomyopathy, arrhythmias), pancreas (diabetes), joints (arthritis), and skin (bronzing). Therapeutic phlebotomy is the standard treatment because removing blood directly removes iron — each unit (about 500 mL) of blood contains roughly 200-250 mg of iron.
Diagnosis typically happens through blood testing showing elevated ferritin (iron stores) and transferrin saturation. Genetic testing confirms the responsible gene mutations, most commonly in the HFE gene (C282Y and H63D variants). Once diagnosed, patients begin a phlebotomy regimen with two phases: an aggressive depletion phase to bring ferritin levels into the normal range, then a maintenance phase to keep them there. The depletion phase often involves weekly or bi-weekly sessions for several months; maintenance typically requires sessions every 2 to 4 months indefinitely.
Polycythemia vera is a different beast. It's a chronic myeloproliferative neoplasm — a type of blood cancer where bone marrow produces too many red blood cells, often along with elevated white cells and platelets. The thickened blood increases stroke and clot risk significantly. Therapeutic phlebotomy reduces hematocrit (the percentage of blood made up of red cells), bringing it into safer ranges. Treatment goals typically aim for hematocrit below 45% in men and below 42% in women. The procedure is often combined with low-dose aspirin and sometimes additional medications like hydroxyurea for higher-risk patients.
Porphyria cutanea tarda (PCT) is a less common indication. PCT involves disrupted heme synthesis combined with iron-related liver dysfunction. Phlebotomy reduces iron stores, which improves the underlying enzyme function and reduces skin manifestations. The phlebotomy schedule for PCT is similar to early-phase hemochromatosis treatment — weekly or bi-weekly sessions until ferritin reaches a target range, then less frequent maintenance.
Specialized phlebotomists trained in phlebotomy and therapeutic procedures perform most of these treatments at hospital outpatient centers, blood donation facilities, hematology clinics, and some primary care offices that handle hemochromatosis management. Training for therapeutic phlebotomy goes beyond standard phlebotomy training to include specific protocols for adverse reaction management, large-volume draw techniques, and patient monitoring during longer sessions.
Family screening is an important consideration when one family member is diagnosed with hereditary hemochromatosis. The HFE gene mutations responsible follow autosomal recessive inheritance, meaning siblings of an affected person have a 25% chance of having the condition themselves and a 50% chance of being carriers. First-degree relatives (parents, siblings, children) of newly diagnosed patients are typically advised to undergo screening, since early diagnosis allows treatment to begin before iron accumulates to harmful levels. Many cases are identified through family screening rather than symptom-driven evaluation.
Conditions Treated with Therapeutic Phlebotomy
Genetic iron overload disorder. Most common indication for therapeutic phlebotomy. Removes excess iron stored in liver, heart, pancreas. Typical schedule: weekly during depletion phase, then every 2-4 months for life.
Bone marrow disorder producing too many red blood cells. Phlebotomy reduces blood thickness and clot risk. Treatment targets hematocrit under 45% (men) or 42% (women). Often combined with low-dose aspirin and other medications.
Disorder of heme synthesis with iron-related skin manifestations. Phlebotomy reduces ferritin, improving enzyme function. Schedule similar to hemochromatosis depletion phase initially, then maintenance based on ferritin levels.
Elevated red blood cell count from causes like sleep apnea, smoking, high-altitude living, or testosterone supplementation. Less common indication; phlebotomy used selectively when hematocrit reaches dangerous levels.
The actual procedure for therapeutic phlebotomy is straightforward but requires more equipment and time than a routine diagnostic blood draw. Patients arrive at the clinic, complete check-in (which usually includes a brief health questionnaire and vital signs check), and are escorted to a comfortable reclining chair. The phlebotomist confirms identity, reviews the order from the prescribing physician, and explains the procedure if the patient is new.
Vein selection follows standard practices — a large vein in the antecubital fossa (inner elbow) is preferred. The phlebotomist applies a tourniquet, identifies the vein, cleans the site, and inserts a 16- to 18-gauge needle (larger than diagnostic blood draw needles to allow faster blood flow). Blood flows by gravity into a collection bag positioned below the patient. The bag is on a scale that monitors weight as it fills, ensuring the correct volume is collected.
During collection, the phlebotomist monitors the patient for any signs of vasovagal reaction (lightheadedness, nausea, sweating) or other adverse effects. Some clinics provide patients with a small ball to squeeze and release rhythmically, which keeps blood flowing steadily. Most therapeutic phlebotomy sessions take 15 to 30 minutes for the actual blood removal portion, with an additional 15-30 minutes for setup and recovery, totaling about an hour per visit.
After the bag reaches the prescribed volume, the phlebotomist clamps the line, removes the needle, and applies pressure with sterile gauze. A bandage is applied. The patient is offered fluids (water, juice) and typically a light snack to support blood volume recovery. The patient remains in the chair for 10-15 minutes of monitoring before being discharged, with instructions to avoid strenuous activity for the rest of the day, drink extra fluids, and monitor for any delayed reactions like persistent dizziness or significant bruising.
Cost and insurance coverage vary by indication. Therapeutic phlebotomy for diagnosed conditions like hemochromatosis and polycythemia vera is typically covered by insurance because it's a medically necessary treatment. Some patients find their hospital outpatient phlebotomy charges higher than expected — exploring alternatives like blood donation centers (which may accept therapeutic phlebotomy patients for free or reduced fees in some regions) can substantially reduce costs over years of treatment. Phlebotomy classes often cover therapeutic phlebotomy as a specialty topic for those interested in working in this niche of the field.
Treatment of polycythemia vera requires careful monitoring of more than just hematocrit. Platelet counts, white blood cell counts, and the patient's overall thrombosis risk all factor into management decisions. Some patients also receive cytoreductive medications like hydroxyurea or interferon alongside phlebotomy, especially those at higher thrombotic risk based on age and prior clot history. Coordination between hematology specialists managing the medical regimen and the phlebotomy team performing scheduled draws is essential for optimal long-term outcomes in this complex condition.
Therapeutic Phlebotomy: Process Stages
Before therapeutic phlebotomy begins, your physician confirms the underlying diagnosis through:
- Lab tests: Ferritin, transferrin saturation, hematocrit, hemoglobin, CBC
- Genetic testing for hemochromatosis (HFE gene mutations)
- Bone marrow biopsy for polycythemia vera diagnosis
- Baseline organ function: Liver enzymes, EKG, cardiac evaluation
Establishing baseline values guides treatment intensity and target endpoints.
Therapeutic phlebotomy and blood donation share many similarities — both involve removing approximately one unit of blood through similar techniques. However, they're regulated and performed differently. Blood donation collects blood for transfusion to other patients; donors must meet rigorous health screening requirements, and the blood undergoes infectious disease testing and processing before transfusion. Therapeutic phlebotomy is performed for the patient's own benefit, with no requirement for the patient to meet donor health standards (though they cannot also be donors if their condition makes them ineligible).
Some hemochromatosis patients can have their therapeutic phlebotomy collected as eligible blood donations through programs that allow this — providing a benefit to the broader blood supply while still receiving treatment. The patient still receives medical management of their condition, but the cost may be reduced or eliminated since blood donation centers don't typically charge donors. Eligibility depends on the specific blood center's policies and the patient's overall health status. The American Red Cross and many community blood centers have programs allowing this, sometimes called "Hemochromatosis Donor Programs."
Side effects of therapeutic phlebotomy are generally mild but can include fatigue (especially in the hours following treatment), lightheadedness, bruising at the needle site, and occasional vasovagal episodes during the procedure itself. Patients on the depletion phase — getting weekly sessions — typically feel more fatigued than those on maintenance. Some patients develop iron-deficiency related symptoms (more common in hemochromatosis treatment if the depletion phase is too aggressive) like restless legs, brittle nails, or hair thinning; these resolve once iron levels stabilize and maintenance frequency adjusts.
For patients managing therapeutic phlebotomy long-term, lifestyle considerations help optimize outcomes. Iron-rich foods (red meat, organ meats, iron-fortified cereals) don't need to be strictly avoided in hemochromatosis but shouldn't be over-consumed; a balanced diet works well alongside treatment. Vitamin C with iron-rich meals enhances absorption — relevant to monitor in hemochromatosis. Alcohol consumption should be limited because it accelerates liver damage in iron-overload conditions. Most patients with managed hemochromatosis or polycythemia live full normal lifespans with appropriate phlebotomy maintenance, making these treatable rather than progressive conditions.
Insurance coverage and authorization for therapeutic phlebotomy varies significantly between insurers. Most plans cover medically necessary therapeutic phlebotomy for documented diagnoses, but some require prior authorization, specific provider credentials (hematologist orders), or particular billing codes. Patients new to therapeutic phlebotomy benefit from confirming coverage and authorization requirements with both the prescribing physician's office and their insurance company before beginning treatment. Out-of-pocket costs without proper authorization can be substantial, especially during the depletion phase requiring weekly sessions over several months.
Don't continue weekly sessions indefinitely after your levels reach the target range — over-aggressive phlebotomy causes iron deficiency and anemia. Likewise, don't extend intervals beyond what your labs support — under-treatment lets iron or blood cell counts drift back into harmful ranges. Regular lab monitoring (ferritin, hematocrit, CBC) is the basis for adjusting your schedule. Treat the schedule as flexible based on your individual response, not a fixed protocol.
For phlebotomists and nurses interested in working in therapeutic phlebotomy, the role offers different challenges and rewards than routine diagnostic phlebotomy. Patients are seen repeatedly over time, building therapeutic relationships and trust that develop differently from a single-encounter blood draw at a lab. Recognizing subtle changes in patient condition — increased fatigue, mood changes, signs of iron deficiency — becomes part of the role beyond just the technical procedure.
Pursuing this work typically requires holding a phlebotomy certification first (the standard credential demonstrating you've completed an approved phlebotomy certification program), then specific on-the-job training in therapeutic protocols. Many therapeutic phlebotomy positions are at hospital outpatient centers, hematology and oncology clinics, and some specialty blood centers. The roles often pay slightly higher than routine phlebotomy because of the specialized skills required and the more complex patient population.
Therapeutic phlebotomy programs are also growing in scope as awareness of hemochromatosis improves diagnosis rates. Many people with the condition go undiagnosed for years before symptoms become severe, and family screening of newly diagnosed patients often reveals additional cases. As more patients enter long-term phlebotomy programs, the demand for trained phlebotomists in this specialized area continues to grow alongside the broader phlebotomy field.
For patients themselves, accepting therapeutic phlebotomy as a permanent part of life can be psychologically challenging at first. The procedure is inconvenient, time-consuming over the years, and a constant reminder of the underlying condition. But framed against the alternative — progressive organ damage in untreated hemochromatosis or stroke and clot risk in untreated polycythemia — therapeutic phlebotomy is a remarkably effective treatment that allows most patients to live normally. Many patients adapt to the routine well, scheduling sessions around their lives like any other recurring health appointment, and find the visible objective progress (lab values normalizing, symptoms improving) genuinely satisfying.
Quality of life with managed hemochromatosis or polycythemia vera is generally excellent for patients diagnosed and treated before significant organ damage occurs. The treatments themselves are minor compared to many chronic disease management protocols — no daily medications, no dietary restrictions for most patients, and a procedure that takes about an hour every few months once stable. Patients often describe the routine as similar to going to the gym in time commitment and overall impact on their lives. Communicating openly with employers about needing periodic medical appointments helps make the schedule sustainable across decades of treatment.
Therapeutic phlebotomy is one of the most direct demonstrations of how a simple procedure can manage a serious chronic condition effectively over a patient's lifetime, often without significantly diminishing their quality of life or daily activities.
Therapeutic Phlebotomy Numbers
Therapeutic Phlebotomy: Treatment Tradeoffs
- +Highly effective for iron overload and elevated red blood cell counts
- +No medication side effects — relies on natural blood-volume restoration
- +Inexpensive long-term compared to medication-based alternatives
- +Generally well-tolerated with mild side effects
- +Some hemochromatosis patients can donate to blood supply, benefiting others
- −Lifelong commitment for genetic conditions like hemochromatosis
- −Time-consuming — sessions can take an hour or more including transit
- −Frequent sessions during depletion phase can cause fatigue and inconvenience
- −Requires regular lab monitoring to guide schedule adjustments
- −Vein access can become difficult after years of repeated draws in the same site
Phlebotomy Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.