MRI vs CT Diagnostics: How Each Scan Works, When Doctors Choose One, and What Techs Should Know
Compare MRI and CT diagnostics in plain English. See how each scan works, what conditions they spot, and which test physicians order in real cases.
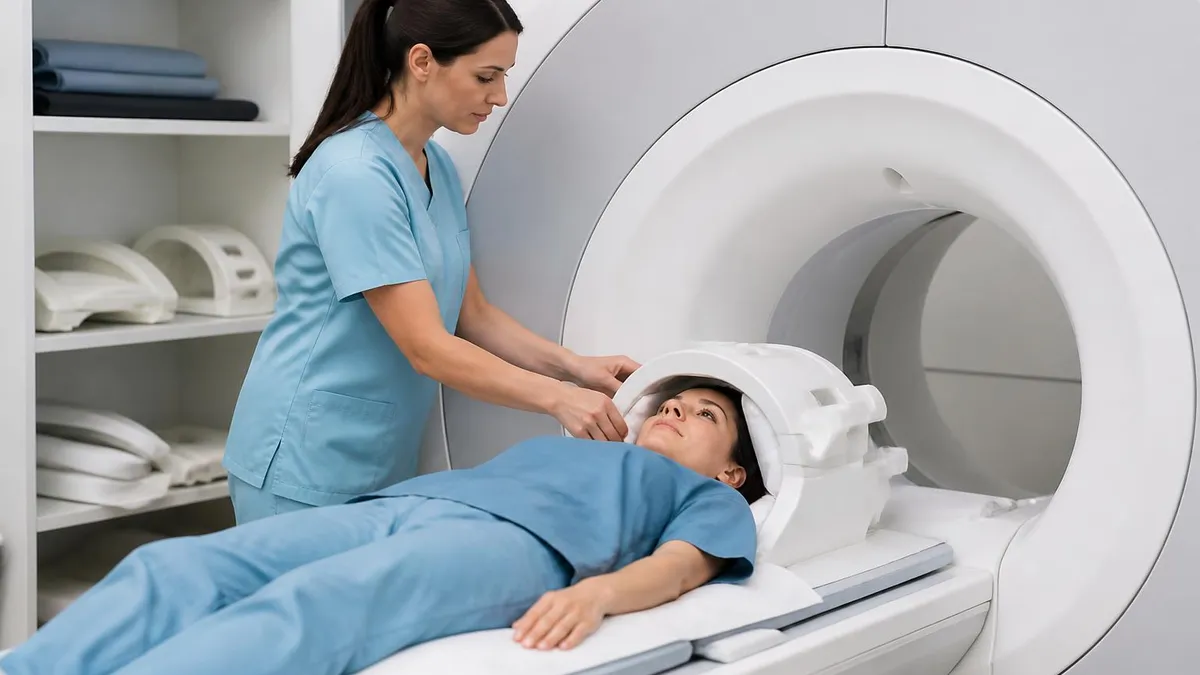
If you have ever sat in a hospital waiting room watching a colleague get wheeled toward radiology, you have probably wondered the same thing most patients wonder. Why does one person get an MRI and the next person get a CT scan? They both produce slick cross-sectional images. They both cost a lot of money. They both ask you to lie very, very still. Yet doctors pick between them with surprising confidence, sometimes inside thirty seconds of looking at a chart.
The short answer: these machines are good at very different things. CT is fast and brilliant at bone, bleeding, and lung tissue. MRI takes longer but delivers staggering soft tissue detail without ionizing radiation. Knowing which tool fits which clinical question is half the job for anyone working in diagnostic imaging, and it is also the part that the certification exams love to test.
This guide walks through the practical side of MRI and CT diagnostics, the kind of thing a working tech needs in their head every shift. We will cover how each modality forms an image, the conditions where each shines, common pitfalls, and what the exam writers expect you to know on test day. Some of it is bookwork. Some of it only comes from time in the scan room. Both matter.
MRI and CT by the Numbers
Those four numbers tell you almost everything about why both scanners earn their place in a hospital. MRI uses no radiation at all, which is huge for pediatric patients, pregnant patients, and anyone who needs repeat imaging over years. CT, on the other hand, finishes a chest study before the patient has time to ask whether they should hold their breath again. Speed wins in trauma. Contrast wins in tumor follow-up. The machines complement each other more than they compete.
Most diagnostic imaging programs teach the physics behind each modality early on, but in practice the field strength of your magnet and the slice thickness on your CT protocol matter more day-to-day than any equation. The exam will still ask you about Larmor frequency and Hounsfield units, so we will not skip those, but the goal here is to connect the textbook to the patient on the table.
One useful exercise: walk through a typical day in a busy radiology department in your head. Morning starts with outpatient MRI knees, shoulders, and lumbar spines. Mid-morning the ED starts dropping trauma CTs and stroke head CTs. Afternoon brings oncology follow-ups, both modalities. Late evening tilts back toward ED, mostly CT. The pattern shows you which exams support which clinical questions far better than any flowchart ever will.
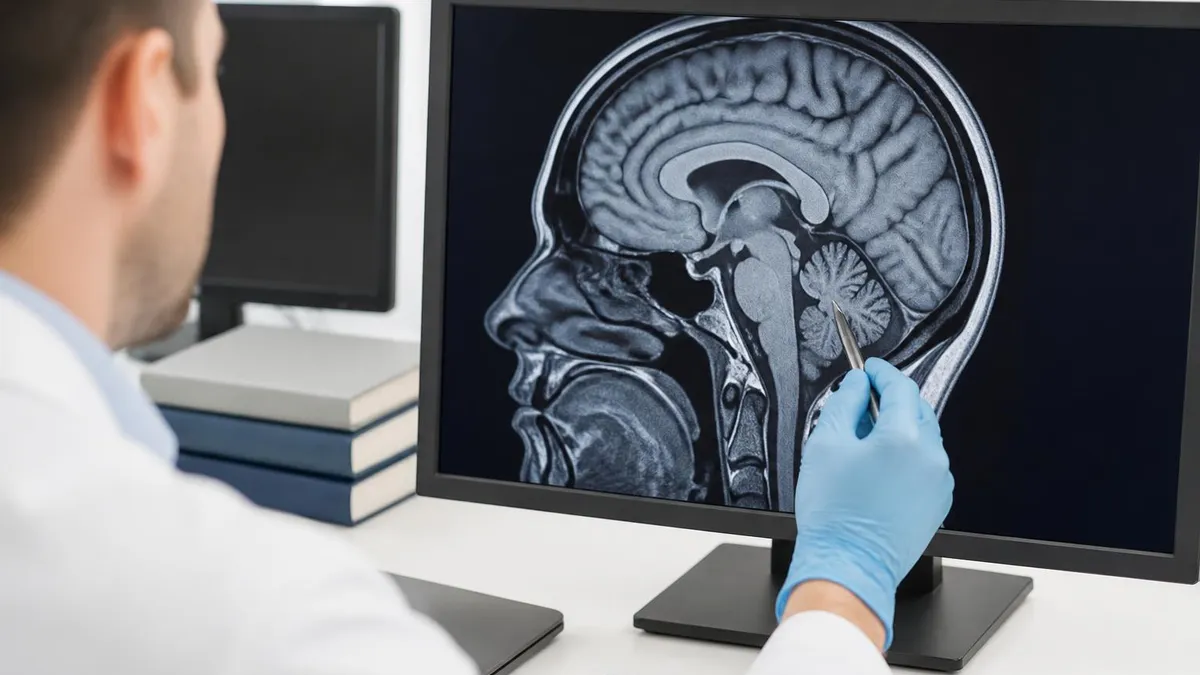
Think bone, blood, or breath, lean CT. Think brain tissue, ligaments, cartilage, spinal cord, or any soft tissue tumor, lean MRI. It is not perfect, but it covers maybe seventy percent of the everyday decisions a referring physician makes.
That rule of thumb hides a lot of nuance. A stroke patient gets a non-contrast head CT first, almost always, because CT rules out hemorrhage in minutes. Once bleeding is excluded, MRI takes over to define the actual ischemic territory with diffusion-weighted sequences. Two machines, same patient, two completely different answers, both critical. Acute care is where you really see the team play out.
Outpatient work tells a different story. A 35-year-old with a torn meniscus does not need a CT. The orthopedic surgeon wants T2 fat-suppressed images of the knee, and only MRI delivers that. A 60-year-old with new abdominal pain and weight loss probably gets a contrast-enhanced CT abdomen and pelvis on day one, because CT covers a huge volume fast and catches the most common emergencies, from appendicitis to bowel obstruction to mass lesions.
The choice almost always comes down to three questions. What tissue am I trying to see. How fast do I need the answer. Can the patient tolerate the scan. Tolerance matters more than people admit. A claustrophobic patient may simply refuse the MRI bore. A patient with a pacemaker may not be MRI conditional. A patient with kidney disease may not get iodinated CT contrast. These constraints shape the order set as much as the clinical question does.
How Each Modality Forms an Image
An x-ray tube rotates around the patient while detectors opposite measure how much radiation gets through. A computer reconstructs cross-sectional slices based on tissue attenuation. Bone blocks the most x-rays and shows up bright. Air blocks the least and shows up dark. Everything else falls somewhere in between on the Hounsfield scale, which is the standard reference radiologists use to interpret CT images.
Patients enter a powerful static magnetic field that aligns hydrogen protons in the body. Radiofrequency pulses knock those protons out of alignment, and when they relax back, they emit signals that coils detect. Different tissues relax at different rates, which is where T1 and T2 weighting comes from. The sequences a tech selects determine which tissue contrasts show best.
CT uses iodinated contrast, usually injected through an IV, to highlight blood vessels and well-perfused organs. MRI uses gadolinium-based contrast for similar reasons. Each has different contraindications, and the techs running the scan are the last line of defense for catching them. Kidney function, allergy history, and pregnancy status all factor into the contrast decision.
Both machines produce DICOM files that PACS systems can store, send, and display. The pixel data is different under the hood, but the workflow downstream looks similar. Radiologists read both off the same workstations using window and level controls to emphasize the tissue of interest in any given image.
Hounsfield units come up constantly on the CT side. Water sits at zero by definition. Air is around negative one thousand. Cortical bone runs from about three hundred up past two thousand. Fat hovers around negative one hundred. Acute blood reads roughly fifty to eighty, which is why a fresh hemorrhage looks bright on a non-contrast head scan even before any contrast goes in. Memorize the rough numbers because the exam will ask, and the day-to-day window and level adjustments make a lot more sense once you have them.
On the MRI side, the signal intensity vocabulary is different. Bright on T1 weighted images means short T1 relaxation time, which is what fat and subacute hemorrhage and high-protein fluid show. Bright on T2 weighted means long T2, which is what water, edema, CSF, and most pathology show. T2 weighting is sometimes called the pathology sequence for a reason. Fluid loves to be bright on T2.
FLAIR, diffusion, gradient echo, STIR, post-contrast T1 with fat saturation. Each sequence is essentially a different physics recipe to make certain tissues more conspicuous. Stroke protocols rely heavily on diffusion-weighted imaging because acute ischemia restricts water movement, lighting up like a beacon while the rest of the brain stays dim. Spine protocols add STIR to suppress fat and bring out edema in vertebral bodies and discs. Knowing why a sequence exists, not just what it looks like, is what separates the techs who run the protocol from the techs who own the exam.
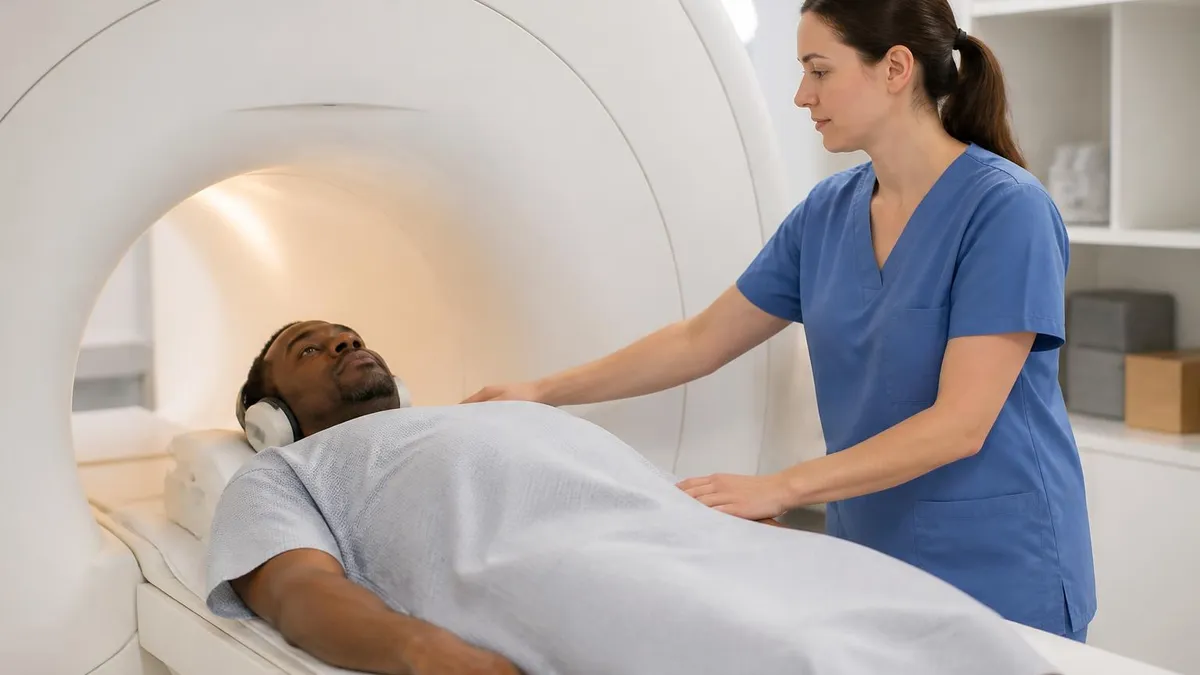
Modality Choice by Body Region
Those tabs are not academic, they map directly to how a busy reading room actually triages cases. A radiologist clearing the worklist will spot a head CT done at three in the morning and assume trauma or stroke until proven otherwise. They will spot a knee MRI done at three in the afternoon and assume meniscus or ACL. The protocol tells a story before any image opens.
One of the most useful skills you can build as a new tech is reading the order alongside the protocol. If the order says rule out pulmonary embolism but the protocol is a non-contrast chest, somebody made a mistake. Catching that before the patient comes off the table saves a redo scan, an extra contrast dose, and probably a phone call to the ordering provider. The exam writers love these scenarios because they capture real workflow problems.
Patient prep matters too. CT abdomen with oral contrast needs the patient to drink one to two hours ahead. MRI enterography needs different oral prep. Cardiac CT needs heart rate control with beta blockers. MRI of the inner ear needs specific high-resolution sequences. None of this lives in the physics textbook, but all of it lives in the daily routine, and it is exactly the kind of question that shows up on board-style exams disguised as patient scenarios.
MRI safety zones one through four are not optional paperwork. Zone four is the magnet room, and that magnet is always on. Even when no scan is running. Oxygen tanks, IV poles, scissors, hairpins, and worse have all become projectiles. Always screen patients twice and never assume staff badges mean someone has been cleared.
Magnetic safety is the single most tested topic on the MRI registry, and it should be. The American College of Radiology publishes a safety framework that nearly every department adopts, and the four zones map roughly to escalating risk. Zone one is public access. Zone two is the screening area. Zone three is the controlled approach to the scanner. Zone four is the scanner room itself. The line between zone three and zone four is where the magnet field starts to throw ferromagnetic objects.
CT has its own safety conversation, but it centers on radiation dose. ALARA, as low as reasonably achievable, is not just a slogan. It drives protocol choices. Iterative reconstruction, automatic exposure control, tube current modulation, kilovoltage adjustment, all of these are knobs the tech can use to lower dose without losing diagnostic quality. Pediatric protocols in particular have evolved enormously. A modern pediatric chest CT delivers a fraction of the dose it did fifteen years ago.
Contrast reactions on both sides need quick recognition. Mild reactions like hives or a transient warm flush usually need only observation. Moderate reactions like bronchospasm or significant urticaria need treatment. Severe anaphylactoid reactions are rare but real, and every imaging suite should have a crash cart and protocols. Iodinated contrast reactions tend to happen within minutes. Gadolinium reactions are much less common, but nephrogenic systemic fibrosis is the long-term concern in patients with poor kidney function, especially with older linear agents.
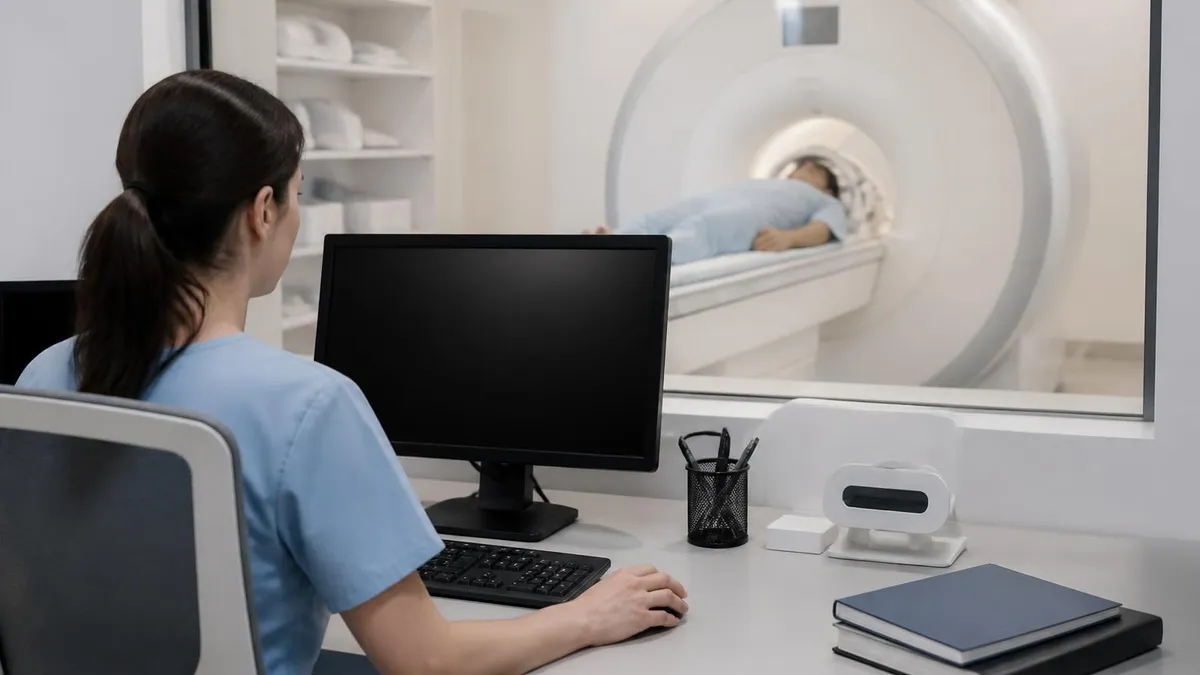
Pre-Scan Checklist Every Tech Should Run
- ✓Confirm patient identity with two identifiers, name and date of birth at minimum, and check the wristband against the request before any contrast goes in
- ✓Review the order and confirm the protocol matches the clinical question. If the protocol does not match the indication, stop and call the ordering provider
- ✓Screen for metal implants, pacemakers, neurostimulators, cochlear implants, aneurysm clips, drug pumps, and prior surgeries before any MRI
- ✓Check kidney function with a recent eGFR before iodinated or gadolinium contrast administration, and document the value in the patient record
- ✓Verify pregnancy status when appropriate, especially for CT abdomen and pelvis, and document a urine or serum test for women of childbearing age
- ✓Confirm IV access is patent, flushes freely, and the gauge is appropriate for the contrast injection rate the protocol requires
- ✓Brief the patient on breath holds, motion expectations, claustrophobia management, and how to signal the tech if they need to stop
- ✓Position the appropriate surface coil and use immobilization supports for the body part being imaged to keep motion artifact down
- ✓Document any deviations from standard protocol clearly in the patient record with the reason and the supervising radiologist contacted
- ✓Watch the patient through the first acquisition for motion, discomfort, or early signs of a contrast reaction before continuing the study
Reading a real case is the moment all that prep work pays off. Imagine a 52-year-old man comes through the emergency department with sudden severe headache. The triage nurse marks worst headache of life. The ED doctor orders a non-contrast head CT first because that is the fastest way to rule out a subarachnoid hemorrhage. The scan finishes in under a minute. The radiologist sees blood layered in the basal cisterns. Diagnosis confirmed, neurosurgery paged, time saved.
Now imagine a different 52-year-old, no headache, but new weakness in the right arm over two days. Same hospital, same imaging suite. Head CT shows nothing acute. The neurologist asks for an MRI brain with diffusion-weighted imaging. The MRI shows a small left motor cortex stroke, only a few hours old based on the diffusion characteristics. Two patients, two scanners, two diagnoses, both right the first time.
That is why no working radiology department picks one modality over the other. They run in parallel because they answer different questions. The job for the tech, and for anyone training for the registry, is to know which question fits which modality and to execute the protocol cleanly when the time comes.
MRI vs CT Pros and Cons
- + —
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
- − —
If you have ever scrolled through a knee MRI, you know how immediately satisfying soft tissue contrast can be. Cartilage, ligaments, marrow, fat, and fluid all separate cleanly. Compare that to a knee CT, which is great for fractures but does not show you a torn ACL clearly. The tradeoff cuts the other way in the chest. Lung parenchyma jumps off a CT image with stunning detail, while MRI struggles because air protons are sparse and motion artifact is brutal.
Cost and access matter outside the textbook. A typical CT scanner runs roughly one to two million dollars, while a high-field MRI runs three to five million or more. Rural hospitals are far more likely to have a CT than a 3T MRI. Outpatient imaging centers often have both, but their MRI schedule books out further. None of that changes what is best for a given patient, but it shapes how studies actually get ordered and read.
Workflow is another underrated factor. A trauma CT covers head, cervical spine, chest, abdomen, and pelvis in a single trip to the scanner. The patient goes from gurney to scan to back on the gurney inside ten minutes. MRI cannot match that throughput, and trauma surgeons know it. Even with the most efficient protocols, MRI takes time, and time costs lives in unstable patients.
There is also the radiologist side of the equation. Reading a brain MRI with five sequences across two planes takes longer than reading a single-pass head CT. Studies show MRI reads can take three to five times the wall-clock time of CT reads, and that gap shapes department scheduling. Faster equals more throughput, and CT is faster. None of this is a knock on MRI. It just explains why CT volumes are an order of magnitude higher than MRI volumes in most hospital systems.
MRI Questions and Answers
Building a real working knowledge of MRI and CT diagnostics takes repetition. The physics matters, the safety matters, the protocols matter, but case exposure is what locks it in. Every patient on the table teaches something the textbook missed. The tech who can articulate why one sequence was added and another was dropped becomes the tech the radiologists trust to set up the difficult cases.
If you are preparing for the MRI registry or a CT certification, treat this material as the skeleton and hang real cases on it. Walk into the reading room when you can. Ask what the radiologist is looking for before each scan. Read the protocols your department uses and ask why they look the way they do. The exam will reward that habit, and your patients will too. Good imaging is a team sport and the techs in the room set the tempo as much as anyone else.
One last thought before you head back to the work. Confidence on exam day usually comes from a small number of fundamentals practiced until they are automatic. Patient screening, contrast safety, basic physics, sequence purpose, modality choice by body region. Master those and the harder questions tend to fall into place. The exam writers are not trying to trick you. They want to see you reason through a clinical scenario the way a working tech would. That is exactly what diagnostic imaging is, scenario after scenario, every shift, every patient.
A practical study habit that pays off: keep a small notebook with every unusual case you see in the scan room. Even one or two lines per case. What was ordered, what protocol you ran, what the radiologist concluded, and what you would do differently.
After a few months, that notebook becomes the most personalized study guide you could possibly have. The cases you saw with your own eyes stick in memory in a way no textbook chapter ever does. Combine that with regular reading of standard references and you will walk into the exam room with both depth and breadth covered.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.