ACL Tear MRI: Findings, Grading and What to Expect
ACL tear MRI guide — how a torn ACL looks on MRI, partial vs complete tears, bone bruise patterns, sequences used, scan timing, cost and reading your report.
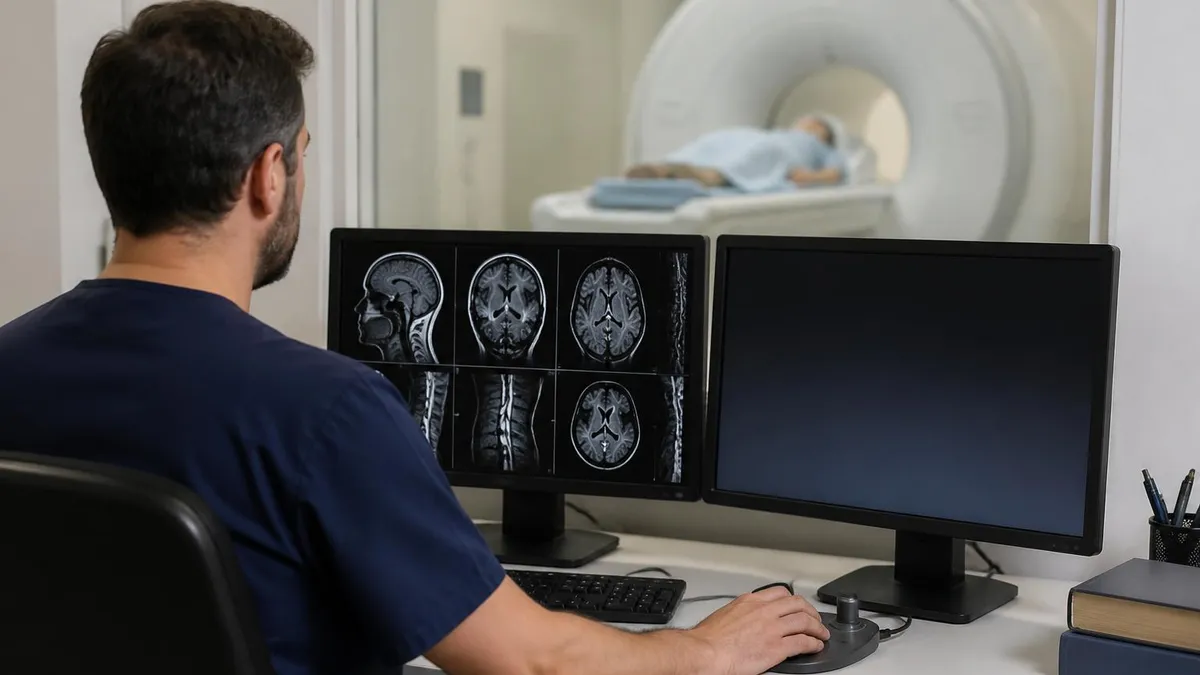
How an ACL Tear Shows Up on MRI
An ACL tear MRI is the imaging study that turns a clinical suspicion into a confirmed diagnosis. The athlete planted, twisted, heard a pop, and the knee blew up with swelling within hours. The Lachman test on exam felt loose. Now the orthopaedic surgeon needs to know exactly what tore, how badly it tore, and what else came along for the ride.
MRI answers those questions in a way no other imaging can — x-rays show bone, ultrasound struggles with deep ligaments, and CT lacks the soft-tissue contrast to grade ligament injury. Magnetic resonance imaging is the gold standard for ACL evaluation, and a well-performed knee MRI on a modern 1.5T or 3T scanner identifies ACL tears with sensitivity and specificity both above 90 percent.
This guide walks through the imaging itself — what sequences capture an ACL tear, the patterns radiologists look for, partial versus complete tears, the bone bruise signature that almost always accompanies a pivot injury, and the associated meniscus and ligament injuries that change surgical planning.
It also covers the patient experience, scan timing after the injury, cost without insurance, and the steps between MRI and either surgery or non-operative rehab. The aim is to give patients, parents of teenage athletes and weekend warriors a clear picture of what the scan shows so the conversation with the surgeon afterward is grounded in what the imaging actually means.
ACL Tear MRI Numbers
The MRI Signs of an ACL Tear
Radiologists look at several specific things on the sagittal images, which is where the ACL is best seen running from the back of the femur to the front of the tibia. In a normal knee, the ACL appears as a continuous low-signal (dark) band of fibres with a smooth, taut profile.
A complete tear interrupts that continuous band — the fibres are discontinuous, the ligament looks wavy or absent, and the empty space where the ACL should be fills with fluid signal that appears bright on T2 and proton-density sequences. The radiologist describes this as "discontinuity of the ACL fibres" or "non-visualisation of the ACL."
The secondary signs strengthen the diagnosis when the primary signs are subtle. The anterior tibial translation sign — the tibia has slid forward relative to the femur because the ACL is no longer holding it back — is one of the most reliable. The PCL buckling sign — the posterior cruciate ligament looks unusually curved because the femur has rotated relative to the tibia — is another.
The bone bruise pattern of marrow edema in the lateral femoral condyle and the posterior lateral tibial plateau is the third, and it appears in roughly 70 to 80 percent of acute complete ACL tears. These bone bruises happen because in the pivot mechanism the lateral femoral condyle slams into the posterior lateral tibial plateau, leaving a microfracture signature that is invisible on x-ray but bright on fat-suppressed MRI sequences.
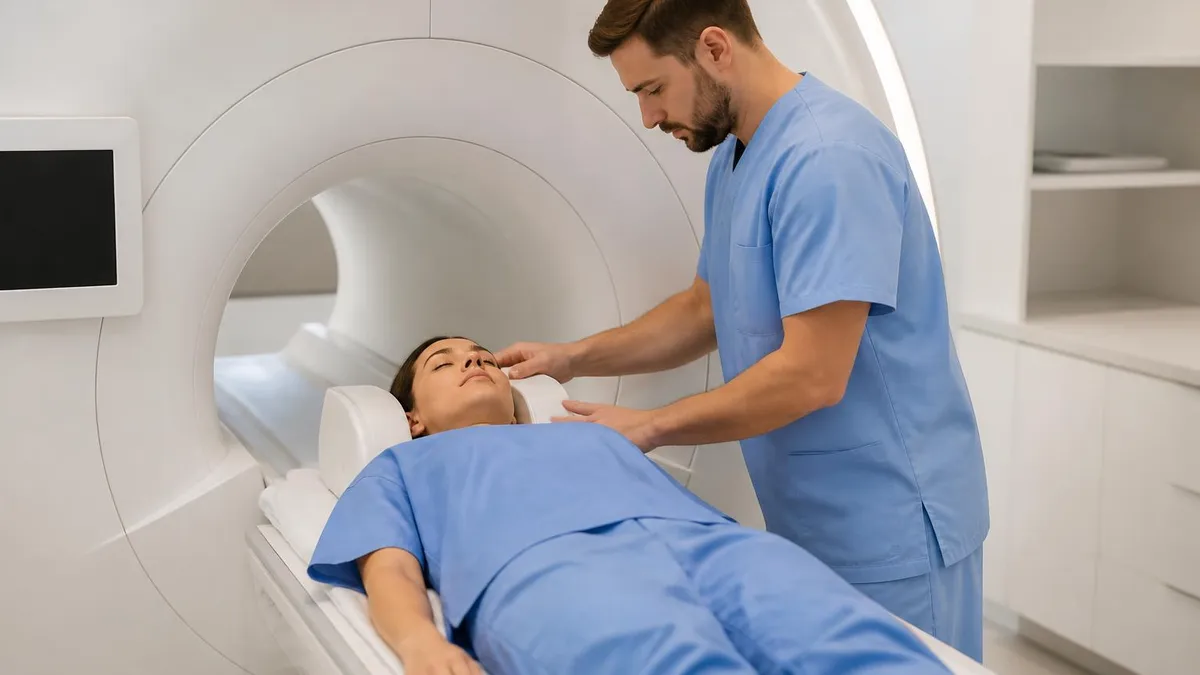
What the report usually says
A typical acute ACL tear MRI report reads: "Complete tear of the anterior cruciate ligament with discontinuity of fibres. Bone marrow edema involving the posterolateral tibial plateau and the lateral femoral condyle consistent with pivot shift mechanism. The PCL, MCL and LCL are intact. The medial meniscus is intact. There is a probable peripheral tear of the posterior horn of the lateral meniscus. Moderate joint effusion. Findings are consistent with acute ACL tear." Each clause matters — the ACL diagnosis itself, the bone bruise pattern that dates the injury, the ruled-out collaterals and PCL, and the associated meniscal injury that shapes the surgery.
Partial Tears vs Complete Tears
Most ACL tears imaged on MRI are complete tears. Partial tears exist but are clinically less common and harder to grade reliably. A partial tear shows some intact fibres alongside disrupted fibres, the overall ligament profile is preserved, and the secondary signs of complete tear (anterior tibial translation, PCL buckling, the classic bone bruise pattern) are typically absent or much subtler.
The radiologist describes a partial tear with language like "high-grade partial tear with the majority of fibres disrupted" or "low-grade partial tear with predominantly intact fibres and mild signal abnormality." Surgical decisions for partial tears are individualised — high-grade partial tears in young pivoting athletes often get reconstructed; low-grade partial tears in less active patients often heal with bracing and rehab.
The terms intact, sprained, partial tear and complete tear correspond loosely to grades 0 through 3 in the ligament injury grading system, although the formal grading is more commonly applied to MCL injuries than to the ACL. ACL tears are usually described qualitatively rather than with a numeric grade.
The clinical exam at the time of injury — particularly the Lachman test and pivot shift, ideally performed before the patient guards from pain — provides functional information that complements the structural imaging. Patients with a positive pivot shift under anaesthesia and a partial tear on MRI sometimes still benefit from reconstruction because the functional instability outweighs the imaged structural preservation. The decision is made by the surgeon in the clinic, not by the MRI alone.
Things the Radiologist Checks on ACL Tear MRI
Primary sign. Looks for discontinuity of the ligament fibres on sagittal images. Complete tear shows fibres disrupted across their full thickness. Partial tear shows some intact fibres with abnormal signal in the others. Chronic tear may show an absent or scarred ligament without acute fluid signal.
Look for marrow edema in the posterolateral tibial plateau and the lateral femoral condyle. Present in 70 to 80 percent of acute complete ACL tears. The pattern is so specific that it raises ACL tear concern even when the ligament itself looks ambiguous.
The tibia has slid forward relative to the femur on sagittal images because the ACL is no longer restraining it. The line drawn along the posterior femoral condyle extends beyond the posterior tibia. Strong secondary sign of complete ACL tear.
The posterior cruciate ligament appears unusually curved because of the abnormal femoral-tibial relationship. A normal PCL is gently curved; a buckled PCL has a sharp inflection. Suggests ACL deficiency causing the abnormal joint position.
Approximately 50 percent of ACL tears have associated meniscus tears — most commonly the lateral meniscus in acute injuries and the medial meniscus in chronic ACL deficiency. The radiologist describes location (anterior horn, body, posterior horn), pattern and whether the tear extends to the meniscal surface.
MCL, LCL, PCL all evaluated individually. Articular cartilage assessed for chondral defects or osteochondral lesions. Joint effusion noted. Any incidental findings like Baker cysts or popliteal lesions reported separately. Each contributes to surgical planning.
Why Timing of the MRI Matters
For most acute ACL injuries, the MRI is done within the first week. The bone bruise pattern is at its most prominent in the first two to three weeks after injury and gradually fades over months. Imaging during this window captures the cleanest signature of a pivot mechanism.
Joint effusion is also at its peak in the first week, and a tense knee with swelling that limits range of motion is itself part of the diagnostic picture. Some practices delay the MRI for a few days specifically to let the acute swelling settle and improve image quality, but no longer than that — earlier imaging is generally better.
Chronic ACL tears — those imaged months or years after the injury — look different from acute tears. The bone bruise pattern has resolved. The joint effusion may be minimal. The ACL itself may appear absent, scarred or remodelled rather than acutely discontinuous. The associated injuries shift too — chronic ACL deficiency wears down the medial meniscus and the articular cartilage on the medial compartment over time, so chronic tears more often show medial meniscus tears, chondral defects and early osteoarthritis.
The MRI report for a chronic ACL tear typically reads: "Chronic ACL deficiency. The native ACL is not clearly identified. Mild osteoarthritis of the medial compartment. Complex tear of the posterior horn of the medial meniscus." The clinical story matches — the patient has had years of intermittent giving-way episodes and now has nagging chronic knee pain.
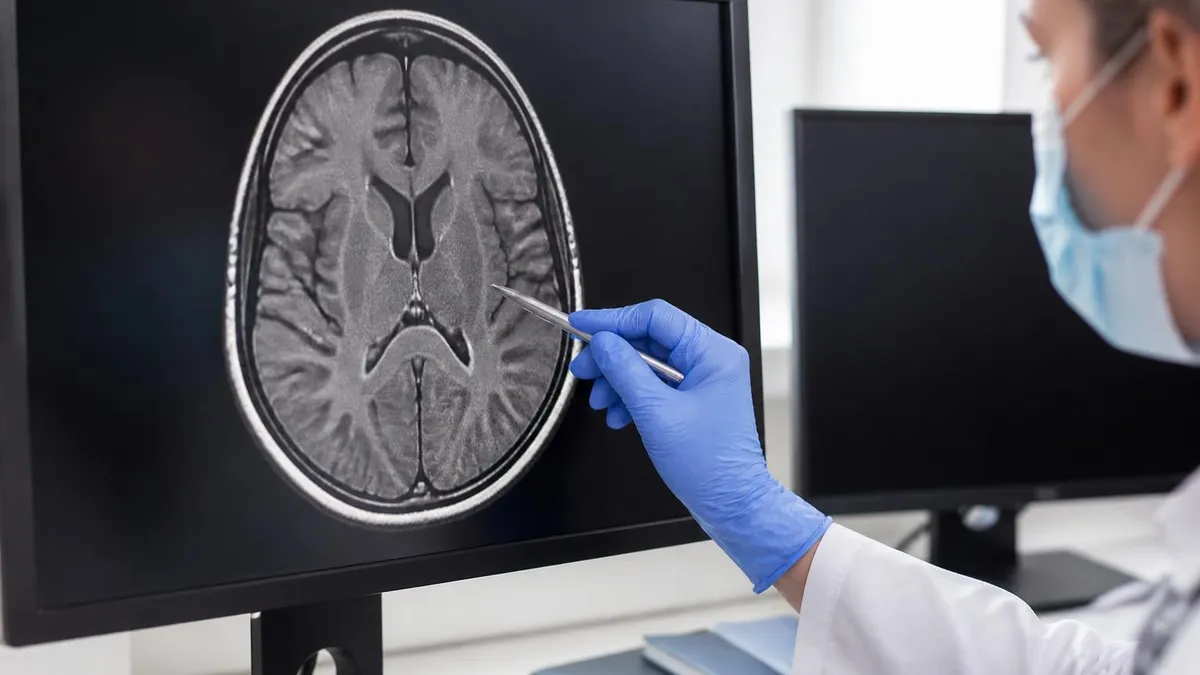
MRI Sequences Used to Evaluate the ACL
The single most important sequence for ACL evaluation. Proton-density-weighted with fat suppression. The ACL is best seen running diagonally on sagittal images. Fluid signal in the torn ligament gap appears bright, while intact fibres appear dark. Bone marrow edema in the lateral femoral condyle and posterior lateral tibia stand out because the fat signal is suppressed.
What the Scan Is Like for the Patient
The patient lies on their back on the scanner table. The injured knee goes into a dedicated knee coil — a cylindrical or rigid receiver that fits around the leg from mid-thigh to upper calf to maximise signal. The unaffected leg stays outside the coil and the rest of the body is largely out of the magnet bore.
This is one of the reasons knee MRI is generally easier to tolerate than head or spine MRI — much of the body never enters the scanner tunnel. The knee is positioned in slight flexion or with a small wedge of foam, depending on the protocol, and Velcro straps stabilise the leg.
Total scan time runs 20 to 40 minutes for a routine ACL tear workup. Each sequence takes 3 to 7 minutes, and the technologist communicates between sequences through an intercom. The scanner produces loud thumping and buzzing noises during gradient activity, and earplugs or headphones are provided.
The patient stays still throughout — even small movements blur the images and may require sequences to be repeated. Most patients with an acute knee injury find lying still for 30 minutes manageable; the bigger discomfort is often the swollen knee itself rather than the scanner. No contrast is needed in routine ACL evaluation, so there is no IV line and no fasting requirement.
Bring the MRI images and the radiology report to your surgical consultation, not just the report alone. Most orthopaedic surgeons want to look at the images themselves rather than rely entirely on the radiologist's written interpretation. The imaging centre will burn a CD or push the study to the surgeon's hospital system. Confirm that the surgeon's office can access your images before the appointment so the consultation is productive rather than spent chasing the imaging. Many practices have patient portals that let you download the images directly.
What Happens After the MRI Confirms an ACL Tear
If the MRI confirms a complete ACL tear in an active patient, the next conversation is about reconstruction. ACL reconstruction is the standard surgical treatment for complete tears in patients who want to return to pivoting sports — basketball, soccer, football, skiing, lacrosse, tennis.
The surgeon discusses graft options (patellar tendon autograft, hamstring autograft, quadriceps tendon autograft, allograft), timing (typically waiting until acute swelling resolves and range of motion returns, often 2 to 6 weeks after injury), and rehabilitation expectations (6 to 9 months of structured rehab before return to sport, with some surgeons preferring 9 to 12 months for younger athletes).
Non-operative treatment is reasonable for some patients — older adults who do not participate in pivoting activities, patients with significant medical contraindications to surgery, or those who prefer to try rehab and bracing first. The trade-off is the risk of repeated giving-way episodes that cause secondary meniscus tears and accelerate medial compartment osteoarthritis over time. The clinical decision is individualised based on activity goals, age, associated injuries and patient preference. The MRI provides the structural information; the conversation in clinic provides the path forward. Either way, the imaging is the pivot point between injury and a plan.
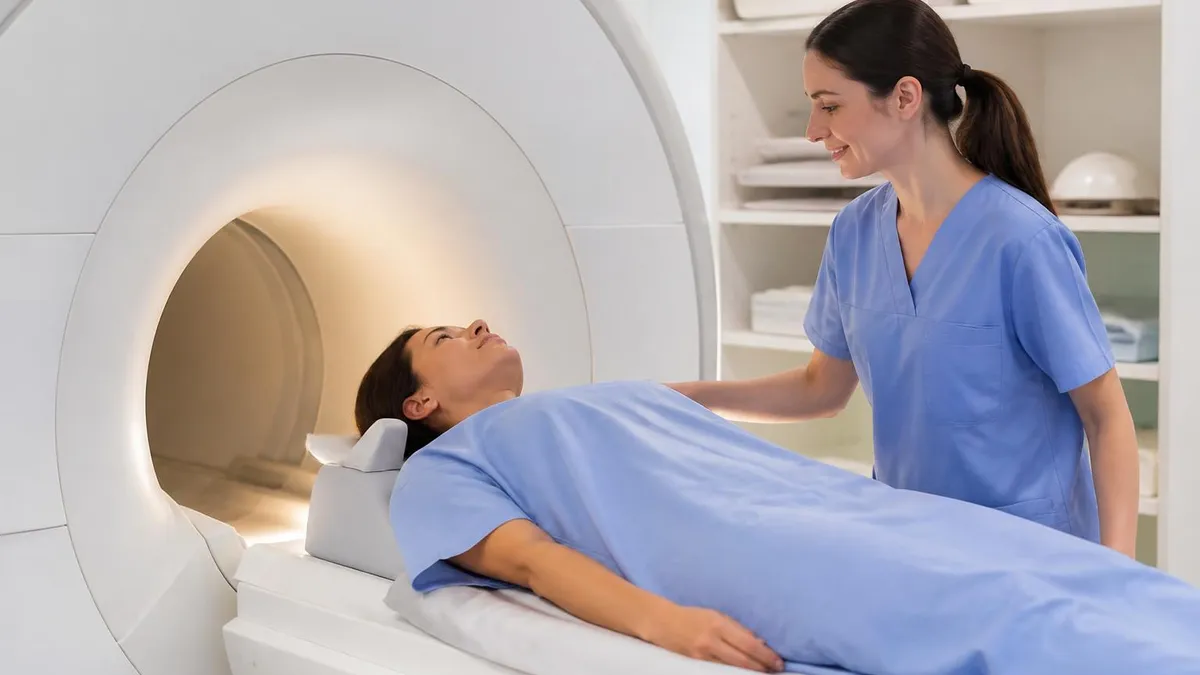
Preparing for an ACL Tear MRI
- ✓Confirm whether contrast is part of the order — most ACL evaluations do not need it
- ✓Disclose any metal implants, surgical clips, pacemakers or shrapnel
- ✓Wear comfortable clothing without metal — gym clothes work well, gowns are also fine
- ✓Remove jewellery, watches and any metal accessories before the scan
- ✓Take any pre-scan pain medication you have been prescribed for the swollen knee
- ✓Bring a knee brace if you wear one — it will need to come off for imaging
- ✓Arrive 30 minutes early to complete safety screening and check-in
- ✓Plan for a 20 to 40 minute session lying still inside the scanner
- ✓Arrange a driver if you took anything sedating before the scan
- ✓Confirm how you will receive results — patient portal, surgeon's office, or both
Cost of an ACL Tear MRI Without Insurance
Knee MRI is one of the lower-cost MRI body parts because routine ACL evaluation does not require contrast and the scan time is shorter than full-body or detailed brain protocols. Cash-pay rates at freestanding outpatient imaging centres typically run $500 to $1,500 in most US markets. Hospital-based imaging often costs 2 to 4 times more for the same study because of facility fees layered on top of the technical and professional charges. Major freestanding chains include RadNet, Akumin, Touchstone Medical Imaging, SimonMed and many regional independent centres, with availability varying by region.
Imaging marketplaces like MDsave and New Choice Health aggregate cash-pay knee MRI offerings from multiple centres at competitive bundled rates that include both the scan and the radiologist read. Cash-pay shopping pays off substantially for non-emergency knee imaging — a $500 freestanding scan saves $1,000 to $3,000 versus a hospital scan, and the diagnostic quality is essentially identical for routine ligament evaluation.
Sports medicine clinics and orthopaedic groups often have preferred imaging partners with bundled rates that the practice arranges on the patient's behalf, which simplifies logistics for patients who do not want to compare-shop. The cost of the MRI itself is also small compared to the cost of an ACL reconstruction that may follow, so spending time finding the cheapest scan should not delay the imaging when surgical timing matters.
ACL Tear MRI: Strengths and Limits
- +Sensitivity and specificity above 90 percent for complete ACL tears
- +Identifies associated meniscus, ligament and cartilage injuries that shape surgery
- +No ionising radiation — safe for repeat imaging during rehab if needed
- +Bone bruise pattern dates the injury and confirms pivot mechanism
- +Routine ACL evaluation does not require contrast, simplifying the experience
- −Partial tears are harder to grade reliably than complete tears
- −Chronic tears can be difficult to distinguish from absent ACL from a remote injury
- −Static imaging cannot capture dynamic instability that drives symptoms during activity
- −Some incidental findings on MRI do not correlate with clinical symptoms
- −Hospital-based imaging is dramatically more expensive than freestanding for the same study
Common Mistakes Patients Make Around the ACL MRI
The first common mistake is waiting too long. Athletes who pop the knee, swell, walk it off and assume it is a sprain sometimes wait weeks or months before getting imaging. By then the acute findings have faded, surgical timing has been pushed further out, and meanwhile the unstable knee has caused secondary meniscus damage from repeated giving-way episodes. If the knee popped, swelled within hours, and felt unstable, get evaluated by an orthopaedic specialist within a week and image within two weeks. The acute window is short.
The second common mistake is getting imaging at the most expensive facility because it is the closest or the most familiar. Hospital-based imaging departments often charge two to four times what an equivalent freestanding outpatient centre charges for the same study with the same diagnostic quality. For a non-emergency study like ACL evaluation, the few extra hours of scheduling at a freestanding centre saves thousands of dollars.
The third common mistake is reading the radiology report alone through a patient portal and panicking at the language. "Complete disruption of the anterior cruciate ligament with associated bone marrow oedema and joint effusion" sounds catastrophic in clinical language but is the expected and treatable finding after a typical pivot injury. The surgeon's appointment puts the report in context and outlines a clear path forward — wait for the consultation rather than spiralling on the wording.
A fourth mistake worth flagging is repeat imaging in the wrong window. Patients who feel that the surgeon did not adequately explain the MRI sometimes seek a second opinion and assume a new MRI is needed. Usually it is not. The original images are diagnostic, and a second surgeon can review them on disc or via a shared imaging portal.
Repeating the MRI weeks later may even produce a less clear picture because the bone bruises have faded and the joint effusion has resolved, leaving the second study with less information than the first. Save the second MRI for situations where the original study was technically inadequate or where many months have passed and the clinical picture has changed.
MRI Questions and Answers
The Bottom Line
An ACL tear MRI is the definitive structural test that turns a clinical suspicion into a treatment plan. For the athlete with a popped knee, sudden swelling and a positive Lachman, the scan confirms the diagnosis with above-90-percent accuracy and adds information about associated meniscus, cartilage and collateral ligament injuries that the orthopaedic surgeon uses to plan reconstruction.
The scan is short, no contrast is needed, the patient experience is generally easy compared to other MRI body parts, and cash-pay options at freestanding centres make it affordable even without insurance. Get the imaging within a week or two of the injury, bring the images to the surgical consultation, and let the conversation in clinic translate the report into a plan that matches activity goals.
Patients who understand what the scan shows and what the report language means are better partners in their care. The radiology report's words — complete tear, bone marrow edema, joint effusion, associated meniscus injury — sound clinical but describe a familiar pattern that orthopaedic surgeons treat routinely.
The MRI is the start of the conversation, not the end. Surgery or rehab, graft choice, timing and return-to-sport expectations all get worked out with the surgeon based on the imaging plus the activity goals and the clinical exam findings. Imaging is essential, but it is the pivot point in the workup rather than the final answer.
One last point worth underlining: the radiologist's reading is good but not perfect, and the most important second opinion is the surgeon looking at the actual images. Surgeons evaluate ACL tear MRIs all day, every day. They notice things that a generalist radiologist may not flag, particularly subtle associated injuries that affect the choice of graft or the surgical approach.
Bring the disc or push the study electronically to whoever you are seeing in clinic. The 30 minutes of looking at the images together during the consultation is worth more than any number of phone calls trying to interpret the written report after the fact.
And if the scan turns out to be normal — the ACL is intact, the menisci look fine, the cartilage is preserved — that information is also useful. Negative imaging in a patient with a swollen knee and a positive clinical exam shifts the conversation toward less obvious diagnoses like patellar dislocation, occult fracture, or a transient subluxation that has spontaneously reduced.
A normal MRI is not nothing. It rules out the diagnoses that matter most and points the workup in a different direction. Either way, the patient walks out of the imaging centre with information that did not exist before. That is what the scan is for, and that is why the orthopaedic surgeon ordered it.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.