BLS Algorithm: Step-by-Step Guide to Basic Life Support Protocols
Complete guide to the BLS algorithm covering adult, child, and infant resuscitation sequences, CPR steps, AED use, team dynamics, and protocol updates.

The BLS algorithm provides a standardized sequence of actions trained rescuers follow when responding to cardiac arrest, choking, and other life-threatening emergencies. Developed by the American Heart Association and revised every five years based on the latest resuscitation science, the algorithm guides healthcare providers, professional rescuers, and trained laypeople through the critical first minutes of an emergency. Following the algorithm consistently produces better outcomes than improvising responses or skipping steps that intuition might suggest are unnecessary.
Cardiac arrest is the leading cause of death in adults in the United States with approximately 350,000 out-of-hospital cardiac arrests occurring each year. Survival rates remain low at roughly 10 percent though high-quality bystander CPR combined with rapid AED use can double or triple survival chances. The BLS algorithm exists to maximize the impact of trained rescuers during the precious minutes before advanced medical care arrives. Every step in the algorithm has a specific purpose grounded in research showing it improves outcomes for victims of cardiac arrest or respiratory emergencies.
This guide walks through the complete adult BLS algorithm, the pediatric BLS algorithm for children and infants, and the special considerations that change the standard sequence. Anyone preparing for BLS certification, recertification, or healthcare provider examinations can use this resource to study the steps, understand the reasoning behind each action, and practice mental rehearsal of emergency responses. Mental rehearsal supplements hands-on training and helps ensure that when a real emergency happens, the correct sequence flows automatically without hesitation or confusion.
The adult BLS algorithm follows the sequence: scene safety, check responsiveness, call for help and AED, check breathing and pulse simultaneously for no more than 10 seconds, begin CPR with 30 compressions and 2 breaths if no pulse, attach the AED as soon as it arrives, and continue cycles until advanced help takes over. Compression rate is 100 to 120 per minute at a depth of at least 2 inches for adults. Minimize interruptions and rotate compressors every 2 minutes to prevent fatigue.
Scene safety is always the first step before approaching any victim. Rescuers who become victims themselves cannot help anyone and add to the emergency. Common scene hazards include traffic, electrical hazards, fire, hazardous materials, violent people, unstable structures, and infectious disease exposure. Quick scene assessment takes only seconds and is non-negotiable regardless of how urgent the medical emergency appears. Personal protective equipment including gloves and a barrier device for rescue breathing should be used when available to prevent infectious disease transmission during patient contact.
Checking responsiveness involves tapping the victim firmly on the shoulder and shouting loudly to determine whether they can respond. The shout should be specific and loud enough to wake someone in deep sleep. If the victim responds verbally, moves purposefully, or opens their eyes, they are not in cardiac arrest and need different assessment focused on their specific complaint. Unresponsive victims who do not move, do not open their eyes, and make no sound require immediate progression through the algorithm to activate emergency response and assess for breathing and pulse.

Adult BLS Algorithm Steps
Scan the area for hazards including traffic, electrical dangers, fire, and violent people. Move the victim only if remaining in place creates ongoing danger that cannot be controlled.
Tap the shoulder firmly and shout loudly to assess for response. Lack of response, movement, or eye opening indicates unresponsiveness requiring full algorithm activation.
Shout for nearby help, call 911 or designate someone to call, and request an AED. In hospital settings, activate the code team using facility-specific procedures.
Scan the chest for normal breathing while simultaneously palpating the carotid pulse for no more than 10 seconds. Gasping is not normal breathing.
If no normal breathing and no definite pulse, begin chest compressions immediately. Use 30 compressions followed by 2 breaths if trained in rescue breathing.
Attach the AED pads as soon as the device arrives. Follow voice prompts for analysis and shock delivery. Resume compressions immediately after shock or no-shock advice.
Activating the emergency response system happens immediately after confirming unresponsiveness. In community settings, this means calling 911 directly if alone or directing a specific person nearby to call while pointing at them and giving clear instructions. Vague requests like asking the crowd to call for help often fail because each bystander assumes someone else will act. Specific designation eliminates this bystander effect and ensures the call actually happens. The caller should provide location, nature of emergency, and any landmark information that helps dispatch route emergency services efficiently to the scene.
Requesting an AED happens simultaneously with the 911 call because defibrillation is the definitive treatment for the most common shockable cardiac arrest rhythms. Public access AEDs are increasingly available in airports, schools, gyms, casinos, and other public spaces. The dispatcher can often direct callers to the nearest AED location if one is available nearby. Every minute defibrillation is delayed reduces survival by approximately 10 percent making rapid AED acquisition one of the most impactful actions trained rescuers can take during cardiac arrest response.
BLS Algorithm by Age Group
Adult BLS applies to victims past the onset of puberty. The compression to ventilation ratio is 30:2 for single rescuer CPR and remains 30:2 for two-rescuer CPR. Compression depth is at least 2 inches but not more than 2.4 inches. Compression rate is 100 to 120 per minute. Allow complete chest recoil between compressions. Two-rescuer teams should switch compressor roles every 2 minutes or sooner if the compressor becomes fatigued because compression quality degrades significantly when rescuers tire.
Checking for breathing and pulse happens simultaneously to minimize delays in starting compressions. Look at the chest for movement consistent with normal breathing while placing two fingers on the carotid artery in the neck. The carotid pulse check is for healthcare providers and professional rescuers because lay rescuers often have difficulty reliably finding a pulse and may delay critical compressions trying.
The entire assessment should take no more than 10 seconds. If there is any doubt about pulse presence or breathing adequacy, default to starting compressions because the risk of delayed CPR exceeds the risk of compressions in someone who has a pulse.
Agonal gasping is a common finding in early cardiac arrest and represents a respiratory pattern that is not normal breathing. Agonal gasps appear as occasional, irregular gasping movements that may include audible noises but provide no effective ventilation. Recognizing agonal breathing as abnormal is critical because rescuers who interpret these gasps as normal breathing dangerously delay starting CPR. When in doubt about whether breathing is normal, assume it is not normal and proceed with the algorithm. Pulse checks taking longer than 10 seconds delay compressions unnecessarily and should be abandoned in favor of beginning CPR.
Never delay starting chest compressions to perform a perfect assessment. The pulse check should take no more than 10 seconds total. If you cannot definitely feel a pulse within that window, begin compressions immediately. Research consistently shows that delays in starting compressions reduce survival far more than the small risk of doing compressions on someone with a faint pulse you missed. When in doubt, push hard and push fast.
High-quality chest compressions form the foundation of successful resuscitation. The current guidelines specify compression depth of at least 2 inches but not more than 2.4 inches in adults, with similar proportional depths in children and infants based on chest size. Compression rate should fall between 100 and 120 per minute, which corresponds to the beat of several familiar songs including the Bee Gees Stayin Alive. Allow complete chest recoil between compressions because incomplete recoil reduces venous return to the heart and decreases the effectiveness of subsequent compressions in maintaining cardiac output.
Hand placement matters for both effectiveness and safety. The heel of one hand goes on the center of the chest on the lower half of the sternum with the second hand on top with interlocked fingers. The rescuer position should be directly over the chest with elbows locked and shoulders directly above the hands. Body weight rather than arm strength generates compression force, which both produces deeper compressions and reduces rescuer fatigue. Rescuers should count compressions out loud during the cycle to maintain rhythm and help track when to deliver rescue breaths after each set of 30.
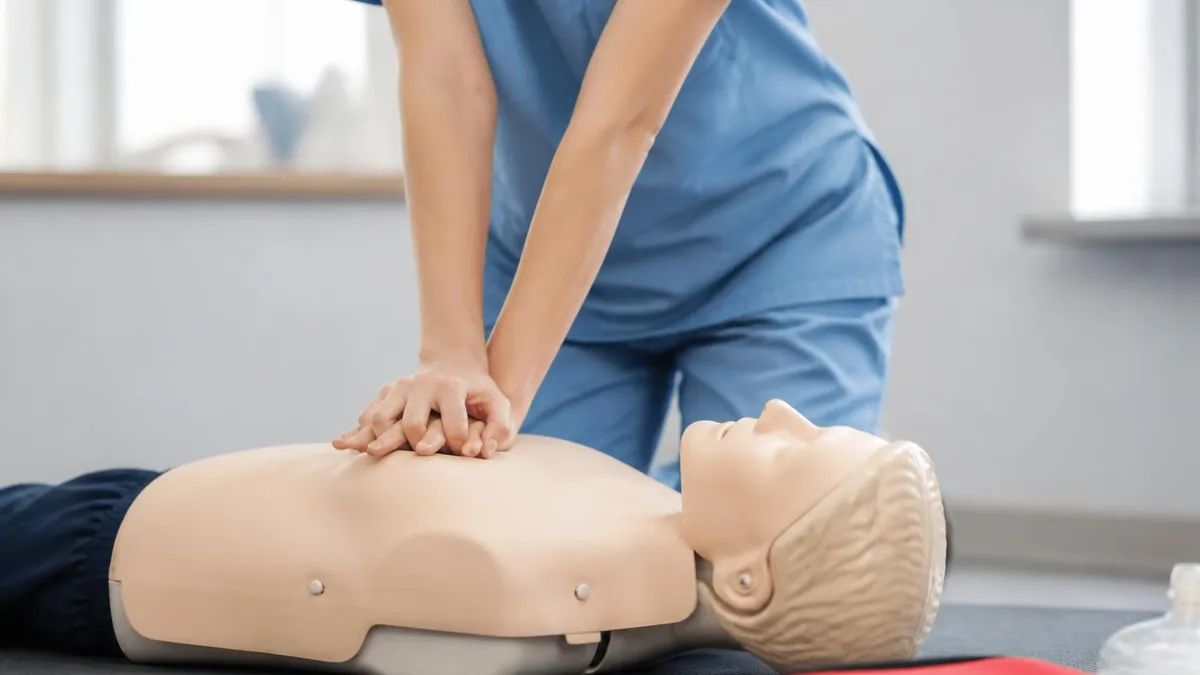
High-Quality CPR Checklist
- ✓Verify scene safety before approaching the victim and use personal protective equipment when available
- ✓Confirm unresponsiveness with shoulder tap and loud verbal stimulus before activating emergency response
- ✓Activate 911 and request an AED with specific direction to nearby helpers, not vague crowd requests
- ✓Check breathing and pulse simultaneously for no more than 10 seconds before starting compressions
- ✓Compress at a rate of 100 to 120 per minute at a depth of at least 2 inches in adults
- ✓Allow complete chest recoil between compressions and minimize interruptions to less than 10 seconds
- ✓Rotate compressor role every 2 minutes or sooner if fatigue affects compression quality
- ✓Attach the AED immediately upon arrival and follow voice prompts for analysis and shock delivery
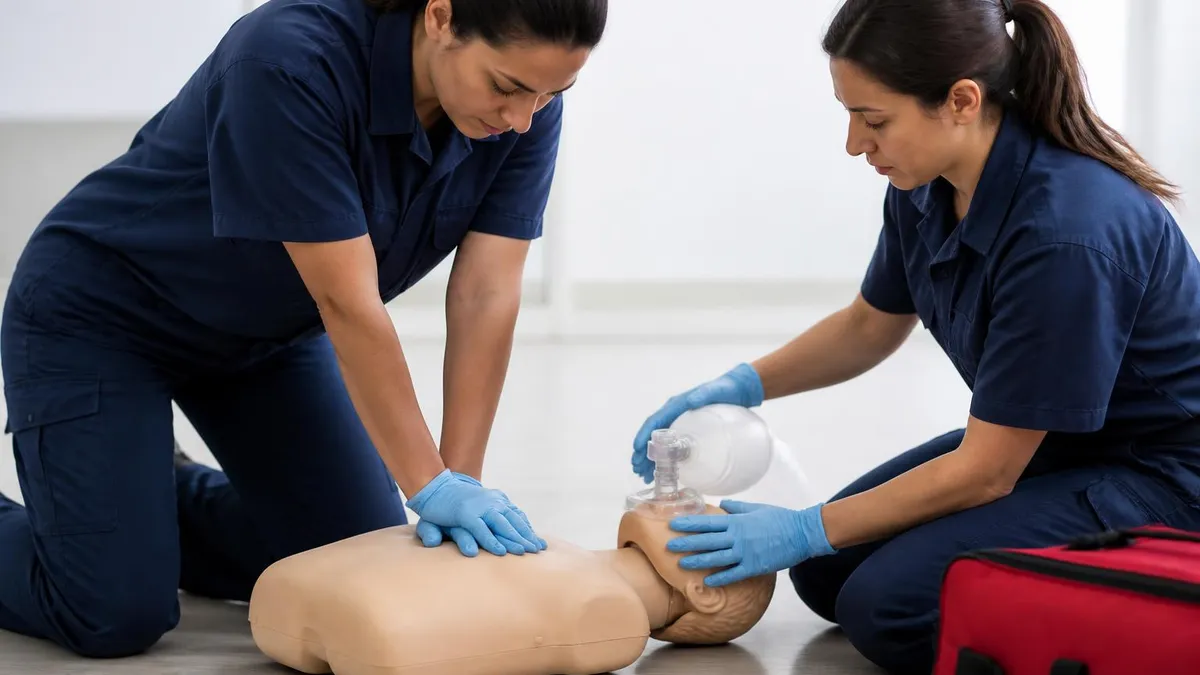
Rescue breathing requires an open airway and a proper seal during ventilation. The head tilt chin lift maneuver opens the airway in victims without suspected spinal injury. The jaw thrust maneuver maintains spinal alignment for trauma patients with possible cervical injury. Each rescue breath should last about 1 second and produce visible chest rise. Avoid excessive ventilation volumes or rates because hyperventilation increases intrathoracic pressure, decreases venous return, and reduces cardiac output. The goal is the minimum effective ventilation rather than maximum vigorous breathing that intuition might suggest is better.
Barrier devices reduce infection risk during rescue breathing. Pocket masks with one-way valves are the preferred barrier for single rescuers because they create a good seal and prevent backflow of fluids or air from the victim. Bag valve mask devices require two rescuers for optimal use with one maintaining the seal while the other squeezes the bag. Lone rescuers without a barrier device may consider compression-only CPR which research shows is acceptable for adult cardiac arrest of cardiac origin though full CPR with breaths remains preferred for respiratory arrests, drowning, and pediatric patients.
AED operation follows a consistent pattern across manufacturers though specific device interfaces vary slightly. Power on the device, attach the pads to bare skin following diagrams on the pads, ensure no one is touching the victim, and follow voice prompts for rhythm analysis. Modern AEDs analyze the rhythm automatically and advise either shock or no shock based on whether the rhythm is shockable. Shockable rhythms include ventricular fibrillation and pulseless ventricular tachycardia. Non-shockable rhythms include asystole and pulseless electrical activity which require continued CPR without defibrillation.
Pad placement matters for effective defibrillation. Standard anterolateral placement positions one pad on the upper right chest below the clavicle and the other on the left lateral chest below the armpit. Some manufacturers use anteroposterior placement with one pad on the chest and the other on the back.
Pediatric pads or attenuated dose adapters should be used for children under 8 years old or under 25 kg though adult pads may be used if pediatric pads are not available. Avoid placing pads over medication patches, implanted devices, jewelry, or excessive body hair, which may require quick removal or shaving for proper contact.
BLS Performance Metrics
Team dynamics become critical when multiple rescuers respond together to a cardiac arrest. Clear role assignment prevents confusion and ensures all necessary tasks happen efficiently. Common team roles include team leader, compressor, ventilator, AED operator, and recorder or timer. The team leader oversees the resuscitation, makes decisions, and ensures algorithm adherence without performing hands-on tasks that would compromise oversight. Closed-loop communication confirms that orders given by the team leader are heard, understood, and completed by the receiving team member. This communication style reduces errors and missed tasks during high-stress events.
Constructive intervention by team members can prevent errors when individual rescuers notice problems with the resuscitation. A compressor who notices the team leader has forgotten to check the rhythm at the 2-minute mark should speak up. A ventilator who sees compression depth is inadequate should respectfully suggest the compressor push harder. Effective teams welcome this kind of input because errors caught during the event are easier to fix than problems identified only during debriefing afterward. Hierarchical workplace cultures that suppress junior team member input often produce worse resuscitation outcomes than flatter team structures.
Common BLS Algorithm Errors
Spending too long on pulse checks or trying to verify breathing delays the start of compressions, reducing survival probability with each second lost.
Compressions less than 2 inches deep do not produce adequate cardiac output. Rescuer fatigue often produces progressively shallower compressions requiring rotation.
Leaning on the chest between compressions prevents full recoil and reduces venous return. Lift hands slightly between each compression to allow complete chest expansion.
Hyperventilation increases intrathoracic pressure and reduces cardiac output. Give breaths just large enough to produce visible chest rise, not maximum lung volume.
Pausing compressions for pulse checks, intubation attempts, or other tasks reduces survival. Limit pauses to less than 10 seconds and resume compressions immediately.
Delays attaching the AED reduce shock effectiveness. Apply pads as soon as the device arrives and minimize the pause between compressions and shock delivery.
Choking emergencies trigger a different sequence within the broader BLS framework. A conscious adult or child with severe airway obstruction who cannot speak, cough, or breathe needs abdominal thrusts also known as the Heimlich maneuver. Stand behind the victim, place a fist with thumb side against the abdomen just above the navel, grasp the fist with the other hand, and deliver inward and upward thrusts until the object dislodges or the victim becomes unresponsive. For infants under 1 year, use alternating sets of five back blows and five chest thrusts rather than abdominal thrusts which can cause internal injury.
If a choking victim becomes unresponsive, lower them safely to the ground and begin CPR starting with chest compressions. Before delivering rescue breaths, look in the mouth for a visible obstructing object and remove it with a finger sweep only if you can see it. Blind finger sweeps risk pushing the object deeper and are not recommended. Continue CPR cycles until the object is dislodged, the victim recovers, or advanced medical personnel take over the resuscitation. Successful object removal in a victim who has become unresponsive often happens during chest compressions which generate sufficient pressure to expel the obstruction.
Compression-Only vs Standard CPR
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
BLS certification typically lasts two years before requiring renewal through a refresher course. Healthcare providers including nurses, physicians, paramedics, dental staff, and many allied health professionals are required to maintain current BLS certification as a condition of employment. Lay rescuer BLS courses are widely available through the American Heart Association, the American Red Cross, the National Safety Council, and other approved providers. Many courses now offer blended learning that combines online coursework with brief in-person skills practice and testing, reducing total class time while preserving hands-on skill assessment.
Skill retention degrades quickly after initial training even among professionals who use BLS skills regularly. Studies show that compression quality begins to decline within months of training and that recertification at standard two-year intervals leaves substantial windows when skill performance is suboptimal. Many organizations now supplement standard recertification with brief monthly or quarterly practice sessions on training manikins with feedback devices that measure compression rate, depth, and recoil. These low-stakes practice sessions reinforce muscle memory and identify areas needing improvement before they affect a real resuscitation event.
Study Tips for BLS Exams
- ✓Practice running through the algorithm out loud from memory until the sequence flows without effort or hesitation
- ✓Use scenario cards or online practice tests that simulate realistic emergencies and require selecting the next step
- ✓Memorize key numbers including compression rate, depth, ratios, and time limits that appear on written exams
- ✓Watch high-quality demonstration videos of two-rescuer CPR and AED operation to internalize team choreography
- ✓Pair classroom training with regular feedback-device manikin practice to maintain skill between certification cycles
Documentation requirements for BLS events have grown stricter in many healthcare settings as part of broader quality improvement programs. Code documentation typically includes time of arrest recognition, time CPR started, intervals between compression rotations, shock delivery times and energies, medications given by ACLS providers, time of return of spontaneous circulation if achieved, and disposition of the patient. Time stamps from defibrillator data and continuous capnography monitoring now provide objective measurement of compression quality, ventilation rate, and physiological response to resuscitation efforts that supplements observer-recorded data during the event.
Family presence during resuscitation has become more common as research shows that allowing relatives to witness CPR efforts often reduces grief and provides closure even when resuscitation is unsuccessful. A designated team member, often a chaplain or social worker, supports family members during the event, explains what is happening, and ensures families do not interfere with the resuscitation. Surveys consistently show that family members who choose to be present report positive experiences while families excluded from rooms often report wondering whether everything possible was done.
Return of spontaneous circulation is the immediate goal of BLS but represents only the start of recovery. Continue monitoring for re-arrest, support breathing as needed, place the victim in the recovery position if breathing is adequate, and hand off to advanced providers with a clear summary of events, interventions, and patient response.
Post-resuscitation care begins as soon as return of spontaneous circulation occurs. The patient who regains a pulse after CPR remains critically ill and requires careful monitoring during transport to definitive care. Position considerations include the recovery position for unconscious breathing patients which involves rolling the victim onto their side with the head supported to maintain airway patency. Continued monitoring for re-arrest is essential because the underlying cause of the original arrest often persists and may produce another arrest within minutes or hours of the initial resuscitation. Advanced cardiac life support providers take over management once they arrive.
Documentation and debriefing complete the resuscitation event for the team. Recording compression quality, ventilation adequacy, time intervals between key events, shock delivery, and patient response supports quality improvement efforts. Debriefing within minutes of the event captures observations while they are fresh and allows the team to identify what went well and what could improve. Effective debriefings focus on systems and processes rather than blaming individuals and create learning opportunities that improve future resuscitation outcomes for the team and the broader organization.
BLS Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.