ATLS Certification Guide: Advanced Trauma Life Support Course and Exam
ATLS certification guide: course format, exam structure, skill stations, ABCDE assessment framework, renewal requirements, and who needs ATLS.
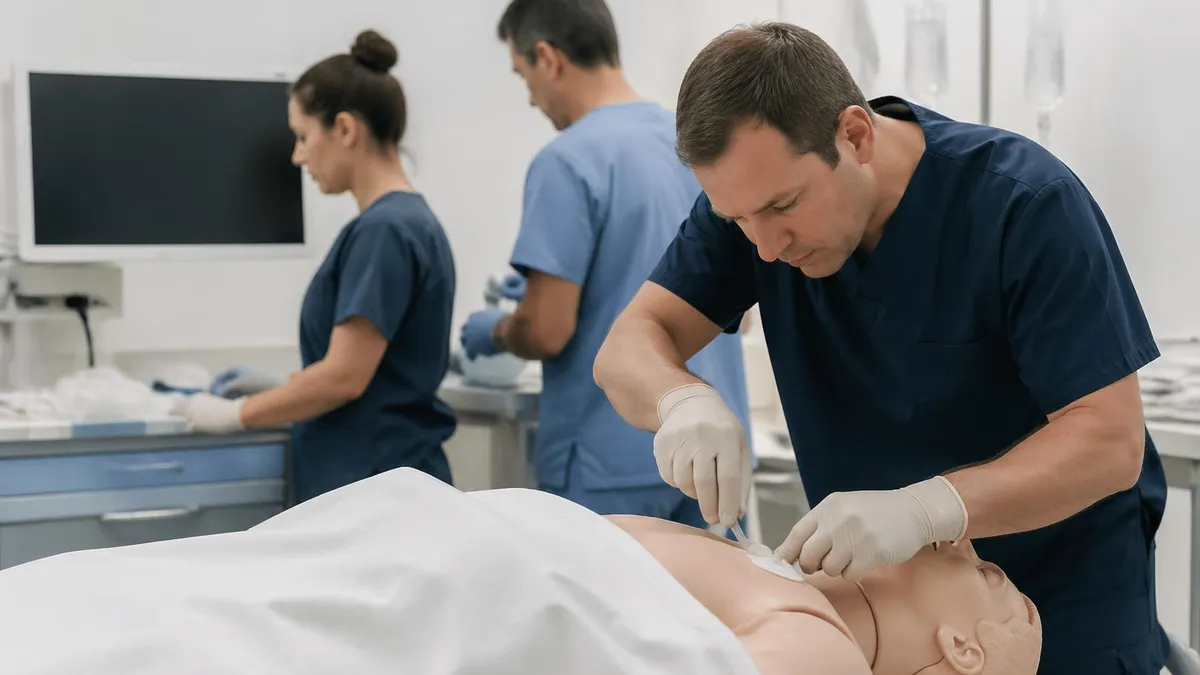
ATLS Certification: What It Is and Who Needs It
Advanced Trauma Life Support (ATLS) is the standardized trauma training program developed and administered by the American College of Surgeons (ACS). Since its introduction in 1978, ATLS has become the global standard for initial trauma assessment and management, now taught in more than 80 countries and used as the foundational framework for trauma care in hospitals, emergency departments, and military medical settings worldwide. The program teaches a systematic, prioritized approach to the multiply-injured patient — the ABCDE framework (Airway, Breathing, Circulation, Disability, Exposure) — designed to identify and treat life-threatening injuries in the correct order, regardless of the complexity or mechanism of the trauma presentation. ATLS certification is required or strongly recommended for emergency physicians, trauma surgeons, general surgeons, orthopedic surgeons, anesthesiologists, and neurosurgeons who manage trauma patients; it is also increasingly required in residency training programs and by hospital credentialing committees for trauma call coverage.
The core principle of ATLS — treat the greatest threat to life first — organizes the entire course curriculum and examination. The primary survey addresses life-threatening problems in the ABCDE sequence: Airway maintenance with cervical spine protection, Breathing and ventilation, Circulation with hemorrhage control, Disability (neurologic status), and Exposure with environmental control. The secondary survey, conducted only after the primary survey is complete and the patient is hemodynamically stable, performs a head-to-toe examination identifying all injuries. This two-survey framework is the lens through which every ATLS topic is taught and tested. Practicing with ATLS initial assessment and management practice tests reinforces the primary survey sequence, decision points, and intervention priorities that form the foundation of every ATLS scenario. Working through ATLS airway and ventilatory management practice tests covers the airway assessment, intubation decision algorithm, surgical airway indications, and ventilatory support content that the ATLS course addresses as the first and most critical primary survey priority.
ATLS is not a course about performing procedures independently — it is a course about assessment priorities, decision-making, and systematic management of the trauma patient within a team. The skills stations teach specific procedural competencies (airway management, chest tube placement, diagnostic peritoneal lavage, extremity immobilization) but the examination emphasizes the cognitive framework: recognizing which intervention is needed next and why. Candidates who approach ATLS preparation focused purely on procedure memorization are less prepared than those who internalize the ABCDE framework and practice applying it to increasingly complex trauma scenarios. Reviewing ATLS shock assessment and management practice tests covers the four shock classes, fluid resuscitation decision points, and the circulation assessment framework that the ATLS primary survey addresses immediately after airway and breathing are stabilized. Completing ATLS head trauma practice tests covers the Glasgow Coma Scale, herniation signs, intracranial pressure management principles, and neurosurgical consultation indications that the ATLS disability assessment addresses in the primary survey.
ATLS Course Format and What to Expect
The ATLS provider course runs approximately 2.5 days for first-time candidates. Day one combines didactic sessions covering each major trauma system, small group skill stations, and pre-course independent study review. Day two and the morning of day three include additional skill stations, the Objective Structured Clinical Examination (OSCE) scenarios where candidates manage simulated trauma patients through the primary and secondary survey, and the 40-question written examination. The written exam requires a score of 75% or higher to pass; skill station and OSCE performances are assessed pass/fail against standardized performance criteria. Candidates who fail the written exam or a skill station may have a single remediation opportunity during the course; those who do not achieve passing performance leave the course without certification and must retake. Practicing with ATLS triage and mass casualty incidents practice tests covers the START triage algorithm, resource-limited trauma management, and mass casualty decision-making that the ATLS course addresses as a distinct module beyond the individual patient framework.
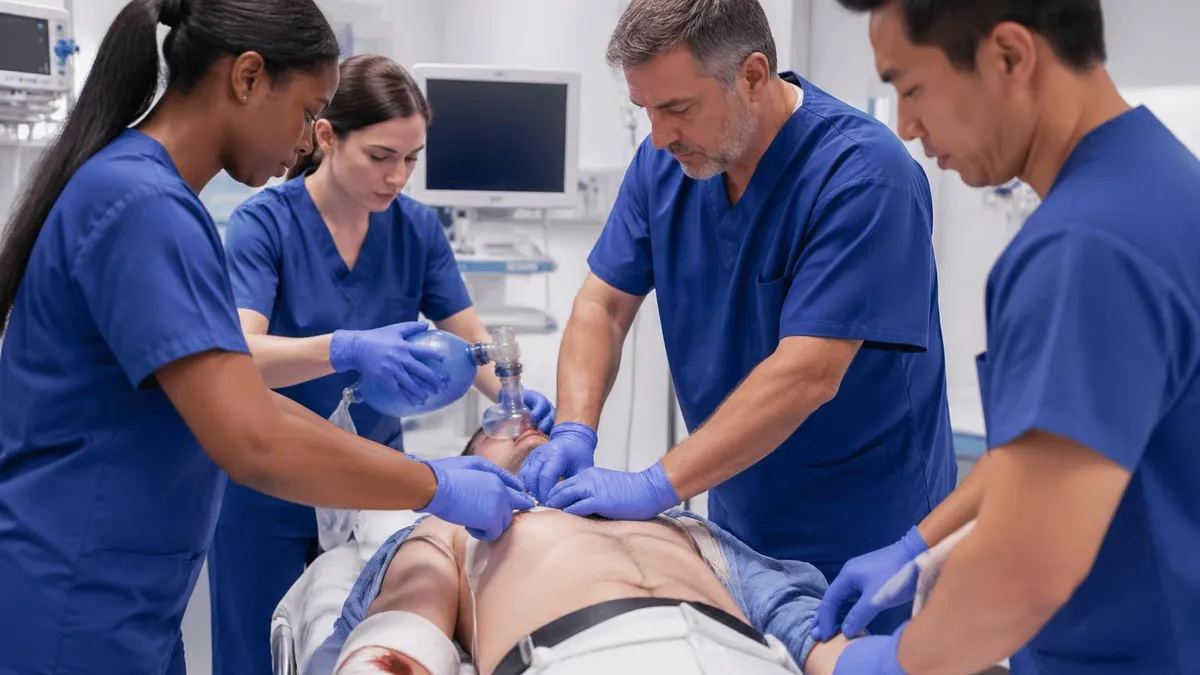
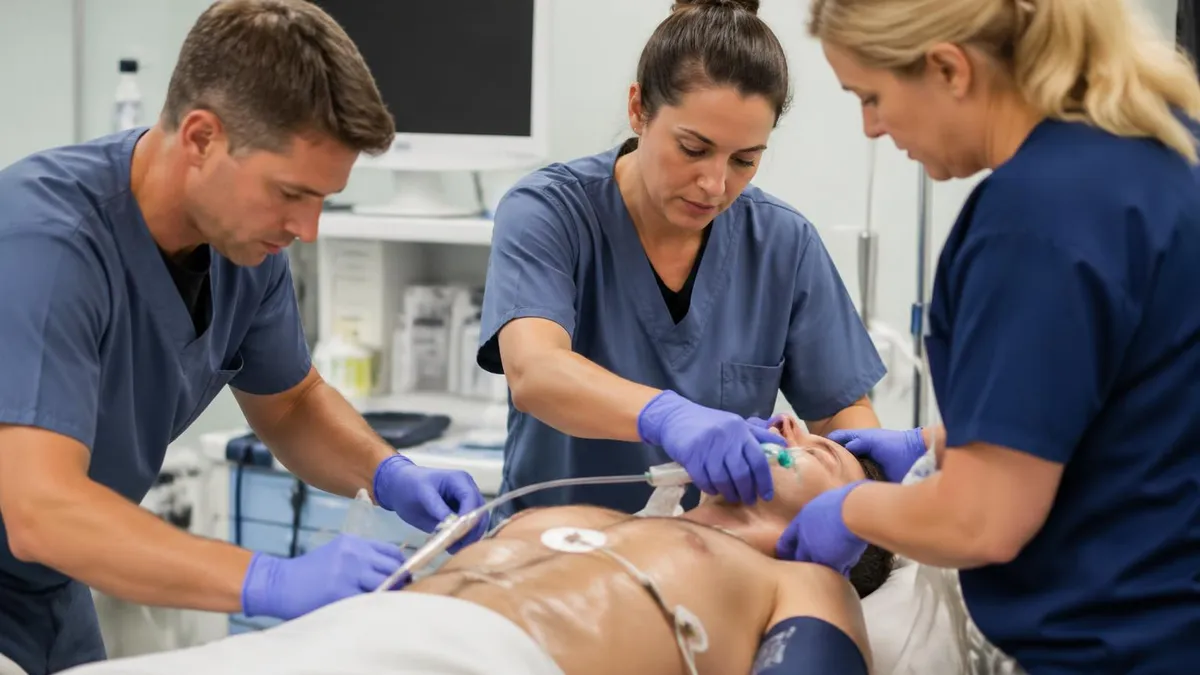
ATLS Overview
- Emergency medicine physicians: ATLS is a core competency for emergency medicine; most residency programs require or strongly recommend ATLS certification during training
- Surgical residents and attendings: Trauma surgery, general surgery, and orthopedic surgery practitioners managing trauma patients; many hospital trauma committees require current ATLS for trauma call privileges
- Anesthesiologists: Called to trauma resuscitations and airways; ATLS provides the trauma assessment framework and systemic injury management context
- Neurosurgeons: Head and spine trauma management is a major ATLS module; ATLS reinforces the disability assessment and intervention thresholds relevant to neurosurgical consultation
- Advanced practice providers: Nurse practitioners and physician assistants working in emergency medicine and trauma surgery settings; many hospitals require ATLS for APP trauma team roles
- Military and austere environment providers: ATLS is foundational for military combat casualty care training; variants exist for prehospital and resource-limited environments
ATLS Breakdown
- ▸Airway management station: oropharyngeal and nasopharyngeal airway insertion, bag-valve-mask technique, laryngoscopy and intubation, surgical airway (cricothyrotomy) on a mannequin, and recognition of esophageal intubation
- ▸Thoracic trauma station: needle decompression for tension pneumothorax, chest tube thoracostomy technique, assessment for tension pneumothorax vs. massive hemothorax vs. open pneumothorax, and pericardiocentesis for cardiac tamponade
- ▸Abdominal and pelvic assessment: FAST exam interpretation on case images, diagnostic peritoneal lavage procedure and interpretation, pelvic fracture assessment and temporary stabilization technique
- ▸Shock resuscitation station: IV access including intraosseous access, central venous access technique, blood product selection and massive transfusion protocol activation criteria, end-points of resuscitation
- ▸Immobilization station: long bone fracture splinting techniques, spinal motion restriction, extremity vascular injury recognition, compartment syndrome assessment and fasciotomy indications
- ▸Pediatric and burn modules: burn surface area estimation (rule of nines), burn fluid resuscitation (Parkland formula), pediatric GCS modification, physiologic differences in pediatric trauma response
- ▸Study the ATLS Student Manual before the course: the 10th edition covers all written exam content; reading it cover-to-cover before attending is the most effective preparation strategy
- ▸Master the ABCDE primary survey sequence: be able to name the complete primary survey, the key assessments at each step, and the life-threatening conditions each step is designed to catch
- ▸Memorize the shock classification table: Classes I through IV by estimated blood loss, heart rate, blood pressure, respiratory rate, GCS, urine output, and base deficit -- high-yield for both written exam and scenario management
- ▸Learn the Glasgow Coma Scale in detail: eye opening (1-4), verbal response (1-5), motor response (1-6); know what GCS 8, 13, and 15 each indicate clinically and their intervention thresholds
- ▸Review thoracic emergency recognition: know the immediate life threats (tension pneumothorax, open pneumothorax, massive hemothorax, flail chest, cardiac tamponade, aortic disruption) and their distinguishing features
- ▸Practice scenarios aloud: rehearsing the verbal presentation of a primary survey reduces cognitive load during the OSCE and builds the systematic habit ATLS assessors look for
- ▸ATLS scope: trauma patients only -- systematic assessment and management of patients with injuries from any mechanism (blunt, penetrating, burns, blast); addresses hemorrhage, airway, thoracic injuries, head/spine trauma, abdominal trauma
- ▸ACLS scope: cardiac arrest and peri-arrest arrhythmias -- the American Heart Association course covers CPR, defibrillation, ACLS algorithms (VFIB, VTACH, asystole, PEA), and post-cardiac arrest care; no trauma content
- ▸PALS scope: pediatric emergencies -- covers pediatric assessment triangle, respiratory and circulatory failure recognition, cardiac arrest management in children; complements ATLS for pediatric trauma
- ▸ALSO (Advanced Life Support in Obstetrics): addresses maternal emergencies including obstetric trauma; ATLS covers trauma in pregnancy as a special population module
- ▸Who needs all three: emergency medicine physicians typically hold ATLS + ACLS + PALS as a standard certification package; surgeons primarily need ATLS; intensivists typically hold ACLS + ATLS
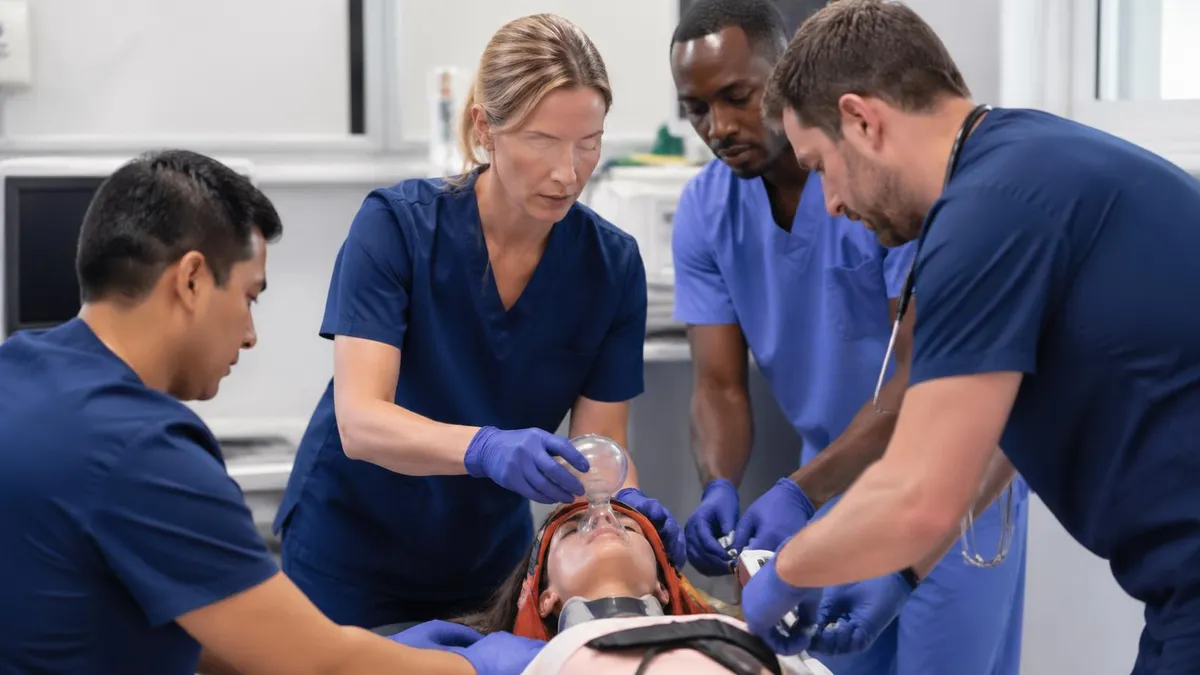
Maximizing Your ATLS Course Performance
Candidates who perform best on the ATLS written exam and OSCE scenarios are those who understand the underlying reasoning behind the ABCDE framework, not just the steps in isolation. The written exam presents clinical scenarios where you must identify which component of the primary survey has been neglected, which life-threatening condition has been missed, or which next intervention is most appropriate given the patient's current status. These questions test clinical decision-making within the ATLS framework, not recall of isolated facts. For example, a question presenting a trauma patient with distended neck veins, absent breath sounds, and hypotension after a chest injury is testing whether you recognize tension pneumothorax — and that the correct immediate intervention is needle decompression before chest X-ray, before CT, before anything else. Reviewing ATLS spine and spinal cord trauma practice tests covers the spinal cord injury assessment, neurogenic vs. spinal shock distinction, and clearance protocols that the disability component of the primary survey addresses in trauma patients with altered neurological status. Working through ATLS musculoskeletal trauma practice tests covers extremity injury assessment, compartment syndrome recognition, vascular injury evaluation, and the splinting and stabilization techniques covered in the skills stations.
The OSCE scenarios test your ability to manage a simulated trauma patient from initial presentation through the primary survey, resuscitation decisions, and disposition — all while communicating your assessment and reasoning aloud to the ATLS assessors. Candidates who think aloud during scenarios consistently perform better because assessors can only score what they observe; silent correct reasoning is indistinguishable from no reasoning in the OSCE format. Practice narrating your assessment out loud during preparation: call the airway assessment, announce your finding, state your intervention. This verbal rehearsal is the preparation that most candidates skip and that most commonly differentiates strong OSCE performance from marginal performance. Reviewing ATLS abdominal and pelvic trauma practice tests covers the assessment approach, FAST exam integration, damage control decision-making, and pelvic hemorrhage management that the abdominal component of the secondary survey addresses. Completing ATLS ocular and facial trauma practice tests covers facial fracture assessment, eye injury evaluation, and the airway implications of maxillofacial trauma that are high-yield for the ATLS written examination scenarios involving upper airway compromise.
Building a structured study plan before attending the ATLS course significantly improves both confidence and exam performance. Candidates who allocate dedicated daily sessions over two to three weeks before the course consistently report feeling prepared for both the written exam and OSCE scenarios. A practical preparation schedule covers the ATLS Student Manual chapter by chapter, following the primary survey structure: start with the overview chapter and initial assessment, work through each injury system (airway, thorax, abdomen, musculoskeletal, head, spine), and finish with special populations (pediatric, burn, geriatric, pregnant patients). Practice questions after each chapter reinforce recognition of the patterns each topic tests — tension pneumothorax signs, shock class differentiation, GCS scoring, and the specific indications for procedural interventions. Candidates who arrive at the course having already visualized the ABCDE primary survey sequence multiple times through practice can focus their cognitive bandwidth on the nuances and edge cases the OSCE scenarios introduce, rather than working to recall the basic framework under pressure for the first time. The investment in pre-course preparation pays dividends not only during certification but throughout a clinical career in which the systematic approach to trauma assessment becomes second nature. Physicians who trained with ATLS consistently report that the ABCDE framework remains the mental model they reach for first in every trauma resuscitation, regardless of how many years have passed since the course.
ATLS Pros and Cons
- +Global recognition -- ATLS is recognized in 80+ countries as the standard trauma training framework; certification earned in one ACS-affiliated country is valid worldwide for clinical credentialing purposes
- +Systematic framework -- the ABCDE approach provides a cognitive framework that prevents missed injuries under pressure; practitioners report using the primary survey mental model throughout their careers
- +Required for trauma privileges -- most Level I and II trauma centers require current ATLS for trauma call coverage; completing ATLS opens clinical opportunities otherwise unavailable
- +Evidence-based curriculum -- the 10th edition reflects current evidence on permissive hypotension, damage control resuscitation, and other evolved trauma practices; the curriculum updates with practice changes
- +Team-based skills -- ATLS teaches communication and team leadership within trauma resuscitation, not just individual procedural competency; these skills transfer directly to real resuscitations
- −Cost -- the ATLS provider course runs $700-$1,000+ depending on location and institution; recertification every 4 years adds ongoing cost for providers maintaining the credential long-term
- −Time commitment -- 2.5 days away from clinical responsibilities is a significant scheduling challenge for residents and attendings with demanding call schedules
- −Pre-reading required -- the ATLS Student Manual must be studied before the course; candidates who arrive without pre-course preparation consistently underperform on both the written exam and skills stations
- −Focused scope -- ATLS covers initial assessment and stabilization, not definitive care; practitioners needing depth in specific trauma subspecialties require additional training beyond ATLS
- −4-year renewal burden -- unlike some certifications with longer validity periods, 4-year renewal means practicing physicians recertify multiple times per career, each requiring time and expense
ATLS Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.