PCA Medical: Personal Care Assistant and Patient-Controlled Analgesia Guide
PCA medical explained: what PCA stands for in healthcare, the personal care assistant role, patient-controlled analgesia, and PCA career paths.

PCA is one of those healthcare acronyms that carries two distinct and important meanings depending on context. In the workforce context, PCA stands for Personal Care Assistant — a frontline healthcare support professional who provides daily living assistance to individuals with disabilities, chronic illness, or age-related limitations. In the clinical context, PCA stands for Patient-Controlled Analgesia — a pain management technique that allows hospitalized patients to self-administer measured doses of pain medication via a programmed infusion pump. Understanding pca meaning medical professionals use requires knowing which meaning applies to the situation you're working in or reading about.
The two meanings coexist in hospital environments in a specific way: a PCA (Personal Care Assistant) working in a hospital may assist patients who are receiving a PCA (Patient-Controlled Analgesia) infusion. This overlap in terminology can be confusing in clinical notes and conversations, so healthcare teams increasingly use the full phrase — "PCA pump" or "PCA device" for the analgesia system, and "PCT" (Patient Care Technician) or the full "Personal Care Assistant" when referring to the staff role. In home health and long-term care settings, PCA almost exclusively refers to the Personal Care Assistant role.
This guide covers both meanings in detail. The first and larger section addresses the Personal Care Assistant role — what PCAs do, where they work, what training and certification is required, what they earn, and how the role fits into healthcare career progression. The second section covers Patient-Controlled Analgesia — how PCA pumps work, how they're programmed and monitored, what nurses need to know about managing PCA therapy, and how the technique is used across different patient populations.
For job seekers, the PCA title represents one of the most accessible entry points into healthcare. It typically requires no college degree — only a high school diploma or GED and state-approved training — making it a viable first step into a field with strong employment growth and meaningful career development opportunities.
The Bureau of Labor Statistics projects significant growth in home health aide and personal care aide positions through 2032 as the U.S. population ages and the preference for aging in place rather than institutional care strengthens. Understanding what the what is a pca in healthcare role actually involves is the starting point for anyone considering this career path.
For nurses, nursing students, and other clinical professionals, PCA analgesia is a standard postoperative and pain management technique that requires specific competencies in patient assessment, pump programming, and complication recognition. Many nursing boards and hospital accreditation standards now require documented PCA competency assessments for nursing staff who manage these infusions. The technique is effective, widely used, and generally safe when properly managed — but it carries specific risks, particularly around respiratory depression from opioid medication, that require vigilant monitoring protocols.
The terminology distinction matters more in practice than it might seem. A physician writing discharge instructions may note "patient tolerated PCA well" — which in a postoperative context clearly means Patient-Controlled Analgesia. A home health referral form noting "requires PCA eight hours daily" means the patient needs a Personal Care Assistant for eight hours per day.
Healthcare professionals who move between settings — hospital, long-term care, home health, hospice — regularly encounter both uses and must read context carefully. Standardized documentation practices in most health systems now require the full term at first mention to avoid ambiguity, with the abbreviation used only after establishing context.
For students preparing for healthcare certifications, this guide also serves as a focused review of two exam-tested domains: PCA role responsibilities appear in CNA, home health aide, and healthcare administrator certification exams; PCA analgesia appears in NCLEX-RN, NCLEX-PN, and acute care nursing specialty exams. The overlap in terminology makes a unified guide particularly useful for nurses who work in both acute hospital settings and home health or long-term care, where both meanings of PCA appear regularly in clinical practice and documentation.
Personal Care Assistant (PCA): A frontline healthcare support worker who assists clients with activities of daily living — bathing, dressing, mobility, meal prep, and more. Works in home health, hospitals, nursing homes, and assisted living. Entry-level role requiring state-approved training (no degree required). Median salary: $33,000–$36,000/year.
Patient-Controlled Analgesia (PCA): A hospital pain management system where patients self-administer programmed opioid doses via a bedside pump. The pump enforces lockout intervals and dose limits set by physician orders. Monitored by nursing staff for sedation level, respiratory rate, and pain control effectiveness.
PCA Medical: Core Aspects
Assists with bathing, dressing, grooming, mobility, feeding, and toileting. May also support meal preparation, housekeeping, and transportation depending on setting and scope.
IV infusion device programmed with drug, dose, and lockout interval. Patient presses a button to receive a controlled dose. Used postoperatively and for chronic pain management in hospitals.
PCAs (Personal Care Assistants) work in home health, assisted living, hospitals, nursing homes, hospice, and consumer-directed Medicaid programs across all 50 states.
PCA → CNA (additional training + exam) → LPN (12-month program) → RN (2-4 year degree). Many healthcare systems provide tuition assistance for this career ladder progression.
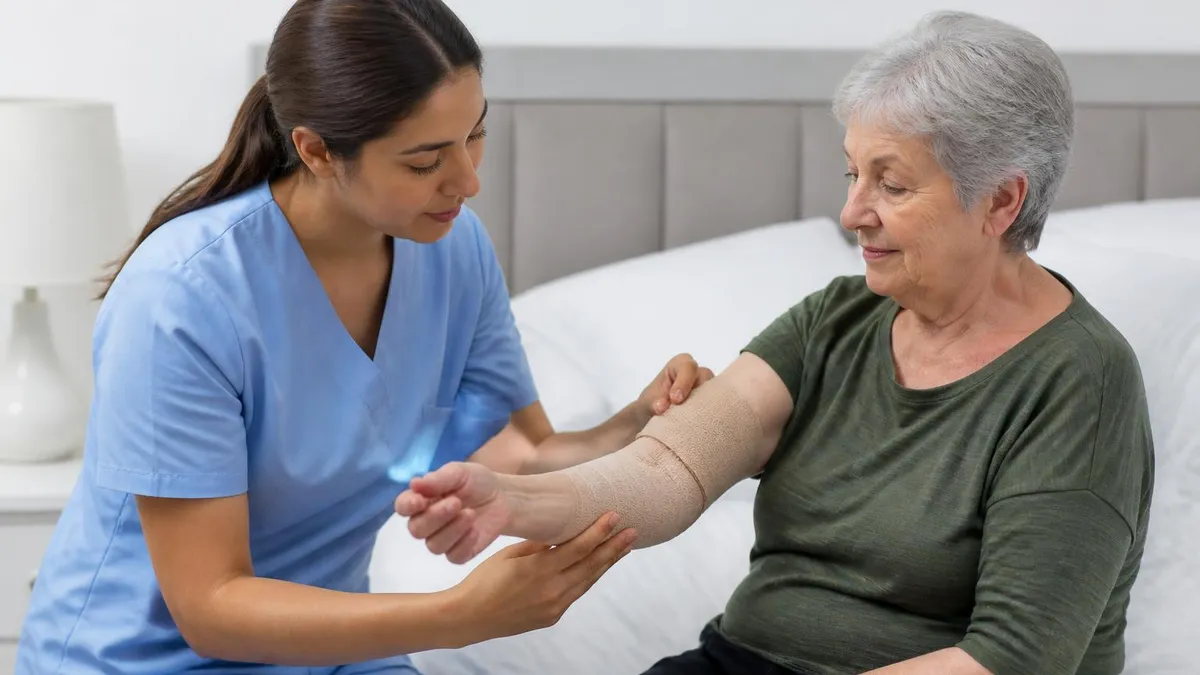
As a Personal Care Assistant, your core responsibility is supporting clients with the activities of daily living (ADLs) they cannot independently perform due to disability, illness, or age. ADLs include bathing, dressing, grooming, toileting, mobility assistance, feeding, and transferring between positions or locations.
Some PCA roles also involve instrumental activities of daily living (IADLs) — meal preparation, light housekeeping, medication reminders, and transportation to medical appointments. The specific tasks vary considerably by setting: home health PCAs often perform a broader range of IADLs, while PCAs in institutional settings like nursing homes or hospitals focus more tightly on the physical care ADLs during assigned shifts.
PCAs work under the supervision of registered nurses, licensed practical nurses, or in some home health settings, under a client's personal direction without a clinical supervisor present. The latter model — consumer-directed or participant-directed care — gives clients with disabilities significant control over who provides their care and how it's delivered. Many states have consumer-directed PCA programs through Medicaid that allow participants to hire, train, and direct their own PCAs, including family members in some cases. These programs have expanded access to care for adults with physical disabilities who want to maintain independence in their own homes.
The training requirements for PCAs vary by state and employer. Some states require completion of a state-certified training program (typically 8–75 hours) and passing a competency evaluation before working. Others require only employer-provided training on the job. Home health agency requirements are generally higher than private-pay home care requirements because Medicaid reimbursement rules apply. In institutional settings — hospitals, nursing homes, assisted living facilities — PCAs typically complete CNA (Certified Nursing Assistant) training or an equivalent program, which provides more extensive clinical skills training than basic PCA coursework.
The pca careers field offers genuine advancement potential. The most common progression moves from PCA to CNA (through an additional training and exam process), then to LPN (Licensed Practical Nurse, requiring a state-approved nursing program of roughly 12 months), and ultimately to RN (Registered Nurse, typically a 2-year ASN or 4-year BSN degree). Many healthcare systems offer tuition assistance programs that support PCAs who want to advance through this career ladder.
The direct patient care experience that PCAs develop — understanding patient needs, communication across health literacy levels, recognizing changes in patient condition — provides a clinical foundation that nursing schools consistently value in applicants.
Salary for PCAs reflects the entry-level nature of the position combined with strong demand. According to BLS data, home health aides and personal care aides earn a median annual wage of approximately $33,000–$36,000, with wide variation by state, employer type, and experience. PCAs working through consumer-directed Medicaid programs typically earn state-set hourly wages ranging from $12 to $21/hour depending on the state.
Hospital-based PCAs and those working through home health agencies that serve higher-complexity patients earn at the top of this range. Benefits availability varies significantly — agency employees typically receive benefits while self-employed consumer-directed PCAs may not. Understanding the full compensation structure is important when comparing PCA positions across different settings and employers.
State certification and the transition to CNA status represent the most common career advancement steps from a PCA role. The CNA exam tests both written knowledge of nursing assistant concepts and a clinical skills demonstration component. PCAs with several months of hands-on caregiving experience typically find the CNA skills test more manageable than candidates without prior direct care experience, which is one of the concrete advantages of starting in a PCA role before pursuing CNA certification.
Many state Medicaid agencies also now recognize advanced PCA competency levels that allow PCAs to perform limited expanded-scope tasks — such as medication administration reminders or simple wound care observation — with additional training and without requiring full CNA certification.
PCA Role by Healthcare Setting
Home health PCAs provide care in the client's own home, supporting aging adults, people with disabilities, and individuals recovering from surgery or illness. The scope typically includes ADLs (bathing, dressing, grooming, feeding, toileting) and IADLs (meal preparation, light housekeeping, laundry, medication reminders, transportation to appointments).
Consumer-directed Medicaid programs in many states allow participants to hire family members as their PCA, with the state or a fiscal intermediary processing payroll. Home health is the fastest-growing PCA employment setting, driven by the preference for aging in place and the cost advantages of home care versus residential facility care.

PCA Medical: By the Numbers
Patient-Controlled Analgesia is a pain management method in which the patient uses a bedside control device to self-administer pre-programmed doses of analgesic medication — most commonly opioids such as morphine, hydromorphone, or fentanyl — via an intravenous infusion pump. The physician enters orders that specify the drug, concentration, demand dose amount, lockout interval, and optional continuous background infusion rate. The pump enforces these parameters, preventing the patient from exceeding the prescribed dose regardless of how often the button is pressed.
The clinical rationale for PCA is well-established: patients who control their own pain medication timing tend to use less total opioid while achieving better pain control than those relying on nurse-administered PRN (as-needed) dosing. The ability to self-dose at the first onset of pain — rather than waiting for a nurse to assess, access the medication dispensing system, and administer — reduces the delay between pain and relief. The psychological aspect also matters: patients who feel in control of their pain management consistently report higher satisfaction and less anxiety during recovery.
The lockout interval is the central safety feature of the PCA system. After the patient presses the button and receives a dose, the pump enters a lockout period — typically 6–10 minutes — during which additional button presses are recorded but no additional medication is delivered.
This interval is based on the time required for the drug to reach peak effect, preventing the patient from stacking doses before the first dose's full effect is apparent. Even if a patient pressed the button continuously, the total drug delivered cannot exceed the programmed parameters. This design means that a properly programmed PCA pump with intact parameters is inherently dose-limited.
Nursing management of PCA therapy involves regular assessment of pain control, sedation level, respiratory rate, and oxygen saturation. The standard monitoring tool for sedation is the Pasero Opioid-Induced Sedation Scale (POSS), which describes four levels of sedation. POSS level S (sleep, easily aroused) is acceptable; POSS level 3 (hard to arouse) requires immediate intervention including holding further doses. Respiratory depression — typically defined as respiratory rate below 8–10 breaths per minute or SpO2 below 94% in baseline-normal patients — requires emergency intervention: naloxone administration per protocol and immediate physician notification.
Nurses caring for patients on PCA therapy should also be familiar with the concept of PCA by proxy — where family members or untrained visitors press the PCA button on behalf of the patient. This practice bypasses the fundamental safety mechanism of the system (that only a conscious, responding patient presses the button, providing feedback that the pain is present and the patient is awake enough to request medication). All nursing assessments and patient/family education for PCA therapy should explicitly address the dangers of proxy dosing.
Most hospital policies and ISMP (Institute for Safe Medication Practices) guidelines prohibit PCA by proxy except in specific clinical circumstances with physician orders and documented nursing supervision.
The choice of opioid for PCA therapy depends on the clinical setting, patient history, and institutional formulary. Morphine remains the most widely used PCA opioid due to its familiarity, established dosing parameters, and cost. Hydromorphone is preferred for patients with morphine intolerance or when a more potent agent is needed — it is approximately 5–7 times more potent than morphine on a milligram basis and has a slightly shorter duration of action.
Fentanyl PCA is used primarily in ICU settings or for patients with renal impairment, as fentanyl does not accumulate active metabolites the way morphine does. The nurse's role in PCA management includes verifying drug and concentration against the physician order and the pharmacy-prepared label, which is a critical safety check before initiating any PCA infusion.

PCA Certification Study Plan
- ▸Study basic anatomy and body systems relevant to daily care
- ▸Learn infection control: handwashing, PPE, standard precautions
- ▸Practice ADL assistance techniques: bathing, dressing, grooming, feeding
- ▸Review patient rights, dignity, privacy, and HIPAA basics
- ▸Learn body mechanics for safe transfers and repositioning
- ▸Practice wheelchair and ambulation assistance techniques
- ▸Study fall prevention, restraint policies, and environmental safety
- ▸Review emergency procedures: fire safety, cardiac events, choking
- ▸Practice vital sign measurement: temperature, pulse, respirations, blood pressure
- ▸Study observation and reporting skills — what changes to document and report
- ▸Learn therapeutic communication with patients, families, and care teams
- ▸Complete practice competency evaluations; review any weak areas before exam
The pca meaning spans caregiving support and clinical analgesia — two very different applications of the same three-letter abbreviation. Both involve direct engagement with patient wellbeing, both require trained personnel who understand how to recognize and respond to changes in patient status, and both play significant roles in modern healthcare delivery. Whether you're encountering "PCA" in a job listing, a hospital chart, a nursing textbook, or a state Medicaid program description, the context determines which meaning applies — and knowing both equips you to function effectively across the healthcare settings where these applications overlap.
For professionals preparing for healthcare certifications, PCA competencies appear in different examination domains depending on the credential. CNA and home health aide certification exams test PCA role responsibilities, ADL assistance techniques, patient rights, and communication with the care team. RN and LPN licensing exams (NCLEX) test PCA pump management, analgesic pharmacology, monitoring parameters, and complication recognition. Healthcare administrator and case management certifications test both — the organizational and reimbursement context of PCA programs and the clinical management protocols that determine quality of care outcomes for patients receiving both types of PCA services.
The growing demand for PCAs in home health settings reflects a fundamental shift in how the United States delivers long-term care. As hospital stays shorten and aging adults choose to remain at home rather than entering skilled nursing facilities, the volume of care needed in community settings grows.
PCAs are the workforce that makes this model work — providing consistent, reliable daily care that prevents hospitalizations, supports rehabilitation recovery, and enables aging adults and people with disabilities to maintain dignity and independence in their preferred living environment. Understanding the role from this broader system perspective helps PCAs appreciate the significance of their work beyond individual care interactions.
Digital health technologies are beginning to reshape both PCA meanings. Smart PCA pumps now integrate with hospital electronic health record systems to log every button press, dose delivered, lockout event, and alarm — creating an auditable medication administration record that reduces documentation burden on nursing staff and provides data for quality improvement review.
On the Personal Care Assistant side, home health technology platforms now use mobile applications to enable PCAs to document care tasks in real time, communicate with supervising nurses, and alert care coordinators when client conditions change. Telehealth models allow supervising nurses to observe and guide PCAs during complex care tasks via video connection, extending clinical oversight into home settings without requiring in-person visits for every interaction.
For anyone researching PCA career information, connecting with state-specific resources is essential because training requirements, Medicaid reimbursement rates, and scope-of-practice rules differ significantly across states. State departments of health and Medicaid agencies publish current PCA training requirements, approved training provider lists, and consumer-directed program eligibility rules.
Professional associations such as the National Association for Home Care and Hospice (NAHC) and the Direct Care Workers Association of North Carolina provide advocacy resources and policy updates relevant to the PCA workforce. Understanding both the clinical skills and the workforce policy context gives PCAs and prospective PCAs a fuller picture of the field they're entering and the systems they work within.
PCA Career: Pros and Cons
- +Low barrier to entry — no college degree required, training typically completed in weeks
- +Strong job security with 22% projected growth driven by an aging population
- +Direct patient impact — meaningful daily work supporting independence and dignity
- +Clear career ladder: PCA → CNA → LPN → RN with many employers offering tuition assistance
- +Flexible schedules available across home health, hospitals, and long-term care settings
- −Entry-level pay ($14–$18/hour) is modest for physically demanding work
- −Physical demands are significant — lifting, transfers, and extended standing cause high injury rates
- −Benefits availability varies widely, especially for home health and consumer-directed PCAs
- −Emotional demands of caregiving — particularly in hospice and dementia care — require resilience
- −Career advancement requires additional education and licensing beyond the PCA credential
PCA Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.