MRI Enterography
MRI enterography guide: what to expect, oral contrast prep, scan time, Crohn disease evaluation, MRE vs CTE, and how to read your report.
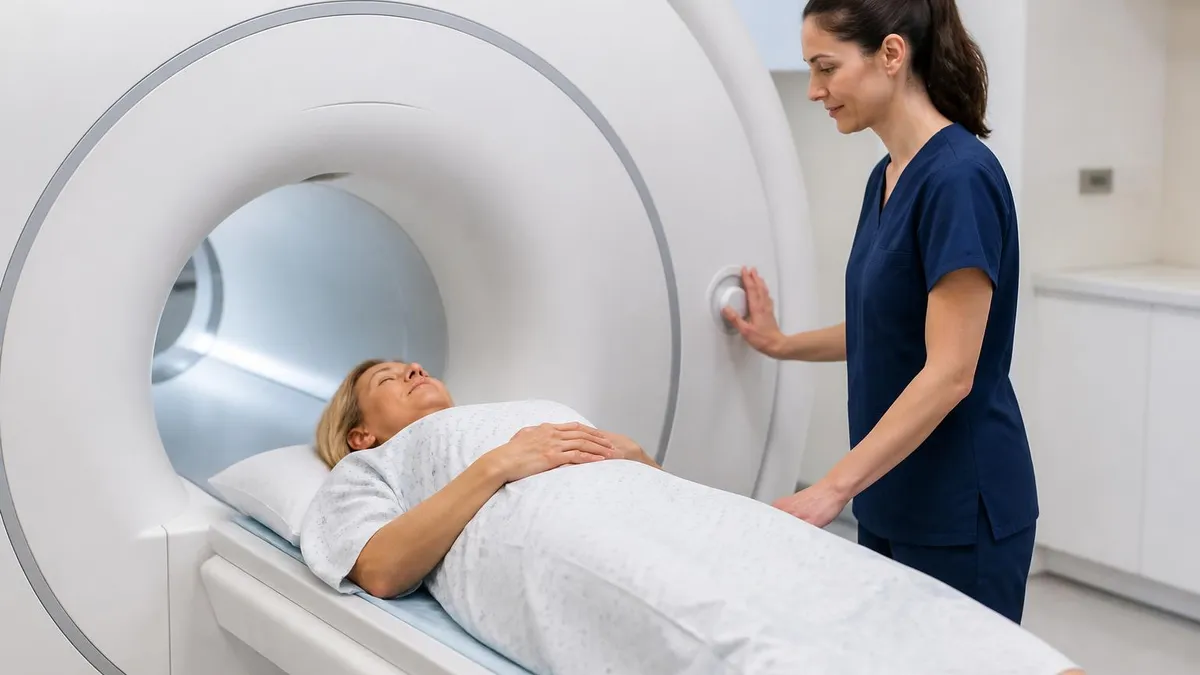
You probably landed here because a gastroenterologist mentioned MRI enterography and you want to know what is coming. Maybe the order says MRE, maybe your referral letter spells it out in full. Either way, the test is more common than most patients realize.
The experience is less intimidating once you know the rhythm of the scan. MRI enterography is a focused study of the small bowel using magnetic resonance imaging, oral contrast, and sometimes intravenous gadolinium. It produces detailed cross-sectional views of the bowel wall, the mesentery, and the surrounding structures without the ionizing radiation associated with CT.
The procedure has grown into one of the most reliable tools for evaluating inflammatory bowel disease, particularly Crohn disease, and for monitoring patients over years rather than weeks. Because Crohn often affects young adults who will face repeated imaging across a lifetime, the absence of radiation matters.
Radiologists, technologists, and gastroenterologists have refined the protocol so that a single ninety-minute appointment can document active inflammation, fibrosis, fistulas, strictures, and extraluminal complications that endoscopy alone cannot see. This guide walks through what the scan shows, how to prepare, and what happens on the table.
MRI Enterography by the Numbers
The numbers above tell you what to expect in broad strokes. A typical appointment runs about ninety minutes door to door, with roughly forty-five minutes spent inside the magnet bore.
The remainder is spent drinking the oral contrast in measured volumes over the preceding hour, changing into a gown, getting an IV line placed, and a short post-scan observation period. Most patients tolerate the procedure well.
The oral contrast can produce a feeling of fullness and, occasionally, transient diarrhea after the exam. Sensitivity figures vary by study and by what radiologists are looking for. For active small bowel inflammation in Crohn disease, modern MRE protocols achieve sensitivity in the high eighties to low nineties and specificity above ninety percent.
These numbers are competitive with CT enterography and superior to most endoscopic approaches when it comes to evaluating the terminal ileum and segments of the small bowel that a colonoscope cannot reach. Penetrating complications such as fistulas, sinus tracts, and abscesses are particularly well demonstrated.
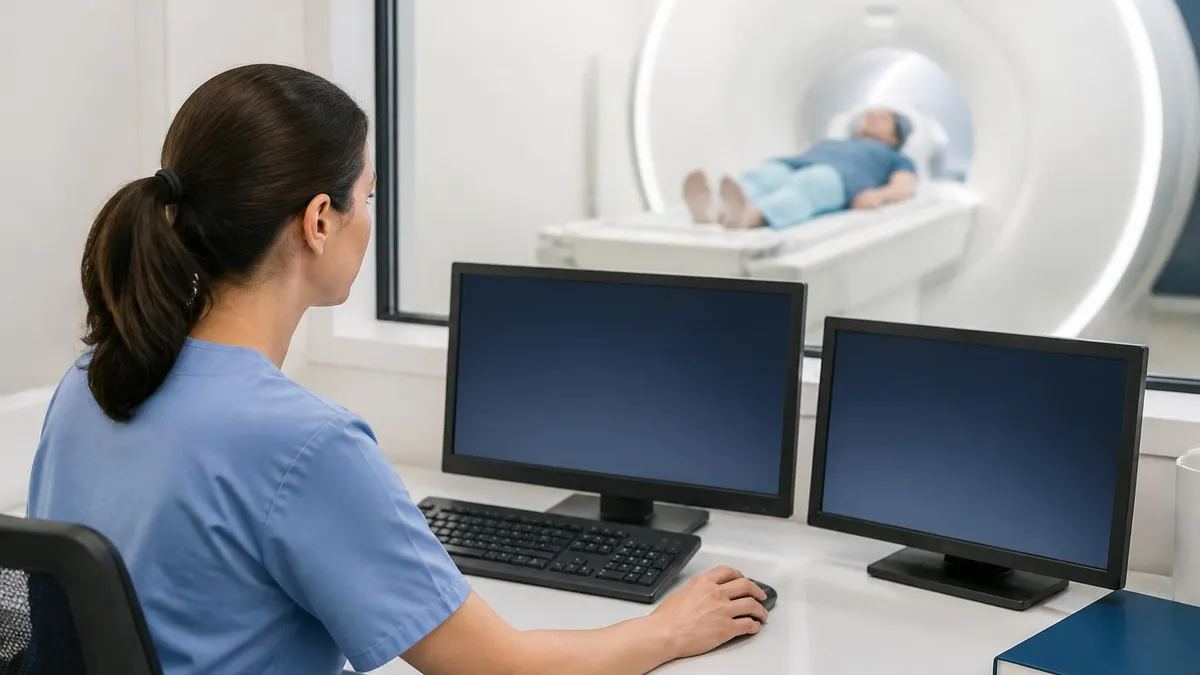
Why Radiation Matters in Crohn Disease
Patients with Crohn disease often need imaging every one to three years for life. Cumulative radiation exposure from repeated CT studies has historically been a concern in this population. MRI enterography removes that variable entirely, which is why most major referral centers have transitioned to MRE as the default cross-sectional study for known or suspected small bowel Crohn.
The trade-off is longer scan time and a more involved preparation, but for a thirty-year-old facing four decades of follow-up imaging, the radiation savings are substantial.
Before we get into the granular protocol, it helps to understand the clinical questions MRE is designed to answer. The test was not developed as a screening tool.
It is requested when a gastroenterologist already suspects small bowel disease and needs anatomic detail that endoscopy, ultrasound, or laboratory work cannot provide. The most common indication is Crohn disease, both at initial diagnosis and during surveillance.
Other indications include unexplained iron deficiency anemia with negative endoscopy, suspected small bowel tumors, evaluation of GI bleeding of obscure origin, polyposis syndromes, celiac disease with atypical features, and surgical planning before bowel resection.
The radiologist reading your scan is looking at several layers at once. The bowel wall thickness, the pattern of mucosal enhancement, the appearance of the mesentery, the presence or absence of lymph nodes, and the configuration of any narrowed segments all factor into the report.
Newer protocols also include diffusion-weighted imaging, which highlights areas of restricted water movement that often correspond to active inflammation. Cine sequences, captured as short movie loops, show how the bowel contracts and whether a strictured segment moves normally or remains rigid.
What the Scan Evaluates
Thickness, enhancement pattern, ulceration, and edema are mapped across every small bowel segment from duodenum to terminal ileum.
Fat stranding, fibrofatty proliferation, vascular engorgement called the comb sign, and reactive lymph nodes are all visible.
Fistulas, sinus tracts, phlegmons, and abscesses appear with high contrast against well-distended bowel loops.
Narrowed segments are measured, characterized as inflammatory or fibrotic, and assessed for upstream dilation.
Preparation begins the day before. Most centers ask you to eat a low-residue diet for twenty-four to forty-eight hours leading up to the appointment, then to fast for four to six hours before arrival.
Fasting matters because food in the small bowel competes with the oral contrast for visibility, and a stomach full of breakfast will produce streaks and motion artifact. Water sips are usually permitted up to two hours before the scan.
Routine medications can be taken with small amounts of water unless specifically restricted by the ordering physician. The oral contrast itself is the part most patients ask about.
Several formulations exist, but they share a common goal: distending the small bowel uniformly so that the entire mucosal surface can be evaluated. The most common agent is a polyethylene glycol solution mixed with mannitol or sorbitol.
It is biphasic, meaning it appears bright on certain sequences and dark on others, which gives the radiologist contrast both with the bowel wall and with the surrounding tissue. You will drink it in three to four portions over roughly an hour.
Some patients ask whether they can sip rather than drink the contrast quickly. The answer is usually no. The radiology team has timed the protocol carefully to ensure the contrast front advances at a predictable rate.
Drinking too slowly leaves the distal ileum collapsed; drinking too fast can cause cramping and incomplete uptake. The technologist will pace you and check in between rounds. If you cannot tolerate the full volume because of nausea or a sensitive stomach, let the team know.
Scan Day Walkthrough
Arrive sixty to ninety minutes before your scheduled scan time. Complete the safety questionnaire covering implanted devices, prior surgeries, and allergies. Change into a gown and remove all metal items including jewelry, hairpins, and watches. The questionnaire is detailed and worth answering carefully — anything ferromagnetic in the bore can become a projectile.
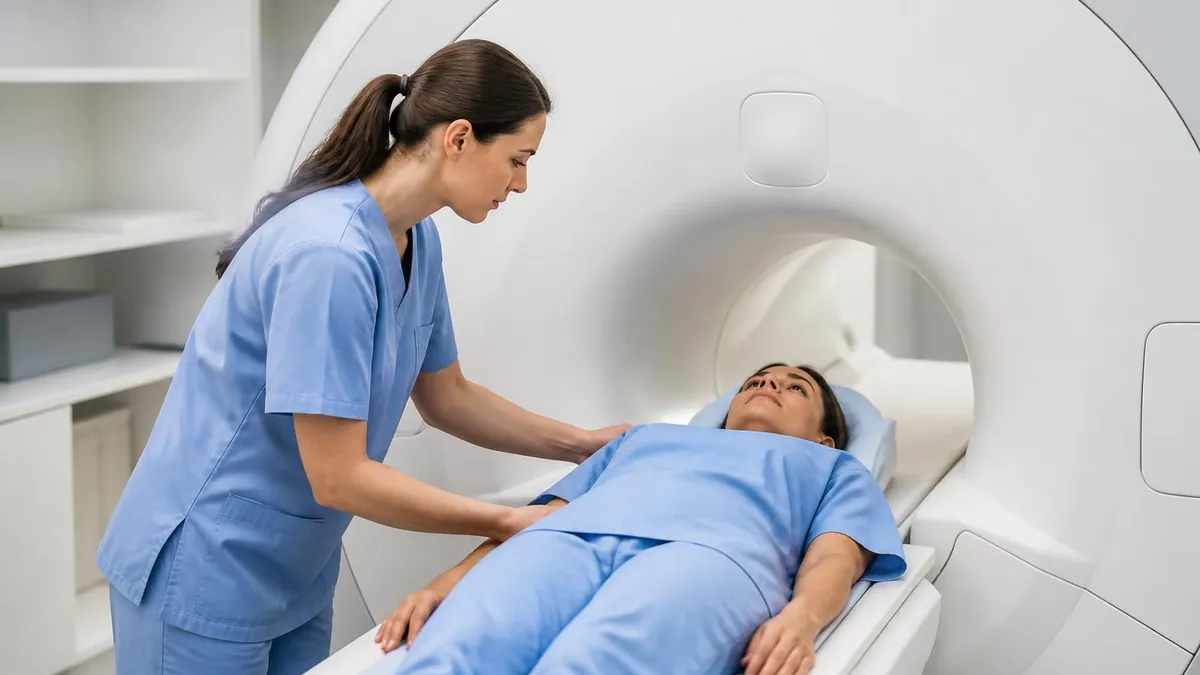
Inside the bore, the technologist will give you a small squeeze ball that triggers an alarm if you need to pause. Most patients find the experience straightforward, although the magnet is loud and the breath-hold instructions can feel relentless during the first ten minutes.
Each breath-hold is brief, usually fifteen to twenty seconds, and the technologist will alternate them with rest periods. If you have claustrophobia, mention this when scheduling.
Many centers offer prone positioning, music through headphones, mirror systems that let you see out of the bore, or mild oral anxiolytics taken before arrival. About halfway through the protocol, the technologist will inject the antispasmodic.
The purpose is to temporarily reduce peristalsis so that the small bowel holds still long enough for high-resolution images. Glucagon and hyoscine butylbromide both work for ten to twenty minutes.
Side effects are uncommon but can include a brief dry mouth, blurred vision, or a sensation of warmth. The gadolinium contrast follows later, usually toward the end of the protocol, and provides the post-contrast images that highlight active inflammation through bright enhancement of thickened bowel walls.
Pacemakers, cochlear implants, aneurysm clips, deep brain stimulators, or any electronic implant. Severe kidney impairment, especially eGFR below 30, which affects gadolinium safety. Pregnancy, particularly the first trimester.
Severe claustrophobia. Recent stomach or bowel surgery. Known iodine or gadolinium contrast reactions. The questionnaire covers all of this, but mention anything unusual directly, even if you think it has already been recorded in your chart.
Once the scan is complete, you can resume normal activities almost immediately. The oral contrast will work its way through your system over the next four to twelve hours, and a brief episode of loose stool is normal.
Drink water afterward to rehydrate and to help flush the gadolinium, which is renally cleared. If you developed nausea during the oral prep, dry crackers and a quiet meal often help. Avoid heavy or greasy food for the rest of the day.
The radiologist reads the study afterward, typically within twenty-four to forty-eight hours at most centers, sometimes the same day at high-volume gastrointestinal practices. The report follows a structured template.
It names each small bowel segment, describes its wall thickness and enhancement, lists any strictures with their length and degree, notes any penetrating disease, and concludes with an impression.
Many institutions now use disease severity scores such as the MaRIA index or the simplified MaRIA for Crohn disease, which give a numerical readout that helps track changes between scans. These scores translate visual findings into reproducible numbers.
Day-Before Preparation Checklist
- ✓Switch to a low-residue diet starting twenty-four hours before
- ✓Stop fiber supplements and avoid raw vegetables, whole grains, and seeds
- ✓Confirm your fasting window with the imaging center (typically four to six hours)
- ✓Continue prescription medications unless explicitly told otherwise
- ✓Arrange a ride if you plan to take an oral anxiolytic
- ✓Wear loose two-piece clothing for easy gowning
- ✓Leave metal jewelry, watches, hairpins, and underwire bras at home
- ✓Bring a list of prior imaging dates and locations for comparison
- ✓Confirm recent kidney function lab results if you have renal disease
- ✓Allow ninety minutes total for the appointment from check-in to checkout
One question that comes up often is the difference between MR enterography and MR enteroclysis. The names sound similar, but the techniques diverge in one important way.
Enterography uses oral contrast that you drink, allowing for gradual bowel distension. Enteroclysis involves placing a tube through the nose or mouth, passing it past the ligament of Treitz, and infusing contrast directly into the jejunum.
Enteroclysis achieves slightly better distension and may detect subtle disease that enterography misses, but the tube placement is uncomfortable for patients and adds time and expertise that not every center can provide.
For routine evaluation of small bowel inflammation, enterography is the modern standard. Enteroclysis is reserved for cases where prior enterography was equivocal or where suspicion of a small focal lesion remains high.
Comparison with CT enterography also comes up frequently. CT remains faster, more widely available, and arguably better at detecting small mesenteric stranding or tiny abscesses because of its higher spatial resolution.
MRI gives superior contrast resolution and avoids radiation. The current consensus from major societies, including the Society of Abdominal Radiology and the European Crohn and Colitis Organisation, is that MRI enterography should be the preferred study for known or suspected Crohn in patients under fifty whenever it is available.
CT remains appropriate in emergency settings, when MRI is contraindicated, or when the suspected pathology requires the fastest possible answer. The choice often comes down to a conversation between gastroenterologist and radiologist.
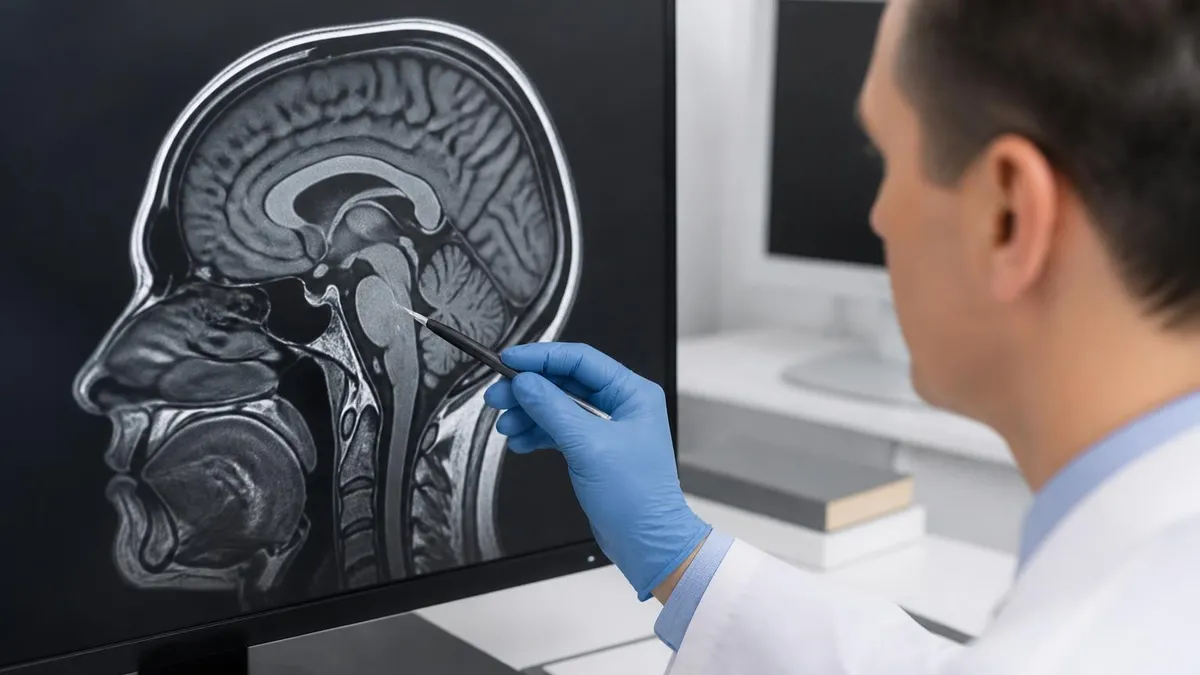
MRE vs CTE
- +No ionizing radiation across a lifetime of follow-up
- +Superior soft-tissue contrast for bowel wall layers
- +Cine imaging captures peristalsis and stricture motion
- +Diffusion-weighted imaging adds inflammation specificity
- +Better characterization of fistulas and sinus tracts
- −Longer scan time, typically forty to sixty minutes
- −Higher cost and limited availability in smaller hospitals
- −Requires patient cooperation with breath-holds
- −Contraindicated with several implanted devices
- −Image quality depends heavily on adequate distension
For patients facing their first MRE, the most useful piece of advice is to ask the imaging center what their protocol expects. Centers vary in the brand of oral contrast they use, the timing of fasting, whether they perform prone or supine imaging, and whether they offer pre-scan anxiolytics.
A two-minute phone call clarifies all of this and removes most of the day-of surprises. If you are a returning patient, request that the new scan be performed on the same magnet field strength as your prior study, ideally 1.5 or 3 Tesla.
This makes comparison images easier to interpret. Subtle changes in wall enhancement or mucosal surface look different across field strengths and across MRI vendors, and a consistent acquisition makes longitudinal monitoring more reliable.
Costs vary widely by country and insurance arrangement. In the United States, MRE typically runs between one thousand and four thousand dollars before insurance, with significant variation between hospital-based and outpatient imaging centers.
In the United Kingdom, the procedure is available through the NHS without direct cost to the patient when indicated by a gastroenterologist. In private healthcare systems across Europe and Asia, MRE is generally covered under standard imaging reimbursement when ordered for inflammatory bowel disease or suspected small bowel pathology.
Always confirm coverage with your insurer before scheduling, particularly for elective indications such as polyposis surveillance. Pre-authorization requirements are common and can delay scheduling by a week or more if not handled in advance.
MRI Questions and Answers
It also helps to understand how the radiologist communicates with your gastroenterologist after the scan. Reports follow a standardized structure that names every small bowel segment in turn: duodenum, proximal jejunum, mid jejunum, distal jejunum, proximal ileum, mid ileum, terminal ileum.
For each segment, the radiologist records wall thickness in millimeters, the pattern of enhancement after gadolinium, the presence of mural edema on T2-weighted sequences, and any abnormal diffusion signal. Strictures are characterized by length, luminal diameter at the narrowest point, the degree of upstream dilation, and whether the narrowing appears predominantly inflammatory or fibrotic.
This distinction matters because inflammatory strictures often respond to medical therapy, while fibrotic strictures may need balloon dilation or surgical resection. The report concludes with an impression that summarizes active versus chronic findings and flags any urgent concerns.
Your gastroenterologist uses this language to adjust your treatment plan. A new active segment may prompt a step up in biologic therapy. A stable picture across two consecutive scans may justify dose spacing or a treatment holiday in selected patients.
Reports follow a standardized template: each small bowel segment is named (duodenum, jejunum, terminal ileum), wall thickness is recorded in millimeters, enhancement pattern after gadolinium is described, and any strictures are measured. The final impression flags active versus chronic findings and any urgent concerns.
Patient experience varies, and a few practical tips help with the day itself. Bring a book, a pair of warm socks, and a light snack for the post-scan window. The waiting area can be chilly and the gowns are thin. Use the restroom right before you start drinking contrast, then again before you enter the magnet room, because the bore is not a place to discover you need a break.
If you have a history of vasovagal episodes with IV placement, mention it so the technologist can have you lie back during the stick. Hydrate well the day before, especially if you have prominent veins on only one arm; a well-hydrated patient is much easier to cannulate.
For follow-up scans, keep a personal log of the date, the facility, the field strength, and any symptoms you had at the time. This becomes invaluable for the radiologist comparing studies a year apart, and it gives you a sense of your own disease trajectory beyond the words in the report.
Day-Of Practical Tips
- ✓Bring a book, warm socks, and a light post-scan snack
- ✓Use the restroom right before drinking contrast, and again before entering the magnet
- ✓Mention any history of vasovagal episodes with IV placement
- ✓Hydrate well the day before for easier cannulation
- ✓Keep a personal log of date, facility, and field strength for future comparisons
- ✓Note any symptoms or flare-ups you had on scan day for the radiologist
MRI enterography sits at the intersection of advanced imaging, gastroenterology, and longitudinal patient care. Done well, it gives a clearer picture of the small bowel than any other non-invasive test, and it does so without the cumulative radiation burden of repeated CT studies.
The preparation feels involved on first encounter, but most patients settle into the routine after the first or second scan and find the experience tolerable. Understanding what each step does, why the oral contrast volume matters, and what the radiologist is looking for in the final report turns the scan from a black box into a clinical conversation.
If you are scheduled for your first MRE, the most useful preparation is also the simplest: follow the diet instructions, arrive on time, communicate openly about any anxiety or device history, and ask your gastroenterologist to walk through the report with you afterward.
Imaging is only one part of the picture in inflammatory bowel disease management. Combined with endoscopy, laboratory markers such as fecal calprotectin and C-reactive protein, and your symptom diary, the MRE findings help guide decisions about medication adjustments, dietary modifications, and surgical planning when needed.
The technology continues to improve, with newer sequences shortening scan time and machine learning tools beginning to assist radiologists in detecting subtle changes between studies.
For now, the protocol described here represents the global standard of care, and the few hours you spend on scan day deliver information that will shape your treatment plan for years to come. Bring questions to your follow-up appointment, ask for a copy of the report, and use the findings as a baseline for the next study.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.