Chiari Malformation MRI: Complete Patient Guide
Chiari malformation MRI guide — diagnostic criteria, imaging sequences, CINE flow studies, types, treatment correlation, and follow-up considerations.
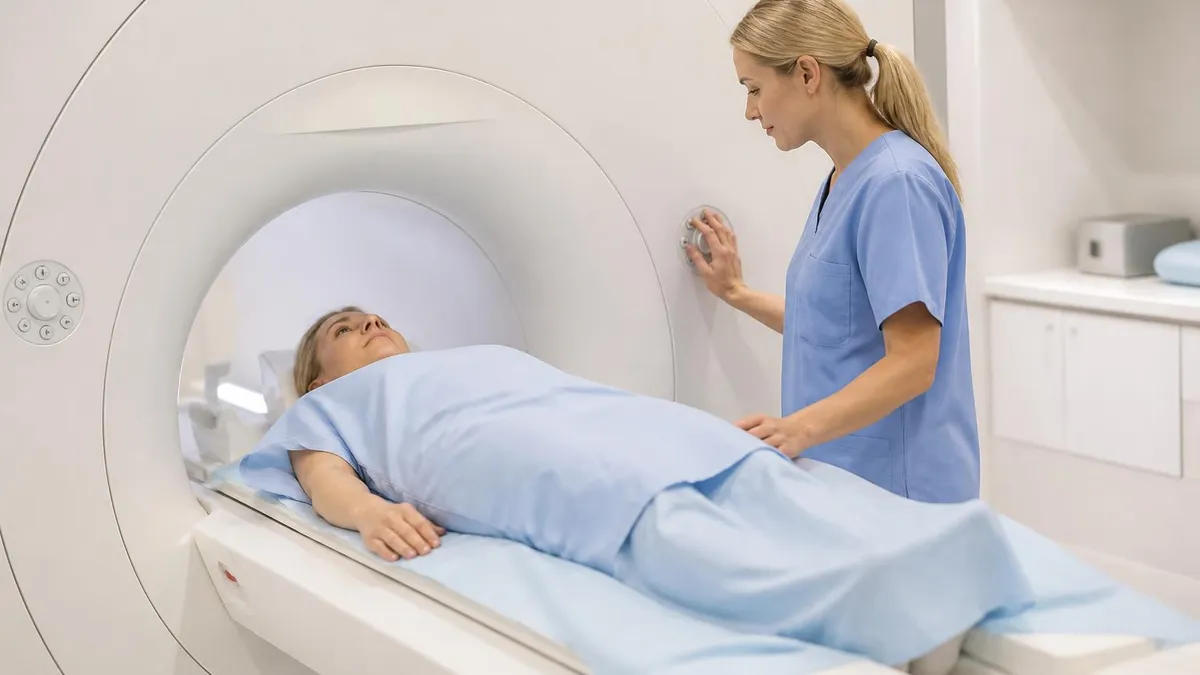
Chiari malformation MRI is the imaging study of choice for diagnosing and characterizing Chiari malformations — structural abnormalities where brain tissue extends into the spinal canal. MRI provides detailed visualization of the brain stem, cerebellum, and the cervical spinal cord junction where Chiari malformations occur, making it essential for both initial diagnosis and ongoing monitoring of these conditions. The exam uses no ionizing radiation, making it safe for repeat imaging when monitoring is needed across years for patients with Chiari malformations being managed conservatively without surgical intervention.
This guide walks through Chiari malformation MRI including what the imaging shows, the different types of Chiari malformations, specific MRI sequences used, what patients should expect during the exam, the role of MRI in diagnosis and treatment planning, and follow-up imaging considerations. Information here is educational and intended to help patients and caregivers understand the imaging process. It does not replace consultation with neurologists, neurosurgeons, or radiologists who provide actual medical evaluation and management decisions for individual patients with confirmed or suspected Chiari malformations.
Chiari malformations are named after Hans Chiari, the Austrian pathologist who first described them in the late 1800s. The condition involves the cerebellar tonsils (lower portion of the cerebellum) extending below the foramen magnum (the opening at the base of the skull) into the cervical spinal canal. The herniated tissue can affect cerebrospinal fluid (CSF) flow and compress neurological structures, producing various symptoms in some patients while remaining asymptomatic in others. MRI provides the detailed anatomical visualization needed to assess these structural relationships and their potential clinical significance.
Chiari Malformation MRI Quick Facts
Best imaging modality: MRI is the definitive imaging study for Chiari malformations. Key sequences: Sagittal T1 and T2 of brain and cervical spine showing tonsillar position. CINE MRI: Phase-contrast MRI showing CSF flow dynamics, important for treatment decisions. Diagnostic criterion: Cerebellar tonsils extending 5+ mm below foramen magnum (Type I); various criteria for other types. No radiation: Safe for repeat monitoring imaging across years. Duration: 30-60 minutes typical. Contrast: Usually not needed unless evaluating other conditions; gadolinium used selectively.
The most common type of Chiari malformation, Type I, involves cerebellar tonsils extending more than 5mm below the foramen magnum without spinal cord involvement. Type I is by far the most frequently encountered type, with most patients diagnosed as adolescents or adults. Type II Chiari involves the cerebellar vermis and brainstem extending into the spinal canal and is associated with myelomeningocele (a form of spina bifida) typically diagnosed in infancy.
Type III is rarer, involving herniation of cerebellum and brainstem into a posterior encephalocele, typically diagnosed at birth. Type IV (sometimes excluded from current classifications) involves cerebellar hypoplasia. MRI distinguishes these types based on specific anatomical findings.
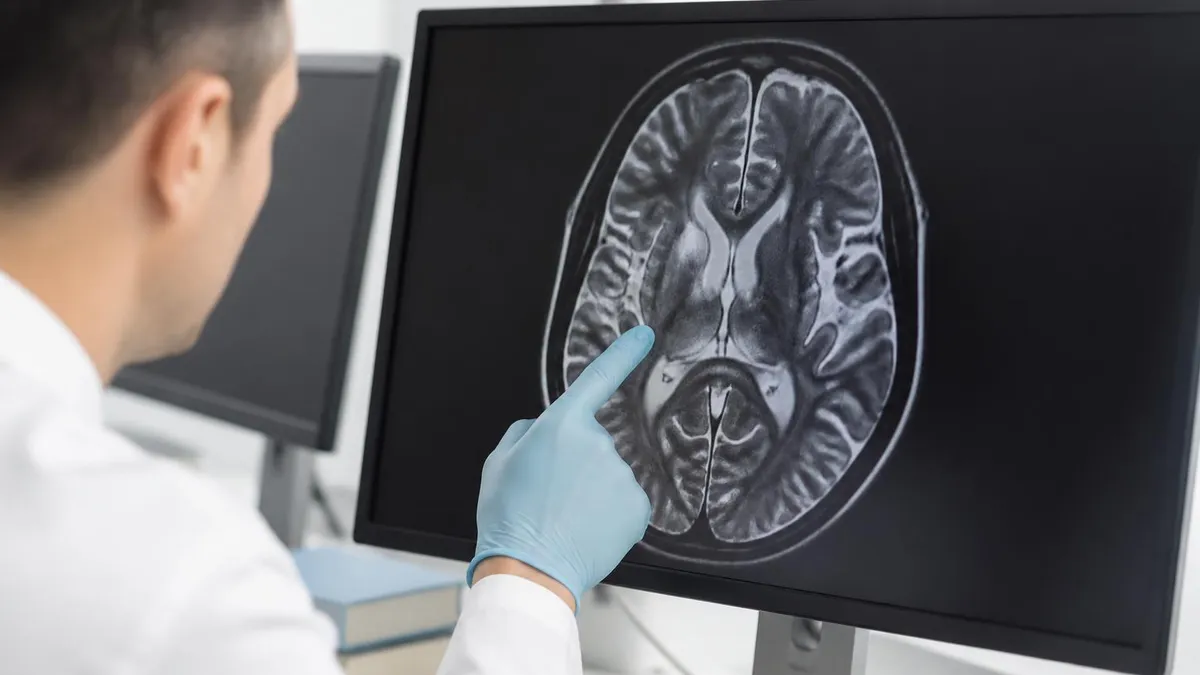
The standard MRI protocol for Chiari evaluation includes sagittal T1-weighted and T2-weighted sequences of the brain and cervical spine. Sagittal images are essential because they show the cerebellar tonsils' position relative to the foramen magnum in the same plane that defines the diagnostic criterion. T2-weighted sequences show CSF as bright (high signal), making the spinal canal and CSF spaces clearly visible. T1 sequences provide anatomical detail and tissue contrast. The combination demonstrates the herniated tonsillar tissue's relationship to surrounding structures including the brainstem, cervical spinal cord, and CSF spaces.

Chiari Malformation Types
Cerebellar tonsils 5+ mm below foramen magnum. Most common. Typically diagnosed adolescent/adult.
Cerebellar vermis and brainstem in spinal canal. Associated with myelomeningocele/spina bifida.
Cerebellum and brainstem in posterior encephalocele. Rare. Typically diagnosed at birth.
Cerebellar hypoplasia (underdevelopment). Sometimes excluded from current classifications.
Variations described in literature with subtle findings or borderline criteria.
Cerebellar herniation from increased pressure or other causes — different from primary congenital Chiari.
For evaluating CSF flow dynamics, CINE MRI (also called phase-contrast MRI or CSF flow study) provides functional imaging beyond standard structural MRI. The technique uses pulse sequences that measure fluid motion across multiple cardiac cycles, showing CSF moving up and down with cardiac pulsations. In normal anatomy, CSF flows freely around the cervical spinal cord. In Chiari malformation, the herniated tonsillar tissue can obstruct or alter CSF flow patterns. CINE MRI demonstrates these flow abnormalities, providing functional information beyond just anatomical measurement of tonsillar position.
The CINE MRI findings substantially influence treatment decisions for symptomatic Chiari patients. Normal CSF flow on CINE despite radiographic Chiari (large tonsillar descent without flow abnormality) often suggests conservative management. Abnormal CSF flow on CINE with corresponding symptoms may support surgical intervention through posterior fossa decompression. The combination of structural MRI showing tonsillar position plus CINE MRI showing flow dynamics plus clinical symptoms drives treatment decisions, with no single imaging finding being definitive on its own without clinical context and symptom correlation.
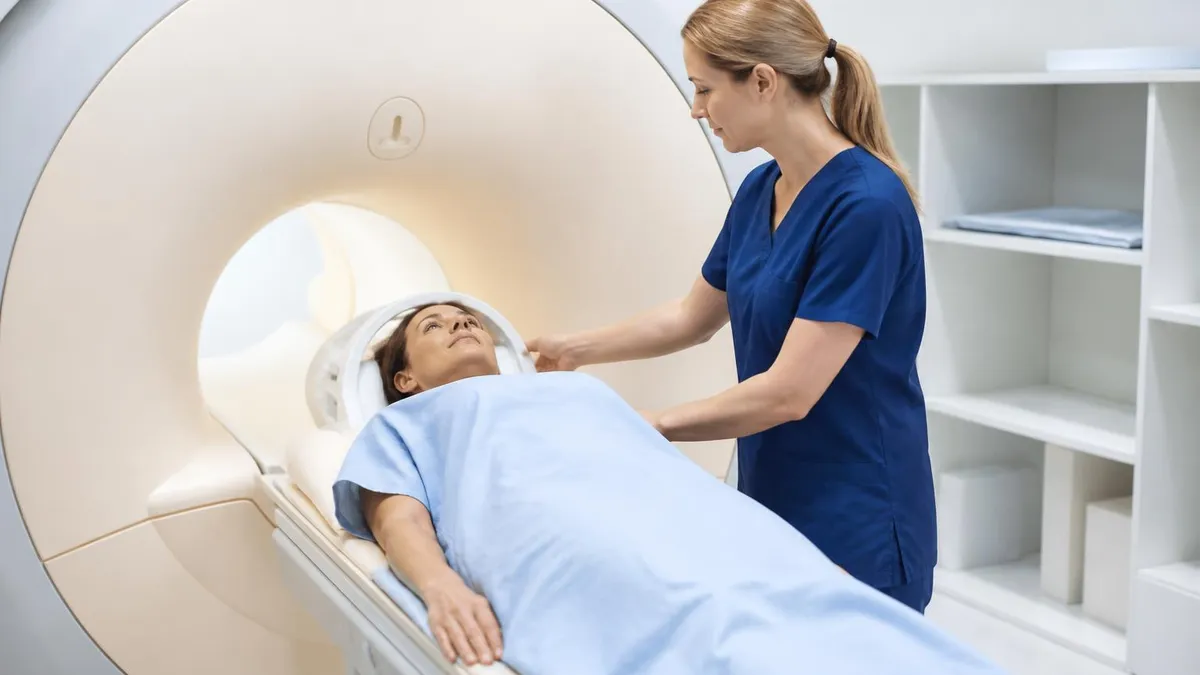
Patient experience during Chiari MRI follows the standard MRI protocol. Patients lie supine on the MRI table, head positioned in a head coil that surrounds the head. The exam typically takes 30-60 minutes including various sequence acquisitions. Patients hear loud knocking and buzzing sounds from the magnet operations. Most patients tolerate the exam without difficulty, though those with claustrophobia may need anxiolytic medication or open MRI configurations. No special preparation is needed for standard Chiari MRI without contrast — patients can eat normally and continue medications before the exam unless specific instructions indicate otherwise.
Sagittal T1: Brain and cervical spine. Anatomical detail. Sagittal T2: Brain and cervical spine. CSF appears bright, clearly showing spinal canal. Axial T2: Confirms findings in different plane. FLAIR: Sometimes added for parenchymal abnormality detection. Coronal T2: Sometimes added for additional anatomical perspective. Total acquisition: 25-40 minutes for standard structural sequences.
For diagnosing Chiari malformation Type I specifically, the radiologist measures the cerebellar tonsils' lowest position relative to a line drawn from the basion to the opisthion (across the foramen magnum). Tonsillar position more than 5mm below this line meets the conventional diagnostic criterion for Chiari I, though some authors propose different cutoffs (3mm for symptomatic patients, larger thresholds for older adults). Tonsillar shape also matters — pointed peg-shaped tonsils are more concerning than rounded tonsils despite similar position. The combination of measurement, tonsillar shape, and presence of associated findings (syringomyelia, scoliosis) supports the complete diagnostic assessment.
Syringomyelia (syrinx) is a fluid-filled cavity within the spinal cord that frequently accompanies Chiari malformations, particularly when symptomatic. MRI shows syringomyelia as a tube-shaped fluid collection within the cord substance, most commonly in the cervical and upper thoracic spinal cord. The syrinx may be small (small thin fluid stripe) or substantial (extensive cavity occupying most of the cord cross-section). Syrinx presence often drives surgical treatment decisions since untreated syringomyelia can progressively damage the spinal cord. Following surgery, MRI tracks syrinx response — successful surgery typically reduces syrinx size over months following the procedure.
Other associated findings on Chiari MRI include various structural anomalies that may accompany the primary malformation. Klippel-Feil syndrome (fused cervical vertebrae) sometimes occurs with Chiari. Basilar invagination (abnormally high position of upper cervical spine into the cranium) can compound the anatomical complexity. Atlas assimilation (fusion of C1 to occiput) sometimes occurs. Hydrocephalus (enlarged ventricles) may accompany severe Chiari especially Type II. Each associated finding affects treatment planning and prognosis. The radiologist's report addresses both the primary Chiari finding and any associated anomalies that affect management decisions.
Chiari malformation MRI findings exist on a spectrum from incidental discovery to severely symptomatic. Reality: Many people have radiographic Chiari malformation without symptoms — discovered incidentally during MRI for other reasons. Treatment decisions depend on clinical symptoms, not just imaging findings. Symptomatic Chiari: Headaches (occipital, worsened with cough/strain), neck pain, dizziness, balance issues, vision changes, swallowing difficulties. Don't: Pursue surgery for asymptomatic Chiari found incidentally on MRI. Do work with neurologist or neurosurgeon to correlate imaging with clinical picture for treatment decisions.
The clinical context substantially affects how Chiari MRI findings are interpreted. Asymptomatic patients with incidental Chiari findings on MRI performed for unrelated reasons typically receive recommendations for periodic monitoring rather than immediate intervention. Symptomatic patients with imaging findings consistent with their symptoms (occipital headaches worsening with Valsalva, balance issues, cranial nerve symptoms) often receive surgical consideration. The challenge lies in patients with imaging findings and symptoms that may or may not be related — distinguishing Chiari-caused symptoms from other causes requires careful neurological evaluation beyond the imaging itself.
For patients diagnosed with Chiari malformation, follow-up imaging strategies vary. Asymptomatic patients with stable findings typically have repeat MRI every 3-5 years for monitoring. Symptomatic patients receiving conservative management may have more frequent imaging. Post-surgical patients have follow-up imaging assessing decompression results and syrinx response over months and years. Children with Chiari may need more frequent imaging during growth phases. The specific schedule depends on patient circumstances — neurologists or neurosurgeons determine appropriate intervals based on individual factors rather than fixed protocols applying to all patients.
Surgical treatment for symptomatic Chiari malformation is posterior fossa decompression — removing a small amount of bone from the back of the skull and sometimes opening the dura to create more space for the herniated tissue. The surgery aims to relieve pressure on neural structures and restore normal CSF flow. Post-operative MRI shows the decompression and assesses results.
Successful surgery typically shows reduced or resolved syringomyelia (when present), restored CSF flow on CINE, and clinical symptom improvement. Surgery isn't always successful — some patients have persistent symptoms despite anatomically successful decompression. The combination of clinical and imaging follow-up assesses surgical outcomes comprehensively.
Chiari MRI Patient Information Checklist
- ✓Confirm exam orderer (neurologist, neurosurgeon, primary care) and reason for MRI
- ✓Verify whether contrast will be used (most Chiari MRIs don't require contrast)
- ✓Discuss claustrophobia concerns with ordering provider — anxiolytics available if needed
- ✓Inform MRI center of any metal implants or devices for safety screening
- ✓Continue regular medications unless specifically instructed otherwise
- ✓Plan 30-60 minutes for the exam plus additional time for check-in and dressing
- ✓Bring previous imaging studies if available for radiologist comparison
- ✓Wear or change into clothes without metal (zippers, buttons, jewelry)
- ✓Receive and review radiologist report through your ordering provider
- ✓Schedule follow-up consultation to discuss findings and treatment plan if needed
For users wondering whether they should pursue Chiari MRI, several considerations matter. Persistent occipital headaches worsening with cough, sneeze, or Valsalva maneuvers are classic Chiari symptoms warranting evaluation. Family history of Chiari malformation may support evaluation given hereditary tendencies. Symptoms suggesting brainstem or upper cord dysfunction (swallowing difficulties, vision issues, balance problems, weakness, sensory changes) warrant evaluation. However, simply having occipital headaches without specific concerning features doesn't necessarily indicate Chiari — most occipital headaches have other causes. Discuss specific symptoms with primary care provider who can determine whether neurology referral and Chiari MRI are appropriate.
For users dealing with the diagnostic uncertainty of borderline Chiari findings, several considerations help. Tonsillar position 3-5mm below foramen magnum is sometimes called Chiari 0 or considered borderline — clinical correlation matters more than just measurement. Tonsillar shape and CINE MRI flow findings provide additional information beyond simple position.
Symptom severity and progression help distinguish meaningful Chiari from incidental finding. Some patients spend years with diagnostic uncertainty before either symptoms progress to clear surgical indications or remain stable enough that conservative management continues indefinitely. Patience with the diagnostic process and trust in qualified specialists usually produces better outcomes than aggressive intervention in unclear cases.
For patients diagnosed with Chiari malformation and considering treatment options, several considerations apply. Conservative management (symptom management, periodic monitoring) works for asymptomatic and mildly symptomatic patients. Surgical decompression addresses symptomatic patients with anatomically appropriate findings. Other interventions (physical therapy, pain management, anxiety treatment for headaches) address symptoms regardless of surgical decisions. Get second opinions from experienced Chiari specialists at major medical centers when surgical decisions are being considered — Chiari surgery has substantial technical complexity and outcomes vary by surgeon experience. Specialty centers with high Chiari case volumes typically provide better outcomes than occasional Chiari surgery at general neurosurgical practices.
Pediatric Chiari malformations present specific considerations beyond adult diagnosis and management. Type II Chiari is most common in pediatric patients and typically associated with myelomeningocele. Pediatric Chiari I patients may show different symptom profiles than adults — feeding difficulties in infants, developmental concerns in children, headaches and other symptoms in older children and adolescents. Pediatric Chiari MRI follows similar protocols to adult imaging but requires age-appropriate techniques (sedation for younger children, specific positioning for cooperation, etc.). Pediatric neurosurgeons specializing in Chiari provide treatment specific to growing children's needs.
For users dealing with the genetic counseling aspects of Chiari, several patterns emerge. Most Chiari malformations occur sporadically without clear hereditary patterns. Some families show clustering suggesting genetic factors. Specific genetic syndromes can include Chiari as one feature (Klippel-Feil, certain other connective tissue disorders). Family screening with MRI may identify undiagnosed family members though this isn't routinely recommended due to the high rate of incidental Chiari findings without symptoms. Genetic counseling supports families with multiple affected members in considering these patterns and family planning implications.
For users wanting to understand the broader research landscape around Chiari malformations, several research directions continue advancing knowledge. Imaging techniques continue improving with higher field strength MRI (3T and 7T) providing more detailed anatomical visualization. CSF flow dynamics modeling supports better understanding of which patients benefit from surgery. Genetic studies identify factors associated with Chiari development. Surgical technique refinements aim to improve outcomes and reduce complications. Patient registries track long-term outcomes across many patients providing data informing future management. Each research area contributes incrementally to improving diagnosis and treatment of Chiari malformations across coming years of medical advancement.
The bottom line on Chiari malformation MRI: it's the definitive imaging study for diagnosing and characterizing these structural abnormalities. Standard MRI sequences plus CINE flow studies provide comprehensive evaluation. The diagnostic findings must be correlated with clinical symptoms before treatment decisions are made — radiographic Chiari without symptoms doesn't usually warrant intervention. Specialty centers with experienced Chiari teams provide best outcomes for complex cases. Patients with confirmed Chiari should establish care with neurologist or neurosurgeon experienced in this condition for ongoing management across the years following initial diagnosis.
Chiari MRI Quick Reference
Chiari MRI Findings
Cerebellar tonsils extending below foramen magnum. Primary diagnostic criterion.
Pointed peg-shaped tonsils more concerning than rounded. Affects clinical significance.
Fluid cavity in spinal cord. Common Chiari association. Drives treatment decisions.
Altered flow on CINE MRI. Supports clinical significance assessment for borderline cases.
Compression of brainstem by herniated tissue. Concerning finding requiring evaluation.
Klippel-Feil, basilar invagination, atlas assimilation, hydrocephalus, other findings.
For users dealing with the emotional aspects of Chiari diagnosis, several considerations help. Initial diagnosis often produces anxiety about brain abnormality regardless of symptom severity. Education about Chiari (most patients with radiographic Chiari are asymptomatic; symptomatic Chiari has effective treatment options; surgery has good outcomes for appropriate candidates) helps reduce anxiety. Connection with patient advocacy organizations like Conquer Chiari provides community support and current information. Discussion with healthcare providers addresses individual concerns. Most patients adjust to diagnosis over time, especially when symptoms are managed appropriately and prognosis is realistic about either conservative management or surgical intervention as appropriate.
For users dealing with insurance coverage of Chiari MRI, the imaging is generally covered when appropriately ordered for symptoms suggestive of Chiari malformation. Pre-authorization may be required for some plans. Specialized sequences like CINE MRI may have additional documentation requirements. Coverage varies by plan and specific clinical context. Work with your healthcare provider's office on insurance authorization and coding to maximize coverage and minimize patient cost. For patients without insurance or with inadequate coverage, hospital financial assistance programs and various other resources may help with imaging costs.
For users transitioning between healthcare providers or relocating, several Chiari-specific considerations apply. Original imaging studies should transfer with you — request copies on CD/DVD or through medical record portals before leaving previous providers. Operative notes and follow-up imaging post-surgery are essential for new providers managing your care. Continuity of care matters substantially for Chiari patients given the chronic nature of the condition and importance of comparing current imaging to baseline studies. Plan ahead for transitions to maintain comprehensive records and minimize gaps in care continuity.
Looking forward, Chiari malformation diagnosis and treatment will continue evolving. Higher resolution imaging will improve diagnostic precision. Better understanding of CSF dynamics will support more refined treatment decisions. Less invasive surgical techniques are being explored. Better post-surgical outcome prediction will help patient counseling about expected results. Patient registries are accumulating long-term outcome data informing future practice. Stay engaged with your Chiari specialist for current best practices specific to your situation rather than relying on outdated information that may not reflect current medical understanding of optimal management approaches for your specific diagnostic findings and symptoms.
Chiari MRI: Pros and Cons
- +Definitive diagnostic test for Chiari malformations
- +No ionizing radiation — safe for repeat monitoring
- +Detailed anatomical visualization of brain stem and cord
- +CINE sequences add functional CSF flow information
- +Supports both diagnosis and treatment planning
- −30-60 minute exam may be challenging for claustrophobic patients
- −Cost varies — typically $400-$3,500+ depending on facility and insurance
- −Findings can be incidental without symptoms creating anxiety
- −Diagnostic threshold (5mm) is somewhat arbitrary cutoff
- −Imaging interpretation requires clinical correlation
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.