Electrocardiogram Cost: How Much Does an EKG Test Cost?
Electrocardiogram cost guide: average EKG test prices with and without insurance, factors affecting cost, where to get an affordable EKG, and what to expect.
- Without insurance: $50–$3,000+ depending on where the test is performed
- With insurance: Typically just a copay or coinsurance after deductible is met
- Primary care office: $100–$300 for the EKG itself; additional office visit fee applies
- ER setting: $1,000–$3,500+ including facility and interpretation fees
- Free-standing lab: $30–$100 for a tracing without physician interpretation
- Medicare coverage: Covered when medically necessary; 20% coinsurance after Part B deductible
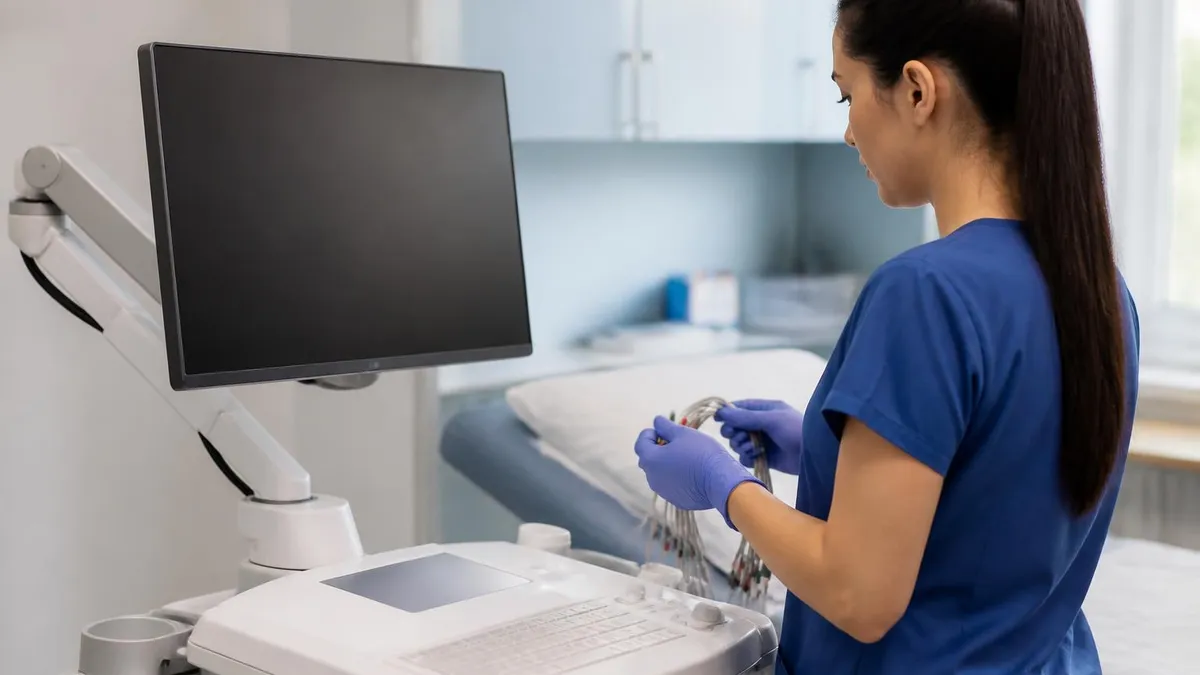
An electrocardiogram (ECG or EKG) is a non-invasive diagnostic test that records the electrical activity of the heart using electrodes placed on the skin of the chest, arms, and legs. The test is painless, takes approximately 5 to 10 minutes to perform, and produces a printed or digital tracing that a physician interprets to assess heart rhythm, rate, and electrical conduction.
EKGs are ordered for a wide range of reasons — from screening and routine check-ups to evaluating chest pain, palpitations, shortness of breath, or suspected arrhythmias — and the cost of the test varies significantly depending on the setting in which it is performed, whether the patient has health insurance, and how the charges are structured by the billing provider.
The cost of an electrocardiogram without health insurance typically ranges from under $100 at a free-standing laboratory or retail health clinic to well over $1,000 at a hospital emergency department. This wide range reflects the dramatic difference in facility fees and overhead costs between settings.
A primary care physician's office or urgent care clinic performing a routine EKG charges for both the technical component (the tracing itself, billed under CPT code 93005) and the professional component (the physician's interpretation, billed under CPT code 93010). When both are performed and billed together, the combined code is CPT 93000, which typically ranges from $50 to $300 in outpatient settings when billed directly, before insurer markups or facility fees are added.
At a hospital outpatient department or emergency room, the same EKG test carries a substantially higher price tag because of the facility fee — a charge assessed for the use of the hospital's resources, equipment, and staffing infrastructure, billed separately from the physician's professional fee.
In an ER setting, the facility fee alone for an EKG can range from $500 to $2,500 or more, in addition to the professional interpretation fee and any other charges associated with the visit. Patients who receive an EKG in the ER as part of a broader workup for chest pain or cardiac symptoms may find the EKG line item buried within a much larger hospital bill that includes additional tests, physician fees, and monitoring charges.
Free-standing imaging and laboratory centres — such as those operated by Quest Diagnostics, LabCorp, or independent cardiac testing facilities — offer EKG tracings at significantly lower prices, often between $30 and $100 for the tracing alone. These facilities typically do not provide immediate physician interpretation on-site; instead, the tracing is sent electronically to a cardiologist or reading service, and results may take one to several days.
This option is appropriate for non-urgent purposes, such as pre-employment screening, pre-surgical clearance, or monitoring of a known stable cardiac condition, but is not suitable when immediate clinical decision-making is needed based on the EKG findings.
Retail health clinics operated by pharmacy chains such as CVS MinuteClinic and Walgreens Health have expanded their cardiac screening services in recent years and offer EKG testing at relatively transparent prices, typically in the range of $75 to $150 per test.
These clinics operate on a walk-in basis and provide fast results, making them a practical option for patients who want an affordable EKG outside of a traditional physician's office. The nurse practitioner or physician assistant at the clinic can typically interpret the EKG on-site and provide a written summary of findings, which can be forwarded to the patient's primary care physician for further review.
The setting where you receive an EKG dramatically affects the final cost. A non-urgent EKG at a free-standing lab or retail health clinic can cost 80–90% less than the same test in a hospital emergency room. For planned EKGs, comparing prices across settings before scheduling is one of the most effective ways to control cost.
Telehealth platforms have also begun offering EKG-adjacent services, particularly through consumer cardiac devices such as the KardiaMobile by AliveCor. These devices allow individuals to record a single-lead or six-lead EKG at home for a fraction of the cost of a clinical EKG, with readings interpreted via artificial intelligence algorithms and optionally reviewed by a remote cardiologist for an additional fee.
While consumer-grade EKG devices do not produce the same 12-lead tracing as a clinical EKG and cannot be used for all diagnostic purposes, they provide a cost-effective option for individuals monitoring for known arrhythmias such as atrial fibrillation or for those who have been advised to track their heart rhythm between clinical visits.
Geographic location is a significant factor in EKG pricing across the United States. Urban centres with high costs of living — particularly metropolitan areas in California, New York, and New England — tend to have significantly higher facility fees and physician charges than rural or suburban areas in the Midwest and South.
The same CPT 93000 service billed in San Francisco may cost two to three times as much as the identical service billed at an independent clinic in rural Arkansas. Patients with the flexibility to travel to a lower-cost facility for a non-urgent EKG can achieve meaningful savings by comparing prices using hospital price transparency tools before scheduling.
The total cost of an EKG visit often includes charges beyond the EKG itself. Physician practices and hospital outpatient departments typically bill a separate evaluation and management (E&M) code for the visit at which the EKG was ordered and interpreted. This E&M charge can range from $100 to $500 or more depending on the complexity of the visit and the provider type.
Patients who receive an EKG as part of an annual physical may find the interpretation included in the preventive visit charge, while patients who come specifically for cardiac evaluation may face separate billing for both the clinical encounter and the EKG procedure. Understanding this distinction helps avoid unexpected double-billing surprises.
Employer-sponsored wellness programmes and occupational health services sometimes offer free or subsidised EKG testing as part of annual health screenings. Certain professions — commercial truck drivers, pilots, and first responders — require periodic cardiac evaluations including EKGs as a condition of licensure or employment, and employers frequently cover these costs directly or reimburse them as an employment benefit. Patients in these categories should verify whether their employer's occupational health provider offers EKG testing and whether the cost is covered before seeking the service elsewhere at their own expense.
Consumer-grade cardiac monitoring devices represent a growing segment of the personal health technology market. The KardiaMobile 6L by AliveCor, the Apple Watch Series 4 and later, and the Withings ScanWatch all offer six-lead or single-lead EKG recordings that can detect atrial fibrillation and certain other rhythm abnormalities.
These devices are available for purchase at costs ranging from $99 to $499, with optional subscription plans for remote physician review. While they do not replace a clinical 12-lead EKG for diagnostic purposes, they provide a cost-effective tool for ongoing monitoring between clinical visits, particularly for patients who have already been diagnosed with an intermittent arrhythmia.
Prior authorisation requirements imposed by insurance companies can affect both the timing and the cost of an EKG in managed care settings. Some health maintenance organisation (HMO) and preferred provider organisation (PPO) plans require that the ordering physician obtain prior approval before certain EKG procedures — particularly stress EKGs or specialised cardiac monitoring — are covered at the contracted rate.
Skipping this step, or having the test performed at an out-of-network facility, can result in the claim being denied or the patient being billed at a much higher out-of-network rate. Confirming prior authorisation requirements with your insurer and ensuring the ordering provider submits any required documentation before the test is scheduled protects against unexpected billing denials.
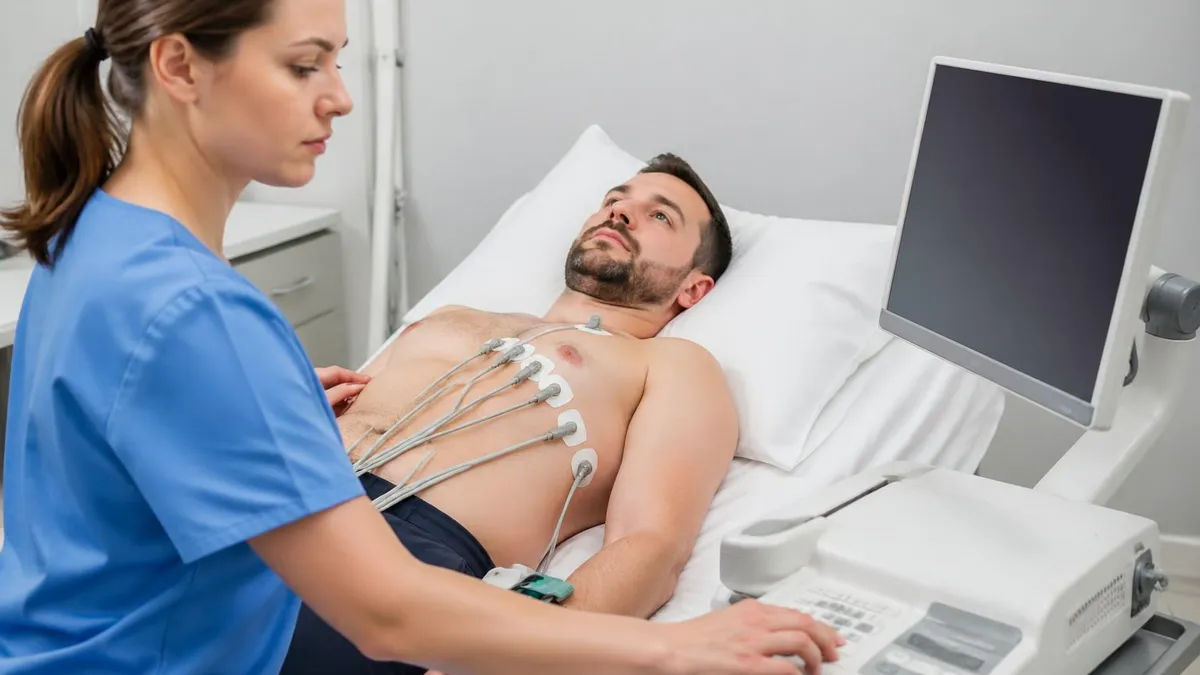
EKG Cost by Setting
Prices are self-pay estimates for the United States and vary by region, provider, and whether interpretation is included. Always request an itemised estimate before scheduling.

Health insurance coverage for an electrocardiogram depends on the type of plan, the deductible status, and the medical necessity determination made by the insurer. Most commercial health insurance plans cover EKG testing when it is ordered for a medically necessary reason — such as evaluating chest pain, shortness of breath, palpitations, pre-operative cardiac clearance, or monitoring of a known cardiac condition.
Coverage for routine or preventive EKGs in asymptomatic patients is less consistent and may require prior authorisation or documentation of risk factors, depending on the plan. Patients undergoing a physical examination may receive an EKG as part of a preventive visit, which can affect how the claim is billed and whether standard cost-sharing applies.
For patients with a high-deductible health plan (HDHP), the full cost of the EKG may be applied to the deductible if it has not yet been met for the year. Once the deductible is satisfied, the patient pays only their coinsurance percentage — typically 10 to 30 percent of the allowed amount — until the out-of-pocket maximum is reached.
Patients enrolled in plans with copayment structures rather than coinsurance typically pay a fixed amount per visit, regardless of the tests performed. Under these plans, a $30 specialist copay or a $50 urgent care copay may cover the entire visit, including the EKG, once the insurer processes the claim and applies their negotiated rate.
Medicare Part B covers EKG testing as a diagnostic test when it is medically necessary and ordered by a physician who accepts Medicare assignment. The patient is responsible for the Part B deductible (currently $240 per year in 2024) and 20 percent of the Medicare-approved amount after the deductible is met.
Medicare also covers a one-time EKG as part of the Welcome to Medicare preventive visit for newly enrolled beneficiaries. Medicare Advantage (Part C) plans cover the same services as Original Medicare but may have different cost-sharing structures and network requirements that affect where beneficiaries can receive an EKG at covered rates.
Medicaid coverage for electrocardiograms varies by state, but most state Medicaid programmes cover EKGs as a medically necessary outpatient diagnostic service with little or no cost-sharing for enrollees. Low-income patients who are not Medicaid-eligible may access free or reduced-cost EKG testing through federally qualified health centres (FQHCs), which are required by federal law to provide services on a sliding-scale fee basis adjusted to household income and family size.
Community health centres, free clinics operated by medical schools and non-profit organisations, and cardiac screening events sponsored by hospitals or professional cardiac associations also offer free or heavily subsidised EKGs to uninsured or underinsured patients who qualify based on income or health risk factors.
Understanding the billing codes associated with an EKG helps patients review their insurance explanation of benefits (EOB) and identify whether charges were billed and processed correctly. CPT code 93000 represents the complete 12-lead EKG with tracing, interpretation, and report; CPT 93005 represents only the tracing; and CPT 93010 represents only the interpretation and report.
If both the facility and the physician bill separately, you may see both CPT 93005 and CPT 93010 on your EOB. Charges submitted under incorrect codes — or charges for both 93000 and 93005/93010 for the same test — are billing errors that can and should be disputed by contacting the provider's billing department and requesting an itemised explanation of all charges billed to your insurer.
Understanding how your insurance plan processes EKG claims — including deductibles, copays, prior authorisation requirements, and in-network vs. out-of-network rules — can significantly reduce your out-of-pocket cost. Confirming coverage before scheduling and keeping records of all billing codes on your explanation of benefits protects you from unexpected charges.
Patients who are uninsured or underinsured may negotiate the cost of an EKG directly with the provider before or after the test. Many hospitals and physician practices have financial assistance programmes or charity care policies that reduce or waive charges for patients below certain income thresholds.
Requesting an itemised bill rather than a summary statement, asking for the cash-pay or self-pay rate (which is typically lower than the standard list price), and comparing costs across facilities before scheduling a non-urgent EKG are practical strategies that can result in significant savings. Price transparency tools published by hospitals in compliance with CMS requirements also allow patients to look up the standard charge and negotiated rates for CPT 93000 at specific facilities before making an appointment.
Annual and lifetime out-of-pocket maximums established by the Affordable Care Act limit the total amount a patient can be required to pay for covered services in a given plan year. For 2024, the maximum out-of-pocket limits for ACA-compliant plans are $9,450 for individuals and $18,900 for families.
Once these thresholds are reached, the insurer pays 100 percent of covered in-network costs for the remainder of the plan year. Patients who have already met their out-of-pocket maximum — for example, following a hospitalisation or major medical event — may effectively receive an EKG at no direct cost if it is scheduled before the plan year resets.
Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) can be used to pay for EKG tests with pre-tax dollars, effectively reducing the after-tax cost of the procedure by the payer's marginal tax rate. An individual in the 22 percent federal tax bracket who pays $200 for an EKG out-of-pocket can save $44 by paying through an HSA or FSA rather than using after-tax income.
HSA funds roll over year to year and can be invested; FSA funds must typically be used within the plan year. Both account types are funded by payroll deductions and are available through most employer-sponsored health benefit programmes.
Hospital financial assistance programmes — sometimes called charity care — are required by law for non-profit hospitals receiving federal tax exemptions. These programmes provide free or reduced-cost care to patients who meet income eligibility criteria, typically expressed as a percentage of the federal poverty level.
A patient with a household income below 200 percent of the federal poverty level may qualify for a complete fee waiver, while patients between 200 and 400 percent may receive a significant discount. Applications for financial assistance must usually be submitted within a set window after the date of service, and documentation of income is required. Contact the hospital's patient financial services department as soon as you receive the bill to inquire about eligibility.
If an insurance claim for an EKG is denied, patients have the right to appeal the decision under the ACA and applicable state laws. Common reasons for denial include lack of prior authorisation, out-of-network provider billing, or a determination that the service was not medically necessary. The appeals process typically involves submitting a written appeal with supporting documentation from the ordering physician explaining the clinical rationale for the test.
External independent review is available as a final appeal step under ACA requirements. Most denied claims that are appealed with appropriate clinical documentation are reversed, particularly when the service was ordered for clear symptomatic reasons and the denial was based on an administrative technicality.
Several states have enacted their own price transparency and surprise billing protections that go beyond federal law, providing additional financial protections for patients who receive EKGs and other diagnostic services. The federal No Surprises Act, effective from January 2022, protects patients from unexpected bills for out-of-network emergency services and certain non-emergency services at in-network facilities when out-of-network providers are used without the patient's informed consent.
If you receive a bill that appears to violate these protections — such as an out-of-network facility fee charge for an EKG performed at an in-network hospital — you have the right to file a complaint with your insurer or the relevant state insurance commissioner, and the billing dispute process can result in the charge being significantly reduced or eliminated.
Never delay an EKG for cost reasons in an emergency: If you are experiencing chest pain, shortness of breath, palpitations, dizziness, or symptoms of a heart attack, call 911 or go to the nearest emergency room immediately. The cost of a hospital EKG is always manageable — through insurance, financial assistance, or a payment plan — and should never be a reason to delay urgent cardiac evaluation. Financial assistance programmes exist specifically for these situations.
Before Your EKG: How to Keep Costs Down
Typical EKG Costs With Insurance
EKG Pros and Cons
- +EKG has a publicly available content blueprint — you know exactly what to prepare for
- +Multiple preparation pathways accommodate different schedules and budgets
- +Clear score reporting shows specific strengths and weaknesses
- +Study communities share current insights from recent test-takers
- +Retake policies allow recovery from a difficult first attempt
- −Tested content scope requires substantial preparation time
- −No single resource covers everything optimally
- −Exam-day performance can differ from practice test performance
- −Registration, prep, and retake costs accumulate significantly
- −Content changes between versions can make older materials less reliable
EKG Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.