MRI Brain: What It Shows, Procedure and Common Findings
MRI brain guide — what the scan shows, sequences (T1, T2, FLAIR, DWI), contrast, procedure, claustrophobia tips, common findings and cost in 2026.
An MRI of the brain is the imaging test of choice for nearly every neurological question. From persistent headaches that have not responded to first-line treatment, to stroke evaluation, to suspected multiple sclerosis, to dementia workup, to brain tumor surveillance — the brain MRI sees pathology that CT misses entirely. Where CT shows blood and bone clearly, MRI shows gray and white matter, the ventricles and the vessels, the cortical sulci and the deep nuclei, the cranial nerves and the brainstem in detail no other imaging modality can match.
Doctors order a brain MRI when the working diagnosis involves something the brain tissue, the blood vessels feeding it or the cerebrospinal fluid surrounding it is doing wrong. Common scenarios include sudden focal weakness or speech disturbance suggesting stroke, persistent unilateral headache that has not responded to treatment, new-onset seizures, progressive cognitive decline, suspected multiple sclerosis, hearing loss to evaluate the auditory nerve, vertigo to evaluate the brainstem, and follow-up of a known mass to track growth or response to therapy.
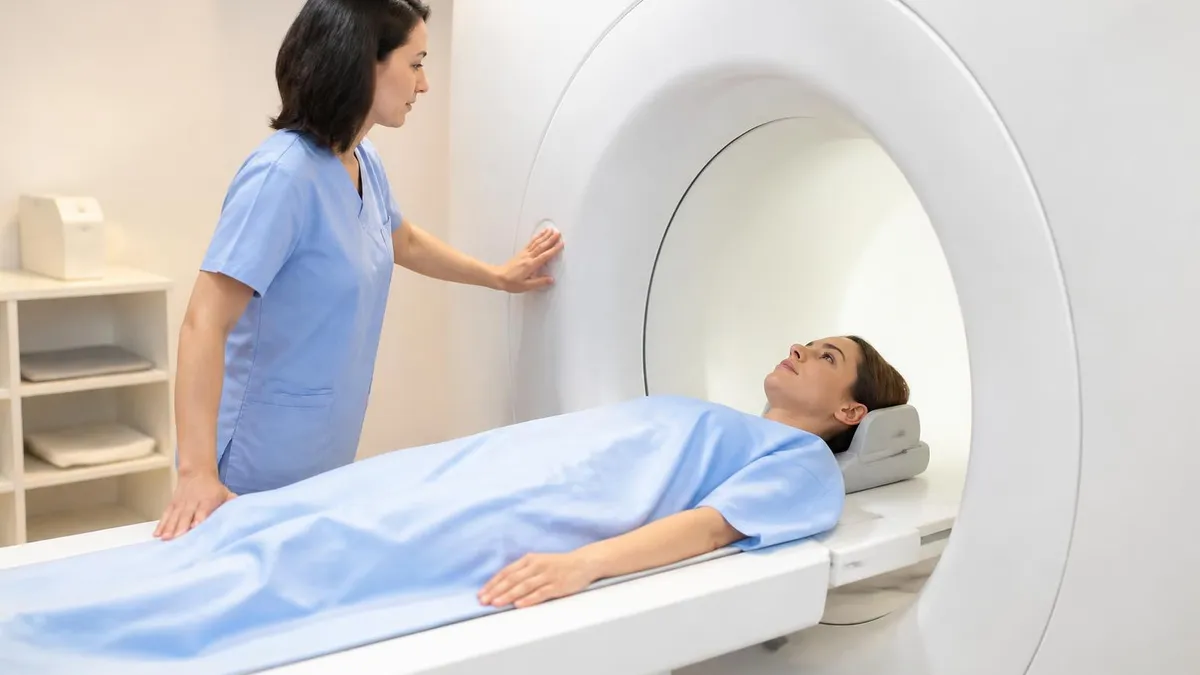
The procedure takes about 30 to 60 minutes depending on whether contrast is used and whether vascular sequences (MR angiography or MR venography) are included. The patient lies flat on a sliding table, a coil is fitted over the head, and the table moves into the magnet bore. Loud knocking, clicking and humming sounds are normal — they are the gradient coils switching as the scan acquires images. Some studies use intravenous gadolinium contrast injected partway through the scan, particularly when looking for tumors, infection, active inflammatory plaques or post-surgical changes.
This guide explains what a brain MRI shows, why each sequence is acquired, what to expect from the appointment itself, when contrast is needed, the contraindications that can exclude a patient from MRI, and what the most common findings actually mean. The goal is to demystify the test so you can prepare for it and read the report afterward with some grasp of what it is telling you about your nervous system.
Brain MRI in 30 seconds
A brain MRI uses a strong magnet and radio waves (no radiation) to produce detailed images of the brain, blood vessels and surrounding tissue. It shows gray matter, white matter, ventricles, blood vessels and lesions including tumors, strokes, multiple sclerosis plaques and hemorrhage. The scan takes 30 to 60 minutes, the patient lies still in a tube-shaped magnet, and the test is painless. Cost ranges from around $400 to $3,500 in 2026.
The clinical questions a brain MRI answers are remarkably specific. Is there a stroke, and is it acute or old? Is there bleeding inside the brain? Is there a mass, and if so what kind and where? Are the white matter changes consistent with multiple sclerosis, with small vessel disease, or with something else? Is the brain atrophy pattern consistent with Alzheimer's, frontotemporal dementia, or Lewy body disease? Are the cranial nerves and the auditory canals symmetric? Each question maps to specific findings the radiologist describes in the report.
Compared to other imaging tests, MRI's strengths are well-defined. CT scans use ionizing radiation and show acute hemorrhage and bone clearly; they remain the test of choice for trauma evaluation and acute stroke screening because of their speed (under 2 minutes versus 30 to 60 for MRI). Plain X-rays show only the bony skull. PET scans evaluate metabolic activity but do not show detailed anatomy. Functional MRI and diffusion tensor imaging are MRI add-ons used for specialized neurosurgical planning.
For most non-emergency neurological complaints — chronic headache, suspected MS, slow cognitive decline, hearing loss, persistent dizziness — MRI is the imaging test of first choice. For acute presentations like sudden weakness, severe head trauma, or possible intracranial hemorrhage, CT is faster and answers the immediate life-threatening question; MRI may follow once the patient is stable. The sequencing of CT then MRI is standard in stroke care because each test answers a different question.
For headaches alone — without red flag features like sudden onset, focal neurological signs, fever, vision changes, or new onset after age 50 — guidelines do not recommend immediate MRI. The yield is low and most chronic headaches respond to lifestyle changes and standard medications. MRI is reserved for headaches that have not responded to treatment, that are accompanied by neurological changes, or that have features suggesting a secondary cause from the outset.

When a brain MRI is ordered
Diffusion-weighted imaging detects acute infarcts within minutes of stroke onset, often before CT changes appear. MRA evaluates the carotid and intracranial arteries for stenosis or occlusion. The combination is the gold standard for ischemic stroke assessment in stable patients.
Brain MRI is the diagnostic standard for MS. T2 and FLAIR show characteristic lesions in the periventricular, juxtacortical, infratentorial and corpus callosum regions. Gadolinium-enhancing lesions indicate active disease. Annual surveillance MRI is standard for monitoring disease progression.
MRI characterizes the location, size, edema and enhancement pattern of suspected masses. Gadolinium contrast distinguishes tumor from edema and helps differentiate primary brain tumors from metastases. Surveillance MRI tracks response to surgery, radiation and chemotherapy over months and years.
MRI evaluates atrophy patterns, vascular contributions and rules out treatable causes like normal pressure hydrocephalus or chronic subdural hematoma. Hippocampal atrophy supports Alzheimer's disease; frontotemporal atrophy supports FTD. Volumetric analysis is increasingly used in clinical practice.
The MRI machine is a strong static magnet — typically 1.5 Tesla or 3 Tesla in modern hospitals — surrounded by gradient coils that switch on and off rapidly to produce position-encoding signals. A radiofrequency pulse perturbs the protons in the tissue and the returning signal creates the image. Different MRI sequences emphasize different tissues by varying pulse timing. The radiologist orders multiple sequences in a single exam to highlight different findings; for the brain, the standard protocol includes T1, T2, FLAIR, diffusion-weighted imaging and (when indicated) gradient echo or susceptibility-weighted imaging.
T1-weighted images show fat as bright and water as dark — the anatomical reference, easiest sequence to read for normal landmarks. T2-weighted images flip that contrast: water glows white, fat appears variable. Cerebrospinal fluid in the ventricles is bright on T2, which makes the ventricular system pop visually. FLAIR (fluid-attenuated inversion recovery) suppresses the bright cerebrospinal fluid signal so periventricular white matter lesions stand out — the workhorse sequence for MS plaques and small vessel disease.
Diffusion-weighted imaging (DWI) detects acute strokes within minutes of onset, even before CT can. DWI lights up areas where water molecules cannot diffuse normally, the hallmark of acute infarction. Gradient echo and susceptibility-weighted imaging detect blood products including microhemorrhages and superficial siderosis. T1 post-contrast images are acquired after IV gadolinium to identify lesions with broken blood-brain barriers, including tumors, infections and active MS plaques.
Vascular sequences are MR angiography (MRA) for arteries and MR venography (MRV) for veins. Both can be done with or without contrast; non-contrast techniques use blood flow itself to create the vessel images. MRA evaluates the carotid arteries, the vertebral arteries and the circle of Willis for stenosis, aneurysm or occlusion. MRV evaluates the cerebral venous sinuses for thrombosis, important in headache patients with risk factors for clotting.
Sequence-by-sequence breakdown
T1 is the anatomical reference sequence — fat bright, water dark, cerebrospinal fluid black. T2 is the workhorse for pathology — water bright, lesions usually appear bright. Reading both side by side establishes anatomy, identifies obvious lesions and provides the foundation for the rest of the protocol.
The decision to use contrast is straightforward in principle. Gadolinium-based contrast is necessary when the question involves blood-brain barrier breakdown — meaning tumors (primary or metastatic), infections (abscess, encephalitis, meningitis), active inflammatory plaques (multiple sclerosis), and post-surgical evaluation. Contrast is unnecessary for the everyday workup of stroke, headache, dementia evaluation, suspected hydrocephalus or follow-up of stable known lesions. The ordering doctor and the radiologist work this out before the scan.
Gadolinium-based contrast agents are generally safe but not without considerations. Patients with severe kidney disease (eGFR below 30) need a careful risk-benefit discussion because of nephrogenic systemic fibrosis associated with older agents. Newer macrocyclic agents are far safer and most institutions use them exclusively now. Allergic reactions to gadolinium are uncommon. Gadolinium retention in tissue including brain has been observed, but the clinical significance remains uncertain — discuss with your doctor if you have had multiple prior gadolinium studies.
The IV is placed before the patient enters the magnet room. Halfway through the scan the technologist injects the contrast through that IV from outside the room, and a final set of post-contrast T1 sequences is acquired. Total time added by contrast is about 10 minutes. Patients should expect a mild cool sensation during injection and occasionally a metallic taste; both pass in seconds. Drinking extra water for 24 hours after the scan helps clear the agent from the system.
Without contrast, the scan is shorter and avoids the IV altogether. For patients with needle phobia or a history of difficult IV access, asking the ordering doctor whether contrast is truly necessary is a fair question. Many brain MRIs done in outpatient settings can answer the clinical question without contrast. The radiologist may add a contrast injection during the scan if non-contrast images suggest something requiring it.
The MRI suite is one of the few places where the wrong metal object becomes a flying projectile. Before you enter the magnet room, expect a thorough safety screening covering pacemakers, defibrillators, cochlear implants, neurostimulators, drug-infusion pumps, intracranial aneurysm clips, certain heart valves and metallic foreign bodies in the eye. Some implants are MRI-conditional (safe under specific conditions), others are MRI-unsafe. Bring documentation if you have an implant — the manufacturer model number determines the answer.
Claustrophobia is the most common patient concern. The MRI bore is a tube about 60 to 70 centimeters in diameter, and most brain scans require the patient to be in the bore from the chest up with the head deepest in the magnet. For mild anxiety, calling ahead to ask about wide-bore MRI options at the facility helps; modern wide-bore magnets feel less confining. Music piped in through MRI-safe headphones, a sleep mask over the eyes and a squeeze-ball panic button reduce anxiety further.
For more severe claustrophobia, ask the ordering doctor about an oral anti-anxiety medication taken about an hour before the scan — diazepam, lorazepam or alprazolam in low doses are common. Patients on these medications need someone to drive them home. Open MRI machines (no full tube, only top and bottom magnets) exist at some facilities, although image quality is somewhat lower. In severe cases anesthesia may be requested, although this is rarely necessary for outpatient brain MRI.
Wear something with no metal — no zippers, no underwire bras, no metal buttons. The facility usually provides scrubs or a gown to change into. Leave watches, jewelry, hearing aids, hairpins, glasses, dental retainers, eye makeup with metallic flecks and credit cards in the locker. Tattoos with old metallic-based inks can warm slightly during the scan but rarely cause problems; report any heat sensation immediately.
Patients with permanent makeup should mention this during screening. Patients with a history of working with metal (machinist, welder) should mention any history of metal fragments in the eye; an X-ray of the orbits before MRI is sometimes ordered to rule out a retained fragment that could shift in the magnetic field. None of these scenarios are show-stoppers; they just require a known answer before the patient enters the magnet room.
Brain MRI preparation checklist
- ✓Confirm the scan is ordered with or without contrast
- ✓Disclose all implants, including dental work and tattoos
- ✓Wear metal-free clothing or plan to change into a gown
- ✓Remove jewelry, watches, hairpins and glasses
- ✓Bring an implant card if you have a pacemaker or stimulator
- ✓Take pre-prescribed anxiolytic about an hour before the scan
- ✓Arrange a driver if taking sedation medication
- ✓Eat lightly beforehand — full meals are fine for non-contrast
- ✓Bring previous MRIs on disc for comparison if available
The day of the scan, plan to arrive 30 minutes early to fill out paperwork and complete the safety screening. The technologist reviews your medical history, asks about implants and metal, and confirms the body part to be imaged. You change into a gown, lie on the table, and the technologist places a head coil over your head. The coil is the antenna that receives the MRI signal — it is plastic and lightweight. The table then slides slowly into the magnet bore.
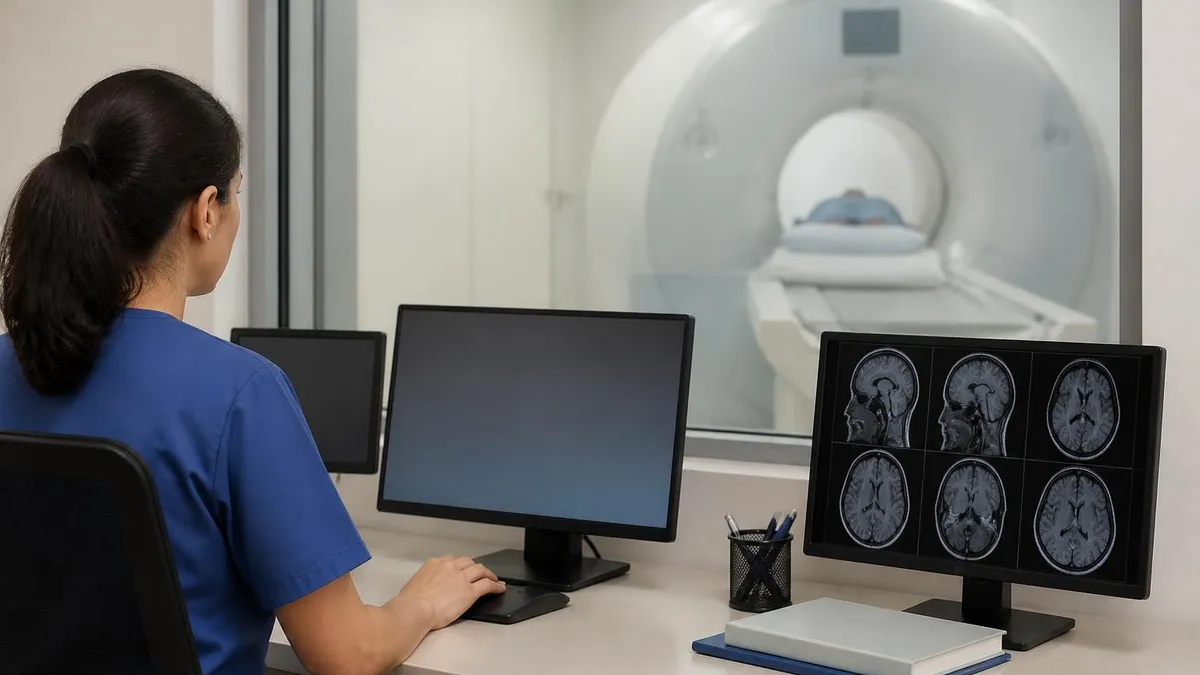
During the scan, the technologist watches you through a window from the control room and can speak to you through the intercom between sequences. You hold a panic-button squeeze ball at all times. The noise of the gradient coils is loud — earplugs and headphones are provided. Hold absolutely still during each acquisition; even small head motion blurs the images and may force the sequence to be repeated. Between sequences (about every 3 to 5 minutes) you can swallow or shift slightly.
After the scan, the technologist removes the coil, slides you out, and you change back into your clothes. There is no recovery time for non-contrast scans. For contrast scans, you may be asked to stay 15 minutes for monitoring. The radiologist reads the images later that day or the next, prepares a report and sends it to the ordering doctor. Most institutions also make the images and report available to the patient through a portal within 24 to 48 hours.
Reading your own report is fair. Reports follow a standard structure: clinical history, technique, comparison studies, findings (broken down by anatomical region), and impression. The impression at the bottom is the radiologist's summary. Words like "unremarkable," "no acute abnormality" or "no significant findings" are reassuring. Words like "infarct," "mass," "enhancement" or "signal abnormality" warrant a follow-up conversation with the ordering doctor.
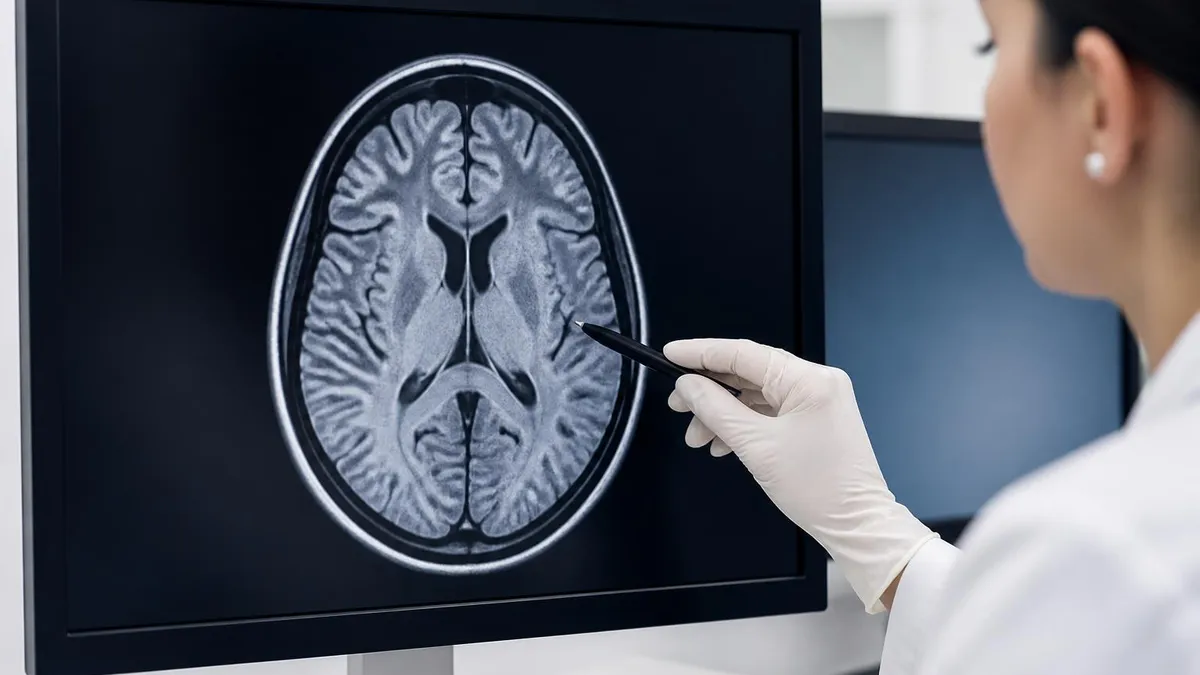
The most common findings on a brain MRI in adults are age-related and do not always have clinical significance. Small T2-bright lesions in the deep white matter — called nonspecific white matter hyperintensities or chronic small vessel ischemic disease — appear in nearly everyone past age 50 and reflect long-standing high blood pressure, diabetes or smoking. The radiologist's job is to tell which findings correlate with the clinical complaint and which are incidental signs of normal aging.
Multiple sclerosis plaques have characteristic features that distinguish them from age-related white matter changes. They appear as oval lesions oriented perpendicular to the ventricles (Dawson's fingers), often involve the corpus callosum, juxtacortical regions and infratentorial structures, and may enhance with contrast when active. The McDonald criteria use specific MRI findings combined with clinical features to make the diagnosis of MS.
Acute strokes appear as bright restricted-diffusion signal on DWI sequences, often before any visible change on CT or even on T2-weighted images. The territory affected indicates which artery is involved — the middle cerebral artery territory in lateral hemisphere strokes, the posterior cerebral artery for occipital strokes, the brainstem and cerebellum for posterior circulation strokes. MRA may show the underlying vessel occlusion.
Brain tumors vary in appearance depending on type and location. Glioblastoma appears as a heterogeneous enhancing mass with surrounding edema. Meningiomas appear as well-defined enhancing lesions attached to the dura. Metastases are typically multiple, well-defined, and located at the gray-white matter junction. The radiologist describes location, size, enhancement pattern and mass effect; the final diagnosis usually requires biopsy or surgical resection.
Brain MRI quick numbers
Common brain MRI findings
Nonspecific bright spots on T2 and FLAIR in the deep white matter. Common in adults over 50, reflecting chronic small vessel disease from hypertension, diabetes or smoking. Most are incidental but extensive disease correlates with cognitive impairment and stroke risk.
Characteristic oval lesions oriented perpendicular to ventricles, often involving corpus callosum and infratentorial structures. Active lesions enhance with gadolinium contrast. The McDonald criteria use specific MRI findings combined with clinical features to diagnose multiple sclerosis.
Bright restricted-diffusion signal on DWI and dark on ADC, often visible within minutes of stroke onset before CT changes appear. Territory affected indicates the involved artery. Critical for stroke triage and treatment decisions including thrombolysis and thrombectomy.
Variable appearance depending on type. Glioblastoma is heterogeneous with edema. Meningioma is well-defined and dural-based. Metastases are often multiple and at the gray-white junction. Final diagnosis usually requires biopsy or surgical resection after imaging characterization.
The cost of a brain MRI in the United States in 2026 ranges widely. Hospital-based outpatient imaging averages around $1,200 to $3,500 for a non-contrast brain MRI; the same scan at a freestanding imaging center often runs $400 to $1,200. With contrast, add about $200 to $400. Adding MR angiography or venography typically adds another $200 to $500. Calling three local facilities for the cash price before scheduling can save several hundred to over a thousand dollars, especially for high-deductible insurance plans.
Insurance coverage for brain MRI usually requires prior authorization. The criteria are clinical: documented neurological symptoms, failure of conservative treatment, the presence of red-flag features, or a clinical scenario where MRI changes management within the next month. Without prior authorization, the patient is responsible for the full cost. Medicare covers brain MRI under similar criteria with a copay. Some insurers steer patients toward specific lower-cost facilities; the network restrictions are worth checking.
Brain MRI: strengths and limits
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.