ATLS Training Programs: Course Format, Requirements, and What to Expect
Pass your ATLS Training Programs: Course Format, exam on the first attempt. Practice questions with detailed answer explanations, hints, and instant scoring.
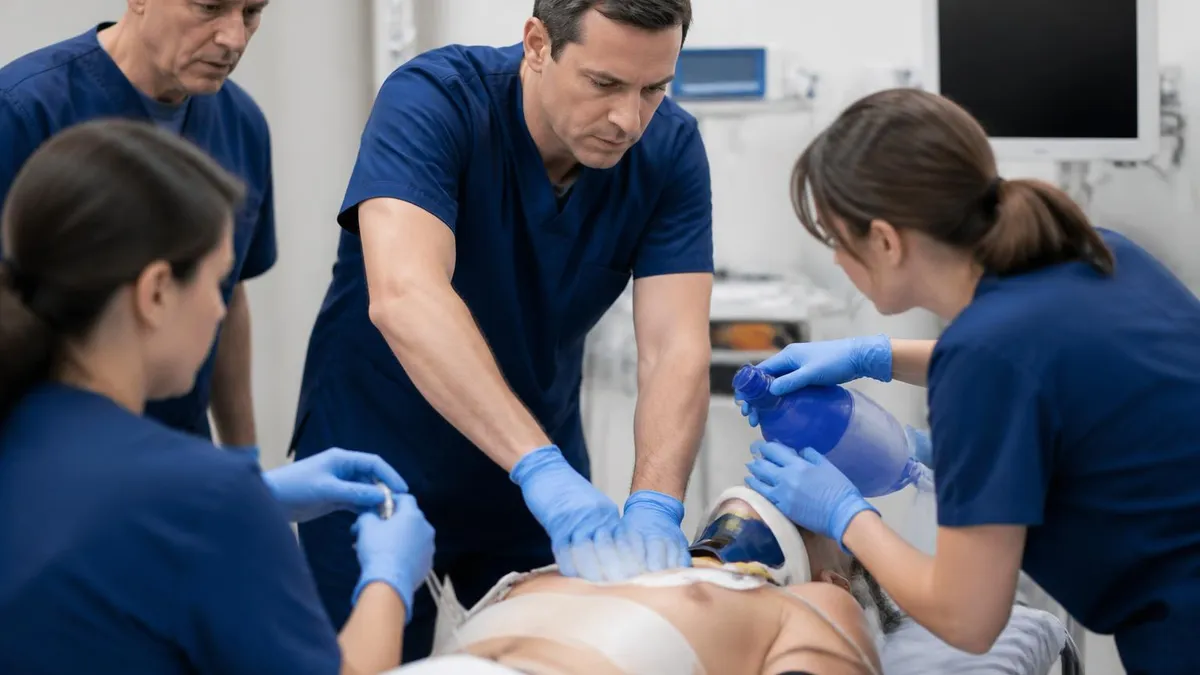
Advanced Trauma Life Support (ATLS) is the global standard for initial trauma assessment and management training. Surgeons, emergency physicians, and other trauma providers worldwide use the ATLS systematic approach—primary survey, resuscitation, secondary survey, and definitive care—to evaluate and stabilize critically injured patients rapidly and consistently. Understanding what ATLS training programs involve, who qualifies to attend, what the course teaches, and where to find certified courses is essential for any clinician working in trauma, surgery, or emergency medicine.
The ATLS program was developed in 1978 by orthopedic surgeon James Styner after a plane crash left him responsible for managing his own critically injured family members in a rural setting with inadequate resources. The experience revealed a stark gap in trauma training, and Styner worked with the ACS Committee on Trauma to create a course that would give any physician a structured, reliable process for evaluating trauma patients within the first hour of care—the so-called “golden hour.”
The course has since been taught in more than 80 countries and remains the most widely recognized trauma training credential in medicine. Today the ACS Committee on Trauma continues to update the ATLS curriculum periodically, incorporating new evidence on hemorrhage control, damage control resuscitation, and trauma neurology to keep the program aligned with current best practices in trauma care.
ATLS is not merely a certification box to check. Programs that require ATLS do so because the systematic primary survey approach reduces errors of omission—critical injuries missed because evaluation was disorganized or incomplete. Hospitals credentialing surgeons or emergency physicians for trauma call frequently list ATLS certification as a requirement. Residency programs in surgery, emergency medicine, and orthopedics commonly require residents to complete ATLS during training. For internationally trained physicians seeking hospital privileges in the United States, ATLS certification often serves as a recognized demonstration of trauma competency.
ATLS training is distinct from hospital trauma orientation protocols, nursing trauma competencies, and EMS-level training in that it provides a unified physician-level framework with procedural skills components. The emphasis on hands-on skills stations—practicing airway management, chest decompression, and trauma simulation in a controlled environment—makes ATLS fundamentally different from a purely didactic course. The procedural confidence built during skills practice is explicitly designed to transfer to real clinical environments, including resource-limited or austere settings where familiar equipment and support may not be available.
Physicians sometimes compare ATLS with other trauma training programs designed for different provider groups. ATCN (Advanced Trauma Care for Nurses) is the nursing-specific parallel program developed by the Society of Trauma Nurses. PHTLS (Prehospital Trauma Life Support) serves EMS providers. ATOM (Advanced Trauma Operative Management) is an ACS-developed course for surgeons focused on operative hemorrhage control. Each program addresses the same foundational trauma priorities through the lens of its specific provider role and scope of practice, and they are complementary rather than competing frameworks.
The global standardization that ATLS has achieved over four decades is one of its most significant contributions to medicine. When a surgeon trained in Nigeria, a physician from Brazil, and a military physician from the United States all hold current ATLS certification, they share a common framework, common terminology, and common prioritization logic that enables effective collaboration on a multiply injured patient even without prior familiarity. This shared language is particularly valuable in military operations, disaster response, and international humanitarian missions where providers from different countries and training systems must work together rapidly and efficiently.
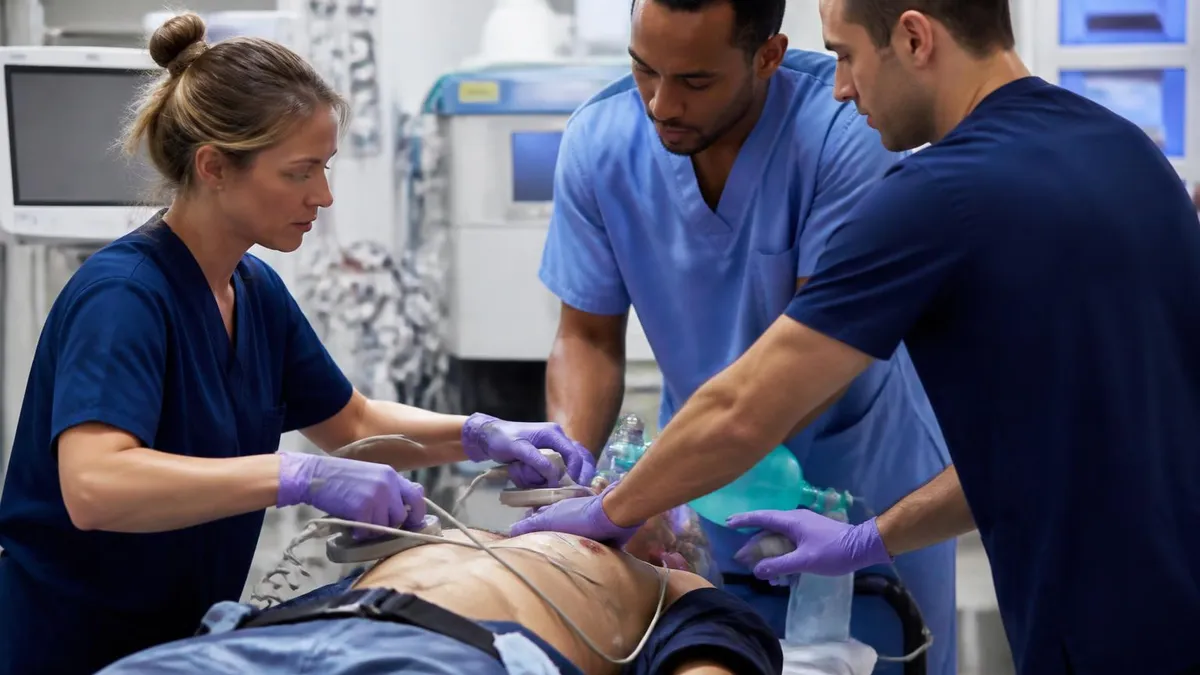
The ATLS course teaches a specific, systematic approach to trauma evaluation designed to be consistent across different providers, different hospitals, and different resource environments. The core framework is the primary survey: Airway (with cervical spine control), Breathing, Circulation, Disability (neurological status), and Exposure/Environment—the ABCDE sequence. This structured sequence ensures that life-threatening conditions are identified and addressed in order of immediate threat to life, rather than in the order in which injuries happen to be noticed.
After the primary survey and resuscitation, providers conduct the secondary survey—a head-to-toe examination designed to identify all injuries, including those not immediately life-threatening. The secondary survey includes history-taking using the AMPLE mnemonic (Allergies, Medications, Past medical history, Last meal, Events leading to injury) and a systematic physical examination of every body region. Together, the primary and secondary surveys form the backbone of the ATLS systematic approach.
ATLS training also covers adjuncts to the primary survey, including x-rays (chest and pelvis), FAST (Focused Assessment with Sonography in Trauma) ultrasound, and urinary catheter placement. The course addresses specific injury patterns in detail: airway emergencies, tension pneumothorax, massive hemothorax, cardiac tamponade, pelvic fractures with hemorrhage, traumatic brain injury, and spinal cord injuries. Special populations—pediatric trauma, geriatric trauma, obstetric trauma, and penetrating versus blunt mechanisms—are addressed as dedicated course components.
The ATLS student course is structured around alternating lecture and skills station sessions. Lectures provide the didactic framework for each content area, and skills stations allow participants to practice procedures under faculty supervision. The skills stations included in the current ATLS curriculum cover airway management and intubation, chest decompression, thoracostomy, assessment of the multiply injured patient, and trauma simulation scenarios in which participants manage a standardized patient through the full primary survey sequence. The simulation scenarios are evaluated by faculty observers using structured checklists.
The final assessment consists of a written multiple-choice examination covering ATLS principles, decision-making, and management priorities, as well as a practical skills examination. Participants must pass both components to receive ATLS certification. The written exam typically covers 50 questions; scores of 70% or higher are generally required to pass, though specific thresholds may vary slightly by program. Participants who do not pass on the first attempt may be given a single opportunity to remediate and retest before the end of the course, depending on the program's policies.
The ATLS curriculum is periodically revised and updated by the ACS Committee on Trauma based on evolving evidence in trauma care. The current edition of the ATLS Student Course Manual is the 10th edition, which introduced significant updates to hemorrhage control protocols (damage control resuscitation, permissive hypotension), the role of tranexamic acid (TXA) in trauma, and updated neurological assessment protocols. Participants receive the current edition of the manual as part of their course materials, and the course content aligns with the manual.
The 10th edition curriculum reflects the shift away from aggressive crystalloid resuscitation toward balanced blood product resuscitation using packed red blood cells, fresh frozen plasma, and platelets in roughly equal ratios—the “damage control resuscitation” approach. Permissive hypotension (targeting a systolic blood pressure of 80–90 mmHg rather than aggressive normalization) is now addressed for penetrating trauma without head injury, reflecting evidence that aggressive fluid administration in the pre-hemostasis phase worsens coagulopathy and mortality. TXA given within three hours of injury is formally included as a component of hemorrhage management, based on the CRASH-2 trial and its follow-on data.
ATLS courses are typically offered multiple times per year at major academic medical centers, regional trauma centers, and hospital systems with active trauma programs. Availability is higher in urban areas, where trauma volume justifies maintaining a local faculty of certified ATLS instructors.
Rural physicians who need to travel to reach the nearest accredited course may find it helpful to check with their state chapter of the American College of Surgeons for regional course listings, since many state chapters coordinate ATLS offerings to improve access for non-urban providers. Some programs offer traveling courses, bringing the training to smaller hospitals with sufficient registrant demand for a local cohort.
ATLS Student Course: What You'll Learn
| Section | Questions | Time |
|---|---|---|
| Primary Survey (ABCDE) | — | — |
| Secondary Survey & Adjuncts | — | — |
| Special Populations & Injury Patterns | — | — |
| Skills Stations | — | — |
ATLS Preparation: Strategy by Phase
Read the manual in advance: The ATLS Student Course Manual (10th edition) is typically distributed at registration or shortly before the course. Reading the chapters on shock, airway management, and thoracic trauma before arriving dramatically improves comprehension during the lecture sessions. Participants who arrive cold to the material spend cognitive resources absorbing new concepts rather than reinforcing and applying them.
Review airway algorithms: The airway management skills station is consistently the most challenging for participants who have limited intubation experience. Reviewing the ATLS airway decision tree—which covers jaw thrust, oral airway, bag-valve-mask, RSI, and surgical airway in sequence—before the skills station allows you to focus on technique rather than the decision framework during practice. Know the indications for a surgical airway and the cricothyrotomy technique steps before you arrive.
Practice the primary survey sequence: Verbalizing the ABCDE sequence out loud, including the actions at each step, prepares you for the simulation scenarios where faculty evaluate your systematic approach. Many high-scorers rehearse the primary survey sequence with a partner or in front of a mirror before the course, reinforcing the habit of working through each step in order rather than jumping to visible injuries.
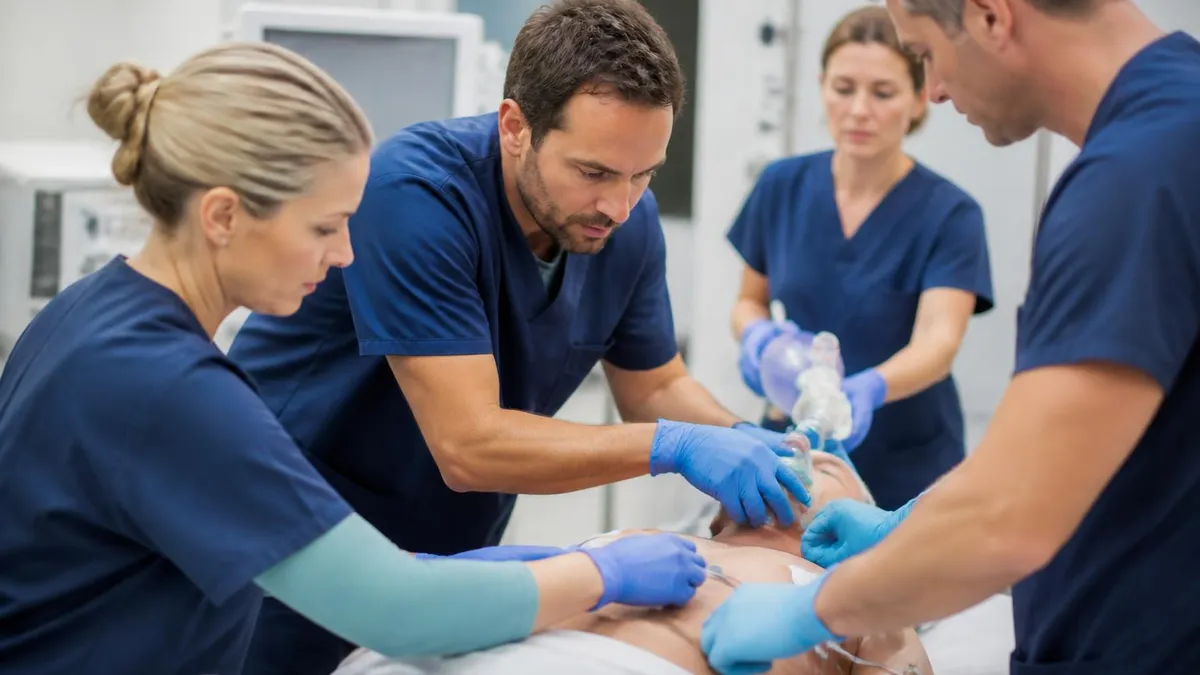
The ATLS student course was originally designed for physicians—specifically those who may be the first physician to evaluate a trauma patient. The ACS continues to define the primary audience as MDs and DOs with a license to practice medicine, though many programs have expanded eligibility in response to changes in advanced practice roles. The eligibility criteria that apply at a given course are determined by the national or regional program, not by individual faculty, so prospective attendees should verify eligibility directly with the sponsoring institution before registering.
In the United States, most ATLS programs require attendees to hold or be enrolled in a clinical medical education program. Medical students in their third or fourth year (MS3 or MS4) are often eligible to attend, particularly those rotating in surgery or emergency medicine. Physician assistants and nurse practitioners may be permitted at some programs, particularly at institutions that have adopted interprofessional trauma training models. Paramedics and flight nurses are generally not eligible for the physician-track ATLS student course but may be eligible for PHTLS (Prehospital Trauma Life Support), which is the prehospital equivalent of ATLS.
For international physicians, ATLS eligibility requirements vary by country. The ACS licenses the ATLS program to national trauma societies and surgical colleges in more than 80 countries, each of which administers their own courses under ACS guidelines. Some national programs have more flexible eligibility criteria than the U.S. program, particularly for non-physician trauma providers. International physicians seeking ATLS primarily for U.S. hospital credentialing purposes should confirm that the certifying authority—the ACS or its licensed national affiliate—is acceptable to the specific hospital or credentialing body.
The ATLS instructor course is a separate pathway for physicians who have completed the student course and wish to become certified faculty. Instructor candidates must have a current ATLS student certification, be nominated by an ATLS course director, and complete a 2-day instructor training program. ATLS instructors are essential to the ongoing operation of local programs and typically receive significant discounts or waivers for their own recertification. Many academic medical centers rely on a core group of ATLS instructors to run their local student courses throughout the year.
Physicians who cannot fund their ATLS registration out of pocket should check with their hospital or training program about continuing medical education (CME) reimbursement. ATLS typically qualifies for CME credit, and many hospitals maintain CME funds specifically to support attending physicians in maintaining required certifications. Residents and fellows whose training programs do not cover ATLS can often request coverage through their program director, particularly at institutions where ATLS is listed as a program requirement. Verifying reimbursement policies before registering avoids the frustration of paying out of pocket for a cost that could have been covered institutionally.
ATLS Key Concepts
What is the passing score for the ATLS exam?
Most ATLS exams require 70-75% to pass. Check the official exam guide for exact requirements.
How long is the ATLS exam?
The ATLS exam typically allows 2-3 hours. Time management is critical for success.
How should I prepare for the ATLS exam?
Start with a diagnostic test, create a 4-8 week study plan, and take at least 3 full practice exams.
What topics does the ATLS exam cover?
The ATLS exam covers multiple domains. Review the official content outline for the complete list.
How to Find and Register for an ATLS Course
- ✓Visit the ACS ATLS course search at facs.org — the official course finder lists all accredited U.S. and international programs
- ✓Verify eligibility for your specific professional degree (MD, DO, PA, NP, MS3/MS4) with the specific program before registering
- ✓Confirm the course is using the current 10th edition curriculum — older editions are no longer valid for new certifications
- ✓Register early — ATLS courses at major academic medical centers often fill several weeks to months in advance
- ✓Obtain a copy of the ATLS Student Course Manual (10th edition) and review the relevant chapters before the course start date
- ✓Prepare for the skills stations by reviewing ATLS algorithm flowcharts, FAST ultrasound views, and chest tube indications
- ✓Arrange the 2 full days off from clinical duties — most programs run 8 AM to 5 PM on consecutive days with no absences permitted
- ✓After passing, download your ATLS certificate from the ACS provider portal and update your CV and hospital credentialing files
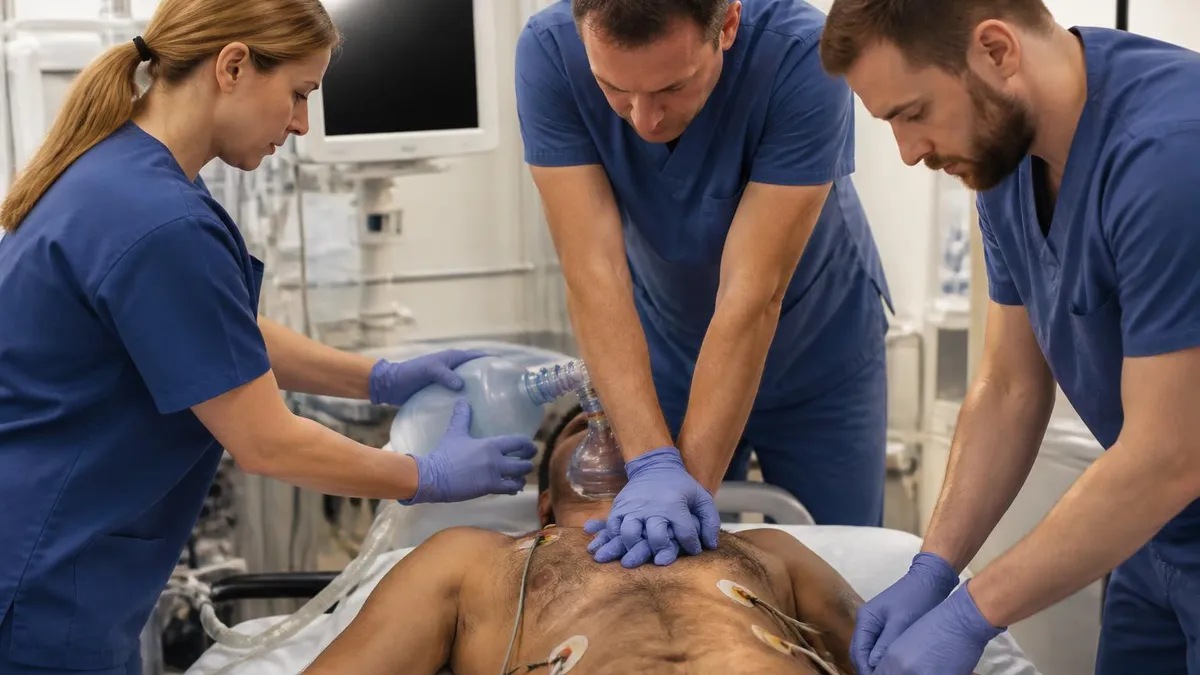
Preparing effectively for the ATLS student course significantly improves both pass rates and the quality of learning during the hands-on sessions. Participants who review the ATLS Student Course Manual (10th edition) chapters before arriving—particularly the chapters on shock, airway management, and thoracic trauma—report that the lecture content is easier to follow and the skills stations feel more productive. Familiarity with the ATLS algorithm structure (primary survey, adjuncts, resuscitation, secondary survey) allows participants to focus on applying the framework during simulation rather than memorizing it.
For the skills stations, reviewing the indications, contraindications, and procedural steps for needle decompression, chest tube thoracostomy, and rapid sequence intubation is the most high-yield preparation. Many participants find that going through the FAST exam protocol (four standard views, what positive findings look like) is time-efficient preparation that pays dividends during the simulation scenarios. The written exam draws heavily from the clinical decision-making scenarios in each chapter, so understanding the logic behind ATLS priorities matters more than rote memorization of isolated facts.
ATLS certification frequently appears as a requirement or strong preference in job postings for trauma surgery fellows, emergency medicine faculty, rural surgeons, military physicians, and international medical volunteers. The certification signals a demonstrated, standardized competency in initial trauma management that employers and credentialing committees can rely on without needing to assess each applicant individually.
Beyond credentialing requirements, ATLS training has practical clinical utility that extends throughout a career in trauma-adjacent medicine. The primary survey framework becomes instinctive after reinforcement through simulation and real patient encounters, enabling faster and more systematic evaluations during high-acuity trauma activations. Many experienced providers apply the ABCDE sequence to all critically ill patients—not only trauma—finding it equally useful for organizing the evaluation of septic shock, massive pulmonary embolism, or respiratory failure in the emergency department.
Hospitals that hold American College of Surgeons-verified trauma center status are required to demonstrate that their trauma providers maintain current ATLS certification as part of the ACS verification criteria. This institutional requirement drives high participation rates among trauma surgeons and emergency physicians at designated trauma centers and provides a recurring mechanism for keeping trauma teams aligned on systematic evaluation protocols across staff turnover and residency training cycles. Community hospitals seeking to develop or strengthen their trauma programs often use ATLS certification requirements as a foundation for standardizing their trauma team's initial assessment approach.
Military physicians who complete ATLS before deployment frequently find the systematic primary survey approach directly applicable to tactical casualty care. ATLS addresses the hospital phase of trauma management while Tactical Combat Casualty Care (TCCC) addresses the field phase, but both frameworks share the same underlying priorities: hemorrhage control, airway management, and rapid progression toward definitive care. Physicians who understand both frameworks are better equipped to integrate care across the continuum from point of injury through operative management.
For physicians working in resource-limited environments—rural hospitals, austere settings, or global health contexts—the ATLS systematic approach is especially valuable because it was designed to produce reliable outcomes regardless of available resources. Using ATLS practice tests and reviewing the ATLS certification guide before your course date can reinforce your knowledge of the framework and improve your readiness for the written assessment.
ATLS Training: Weighing the Investment
- +Universally recognized credential — ATLS certification is understood and respected by trauma programs, hospitals, and credentialing bodies worldwide
- +Systematic framework for trauma care that reduces cognitive error under pressure — valuable in every emergency and trauma setting
- +Practical skills training in airway management, chest decompression, and hemorrhage control builds procedural confidence alongside the didactic content
- +Valid for 4 years — the recertification burden is reasonable relative to most medical credentialing requirements
- +Available internationally in 80+ countries, making it accessible for physicians trained abroad or working in global health contexts
- −Course cost of $775–$1,200 can be a barrier, particularly for residents and fellows not funded by their training programs
- −Eligibility is primarily physician-focused — non-physician advanced practice providers may face restrictions at some programs
- −The 2-day time commitment requires two full clinical days off, which can be difficult to schedule during demanding training or practice periods
- −Course availability varies geographically — rural physicians may need to travel to reach the nearest accredited ATLS program
- −Certification must be renewed every 4 years, requiring ongoing time and financial investment throughout a career
ATLS Training Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.