Wound Care Clinic: What to Expect, Who Treats You, and How to Find One Near You
Wound care clinic guide: services, who works there, costs, insurance, what to bring to your first visit, and how to choose one near you.
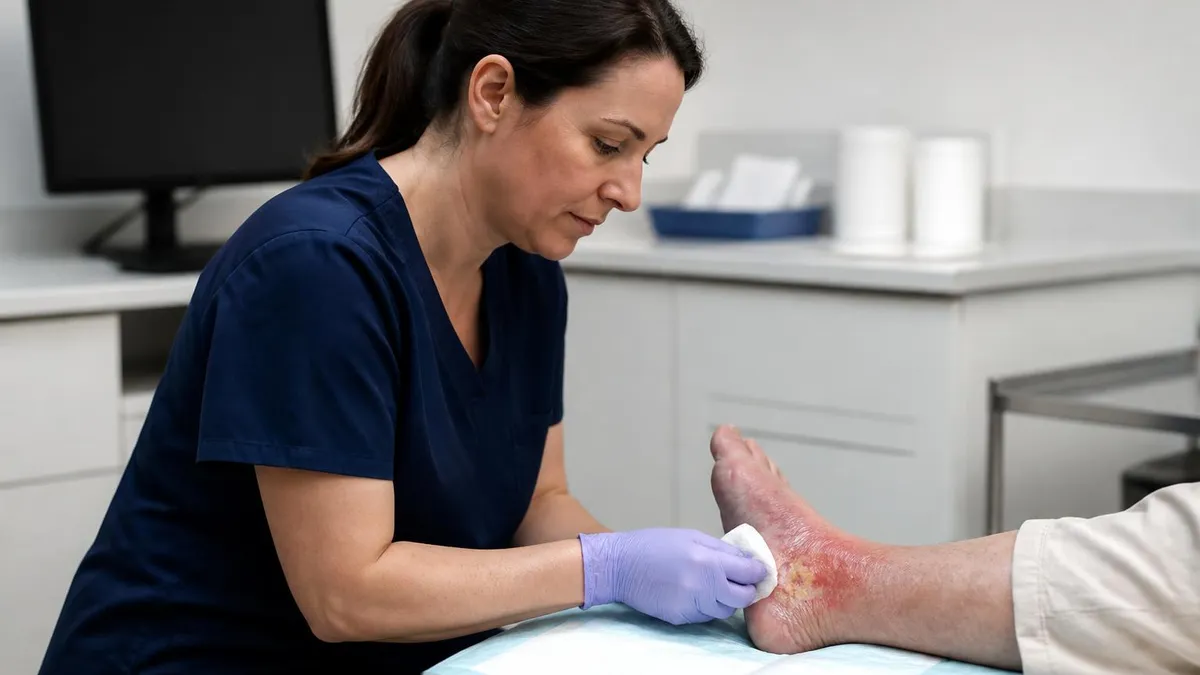
A wound care clinic is a specialty outpatient setting where chronic, non-healing, or complicated wounds get focused treatment that a typical primary-care visit cannot deliver in fifteen minutes. Diabetic foot ulcers. Venous leg ulcers. Surgical wounds that opened back up. Pressure injuries. Skin tears on older adults taking blood thinners. These are the cases that fill the schedule on any given Tuesday, and they need a coordinated plan rather than another tube of antibiotic ointment.
Here is the honest reality. Most people end up at a wound care clinic only after weeks of frustration. They tried at-home dressings. They saw their family doctor. Maybe urgent care. The wound looked the same — or worse. By the time the referral comes through, the tissue is angry, the patient is exhausted, and someone in the household is googling at 11pm whether this is finally an emergency. If that is you, take a breath. Specialty wound centers exist precisely for this stage.
What a wound care clinic actually does differently
Walk into a busy wound care center on a weekday morning and the first thing you notice is the equipment. Sharp debridement at the bedside. Offloading footwear in a closet by the door. A small dressing room that looks more like a pharmacy than a clinic, stacked with foams, alginates, hydrocolloids, silver-impregnated layers, and contact-layer films most family doctors have never opened.
The team plans treatment in weeks, not single visits. They photograph the wound, measure it in millimeters, and trend it. If the surface area has not shrunk by roughly 30 to 50 percent at the four-week mark, the protocol changes. That benchmark — measurable healing trajectory — is the operational heart of the clinic, and it is the thing primary care rarely has the bandwidth to enforce.
Common services on the intake paperwork
The line items vary by center, but most clinics offer wound assessment and staging, sharp and enzymatic debridement, compression therapy for venous disease, negative pressure wound therapy (the vacuum-assisted pump you may have heard called a wound vac), bioengineered skin substitutes, total contact casting for diabetic foot ulcers, and hyperbaric oxygen therapy for select indications. A subset of centers also handle ostomy care, lymphedema bandaging, and post-Mohs surgical follow-up.
The first call to a clinic also tends to reveal how organized the operation is. A front desk that quotes you a same-week appointment, confirms your insurance in one breath, and tells you exactly what to bring is usually attached to a clinic that runs the rest of its workflow with the same discipline. A front desk that puts you on hold for fifteen minutes and then says someone will call back is its own warning.
Some centers bill as hospital outpatient departments, which means a higher facility fee but also direct access to imaging, vascular consults, and admission pathways if a wound infection turns systemic. Other centers are physician-owned freestanding clinics with leaner overhead and often more flexible scheduling. Neither model is inherently better — the question is which one fits your wound type, your insurance, and your travel tolerance.
Wound Care Clinic At a Glance
Trigger for referral. If a wound has not visibly shrunk after two weeks of competent at-home care, or it has been present for more than four weeks, request a wound care clinic referral. Many clinics accept self-referrals — you do not need to wait for primary care to act. Bring photos, dressing names, your A1C if diabetic, and any prior wound history.
The staff mix at a wound care clinic surprises first-time patients. You may meet a podiatrist on Monday, a general surgeon on Wednesday, and an APRN-led visit on Friday. Internists with wound fellowships. Plastic surgeons doing skin graft follow-up. The connective thread is the certified wound care nurse — the person who knows your dressing change schedule by heart and will catch the early signs of infection before the physician walks in.
Certification matters more than people realize. A wound care certification proves the clinician has been tested on staging, biofilm management, advanced dressings, and offloading principles — not just absorbed them from on-the-job experience. If you are evaluating a clinic, ask whether the nurses are WOCNCB or NAWCO certified. The good clinics will tell you proudly. The mediocre ones will fumble the question.
The first visit: what happens and what to bring
Bring the wound history. Not just "it started in March." Bring the dates of any debridement you have already had. Bring the dressings — actual product names, not just "the white one." Bring a current medication list, including supplements, because vitamin C, zinc, and protein status all influence healing. If you have diabetes, bring your most recent A1C. If venous disease is suspected, bring your most recent duplex study.
The clinical workflow is fairly consistent across centers. Vitals first. Then a focused wound exam: location, size in three dimensions, exudate volume and character, surrounding skin condition, presence of tunneling or undermining, and pain. The clinic photographs the wound against a sterile ruler. You will hear words like granulation, slough, and eschar — these refer to the tissue types in and around the wound bed.
Then the plan. Debridement may happen at that first visit if the wound bed needs it. Compression may be applied before you leave. A follow-up cadence is set, usually weekly to start. If the clinic has access to advanced therapies, you will be told which ones are on the table and which insurance is likely to authorize. Expect the visit to run 45 to 90 minutes the first time. Subsequent visits are shorter.
Patients sometimes feel ambushed by the photography. The clinic is not collecting souvenirs — those photographs are the legal and clinical record of trajectory. Some payers will not authorize advanced therapies without proof that the wound failed standard care over four weeks. Photographs are that proof. Get used to seeing your wound on a screen. The team will explain what each piece of tissue tells them.
A note on emotional pacing. Many patients walk in expecting a magic dressing that closes the wound by Friday. The real work is incremental. Better dressings buy you a percent of healing per week. Better offloading buys you another percent. Better glucose control buys you another. Stack the gains. The number that matters is the four-week reassessment, not the daily appearance of the dressing pad.
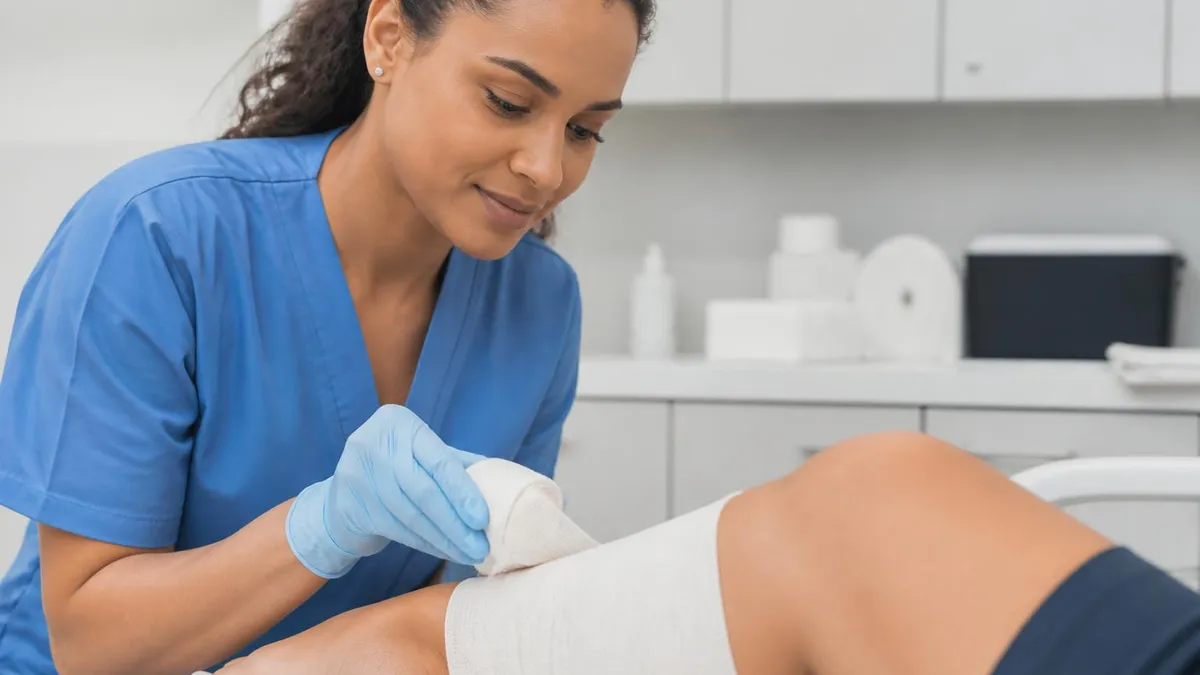
Conditions Wound Clinics Treat Most
Offloading with total contact casting, regular debridement, vascular workup, infection control.
Multilayer compression bandaging, dressing matched to exudate, lifelong stocking transition.
Staging, pressure redistribution, nutrition review, dressing strategy by stage.
Negative pressure wound therapy, closure planning, infection rule-out with culture.
Contact layers, antimicrobials, bioengineered skin substitutes when indicated.
Hyperbaric oxygen therapy for approved late-effect indications such as radiation cystitis or osteoradionecrosis.
Inside the First Wound Clinic Visit
Wound history with dates of any prior debridement. Current dressing product names. Full medication list including supplements. Recent A1C if diabetic. Venous duplex report if available. List of allergies — especially silver, latex, and adhesives. Photos taken at home over the past two to three weeks help the clinic see the trajectory.
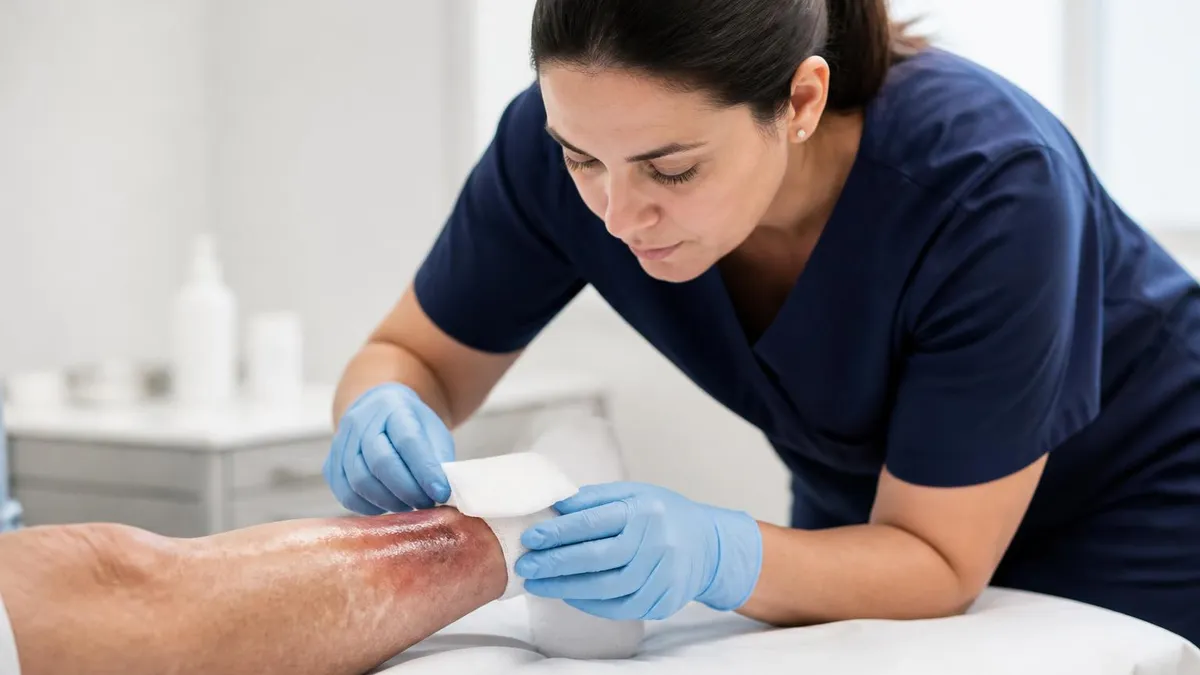
Diabetic foot ulcers deserve their own paragraph because they account for the lion's share of preventable amputations. A wound care clinic treating one should be doing three things at minimum: offloading (total contact casting or a removable cast walker), regular sharp debridement, and vascular workup if there is any pulse abnormality. Add infection workup with deep tissue culture when indicated. Miss any of these and the outcome curve bends the wrong way.
Venous leg ulcers heal when you address the underlying venous hypertension. That means compression — usually a multilayer bandaging system applied at the clinic and worn until the next visit. Without compression, no dressing in the world reliably closes a venous ulcer. With compression, even old ulcers often start trending closed within four to six weeks. Patients struggle with the heat and weight, but adherence drives outcomes.
Why dressing choice is more complicated than it looks
Most wounds need a moisture balance, not bone-dry sterility. The right wound care dressings match exudate level: alginates and foams for heavy exudate, hydrocolloids for low-to-moderate, hydrogels for dry beds that need rehydration, and contact layers for fragile granulation tissue you do not want to disturb. A clinic chooses the dressing based on what the bed is telling them today, not what worked last month.
That responsiveness is also why varied wound care products exposure matters. Outpatient centers see more variety in a week than primary care sees in a year. They know which silver dressings cause maceration. They know which collagen products absorb best in venous wounds. They have an opinion on antimicrobial honey dressings versus cadexomer iodine for biofilm-heavy wounds, and the opinion is rooted in cases, not catalog reading.
Pressure injuries — what older clinical training called pressure ulcers — are the third great category that fills the wound care clinic schedule. They are usually a system failure, not a skin failure. The patient has been immobile, undernourished, or both. A clinic working a stage three sacral pressure injury will be coordinating with home health for pressure redistribution surfaces, with dietitians for protein and vitamin C, and with the family for repositioning schedules. The dressing is the small visible piece of a larger plan.
Surgical dehiscence — wounds that opened back up after a procedure — get triaged differently. The clinic verifies that there is no abscess hiding underneath, takes culture if there is doubt, and almost always reaches for negative pressure wound therapy to close the wound from the bottom up. The patient usually leaves with a portable pump and a teaching session on canister changes and alarm sounds. These wounds tend to do well with a clinic team that owns the pump rental relationship and can replace dressings rapidly.
Go to the emergency department for active heavy bleeding, fever above 101F with limb redness, red streaks tracking up the limb, sudden severe pain with skin color change, or new black tissue with foul odor. Sepsis and necrotizing soft tissue infections move quickly — these are not clinic-hours problems. Call 911 if the patient is confused, hypotensive, or has rapid breathing.
First-Visit Prep Checklist
- ✓Wound photos taken at home over the past 2-3 weeks
- ✓Names of every dressing you have used (not just colors)
- ✓Updated medication list including OTC and supplements
- ✓Most recent labs — A1C, albumin, prealbumin if available
- ✓Insurance card and any prior authorization paperwork
- ✓Ride home arranged in case debridement is needed
- ✓Comfortable, loose clothing over the wound area
- ✓Written list of questions so nothing gets forgotten
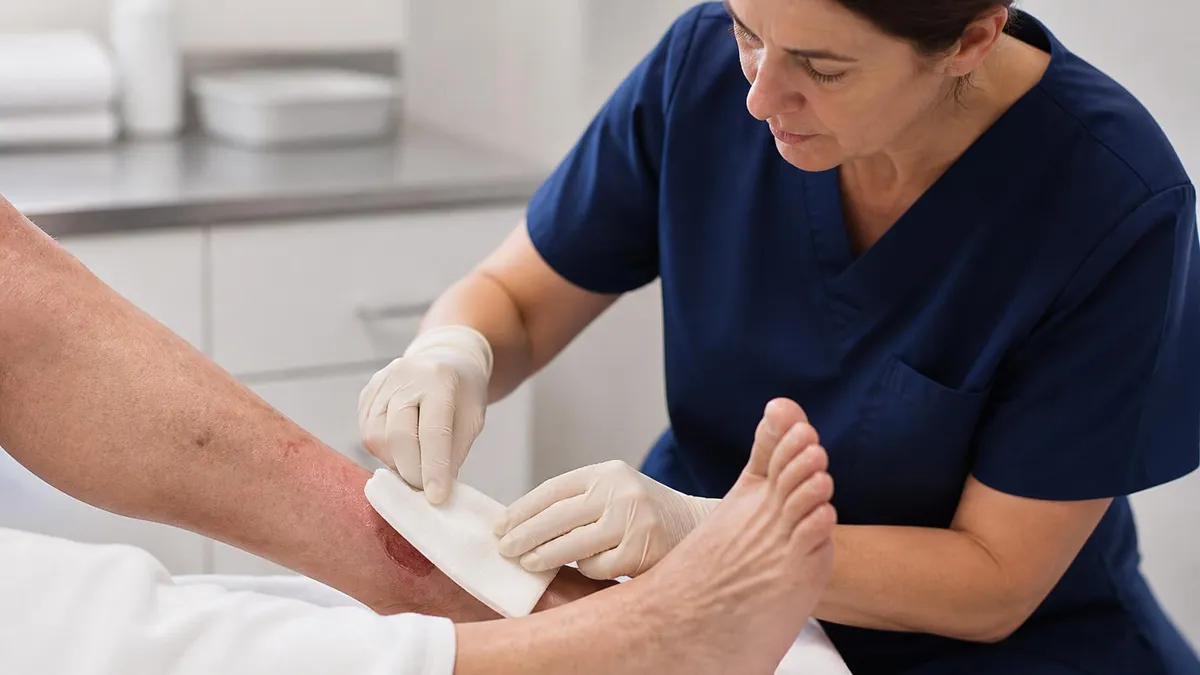
Costs at a wound care clinic depend on three factors: the procedures performed, the dressings supplied, and the facility billing status (hospital outpatient department versus freestanding clinic). A single visit with basic debridement and dressing change can run from $150 to $600 out of pocket without insurance. Advanced therapies — hyperbaric oxygen, bioengineered skin substitutes, prolonged negative pressure rentals — push costs into four-figure territory per session.
Medicare covers most wound care services when documented as medically necessary. Commercial insurance is more variable; some plans require prior authorization for hyperbaric, skin substitutes, and extended NPWT rentals. The billing team usually pulls authorization before scheduling those services, which is part of the reason your first visit may feel administrative. If you are uninsured, ask about charity care or sliding-scale fees — many hospital-based wound centers have programs they do not advertise.
Wound clinic vs ER vs primary care
The ER is for active bleeding, fever with redness streaking up a limb, suspected sepsis, or sudden severe pain with discoloration. Primary care is for the first 7 to 14 days of a small acute wound that is healing on its own trajectory. A specialty clinic is for everything in between — and for any wound that has been around for more than four weeks without clear improvement.
One quiet rule from inside the field: if a wound has not visibly shrunk in two weeks of competent home care, escalate. Do not wait for someone to refer you. Many wound centers accept self-referrals or PCP referrals interchangeably. A phone call is cheaper than another month of stalled healing.
Hyperbaric oxygen therapy is overused in some marketing and underused in some clinical situations. Medicare-approved indications include diabetic foot ulcers (Wagner grade 3 or higher), late effects of radiation, chronic osteomyelitis, and a handful of others. For those indications, oxygen at pressure improves outcomes. Outside those indications, the evidence thins quickly. Ask your wound care clinic which specific indication they are billing under before agreeing to a 40-session protocol — it is your right to know.
Hospital-Based Wound Center vs Freestanding Clinic
- +Hospital centers usually have hyperbaric chambers and advanced imaging on-site
- +Easier specialist consults — vascular, infectious disease, plastics — under one roof
- +Charity care and financial assistance programs more commonly available
- +Stronger payer relationships for advanced therapy authorization
- +Direct admission pathway if a wound infection turns systemic
- −Freestanding clinics often have shorter wait times for new patient appointments
- −Hospital facility fees can push per-visit costs noticeably higher
- −Parking and walking distance can be tough for mobility-limited patients
- −Freestanding clinics may offer more flexible scheduling and longer visits
- −Smaller clinics sometimes know patients more personally over months of care
Two wound care clinics in the same metro can have dramatically different healing rates. The drivers are case-mix transparency, photographic documentation discipline, debridement frequency, willingness to escalate, and depth of payer relationships. Clinics that publish their own outcomes data tend to be the ones with results worth publishing. Clinics that hide behind anecdote tend to drift.
For patients, the practical takeaway is to ask outcome questions on the first call. What is your average time to closure for venous ulcers? How often do you photograph wounds? Who reviews my chart if the lead clinician is out? A clinic that answers cleanly is a clinic that has thought about its own work.
Working in wound care — a brief note for clinicians
If you are a nurse reading this with an eye on specializing, the path is well-marked. Two to three years of medical-surgical or home health experience. A board exam — WCC, CWCN, or CWS. A portfolio of complex cases. Outpatient centers, hospital-based wound services, and home health agencies are the three main employers. Compensation tends to run above general bedside nursing because of the specialized skill base. Our notes on wound care clinic cover the market in more detail.
Studying for the boards is a structured project. Practice questions help more than passive reading. Pair them with hands-on case exposure and you will be ready when the exam day comes. The broader picture sits inside our wound care overview for anyone wanting a clinical refresher.
One last thought for patients. A wound is healed when the epithelium is fully closed and intact for two weeks under normal activity. Premature discharge is a common reason wounds recur. A good clinic will keep you on the schedule, even at less frequent intervals, until that two-week intact mark is reached, and then transition you to maintenance — skin care, offloading, compression stockings, A1C control, whatever the underlying driver was. Healing is a phase. Maintenance is the rest of your life with that limb or that pressure point.
If you take only one thing from this guide, take this: the right wound care clinic does not just dress the wound — it builds a plan that closes it, then it builds a plan that keeps it closed. Find one near you. Bring the full history. Show up to every appointment, even when the wound looks small. The first visit usually is the moment the trajectory starts to bend in the right direction, and the last visit is the one that tells you which boring habits will keep you out of trouble for the next twenty years.
Wound Care Clinic Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.