MRI of Brain: What It Shows, How It Works, What to Expect
Brain MRI explained: how it works, conditions detected (tumors, stroke, MS), procedure, contrast use, claustrophobia handling, and results timeline.
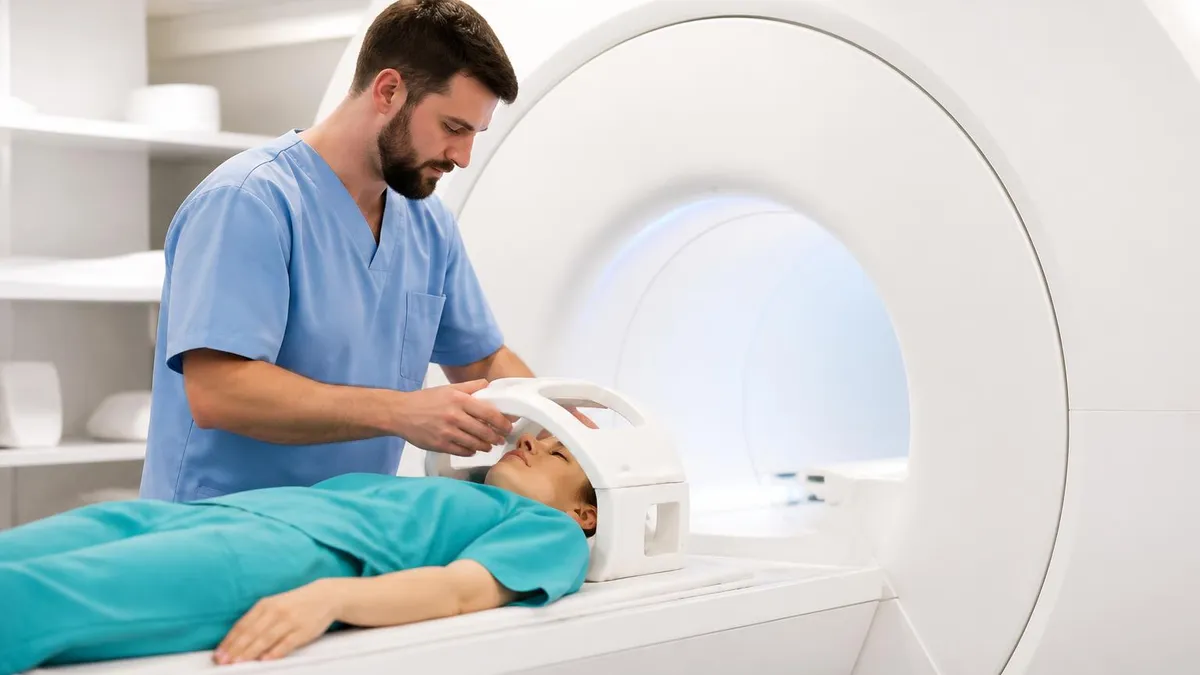
An MRI of the brain is one of the most powerful diagnostic tools in modern medicine, providing detailed images of brain tissue, blood vessels, and surrounding structures without ionizing radiation. Unlike CT scans which use X-rays, MRI uses powerful magnetic fields and radio waves to create cross-sectional images that reveal soft tissue detail impossible to see with other imaging modalities. Neurologists, neurosurgeons, and other physicians order brain MRIs to investigate symptoms ranging from chronic headaches and seizures to suspected stroke, multiple sclerosis, brain tumors, and neurodegenerative diseases.
The technology behind MRI is genuinely remarkable. Powerful superconducting magnets (typically 1.5 Tesla or 3 Tesla in clinical use, with research scanners reaching 7 Tesla and higher) align the protons in your body's water molecules. Radio frequency pulses then disturb this alignment, and as the protons relax back to their original position, they emit radio signals that the scanner detects and processes into images.
Different tissue types relax at different rates, creating contrast between gray matter, white matter, cerebrospinal fluid, blood, and pathological tissues. Specialized sequences can highlight specific features — diffusion-weighted imaging shows acute strokes, FLAIR sequences highlight white matter abnormalities, MR angiography shows blood vessels, and many others.
Brain MRI Quick Facts
Duration: 30-60 minutes typically. Cost: $400-$3,500 (varies dramatically by location and insurance). Contrast: Gadolinium-based, used for tumors, infections, MS, vascular abnormalities. Radiation: None — MRI uses magnetic fields, not radiation. Common findings: Tumors, stroke, MS lesions, aneurysms, hemorrhage, atrophy. Pre-scan check: Metal implants, pacemakers, claustrophobia all matter.
Common indications for brain MRI include suspected stroke (particularly in the first hours when treatment decisions are time-sensitive), persistent or unusual headaches that haven't responded to treatment, seizures of new onset or unknown cause, suspected multiple sclerosis or other demyelinating diseases, suspected brain tumor based on neurological symptoms, head trauma evaluation when CT findings are inconclusive, evaluation of memory loss or cognitive decline, hearing loss that may be neurological in origin, vision problems that may originate in the brain rather than the eye, and follow-up of known conditions to track progression or treatment response.
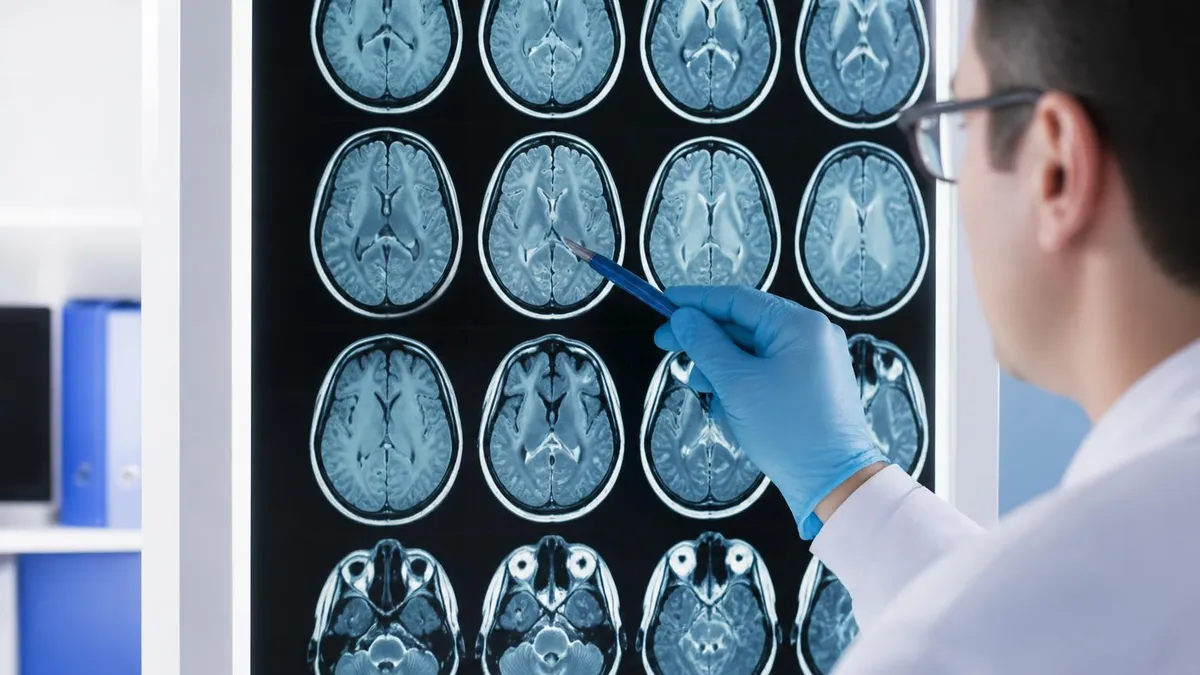
What Brain MRI Detects
Both primary brain tumors (gliomas, meningiomas) and metastases from cancers elsewhere in the body. MRI distinguishes solid masses, cystic components, and surrounding edema.
Acute infarcts visible within minutes on diffusion-weighted imaging. Older strokes appear as encephalomalacia (cystic damage). MR angiography shows vessel occlusions.
Demyelinating lesions in white matter, characteristically in periventricular and juxtacortical locations. FLAIR sequences highlight lesions; gadolinium identifies active disease.
Aneurysms, arteriovenous malformations, cavernous angiomas. MR angiography images vessels; susceptibility-weighted imaging highlights small vessel disease.
Excess cerebrospinal fluid causing ventricle enlargement. MRI quantifies severity and distinguishes types (communicating, obstructive, normal pressure).
Volume loss patterns suggest specific dementia types. Hippocampal atrophy in Alzheimer's; frontal/temporal patterns in frontotemporal dementia.
Stroke evaluation deserves specific attention because brain MRI's role in stroke care has expanded dramatically with newer treatment options. Diffusion-weighted imaging (DWI) shows ischemic injury within minutes of stroke onset, much earlier than CT scans typically detect ischemia. This early detection enables treatment decisions including thrombolysis (clot-busting drugs) and mechanical thrombectomy (catheter-based clot removal) that have time-sensitive windows. Many stroke centers now use MRI rather than CT for primary stroke evaluation when imaging time allows, though CT remains the initial study in many emergency departments due to availability and faster scan times.
Tumor characterization on MRI guides surgical planning, radiation therapy planning, and treatment response monitoring. Different tumor types have characteristic imaging appearances that experienced neuroradiologists can often recognize, though biopsy remains necessary for definitive diagnosis. MRI shows tumor location, size, relationship to critical structures, presence of necrosis or hemorrhage, surrounding edema, and degree of contrast enhancement. Functional MRI (fMRI) and diffusion tensor imaging (DTI) help neurosurgeons plan resections that preserve critical brain functions and white matter tracts. Treatment response monitoring uses serial MRIs to assess whether tumors are responding to therapy.
Multiple sclerosis (MS) diagnosis and management rely heavily on brain MRI. The McDonald criteria for MS diagnosis specifically incorporate MRI findings, and treatment decisions depend on lesion burden and disease activity assessment. Characteristic MS lesions appear as bright spots on T2 and FLAIR sequences, typically located in periventricular white matter, juxtacortical regions, brainstem, cerebellum, and corpus callosum. New lesions appearing between scans or showing gadolinium enhancement indicate active disease, prompting treatment adjustments. MRIs every 6-12 months are common for monitoring stable patients; more frequent imaging during periods of clinical change.
Common MRI sequences for brain: T1-weighted shows anatomical detail with gray/white differentiation. T2-weighted highlights fluid content and pathology. FLAIR (fluid-attenuated inversion recovery) suppresses CSF signal making white matter lesions more visible. Diffusion-weighted imaging (DWI) detects acute ischemia and some other pathologies. Susceptibility-weighted imaging (SWI) highlights blood products and microbleeds. MR angiography (MRA) images blood vessels. Each sequence answers different clinical questions; comprehensive brain MRI uses multiple sequences.
Preparation for brain MRI is generally minimal but specific items matter. Before the scan, the technologist will screen for metal implants and devices that might be affected by the magnetic field or might create image artifacts. Pacemakers and most cardiac defibrillators historically prevented MRI but newer MRI-conditional devices allow scanning under specific conditions. Cochlear implants prevent MRI in most cases. Aneurysm clips, certain orthopedic hardware, retained metal fragments (particularly in eyes), and other implants need verification of MRI compatibility. Bring records of any implants — manufacturer documentation typically includes MRI safety information.
What to wear for MRI matters because metal in clothing can affect image quality. Most facilities provide gowns; if you wear your own clothes, choose items without metal zippers, snaps, hooks, or printed designs that might contain metallic ink. Remove all jewelry, watches, hair accessories, hearing aids, and dental retainers (unless permanently affixed). Makeup containing metallic particles (some mascara, eye shadow) should be removed since it can affect image quality. Bring case for eyeglasses or contacts since vision aids must be removed.
Claustrophobia affects a significant minority of MRI patients and deserves planning before scheduling. The scanner tunnel is approximately 24 inches in diameter and patients lie within it for 30-60 minutes during brain MRI. Anti-anxiety medication (like alprazolam or lorazepam) prescribed by your physician helps many patients tolerate the experience. The medication needs to be taken about an hour before scan time and requires someone else to drive you home afterward. Some facilities offer wider-bore scanners (70cm versus traditional 60cm) that feel less confining. Open MRI scanners trade image quality for patient comfort. Discuss anxiety with the ordering physician before scheduling.
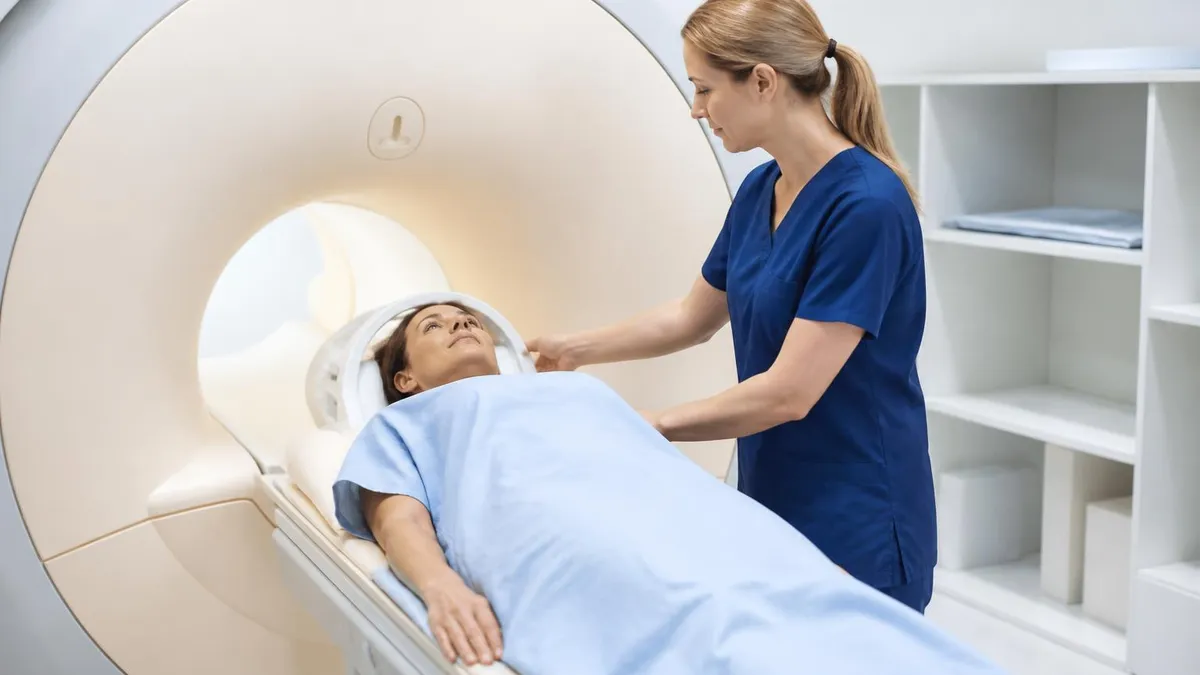
Always disclose: pacemakers, cardiac defibrillators, cochlear implants, aneurysm clips, surgical implants, retained metal fragments (especially in eyes), tattoos with metallic ink, recent surgical staples, body piercings, magnetic dental implants, drug delivery patches with metallic components. Pregnancy: MRI generally avoided in first trimester unless absolutely necessary. Gadolinium contrast specifically avoided during pregnancy. Severe kidney disease: Restricts gadolinium use due to nephrogenic systemic fibrosis risk.
The scanner experience is loud — much louder than most patients expect. The various MRI sequences produce knocking, banging, beeping, and whirring sounds at volumes that can exceed 100 decibels. Standard practice provides earplugs and over-ear headphones for hearing protection and to play music or audiobooks during scanning. Modern scanners are progressively quieter through engineering improvements, but they remain significantly louder than typical medical procedures. The noise serves a purpose — it's caused by gradient coils rapidly switching the magnetic field to enable spatial encoding of signals. Without these gradient pulses, images couldn't be created.
Stillness during scanning matters because patient motion blurs images. Even small movements of the head create motion artifacts that obscure findings or require sequences to be repeated. The head is typically positioned in a specialized coil receiver that stabilizes head position with foam padding. Patients are instructed to remain still and breathe normally — actual breathing motion at the chest doesn't significantly affect head images. Closing your eyes can help reduce the impulse to move. Some patients find that focusing on music through the headphones helps with stillness. Coughing, sneezing, or swallowing should be done between sequences when possible.
After the scan, you can typically resume normal activities immediately if no contrast or sedation was used. With gadolinium contrast, drink extra water for 24 hours to help clear the agent from your system. With sedation medication, you'll need someone to drive you home and should avoid important decisions or operating machinery for at least 12 hours. Contrast can rarely cause delayed reactions including itching, rash, or nausea — contact the imaging facility if these occur. Most patients have no immediate effects from MRI and can return to normal activities right away.
Before Your Brain MRI
- ✓Disclose all metal implants, devices, and surgical history
- ✓Disclose pregnancy status if applicable
- ✓Inform facility of claustrophobia concerns to plan accommodations
- ✓Disclose kidney disease history (affects contrast use)
- ✓Remove all jewelry, watches, hair clips before scan
- ✓Bring list of medications and allergies
- ✓Arrange driver if anti-anxiety medication will be used
- ✓Prepare for 30-60 minute scan in confined space
Result interpretation typically takes 1-3 business days for routine brain MRI. The radiologist generates a report describing findings sequence by sequence, with overall impression and recommendations. The report goes to the ordering physician who shares results with you, often during follow-up appointment. For urgent findings (suspected stroke, large tumor, acute hemorrhage), the radiologist will call the ordering physician immediately rather than waiting for written report. Some facilities offer patient portals for direct access to imaging reports — discuss with your physician how you'll receive results.
Understanding your MRI report requires medical knowledge beyond what most non-physicians have. Reports use specific medical terminology and reference specific anatomical structures. Common findings have specific implications that require clinical context to interpret. Discuss the report with the ordering physician rather than trying to interpret independently. The physician will explain what was found, what it means in your specific context, and what next steps (additional testing, treatment, monitoring) follow. If you don't understand something in the explanation, ask questions until you do — informed decisions require understanding what's happening.
Incidental findings on brain MRI are common — small abnormalities discovered while looking for something else. These might include small white matter changes that may be age-related or related to vascular risk factors, small benign cysts, mild atrophy, or minor anatomical variants without clinical significance. Some incidental findings warrant follow-up (small aneurysms, ambiguous lesions); others are clearly benign and need no action. Your physician interprets findings in context of your symptoms, age, and overall health. Don't panic about incidental findings before discussing with the ordering physician — many require no action at all.
Cost considerations for brain MRI vary dramatically by region, facility type, and insurance coverage. Hospital-based MRI typically costs more than outpatient imaging center MRI for the same study. Insurance coverage usually applies when MRI is medically indicated by physician order. Without insurance, costs range from $400-$3,500 with substantial regional variation. Cash-pay rates at outpatient imaging centers are often dramatically lower than the rates billed to insurance. Some patients without insurance specifically seek cash-pay rates that can be 50-80% less than insurance-billed rates. Health savings account (HSA) and flexible spending account (FSA) funds can be used for MRI expenses.
The technology landscape continues evolving. 3 Tesla scanners produce sharper images than 1.5 Tesla scanners and are increasingly common but cost more and have different safety considerations for some implants. 7 Tesla scanners are starting to appear in research and select clinical applications, providing extraordinary detail particularly for high-resolution brain imaging. Functional MRI (fMRI) maps brain activity by detecting blood oxygenation changes. Diffusion tensor imaging (DTI) maps white matter tracts. MR spectroscopy analyzes chemical composition of tissue. These advanced techniques are increasingly part of standard clinical brain MRI for specific indications.
Artificial intelligence is increasingly involved in brain MRI interpretation. AI algorithms can detect specific abnormalities (some tumors, hemorrhages, large vessel occlusions) with sensitivity comparable to or exceeding human radiologists for those specific tasks. Current clinical use typically involves AI as second-reader assistance — flagging potential findings for human radiologist review rather than replacing the radiologist. The technology continues to advance rapidly, and AI's role in brain MRI interpretation will likely grow substantially over the coming decade. The fundamental clinical relationship between you, your physician, and your imaging will continue but with increasingly sophisticated tools assisting interpretation.
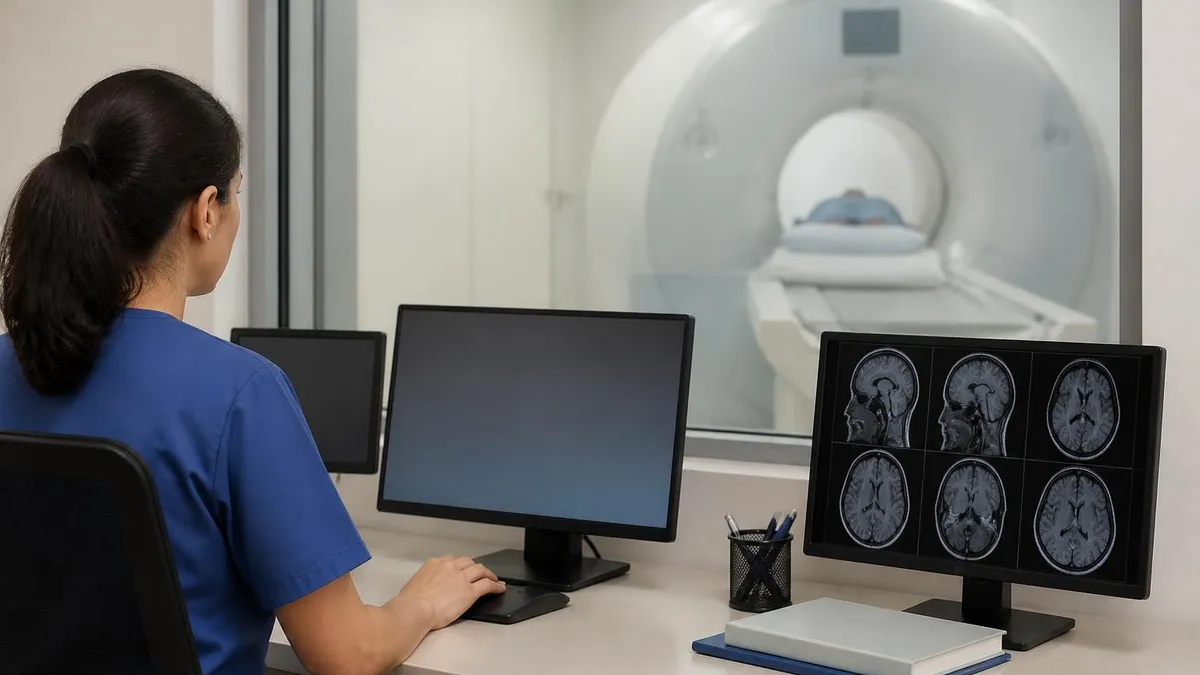
Brain MRI Quick Numbers
Brain MRI vs CT Scan
MRI dramatically better for soft tissue detail. CT shows bone better but soft tissue contrast is far inferior.
MRI detects ischemia minutes after onset; CT typically takes hours. CT remains useful for ruling out hemorrhage quickly.
CT is faster for trauma evaluation when speed matters and patient may be unstable. MRI follows up specific findings or for chronic evaluation.
MRI provides much better tumor characterization than CT. Standard for staging and treatment planning.
CT cheaper and more widely available, particularly in emergency departments. MRI access varies more by location.
CT uses ionizing radiation (small risk with frequent scans). MRI uses no radiation, preferable for repeated imaging.
For radiology technologists and students considering MRI as a career specialty, brain MRI represents one of the most demanding and rewarding subspecialties. Brain anatomy is intricate, the variety of pathologies requires substantial knowledge, and the diagnostic stakes are high. ARRT (American Registry of Radiologic Technologists) certification in MRI requires specific clinical hours and examination passing. Beyond entry-level certification, advanced specialization in neuroimaging develops over years of focused practice. Salaries for experienced MRI technologists in major medical centers typically run $75,000-$120,000+ depending on location and experience.
For radiologists, neuroradiology subspecialty fellowship represents 1-2 additional years of training after diagnostic radiology residency. Subspecialty certification in neuroradiology requires additional examinations beyond core radiology certification. Neuroradiologists at academic medical centers typically focus exclusively on neuroimaging, while community-based radiologists may interpret brain MRIs alongside other imaging types. The specialty continues evolving with advances in functional imaging, AI assistance, and increasingly sophisticated brain imaging techniques. Physician compensation in radiology subspecialties varies but neuroradiologists typically earn $400,000-$700,000+ depending on practice setting and location.
Patient experience improvements have become a focus area for MRI facilities competing for outpatient business. Wider-bore scanners reduce claustrophobia. Music and video systems entertain patients during scans. Faster scan sequences reduce time in the scanner. Comfortable padding makes the scan table tolerable for the duration. Some facilities offer themed scan rooms (ocean, forest, sky) with projected images that distract from the confined environment. Patient communication systems let patients talk with technologists during scanning. These improvements help patients tolerate the experience better and reduce the need for sedation or motion-disrupted scans that require repeating sequences.
Repeat imaging and follow-up scans are common in chronic conditions. Multiple sclerosis patients typically have brain MRIs every 6-12 months to monitor disease activity. Tumor patients have follow-up MRIs every 3-6 months during treatment and less frequently after stable response. Stroke patients often have follow-up imaging weeks or months after the acute event to assess recovery. Each follow-up provides comparison with prior imaging, allowing detection of subtle changes that single scans wouldn't reveal. Maintaining all your imaging at one facility (or ensuring images are shared between facilities) supports better comparison and consistent interpretation over time.
Imaging archives and your right to your images deserve attention. Your imaging studies belong to you medically, though physical or digital copies typically remain with the imaging facility. You can request copies on CD or via electronic delivery to share with other physicians or for your personal records. Many facilities offer patient portal access to view and download your imaging.
Some facilities charge for additional copies; the original interpretation report is typically provided without charge to you and your physician. Keep records of your imaging history — you'll thank yourself in years when comparing new studies with old becomes important for diagnosis or treatment decisions.
Brain MRI continues to be one of the most consequential diagnostic tools in modern medicine, providing detailed information that guides treatment decisions across neurology, neurosurgery, oncology, and many other specialties. Understanding what to expect, how to prepare, and how to interpret results in collaboration with your physician helps you participate effectively in your own healthcare. Don't fear the experience — most patients tolerate brain MRI well, and the information it provides often dramatically improves diagnosis and treatment outcomes for serious neurological conditions.
Brain MRI: Pros and Cons
- +No ionizing radiation — safe for repeated imaging
- +Superior soft tissue detail vs. CT or X-ray
- +Detects acute stroke within minutes of onset
- +Comprehensive tumor characterization
- +Multiple sequences provide different information
- +Functional and advanced techniques available
- −Higher cost than CT in most regions
- −Longer scan time (30-60 min vs CT minutes)
- −Loud scanner noise can be uncomfortable
- −Confined tunnel triggers claustrophobia in many patients
- −Some implants prevent MRI use
- −Gadolinium contrast restricted in kidney disease
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.