CNA Skills Checklist: What You Need to Master for State Certification
Complete CNA skills checklist covering hand hygiene, vital signs, transfers, ADLs, and infection control. Master what state evaluators actually test.

What the CNA Skills Checklist Actually Covers
The CNA skills checklist is the list of hands-on patient care skills every certified nursing assistant must demonstrate to pass the state certification exam. The list varies slightly between states because each state runs its own certification program, but the core skills overlap substantially across all 50 states because they reflect federal Nurse Aide Training and Competency Evaluation Program (NATCEP) requirements established under the Omnibus Budget Reconciliation Act of 1987.
The skills focus on basic patient care, infection control, vital signs, mobility assistance, and activities of daily living that every CNA performs constantly across nursing home, hospital, and home care settings.
Most state exams pull from a list of 20 to 30 possible skills and require candidates to demonstrate 4 to 6 randomly selected skills on test day. The randomization means candidates cannot predict exactly which skills they will be tested on, which forces comprehensive preparation across the entire list.
Hand hygiene is always required because it is foundational to every other skill, and evaluators watch hand hygiene execution throughout the entire testing session. Failing the hand hygiene component fails the entire test regardless of how well other skills are demonstrated. Our CNA practice test covers the knowledge portion that pairs with skills demonstration.
The list of skills evolves slightly over time as best practices in patient care update. State boards of nursing review their CNA exam content periodically to incorporate changes in infection control practices, new equipment, and updated procedure standards. The core skills around vital signs, transfers, and ADLs remain stable across decades, but specific technique details sometimes change. Candidates should use current state-published study guides rather than older materials that may reflect outdated procedural standards no longer aligned with current state evaluator scoring criteria.
CNA Skills Checklist Quick Facts
Most state CNA exams test 4 to 6 randomly selected skills from a list of 20 to 30 possible skills. Hand hygiene is always required and failing it fails the entire test. Common tested skills include vital signs, transfers, feeding, and personal care procedures. Practicing all 20 to 30 possible skills until each one is automatic produces the best test-day outcomes regardless of which specific skills are randomly assigned during evaluation.
Hand Hygiene: The Foundation Skill
Hand hygiene is the most important skill on the checklist because it is performed before and after every other skill. Evaluators watch hand washing technique throughout the entire test session, not just when hand hygiene is the announced skill being tested.
The standard sequence runs: turn on water using a paper towel, wet hands and wrists completely, apply soap, lather and scrub for at least 20 seconds while running water continues, scrub between fingers and around wrists, rinse thoroughly with fingertips pointing down, dry hands with paper towels, turn off water using paper towel, dispose of paper towels in proper container without touching the trash can with bare hands.
The 20 second timing matters. Many candidates rush through the lathering and lose points for inadequate duration. Counting silently to 20 or singing happy birthday twice through provides reliable timing. The water direction also matters. Hands should be lower than elbows throughout washing so contaminated water runs from cleaner to dirtier areas rather than backward. Pointing fingertips down during rinsing keeps the clean rinse running away from the wrists toward the most contaminated areas (hands and fingers). Evaluators specifically watch for these technique details that distinguish trained hand hygiene from casual hand washing that most untrained adults perform.
Alcohol-based hand sanitizer is acceptable in some situations but does not replace soap-and-water washing for all scenarios. Hand sanitizer requires hands to dry completely (typically 30 seconds) before considering the procedure complete. Sanitizer is appropriate when hands are not visibly soiled. Soap and water is required after contact with bodily fluids, after using the bathroom, before eating, and in other specific situations. Knowing when to use each option correctly is part of the broader hand hygiene competence that evaluators assess.

Most Commonly Tested CNA Skills
Always required and watched throughout the entire test session. 20-second wash with proper technique including paper towel use for faucet handling. Master these elements through partner practice with verbal narration.
Blood pressure, pulse, respiratory rate, and temperature measurement. Each requires specific technique that evaluators score against checklist criteria. Master these elements through partner practice with verbal narration.
Bed to chair transfer, gait belt use, ambulation assistance. Safety is paramount and improper technique is heavily penalized. Master these elements through partner practice with verbal narration.
Bedpan use, perineal care, oral care, denture care, and similar ADL assistance procedures with attention to patient dignity and infection control. Master these elements through partner practice with verbal narration.
Vital Signs Measurement
Vital signs appear frequently on CNA skills tests because they reflect core competence that affects every patient interaction. Blood pressure measurement requires palpating the brachial pulse, positioning the cuff 1 inch above the elbow, inflating to 30 mmHg above the palpated systolic, deflating slowly while listening with the stethoscope, and reading both systolic and diastolic values to the nearest even number. Common mistakes include using the wrong cuff size, taking measurements over clothing, and rounding incorrectly. Evaluators score multiple specific steps within the procedure rather than just the final reading accuracy.
Pulse and respiration measurement together also commonly appear. Pulse is typically counted at the radial artery for 60 seconds (not 15 or 30 seconds for the exam, even though shorter counts may be common in practice). Respirations are counted by watching chest rise and fall, also for 60 seconds. The trick is counting respirations without telling the patient because conscious breathing changes the natural rate.
Most evaluators expect candidates to count respirations immediately after pulse while still appearing to count pulse, which masks the respiration counting from the patient. Temperature procedures vary by route (oral, axillary, tympanic) and each has its own specific technique requirements. Our CNA certification guide covers exam structure in detail.
Modern facilities increasingly use automated devices that calculate vital signs without manual technique. CNA skills tests still require manual technique because the equipment can fail and CNAs must be able to perform vital signs without electronic assistance. Practice with manual technique even if your training facility uses automated devices day to day. The manual skills also build deeper understanding of why values change in different physiological states, which helps clinical reasoning beyond just recording numerical values during routine patient interactions.
Vital Signs Skills Breakdown
Palpate brachial pulse, position cuff 1 inch above elbow, inflate 30 mmHg above palpated systolic, deflate 2-3 mmHg per second, read systolic and diastolic to nearest even number. Common errors include wrong cuff size and measuring over clothing. Practice each step until execution is automatic so test-day pressure does not cause skipped or rushed procedure components that cost points.
Transfers and Mobility Skills
Transfers and ambulation skills appear regularly because they involve real fall risk for patients and back injury risk for CNAs. The standard bed to chair transfer involves locking bed wheels, raising bed to working height, lowering bed rails, lowering bed to safe transfer height, positioning chair at correct angle to bed, locking chair wheels, applying a gait belt around the patient torso, helping the patient to a sitting position, swinging legs to dangle off bed edge, allowing dangling for orientation, supporting patient using gait belt, helping to standing position, pivoting toward the chair, and lowering the patient into the chair.
Gait belts are required equipment for most transfers in nursing facilities and hospitals. They go around the patient torso (not neck or hips) snug enough to provide grip but loose enough to allow normal breathing. CNAs grip the belt from below, never from above (which can pull the patient off balance). Body mechanics matter throughout. The CNA stands close to the patient with feet shoulder-width apart, knees bent, back straight, and lifts using legs rather than back. Twisting motions during transfers cause back injuries and result in significant skill demonstration deductions during testing.
Many real-world CNA injuries happen during transfers, which is why the skills test scrutinizes transfer technique carefully. Health care worker back injuries cost employers billions of dollars annually and account for substantial sick leave and worker compensation claims. Strong transfer technique using gait belts, proper body mechanics, and team-lift coordination when needed protects both patients and CNAs. The technique standards on the skills test reflect evidence-based practices proven to reduce injury rates across decades of occupational health research.
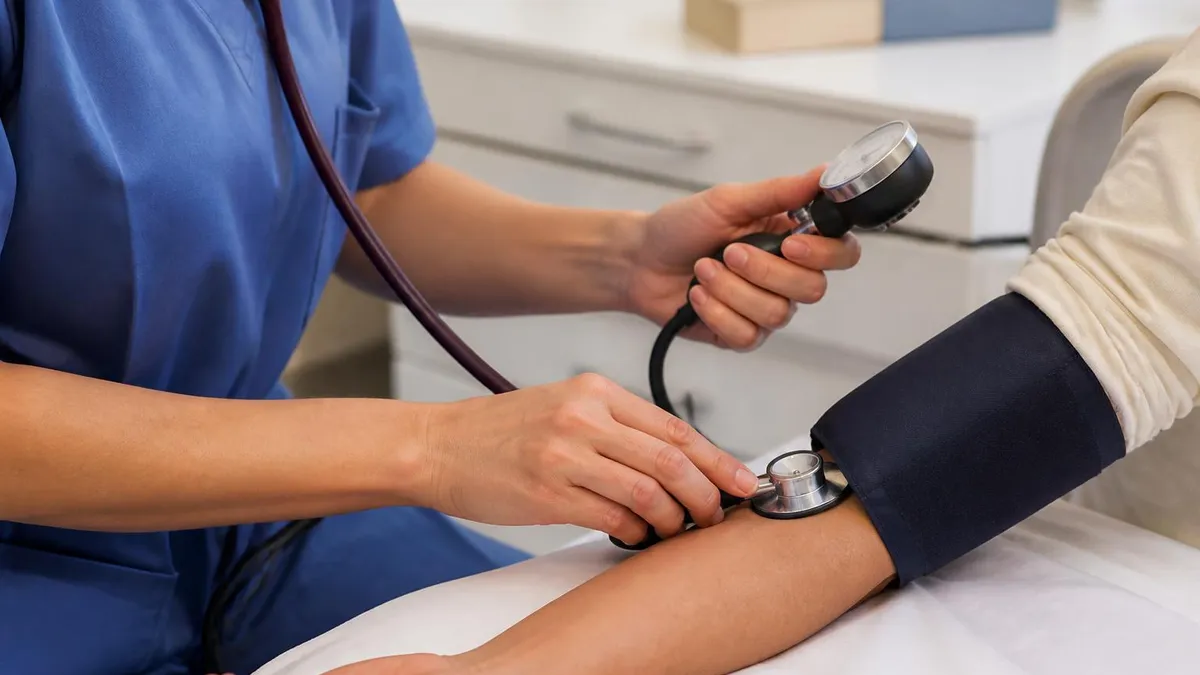
Evaluators watch how candidates protect patient privacy throughout the test. Failing to drape during peri-care, knocking before entering, or asking permission before procedures all result in deductions. Treat the test patient with the same dignity you would in a real clinical setting at all times. Many candidates lose points because they focus exclusively on procedural technique and forget the soft skills that real CNA practice requires consistently across patient interactions.
Activities of Daily Living (ADL) Skills
ADL skills make up a substantial portion of the testable skills list. Feeding a patient with chewing difficulties requires positioning the patient upright at 90 degrees, checking food temperature, alternating bites with sips of fluid, allowing time for chewing and swallowing, watching for signs of choking or aspiration, and proper documentation of intake. Oral care for unconscious patients requires positioning on side, using gauze or soft swab, cleaning all surfaces of teeth and tongue, and managing the swallow-versus-aspirate risk during procedure. Each ADL skill has specific evaluator checklist items beyond just completing the task.
Perineal care (peri-care) for both male and female patients commonly appears as a tested skill. The procedure protects patient dignity throughout (draping, doors closed, voice low), uses front-to-back cleansing direction for females (which prevents UTI risk from contamination), uses gentle motion appropriate to fragile skin, and changes wash cloths or wipes frequently to avoid recontamination. Failing to maintain front-to-back direction is one of the most common technique errors that costs points on this skill. Bedpan placement, removal, and patient repositioning during the procedure have their own specific technique requirements that test candidates regularly miss.
Dressing skills appear frequently in cases involving patients with one-sided weakness from stroke or other conditions. The general rule is to dress the weak side first and undress the weak side last. This minimizes the manipulation of the affected arm or leg by working around it from the strong side. The principle applies broadly to grooming, bathing, and other ADLs where patients have asymmetric capability. Evaluators specifically watch for this technique in dressing scenarios because the correct sequence demonstrates patient-centered thinking.
Master List of Common CNA Test Skills
- ✓Hand washing with proper 20-second technique (drill until execution is automatic)
- ✓Donning and removing gloves correctly (drill until execution is automatic)
- ✓Counting and recording radial pulse for 60 seconds (drill until execution is automatic)
- ✓Counting and recording respirations for 60 seconds (drill until execution is automatic)
- ✓Measuring and recording blood pressure (drill until execution is automatic)
- ✓Measuring and recording oral or axillary temperature (drill until execution is automatic)
- ✓Bed to chair transfer using gait belt (drill until execution is automatic)
- ✓Ambulation with gait belt and proper body mechanics (drill until execution is automatic)
- ✓Bedpan placement, removal, and peri-care (drill until execution is automatic)
- ✓Oral care for conscious and unconscious patients (drill until execution is automatic)
- ✓Dressing patient with weak side affected (drill until execution is automatic)
- ✓Feeding patient at appropriate pace and watching for choking (drill until execution is automatic)
- ✓Position changes including supine to side-lying (drill until execution is automatic)
- ✓Skin assessment and documentation (drill until execution is automatic)
Infection Control Throughout the Test
Infection control runs throughout the entire CNA skills test, not just as a standalone skill. Glove use is required for any procedure involving bodily fluids. Gloves should be removed and disposed of properly between tasks and before touching clean surfaces. Hand hygiene must occur immediately after glove removal. Gowns and masks may be required for specific isolation scenarios that evaluators sometimes work into test cases. Disposal of contaminated linens, used supplies, and biohazardous waste all follow specific procedures that evaluators watch for.
Standard precautions apply to all patient interactions during the test. This means treating every patient as potentially infectious regardless of any specific known diagnosis. Always assume the test patient could have an infection you do not know about, and apply infection control precautions accordingly. Candidates who only follow precautions when explicitly told the patient has an infection often miss points because real CNA practice treats every patient with standard precautions as a baseline. Demonstrating consistent infection control throughout the test session shows the evaluator that you have internalized the practice standard rather than just memorized procedural steps for individual skills.
Standard precautions include hand hygiene, glove use for any bodily fluid contact, gown for splash risk, mask for respiratory droplet risk, and proper disposal of contaminated supplies. Contact precautions add gown and gloves for specific infections that spread through touch. Droplet precautions add masks within 3 feet of the patient. Airborne precautions add N95 respirators and negative pressure rooms. Understanding which precaution level applies to which patient scenario demonstrates the clinical reasoning behind infection control rather than rote procedure memorization.
How to Practice CNA Skills Effectively
The single most effective practice technique is repetition with verbal narration. Walk through each skill step out loud while performing the actions, talking yourself through every component the evaluator will score. This builds both the muscle memory of the physical procedure and the cognitive sequence that prevents skipping steps under test pressure. Practice partners who play the patient role provide realistic feedback about technique that solo practice cannot. Take turns playing patient and CNA across full skill sequences during training.
Recording video of yourself performing skills can reveal technique problems you cannot see while performing. Watch the recordings against published evaluator checklists, score yourself on every checklist item, and identify which items you consistently miss. Common patterns include forgetting to lock bed wheels before procedures, not announcing yourself before entering the patient room, failing to introduce yourself and explain procedures, and rushing through hand hygiene. These small but constant deductions add up to failing scores even when the primary skill is performed adequately. Closing the small technique gaps moves you from borderline pass to confident pass on test day.
Mock test sessions with a trained partner who follows the actual evaluator checklist provide the closest experience to real testing conditions. Many training programs run formal mock tests in the final weeks before state exams. If your program does not, ask the instructor to grade you against the official state checklist during a practice session. Specific feedback on which checklist items you missed produces faster improvement than general feedback about overall performance. Use the mock test feedback to focus remaining practice time on weak items.

CNA Skills Test Numbers
Three Categories of CNA Skills
Hand hygiene, glove use, infection control. Always tested directly or watched throughout the entire test session. Master these elements through partner practice with verbal narration.
Vital signs across multiple routes. Tested frequently because they affect every patient interaction and clinical decision-making. Master these elements through partner practice with verbal narration.
Transfers, ADLs, peri-care, feeding. Make up the bulk of testable skill options across most state checklist versions. Master these elements through partner practice with verbal narration.
Common Test Day Mistakes to Avoid
Many candidates fail the CNA skills test for procedural reasons rather than lack of technical knowledge. The most common is forgetting to wash hands at the right times. Hand hygiene happens before entering the room, between any procedures that touch the patient, after any contamination, and before leaving the room. Missing any of these handwashing moments costs significant points. Setting up a mental cue (hands wet at the start of any procedure block) helps candidates remember to perform hand hygiene at every required point without missing any.
Another common mistake is failing to communicate with the patient throughout procedures. CNAs must announce themselves, explain what they are doing, ask permission for procedures, and check in on patient comfort throughout. Performing procedures silently as if the patient is a mannequin loses points because evaluators score communication explicitly. Even simple statements like I am going to take your blood pressure now or let me know if anything feels uncomfortable accumulate points across the multi-skill test session. Confident verbal communication signals professionalism that evaluators reward consistently across testing locations.
Rushing through procedures because of perceived time pressure also causes errors. The skills test allows adequate time for proper technique, and evaluators specifically watch for candidates who skip steps or shortcut procedures because they think they are running out of time. The published skill timing standards reflect realistic completion times for the procedures, and candidates who feel rushed typically have not practiced enough to internalize the procedure flow. Practicing skills to the point where you no longer need to consciously think about each step produces calm, methodical test-day performance.
Pros and Cons of CNA Skills Test Format
- +Random skill selection ensures comprehensive preparation across all possible items for CNA candidates and current nurse aides
- +Hands-on format directly tests skills CNAs actually use daily for CNA candidates and current nurse aides
- +Evaluator checklists provide clear scoring criteria for preparation for CNA candidates and current nurse aides
- +Practice with a partner mirrors real test conditions well for CNA candidates and current nurse aides
- +Skills test is separate from written knowledge test allowing focused prep for CNA candidates and current nurse aides
- −Test anxiety can degrade technique even for well-prepared candidates worth planning around during preparation
- −Small procedural errors accumulate to failing scores quickly worth planning around during preparation
- −Hand hygiene errors alone can fail the entire test session worth planning around during preparation
- −Limited time per skill creates pressure that real clinical work lacks worth planning around during preparation
- −Different evaluators may interpret checklist criteria slightly differently worth planning around during preparation
CNA Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.