Wound Care: Types, Dressings, Certification & Nurse Guide
Complete wound care guide covering wound types, dressing products, ICD-10 coding, wound care nurse roles, and WCC certification requirements.
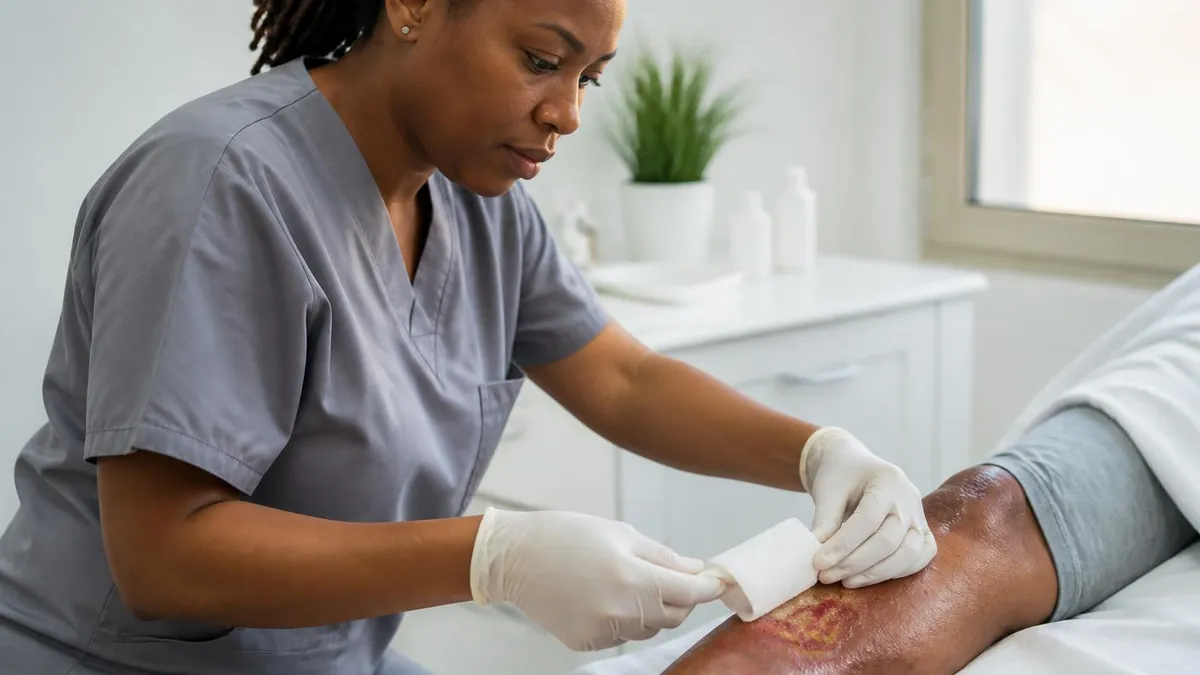
Wound Care at a Glance
What Is Wound Care?
Wound care is the clinical practice of assessing, treating, and managing wounds to promote healing, prevent infection, and minimize complications. It encompasses everything from basic first-aid management of acute cuts and lacerations to highly specialized chronic wound treatment for pressure injuries, diabetic foot ulcers, and venous leg ulcers. In clinical settings, wound care is a recognized clinical specialty with its own certification pathways, dedicated clinics, and evidence-based protocols.
Wounds are classified as either acute or chronic. Acute wounds — surgical incisions, traumatic lacerations, abrasions, burns — follow a predictable healing timeline and typically resolve within weeks with appropriate treatment. Chronic wounds are those that fail to progress through normal healing stages within three months. They include pressure injuries (formerly called bedsores or decubitus ulcers), diabetic foot wounds, venous ulcers, and arterial ulcers. Chronic wounds affect an estimated 6.7 million Americans and account for a disproportionate share of healthcare costs, hospital readmissions, and quality-of-life burden.
The wound healing process follows four overlapping phases: hemostasis (bleeding stops), inflammation (immune response begins), proliferation (new tissue forms), and remodeling (scar tissue matures). Wound care interventions are designed to support each phase — maintaining moisture balance, managing bioburden (bacterial load), protecting the wound from further trauma, and addressing the underlying conditions that impair healing. Understanding these phases is foundational for anyone pursuing a wound care certification or working in wound management.
Types of Wounds and How They're Classified
Wound classification drives treatment decisions. Clinical systems for wound classification range from simple acute/chronic distinctions to detailed staging systems that guide everything from dressing selection to reimbursement coding.
Pressure injuries are staged using the National Pressure Injury Advisory Panel (NPIAP) system: Stage 1 (non-blanchable skin discoloration, no open wound), Stage 2 (partial-thickness loss involving the epidermis and/or dermis), Stage 3 (full-thickness loss through the dermis into subcutaneous tissue), Stage 4 (full-thickness loss with exposed bone, tendon, or muscle), Unstageable (base obscured by slough or eschar), and Deep Tissue Pressure Injury (intact skin with deep tissue damage). This staging system is tested on all major wound care certification exams.
Diabetic foot wounds use the Wagner Classification (Grade 0–5) or the University of Texas Wound Classification System, which layers wound depth with the presence of infection and ischemia — factors that significantly affect healing prognosis and treatment intensity. Peripheral neuropathy is the dominant underlying cause: patients can't feel wound development, which allows small abrasions to progress to deep wounds before they're detected.
Venous leg ulcers typically occur on the medial lower leg and are associated with chronic venous insufficiency. They're characterized by irregular wound margins, moderate-to-heavy exudate, and the presence of hemosiderin staining (brown discoloration) in the surrounding skin. Compression therapy is the cornerstone of venous ulcer management — without addressing venous hypertension, wound healing stalls regardless of dressing choice.
Arterial ulcers are caused by inadequate arterial perfusion. They typically appear on the toes, heels, and lateral lower leg, present as pale and well-defined wounds with minimal exudate, and are associated with rest pain and absent peripheral pulses. Compression is contraindicated in arterial wounds. Vascular surgical consultation is often required before wound closure is achievable.
Not every wound can be healed — some chronic wounds in patients with severe arterial disease, end-stage renal failure, or terminal illness are managed for comfort rather than closure. Goals of care conversations are part of wound care practice. On certification exams, understanding the difference between curative wound care (aiming for closure) and palliative wound management (controlling pain, odor, and infection without expecting closure) reflects advanced clinical judgment.
The Wound Healing Process: Four Phases
Wound healing follows a predictable biological sequence that clinicians must understand to support — and recognize when it's going wrong. The four phases overlap and influence each other, and any disruption can stall the entire process.
Phase 1: Hemostasis begins the moment a wound occurs. Blood vessels constrict, platelets aggregate to form a clot, and the coagulation cascade creates a fibrin mesh that seals the bleeding site. This phase is complete within minutes for most wounds. The fibrin clot also serves as a scaffold for subsequent cellular activity. Patients on anticoagulants or with platelet disorders have impaired hemostasis, which affects both clotting speed and the structural foundation for the next phases.
Phase 2: Inflammation begins immediately after hemostasis and lasts four to six days in an acute wound. White blood cells — neutrophils first, then macrophages — flood the wound site to destroy bacteria, clear debris, and release growth factors that signal the next phase. Inflammation is essential. The redness, warmth, swelling, and pain of early wound healing are signs of normal biological activity, not infection. Chronic wounds often get stuck in the inflammatory phase — persistent inflammation prevents progression to tissue rebuilding, which is why managing bioburden and inflammatory mediators is central to chronic wound treatment.
Phase 3: Proliferation is where rebuilding happens. Fibroblasts produce collagen to form granulation tissue — the red, bumpy, vascular tissue that fills the wound bed. Epithelial cells migrate from the wound edges and any residual hair follicles to cover the granulation tissue surface. This phase lasts two to three weeks in acute wounds. Moisture balance is critical here: wounds that are too dry develop eschar that blocks epithelial migration; wounds that are overly wet develop maceration that damages periwound skin. Appropriate dressing selection directly supports or impairs the proliferative phase.
Phase 4: Remodeling begins around three weeks after injury and continues for up to two years. The initial Type III collagen is replaced by stronger Type I collagen, the scar tissue reorganizes along lines of mechanical stress, and the wound contracts. The fully healed wound regains approximately 80% of its original tensile strength — never quite 100%. Hypertrophic scarring and keloid formation occur when the remodeling phase is dysregulated, particularly in patients with certain skin types or genetic predispositions.
Understanding wound healing phases is foundational knowledge for all wound care certification exams — questions on expected timelines, phase-specific interventions, and signs of stalled healing appear consistently across WCC, CWCN, and CWS certification tests.
Wound Care Dressings and Products
Water-based gel dressings that maintain a moist wound environment and provide cooling, soothing relief. Indicated for dry-to-lightly exuding wounds, necrotic wounds requiring autolytic debridement, and radiation skin reactions. Available in sheet and amorphous (tube) forms. KD:16 — highly searched by nursing staff selecting dressings for wound beds.
Adhesive dressings containing gel-forming agents (carboxymethylcellulose) that absorb exudate and create a moist healing environment. Self-adhesive and waterproof. Appropriate for partial-thickness wounds with light-to-moderate exudate, Stage 2 pressure injuries, and minor burns. Not appropriate for infected wounds, high-exudate wounds, or wounds with sinus tracts.
Highly absorbent dressings derived from seaweed. Form a gel when in contact with wound exudate, maintaining moisture balance in heavily draining wounds. Indicated for moderate-to-heavily exuding wounds, infected wounds (when used with antimicrobials), and cavity wounds. Require secondary dressings to hold in place.
Polyurethane foam dressings with high absorbent capacity. Available in adhesive and non-adhesive forms. Indicated for moderate-to-heavily exuding wounds, diabetic foot ulcers, and pressure injuries. Protect wound from shear and pressure forces while managing exudate. Replace as needed based on exudate level.
Dressings impregnated with silver, iodine, PHMB, or other antimicrobials for wounds with critical colonization or confirmed infection. Silver dressings are most common. Reduce bioburden without systemic antibiotic exposure. Not appropriate as first-line dressings for all wounds — reserve for infections or high-risk patients.
Normal saline (0.9% NaCl) is the gold-standard wound cleansing solution. Gentle irrigation removes surface debris, slough, and wound exudate without damaging granulation tissue. Tap water is acceptable for many acute wounds in community settings. Avoid hydrogen peroxide and povidone-iodine in open wounds — both are cytotoxic to healing tissue.
Wound Care Nurse: Role and Responsibilities
A wound care nurse — formally called a wound, ostomy, and continence (WOC) nurse, or a wound care specialist depending on the practice scope — is a registered nurse with advanced training in wound assessment, treatment planning, patient education, and care coordination for complex wound patients. It's one of the most clinically demanding nursing specialties, requiring both detailed medical knowledge and strong patient communication skills.
Day-to-day responsibilities of a wound care nurse include: comprehensive wound assessment (measuring dimensions, staging, documenting wound bed characteristics and periwound skin), developing individualized wound care plans based on wound type and patient health status, selecting and applying appropriate dressings, performing or coordinating debridement, educating patients and caregivers on home wound management, coordinating with physicians, physical therapists, and nutritionists for complex cases, and documenting wound progress using standardized tools.
Wound care nurses work across multiple settings — acute care hospitals, long-term care facilities, outpatient wound clinics, home health agencies, and hyperbaric oxygen therapy centers. In hospital settings, wound care nurses often serve as consultants, seeing complex wound patients referred from other units and providing documentation support for quality metrics related to hospital-acquired pressure injuries. In outpatient clinics, they often function as the primary clinician managing chronic wound patients over weeks or months of ongoing treatment.
Nutritional support is an underappreciated component of wound care that wound nurses must address. Protein deficiency impairs collagen synthesis; zinc and vitamin C deficiencies slow wound healing; dehydration reduces tissue perfusion. Wound nurses routinely assess nutritional status, refer patients to dietitians, and document nutrition-related barriers to healing. This knowledge is directly tested on wound care certification exams.
The scope of practice varies by state and employer. Some wound care nurses perform sharp debridement independently; others require physician orders. Understanding what falls within your scope — and when to escalate to a physician or specialist — is a core competency in wound care nursing. The WCC and CWCN certification exams both include scope-of-practice content specifically because it varies enough across settings to warrant standardized testing.

Wound Care by Specialty Area
Types of Wound Debridement
Debridement — removing necrotic tissue, slough, and debris from the wound bed — is one of the most important wound care interventions. Non-viable tissue prevents healing and creates an environment that supports bacterial overgrowth. The type of debridement selected depends on wound characteristics, patient factors, and clinician scope of practice.
- Autolytic debridement: Uses the body's own moisture and enzymes under an occlusive dressing. Slow but appropriate for non-infected wounds in patients who can't tolerate more aggressive approaches
- Enzymatic debridement: Topical agents (collagenase) selectively break down necrotic tissue. Requires prescription; useful when autolytic debridement is insufficient
- Mechanical debridement: Wet-to-dry dressings, wound irrigation, hydrotherapy. Broad-spectrum removal — removes both necrotic and viable tissue, so has largely fallen out of favor except for specific uses
- Sharp/surgical debridement: Fastest and most selective removal using scalpel, scissors, or curette. Most effective for thick eschar and devitalized tissue; requires specific training and scope of practice authorization
- Maggot therapy (biosurgical debridement): Sterile larvae consume only necrotic tissue with high selectivity. Used for wounds that have failed other debridement approaches
Wound Care Certification: WCC, CWCN & CWS
Wound care certification validates specialized clinical competency beyond baseline RN or LPN licensure. There are three primary certification pathways in the US, each with different scope and requirements.
The WCC (Wound Care Certified) credential is offered by the National Alliance of Wound Care and Ostomy (NAWCO). It's open to registered nurses, licensed practical nurses, and other licensed healthcare professionals with at least 120 hours of supervised wound care experience. The exam tests wound assessment, wound bed preparation, dressing selection, debridement, infection management, and documentation. The WCC is one of the most commonly held wound care credentials in acute care and long-term care settings.
The CWCN (Certified Wound Care Nurse) is offered by the Wound, Ostomy and Continence Nursing Certification Board (WOCNCB). It requires an active RN license and completion of an accredited WOCN education program or 50 or more hours of wound care education plus 1,500 hours of wound care clinical experience within the past five years. The CWCN exam is generally considered more rigorous than the WCC and is the preferred credential for advanced wound clinic and WOC nursing roles.
The CWS (Certified Wound Specialist) from the American Board of Wound Management (ABWM) is open to a broader range of licensed clinicians including physicians, NPs, PAs, and RNs. It emphasizes evidence-based wound management across all wound types and is structured for clinicians with more extensive wound care experience in specialized settings.
All three certifications require ongoing continuing education for renewal — typically every five years. CE requirements aren't just a formality: wound care evidence evolves rapidly. Updated dressing categories, revised staging systems, new debridement technologies, and changes in reimbursement coding mean that clinicians who don't maintain current knowledge quickly fall behind clinical standards. Renewal CE requirements include wound-specific content: new evidence on dressing materials, advances in debridement techniques, updates to wound staging systems, and changes in reimbursement and documentation standards. Wound care is a rapidly evolving field, and certification renewal requirements reflect the pace of change in clinical best practices.
For nurses considering the certification path, it's worth understanding what exam-specific content is tested before choosing a preparation approach. The WCC exam specifically tests NPIAP staging, wound assessment parameters, dressing product categories and indications, debridement types, infection signs, and the TIME wound bed preparation framework (Tissue, Infection/Inflammation, Moisture, Edge). Use the official NAWCO content outline as your study guide framework, and supplement with wound care practice questions that mirror the format of the actual certification exam. Candidates who practice with exam-formatted questions consistently outperform those who only review reading material.
1. Memorize the NPIAP pressure injury stages — stage descriptions, what's visible, and what's NOT present (Stage 1 has no open wound; Unstageable is not Stage 4). 2. Know dressing indications by exudate level — dry wound → hydrogel; light exudate → hydrocolloid; moderate–heavy exudate → alginate or foam. 3. Understand the TIME framework — Tissue, Infection/Inflammation, Moisture, Edge. It structures the entire wound bed preparation approach and appears across every WCC question category. Use our wound care practice test to drill these before your exam.
Wound Infection and Bioburden Management
Every wound contains bacteria — the clinical question isn't whether bacteria are present, but how many and what kind. The wound bioburden continuum ranges from contamination (bacteria present but not multiplying in wound tissue) to colonization (bacteria present and multiplying but not causing tissue damage) to critical colonization (bacterial load impairs healing without classic systemic infection signs) to infection (bacteria invade surrounding tissue, cause host response, and require intervention).
Recognizing where a wound falls on this continuum determines treatment. Most wounds in colonization don't require antimicrobial treatment — just optimal wound care. Critical colonization shows as stalled healing, increased exudate, discoloration of the granulation tissue, or a distinctive wound odor without the classic local infection signs (erythema, warmth, purulent drainage). Topical antimicrobials — silver dressings, iodine-based products, PHMB — are appropriate for critical colonization. Wound infection with spreading cellulitis, systemic signs (fever, elevated WBC), or osteomyelitis requires systemic antibiotics and often surgical debridement.
Biofilm is a major complication in chronic wounds. Biofilm is a structured community of microorganisms embedded in a protective polysaccharide matrix that adheres to the wound surface. Biofilm bacteria are dramatically more resistant to antibiotics and topical antimicrobials than planktonic (free-floating) bacteria — the biofilm matrix physically blocks penetration of antimicrobial agents. Signs of biofilm include: wounds that appear to stall despite appropriate care, recurrent signs of infection after antibiotics are stopped, and a slippery, shiny film on the wound surface.
Biofilm management requires repeated mechanical disruption — debridement breaks up the matrix and exposes bacteria to treatment. Research-based biofilm protocols combine sharp or mechanical debridement, antimicrobial wound dressings, wound cleansing at each dressing change, and addressing the systemic factors (blood glucose, oxygenation, nutritional status) that support bacterial proliferation. This is why chronic wound management isn't just about choosing the right dressing — it requires systematic, consistent biofilm reduction as a parallel strategy alongside tissue management and moisture balance.
Wound cultures have specific indications and limitations. Surface swab cultures identify surface bacteria but may not reflect the organisms actually causing tissue infection. Quantitative tissue biopsy (greater than 10^5 organisms per gram of tissue = critical colonization/infection threshold) is more accurate but rarely performed outside research or specialist settings. Bone biopsy is the gold standard for suspected osteomyelitis — imaging findings alone are insufficient for diagnosis. When ordering or interpreting wound cultures, understanding what the culture method reflects helps contextualize results and avoid over-treating colonized wounds with systemic antibiotics.
Pain management is another dimension of wound care that's often under-addressed. Procedural pain during dressing changes is one of the most common reasons patients delay or avoid wound care — leading to longer healing times and increased infection risk. Topical lidocaine-impregnated dressings, pre-medication before dressing changes, and using non-adherent dressings that minimize trauma on removal are all strategies wound care nurses use. Assessing and documenting wound-related pain at every visit is part of comprehensive wound assessment and reflects the holistic approach that distinguishes skilled wound care from purely mechanical dressing application.
- ✓Wound location: specific anatomical site with laterality (right, left)
- ✓Wound dimensions: length × width × depth in centimeters
- ✓Wound stage or classification (NPIAP stage, Wagner grade, etc.)
- ✓Wound bed appearance: percentage of granulation, slough, necrosis, eschar
- ✓Exudate: amount (none/minimal/moderate/heavy) and character (serous, serosanguineous, purulent)
- ✓Wound edges: defined/undefined, rolled, undermined, attached to wound base
- ✓Periwound skin: maceration, erythema, induration, excoriation, hemosiderin staining
- ✓Odor: presence, character (sweet, foul, musty can indicate specific organisms)
- ✓Pain: level and character at rest and during dressing changes
- ✓Signs of infection: increased warmth, erythema, drainage change, odor, delayed healing
- ✓Patient factors affecting healing: nutrition, blood glucose, perfusion, pressure offloading compliance
The WCC exam is 110 multiple-choice questions covering wound assessment, dressing selection, debridement, infection management, and patient education. Most candidates report the dressing selection and staging questions as the most challenging — there are many product types with overlapping indications. Our wound care certification practice test is designed around the NAWCO content outline and includes questions from every domain tested on the exam. Start with a diagnostic run to identify your weakest areas before your exam date.
Wound Pros and Cons
- +Wound certification is recognized by employers as verified competency
- +Provides a structured knowledge framework beyond just the credential
- +Certified professionals report 10–20% salary increases on average
- +Maintenance requirements create ongoing professional development
- +Differentiates candidates in competitive hiring and promotion decisions
- −Certification fees, materials, and renewal costs add up over a career
- −Requirements change — delaying may mean facing updated content
- −Salary ROI varies significantly by geography and industry
- −Preparation requires significant time alongside existing responsibilities
- −Validates knowledge at a point in time, not ongoing real-world performance
Wound Care Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.