CNA Subject Knowledge 2026: What CNAs Need to Know
Complete guide to CNA subject knowledge for 2026: anatomy, nursing skills, infection control, patient rights, vital signs, and free CNA practice tests to study.

CNA Core Subject Areas
Certified Nursing Assistant training programs cover a defined set of content areas that are both taught in the program and tested on the state CNA certification exam. The content areas align with federal minimum training standards (75 hours minimum, though most states require more) and state-specific curriculum requirements. Understanding which subjects are covered helps candidates study efficiently and prepare for both the written knowledge test and the clinical skills performance evaluation.
How CNA Content Is Organized
CNA training content is typically organized around seven major subject areas: basic nursing skills (direct patient care procedures); anatomy and physiology relevant to CNA care; infection control and safety; patient rights and promotion of independence; communication and interpersonal skills; mental health and social service needs; and care of residents with specific conditions (dementia, developmental disabilities). State CNA written exams draw questions from all of these content areas, with the largest emphasis on basic nursing skills, infection control, and patient rights.
Written Test vs. Skills Test
The state CNA certification exam has two components: a written (or oral) knowledge test and a clinical skills performance test. The written test evaluates knowledge across all content areas — typically 60 to 70 multiple-choice questions. The skills test evaluates the ability to correctly perform 3 to 5 clinical skills in front of a registered nurse evaluator, drawn from a defined list of skills (which varies by state). Passing both components is required for CNA certification. Study for the written test by reviewing all content areas; prepare for the skills test by practicing each skill against your state's published clinical skills evaluation criteria.

Anatomy and Physiology for CNAs
CNA training and exams include basic anatomy and physiology content focused on the body systems most relevant to caring for patients — particularly older adults in long-term care settings.
Body Systems CNAs Must Know
Integumentary system (skin): the skin is the largest organ and a primary concern in CNA care. CNAs monitor for pressure injuries (pressure ulcers/bedsores) at common bony prominences: sacrum, coccyx, heels, elbows, shoulders, and ears. Staging of pressure injuries (Stage 1–4, Unstageable, Deep Tissue Pressure Injury) and prevention strategies (repositioning every 2 hours, moisture management, protective positioning) are heavily tested. Musculoskeletal system: joint anatomy, range of motion principles, body mechanics for safe lifting and transfers, and common conditions (arthritis, osteoporosis, contractures) affecting mobility and care. Cardiovascular system: basic heart anatomy, what vital signs reflect cardiovascular status (blood pressure, pulse rate and rhythm), and signs of cardiovascular emergencies (chest pain, shortness of breath, irregular pulse). Neurological system: the nervous system's role in movement, sensation, and cognition; stroke signs (FAST — Face drooping, Arm weakness, Speech difficulty, Time to call 911); and care of residents with dementia and cognitive impairment. Respiratory system: anatomy of the airway and lungs, normal respiratory rates, signs of respiratory distress, oxygen use in the facility, and positioning to optimize breathing. Urinary system: kidney function, normal urine output, catheter care basics, signs of urinary tract infection, and fluid balance monitoring. Gastrointestinal system: digestion basics, normal bowel function, constipation prevention, and stool observation and reporting.
CNA Nursing Skills
Basic nursing skills — the hands-on patient care procedures performed by CNAs — are the most tested content area on state CNA exams. Both the written test and the clinical skills performance test evaluate nursing skills knowledge and competency.
Vital Signs
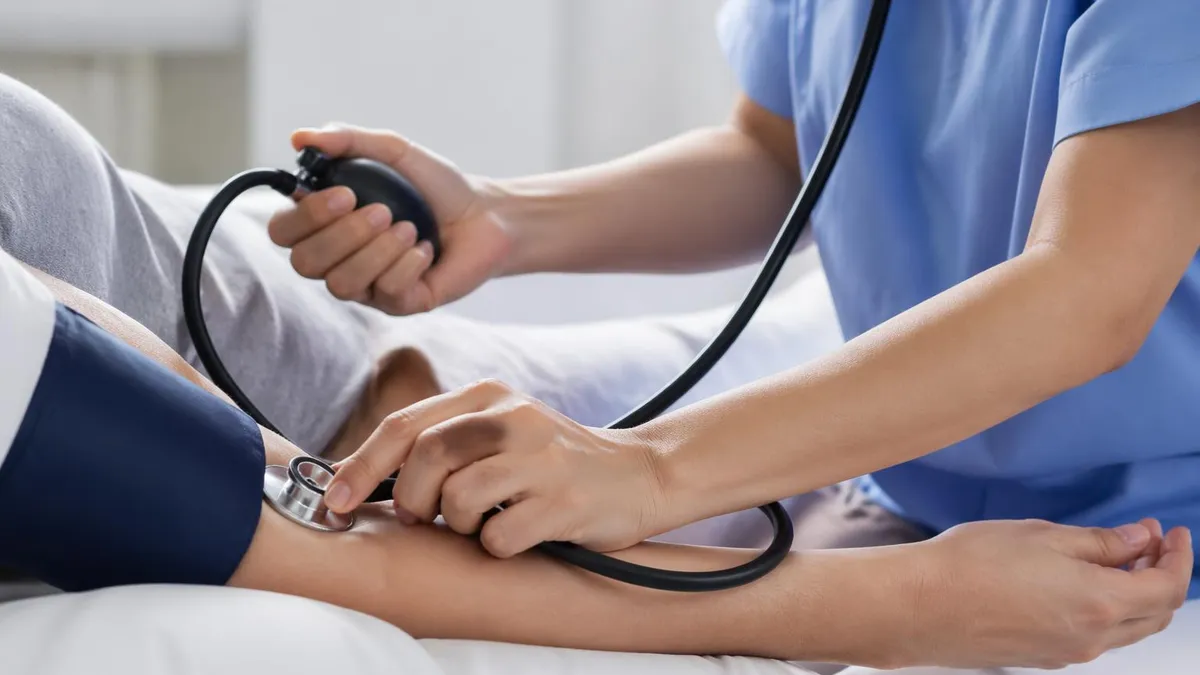
Vital signs measurement and reporting is a foundational CNA skill. CNAs measure: blood pressure (both manual with a sphygmomanometer and auscultation, and using automated devices); pulse rate and rhythm (radial pulse at the wrist is standard; apical pulse with a stethoscope when directed); respiratory rate (counting chest rises for one minute); temperature (oral, axillary, tympanic, temporal artery); and oxygen saturation (pulse oximetry). Normal ranges: blood pressure approximately 90–120/60–80 mmHg; pulse 60–100 beats per minute; respirations 12–20 per minute; oral temperature 97.8–99.1°F; oxygen saturation 95–100%. CNAs do not diagnose conditions from vital signs — they accurately measure and document, and report abnormal values to the charge nurse immediately.
Personal Care and Hygiene
Assisting residents with activities of daily living (ADLs) is a primary CNA function: bathing (bed bath, tub bath, shower assist); oral hygiene (brushing teeth, denture care); hair care; nail care; dressing and undressing; perineal care (careful cleaning of the perineal area to prevent infection); and incontinence care. The key principle across all personal care is preserving patient dignity — provide privacy, explain each step, and encourage the resident to perform as much as they are safely able to independently (restorative approach).
Transfers and Mobility
Safe patient transfers and mobility assistance are essential CNA skills: transfer from bed to wheelchair, wheelchair to chair, bed to stretcher; ambulation assistance with gait belts, walkers, canes; repositioning in bed; and use of mechanical lifts and transfer belts. Safe body mechanics — using legs (not back) to lift, keeping load close to the body, avoiding twisting — protect both the CNA and the patient. Gait belt use is standard for most transfer situations; mechanical lifts are required for non-weight-bearing or bariatric patients per facility policy.
Catheter Care and Urinary/Bowel
CNAs provide indwelling urinary catheter care: perineal care with catheter in place, securing the catheter tubing to prevent tension, positioning the drainage bag below bladder level, monitoring urine output (color, clarity, quantity), and reporting signs of infection or obstruction. CNAs do not insert or remove catheters — that is an RN or LPN function. Incontinent care, condom catheter application (for males), and external catheter care are also within CNA scope.
Safety and Infection Control
Infection control and safety are among the highest-weighted content areas on state CNA written exams. These topics reflect the critical importance of preventing healthcare-associated infections and maintaining a safe environment for both patients and healthcare workers.
Standard Precautions
Standard precautions are applied to all patients regardless of known infection status and include: hand hygiene (the most important infection control measure — wash hands with soap and water or use alcohol-based hand sanitizer before and after every patient contact, before and after glove use, after contact with potentially contaminated surfaces); personal protective equipment (gloves for contact with blood, bodily fluids, or contaminated surfaces; gown for situations with splash risk; mask and eye protection for splash/droplet risk); safe handling and disposal of sharps; and respiratory hygiene (cough etiquette, source control). CNAs must know when to apply each element of standard precautions — exam questions frequently test the sequence of hand washing steps, when to wear gloves vs. gown vs. mask, and proper removal of contaminated PPE.
Transmission-Based Precautions
Transmission-based precautions apply additional controls for patients with known or suspected infections: Contact precautions (gown and gloves required for entry) — used for infections spread by direct contact (MRSA, C. difficile, VRE, wound infections). Droplet precautions (surgical mask required when within 3 feet) — used for respiratory infections spread by large droplets (influenza, RSV, pertussis). Airborne precautions (N95 respirator and negative-pressure room required) — used for infections spread by small airborne particles (tuberculosis, measles, chickenpox). CNAs must know which precaution type applies to common infections and what PPE is required for each.
Patient Safety
Patient safety topics tested on CNA exams: fall prevention (identifying fall risk, using call lights, keeping beds in low position, using non-skid footwear, responding promptly to call lights); restraint use (restraints require a physician order, are a last resort, require monitoring every 2 hours for circulation and skin integrity, and the patient must be able to release them in an emergency); fire safety (RACE: Rescue, Alarm, Contain, Extinguish; PASS for fire extinguisher use); choking/Heimlich maneuver response; and emergency response procedures.

Patient Rights and Communication
Patient rights and communication skills are tested on every state CNA written exam and reflect the legal and ethical obligations CNAs have toward the people in their care.
Residents' Rights in Long-Term Care
The Nursing Home Reform Act (OBRA 1987) established federal residents' rights standards for nursing home residents that CNAs must know: the right to dignity and respect — residents must be treated with dignity in all interactions; the right to privacy — in personal care, mail, phone calls, and medical discussions; the right to confidentiality of health information (HIPAA applies in healthcare facilities); the right to informed consent and to refuse treatment; the right to participate in care planning; the right to freedom from abuse, neglect, and mistreatment; the right to manage one's own finances; the right to voice grievances without fear of retaliation; and the right to choose activities, schedules, and healthcare providers. CNAs who witness or suspect abuse, neglect, or mistreatment of a resident have a mandatory obligation to report it to their supervisor immediately.
Communication Skills
Communication content tested on CNA exams: verbal communication (speaking clearly, using appropriate language, avoiding medical jargon with patients, active listening); nonverbal communication (maintaining eye contact, open body language, respecting personal space); therapeutic communication techniques (open-ended questions, reflection, validation); and communication with residents who have hearing impairment, visual impairment, cognitive impairment, or aphasia (from stroke). CNAs document observations accurately in written form — objectivity (describing what is observed, not interpreted) is essential in nursing documentation.
Mental Health and Psychosocial Care
CNAs care for residents whose needs extend beyond physical health: Maslow's hierarchy of needs (physiological needs first, then safety, belonging, esteem, self-actualization) applies to understanding resident behavior and needs; stages of grief (Kübler-Ross: denial, anger, bargaining, depression, acceptance) are relevant for residents facing loss or terminal illness; depression recognition (withdrawal, loss of interest, changes in appetite and sleep); and dementia care (validation therapy, redirection, maintaining calm environments, consistent routines). CNAs are not mental health professionals — their role is observation, reporting, compassionate care, and supporting the interdisciplinary care plan.
Hand Hygiene Is the Most Important Infection Control Measure