Pediatric CNA: Jobs, Salary, Programs & How to Get Started 2026 June
Prepare for the Pediatric CNA: Jobs, Salary, Programs & certification. Practice questions with answer explanations covering all exam domains.
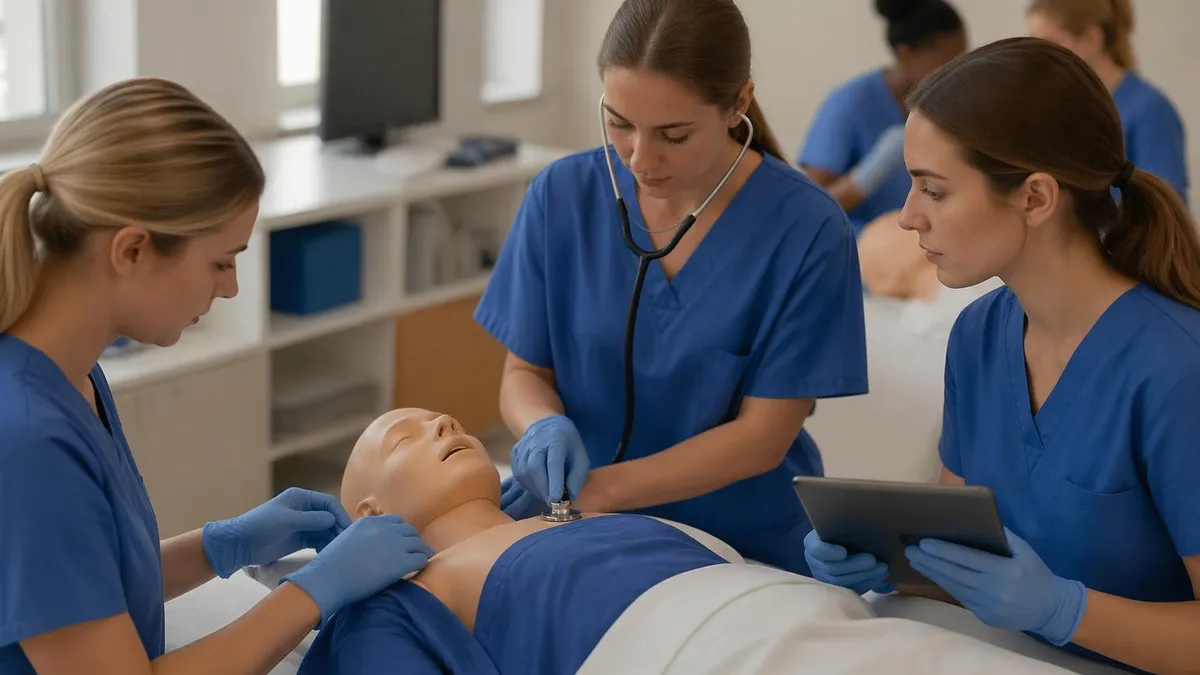
A pediatric CNA works directly with infants, children, and adolescents in hospitals, clinics, and specialty care facilities. It's one of the most rewarding paths you can take as a certified nursing assistant -- and demand for these roles keeps climbing. If you've been searching for pediatric cna jobs or wondering what it takes to break into this field, you're in the right place.
Working with kids isn't the same as caring for adults. Pediatric patients can't always tell you what hurts. They get scared, they cry, and they need someone who stays calm and patient through all of it. That's where you come in. As a pediatric cna jobs specialist, you'll assist nurses with vital signs, comfort anxious patients before procedures, and help families navigate tough moments. The emotional payoff? Enormous -- but you've got to be built for it.
This guide breaks down everything from salary ranges and job availability to training programs and daily responsibilities. Whether you're a newly certified CNA looking to specialize or an experienced aide ready for a change, pediatric nursing offers a career path with genuine purpose. You'll find real numbers, practical steps, and honest pros and cons below -- no fluff, just what you actually need to know to land your first pediatric CNA position. The field is growing fast, and facilities across the country are actively recruiting aides who want to make a difference in children's lives.

The market for pediatric cna jobs has grown steadily over the past few years, and that trend isn't slowing down. Hospitals, urgent care centers, and specialty pediatric clinics are all hiring -- especially in metro areas where children's hospitals anchor the healthcare system. If you search pediatric cna jobs near me, you'll likely see dozens of openings within driving distance, particularly in states like Texas, California, Florida, and New York.
What's driving the demand? A combination of factors. More families have access to pediatric healthcare through expanded insurance coverage. Staffing shortages across nursing mean facilities need CNAs to fill critical support roles. And specialized pediatric units -- think NICU, oncology, and rehab -- require aides who understand child development. The pediatric cna salary reflects this demand, with experienced aides earning well above entry-level CNA pay in many regions.
Part-time and per diem positions are common too, which makes this a flexible option if you're balancing school or family. Some facilities even offer tuition reimbursement for CNAs pursuing nursing degrees -- a solid perk if you're thinking long-term. The bottom line: if you want job security with a specialization that matters, pediatric CNA work delivers on both fronts. And with healthcare systems expanding their pediatric departments nationwide, the opportunities are only going to multiply over the next decade.
Let's talk money. The pediatric cna salary varies depending on where you work, your experience level, and the type of facility. On average, pediatric CNAs earn between $31,000 and $42,000 per year nationally. That range widens significantly in high-cost-of-living areas like the Northeast or West Coast, where hourly rates can hit $20 or more. Night and weekend shifts often come with differentials that bump your take-home pay even higher.
A cna job pediatrics role at a large children's hospital typically pays more than a similar position at a private clinic or doctor's office. Why? Volume, acuity, and union contracts. Major hospitals also tend to offer better benefits -- health insurance, retirement matching, and PTO that actually accrues at a reasonable rate. If maximizing your paycheck matters, aim for children's hospital cna jobs in urban centers.
Experience counts too. A CNA with two-plus years in pediatrics can negotiate starting rates that are 15-20% above what a new grad would accept. Certifications in pediatric first aid or PALS (Pediatric Advanced Life Support) also give you leverage during salary negotiations. Don't underestimate the power of specialized credentials -- they signal to hiring managers that you're serious about this niche. Some employers even offer sign-on bonuses for CNAs with pediatric experience, particularly in regions facing acute staffing shortages.
CNA Study Tips
What's the best study strategy for CNA?
Focus on weak areas first. Use practice tests to identify gaps, then study those topics intensively.
How far in advance should I start studying?
Most successful candidates begin 4-8 weeks before the exam. Create a structured study schedule.
Should I retake practice tests?
Yes! Take each practice test 2-3 times. Focus on understanding why answers are correct, not memorizing.
What should I do on exam day?
Arrive 30 min early, bring required ID, read questions carefully, flag difficult ones, and review before submitting.
Where Pediatric CNAs Work
Large pediatric hospitals are the top employers for CNAs specializing in child care. You'll rotate through units like general pediatrics, NICU, surgical recovery, and emergency. Expect 12-hour shifts, team-based care, and exposure to a wide range of conditions from asthma to post-operative recovery. These roles often require prior CNA experience -- usually at least six months.
Finding cna pediatric jobs in your area doesn't have to be complicated. The best starting points are hospital career pages, Indeed, and state job boards. Many children's hospitals post CNA openings directly on their websites before listing them anywhere else -- so bookmark those pages and check weekly. If you're looking for cna pediatric jobs near me, filtering by "pediatric" or "children's" on job boards narrows results fast.
Networking matters more than you'd think. Clinical instructors from your CNA program often have connections at local hospitals. Former classmates who landed pediatric roles can refer you internally -- and internal referrals skip the resume pile at most facilities. Join CNA groups on Facebook or Reddit where people share job leads and interview tips specific to pediatric settings.
Staffing agencies are another route worth considering. Companies like AMN Healthcare, Aya Healthcare, and local per diem agencies regularly place CNAs in pediatric units. The pay might be slightly lower through an agency, but it gets your foot in the door. Many facilities convert agency CNAs to permanent staff after 90 days if the fit is right. Don't overlook travel CNA positions either -- they pay premium rates and let you test different hospitals before committing.
Children's hospital cna jobs are among the most competitive positions in the CNA field, and for good reason. These facilities offer structured training, mentorship programs, and clear advancement pathways that smaller clinics simply can't match. If you're targeting pediatric cna positions at a major children's hospital, expect a thorough interview process that includes behavioral questions, scenario-based assessments, and sometimes a skills demonstration.
The daily routine at a children's hospital looks different from adult care in significant ways. You'll help restrain toddlers during blood draws (gently, with distraction techniques). You'll measure intake and output for infants who can't report their own symptoms. You'll rock babies in the NICU during overnight shifts when parents can't be there. It's physically and emotionally demanding -- but CNAs who thrive in pediatrics say they could never go back to adult care.
Most children's hospitals require a current CNA certification plus BLS (Basic Life Support) at minimum. Some prefer candidates with previous healthcare experience, though new graduates with strong clinical evaluations can absolutely get hired. Volunteer experience in pediatric settings -- even a few months -- makes your application stand out. Hiring managers want to see that you've been around sick kids before and didn't run the other direction. Shadow days and informational interviews with current pediatric staff can also give you an edge during the hiring process.
Pros and Cons of Pediatric CNA Work
- +Deeply rewarding -- helping children recover creates lasting emotional fulfillment
- +Higher pay than many general CNA roles, especially at children's hospitals
- +Strong job growth and consistent demand across all US regions
- +Excellent stepping stone to pediatric nursing (RN or LPN) careers
- +Variety in daily tasks -- no two shifts are exactly the same
- +Opportunities for specialization in NICU, oncology, or rehab units
- −Emotional toll -- caring for seriously ill children is psychologically heavy
- −Physical demands including lifting, restraining, and extended standing
- −Irregular schedules with nights, weekends, and holiday shifts common
- −Exposure to childhood illnesses and communicable diseases
- −Dealing with anxious or confrontational parents during high-stress moments
- −Lower autonomy compared to nursing roles -- you follow orders, not give them
If you're searching for cna pediatrics jobs with solid training, look for facilities that offer pediatric-specific orientation programs. The best employers don't just hand you a badge and point you toward the floor -- they provide weeks of supervised training where you shadow experienced pediatric CNAs, practice age-appropriate communication, and learn unit-specific protocols. Pediatric cna programs through hospitals often include classroom instruction on child development, growth and nutrition, and family-centered care models.
Community colleges and vocational schools also offer CNA training with pediatric electives or clinical rotations in children's hospitals. These rotations give you hands-on experience before you're on the payroll, which makes the transition to employment much smoother. Some states -- California, New York, and Illinois among them -- have pediatric CNA programs that include specialized coursework beyond the standard CNA curriculum.
Online CNA programs have become more common since 2020, but be cautious. The clinical component -- which is required for certification in every state -- must be completed in person. No legitimate program will let you skip hands-on training. That said, hybrid programs where you complete didactic coursework online and clinicals at a local facility can save time and offer more scheduling flexibility. Just verify that any program you choose is state-approved before you enroll.
Steps to Become a Pediatric CNA
- ✓Complete a state-approved CNA training program (75-180 hours depending on your state)
- ✓Pass the NNAAP or state-specific CNA competency exam (written + skills test)
- ✓Get your CNA certification and register on your state's nurse aide registry
- ✓Obtain BLS/CPR certification through the American Heart Association
- ✓Consider additional pediatric first aid or PALS certification
- ✓Gain clinical experience through volunteer work at a children's hospital
- ✓Build your resume with any relevant caregiving or childcare experience
- ✓Apply to children's hospitals, pediatric clinics, and home health agencies
- ✓Prepare for behavioral interview questions about working with children and families
- ✓Complete facility-specific pediatric orientation and ongoing competency training
The landscape for cna in pediatrics jobs looks different depending on your region. Urban areas with major medical centers -- think Houston, Los Angeles, Philadelphia, Chicago -- have the highest concentration of openings. These cities are home to nationally ranked children's hospitals that employ hundreds of CNAs across multiple units. Rural areas have fewer dedicated pediatric facilities, but family practice clinics and community hospitals still need CNAs comfortable with younger patients.
Pediatrics cna jobs in home health are growing faster than hospital-based roles in some markets. Families with children who have complex medical needs -- tracheostomies, feeding tubes, ventilator dependence -- increasingly prefer home care over extended hospital stays. These positions require additional training and comfort with medical equipment, but they offer one-on-one patient ratios and often pay competitive hourly rates.
Telehealth has created some new adjacent roles too. While CNAs can't provide remote patient care, some pediatric practices hire CNAs to support virtual visits -- managing in-office equipment, coordinating follow-ups, and handling patient intake when families come in for procedures that can't be done remotely. It's a niche but growing area that blends traditional CNA skills with tech-forward healthcare delivery. Whatever setting appeals to you, the core requirement stays the same: genuine compassion for young patients and the willingness to adapt to their unique needs.
Searching for a pediatric cna near me position? Start by mapping out every children's hospital, pediatric urgent care, and specialty clinic within your commute range. Google Maps works surprisingly well for this -- search "children's hospital" or "pediatric clinic" and you'll get a visual overview of what's nearby. Most facilities list CNA openings on their careers page before they hit Indeed or ZipRecruiter.
Pediatric cna classes are available through most community colleges, Red Cross chapters, and some hospital-based training programs. Costs range from $500 to $2,000 depending on your state and the program provider. Financial aid, workforce development grants, and employer-sponsored training can offset these costs significantly. Some children's hospitals run their own CNA training programs and guarantee a job offer to graduates -- these are competitive but absolutely worth pursuing.
Don't forget about state workforce agencies. Many states fund CNA training for qualifying residents, particularly those who are unemployed, underemployed, or transitioning careers. Programs like WIOA (Workforce Innovation and Opportunity Act) can cover tuition, testing fees, and even transportation costs. Check with your local American Job Center to see what's available in your area -- the resources are there, but you have to ask for them. Military spouses and veterans also qualify for additional training benefits through programs like MyCAA, which can fully cover CNA certification costs.
Every state requires background checks for CNAs working with pediatric populations. This typically includes a criminal history review, sex offender registry check, and sometimes fingerprinting. Some facilities also require drug screening. These checks can take 2-4 weeks, so start the process early when applying. Any history involving children will be closely scrutinized -- transparency during the application process is essential.
Understanding pediatric cna requirements is crucial before you invest time and money in training. Every state requires CNAs to complete a state-approved training program and pass a competency exam. The training hours vary -- Florida requires 120 hours, California mandates 150, and some states require as few as 75. Your program must include both classroom instruction and supervised clinical experience with actual patients.
For those pursuing a cna for pediatrics role specifically, additional requirements may apply depending on your employer. Many children's hospitals require what is a bls certification, and some prefer or require PALS. A few facilities ask for a minimum of six months of CNA experience before placing aides in pediatric units, though this isn't universal. If you're a new graduate targeting pediatrics immediately, look for hospitals with dedicated new-grad pediatric CNA residency programs.
Continuing education is part of the deal too. Most states require 12-48 hours of continuing education every two years to maintain your CNA certification. Some of these hours can be fulfilled through pediatric-specific training -- workshops on child abuse recognition, pediatric pain management, or developmental disabilities. These aren't just box-checking exercises; they make you a better caregiver and a stronger candidate for advancement into nursing roles. Staying current on pediatric best practices shows employers you're invested in long-term growth, not just collecting a paycheck.
CNA Practice Test Questions
Prepare for the CNA - Certified Nursing Assistant exam with our free practice test modules. Each quiz covers key topics to help you pass on your first try.
CNA Activities of Daily Living
CNA Exam Questions covering Activities of Daily Living. Master CNA Test concepts for certification prep.
CNA Aging Process
Free CNA Practice Test featuring Aging Process. Improve your CNA Exam score with mock test prep.
CNA Anatomy and Physiology Basics
CNA Mock Exam on Anatomy and Physiology Basics. CNA Study Guide questions to pass on your first try.
CNA Assisting with Daily Living
CNA Test Prep for Assisting with Daily Living. Practice CNA Quiz questions and boost your score.
CNA Assisting with Range of Motion Exercises
CNA Questions and Answers on Assisting with Range of Motion Exercises. Free CNA practice for exam readiness.
CNA Basic Human Anatomy and Age-Related Ch...
CNA Mock Test covering Basic Human Anatomy and Age-Related Changes. Online CNA Test practice with instant feedback.
CNA Basic Nursing Skills
Free CNA Quiz on Basic Nursing Skills. CNA Exam prep questions with detailed explanations.
CNA Basic Nursing Skills 10
CNA Practice Questions for Basic Nursing Skills 10. Build confidence for your CNA certification exam.
CNA Basic Nursing Skills 11
CNA Test Online for Basic Nursing Skills 11. Free practice with instant results and feedback.
CNA Basic Nursing Skills 1
CNA Study Material on Basic Nursing Skills 1. Prepare effectively with real exam-style questions.
CNA Basic Nursing Skills 12
Free CNA Test covering Basic Nursing Skills 12. Practice and track your CNA exam readiness.
CNA Basic Nursing Skills 13
CNA Exam Questions covering Basic Nursing Skills 13. Master CNA Test concepts for certification prep.
CNA Basic Nursing Skills 14
Free CNA Practice Test featuring Basic Nursing Skills 14. Improve your CNA Exam score with mock test prep.
CNA Basic Nursing Skills 15
CNA Mock Exam on Basic Nursing Skills 15. CNA Study Guide questions to pass on your first try.
CNA Basic Nursing Skills 16
CNA Test Prep for Basic Nursing Skills 16. Practice CNA Quiz questions and boost your score.
CNA Basic Nursing Skills 17
CNA Questions and Answers on Basic Nursing Skills 17. Free CNA practice for exam readiness.
CNA Basic Nursing Skills 18
CNA Mock Test covering Basic Nursing Skills 18. Online CNA Test practice with instant feedback.
CNA Basic Nursing Skills 19
Free CNA Quiz on Basic Nursing Skills 19. CNA Exam prep questions with detailed explanations.
CNA Basic Nursing Skills 20
CNA Practice Questions for Basic Nursing Skills 20. Build confidence for your CNA certification exam.
CNA Basic Nursing Skills 21
CNA Test Online for Basic Nursing Skills 21. Free practice with instant results and feedback.
CNA Basic Nursing Skills 2
CNA Study Material on Basic Nursing Skills 2. Prepare effectively with real exam-style questions.
CNA Basic Nursing Skills 3
Free CNA Test covering Basic Nursing Skills 3. Practice and track your CNA exam readiness.
CNA Basic Nursing Skills 4
CNA Exam Questions covering Basic Nursing Skills 4. Master CNA Test concepts for certification prep.
CNA Basic Nursing Skills 5
Free CNA Practice Test featuring Basic Nursing Skills 5. Improve your CNA Exam score with mock test prep.
CNA Basic Nursing Skills 6
CNA Mock Exam on Basic Nursing Skills 6. CNA Study Guide questions to pass on your first try.
CNA Basic Nursing Skills 7
CNA Test Prep for Basic Nursing Skills 7. Practice CNA Quiz questions and boost your score.
CNA Basic Nursing Skills 8
CNA Questions and Answers on Basic Nursing Skills 8. Free CNA practice for exam readiness.
CNA Basic Nursing Skills 9
CNA Mock Test covering Basic Nursing Skills 9. Online CNA Test practice with instant feedback.
CNA Basic Restorative Services
Free CNA Quiz on Basic Restorative Services. CNA Exam prep questions with detailed explanations.
CNA Basic Restorative Services 1
CNA Practice Questions for Basic Restorative Services 1. Build confidence for your CNA certification exam.
CNA Bathing and Dressing
CNA Test Online for Bathing and Dressing. Free practice with instant results and feedback.
CNA Body Mechanics
CNA Study Material on Body Mechanics. Prepare effectively with real exam-style questions.
CNA Career Advancement and Opportunities
Free CNA Test covering Career Advancement and Opportunities. Practice and track your CNA exam readiness.
CNA Career Opportunities and Benefits
CNA Exam Questions covering Career Opportunities and Benefits. Master CNA Test concepts for certification prep.
CNA Care for Residents with Cognitive Impa...
Free CNA Practice Test featuring Care for Residents with Cognitive Impairment. Improve your CNA Exam score with mock test prep.
CNA Care of Cognitively Impaired Residents
CNA Mock Exam on Care of Cognitively Impaired Residents. CNA Study Guide questions to pass on your first try.
CNA Care of Cognitively Impaired Residents 1
CNA Test Prep for Care of Cognitively Impaired Residents 1. Practice CNA Quiz questions and boost your score.
CNA Care Of Cognitively Impaired Residents 4
CNA Questions and Answers on Care Of Cognitively Impaired Residents 4. Free CNA practice for exam readiness.
CNA Common Medical Terms and Abbreviations
CNA Mock Test covering Common Medical Terms and Abbreviations. Online CNA Test practice with instant feedback.
CNA Communication and Interpersonal Skills
Free CNA Quiz on Communication and Interpersonal Skills. CNA Exam prep questions with detailed explanations.
CNA Communication and Interpersonal Skills 1
CNA Practice Questions for Communication and Interpersonal Skills 1. Build confidence for your CNA certification exam.
CNA Communication And Interpersonal Skills 4
CNA Test Online for Communication And Interpersonal Skills 4. Free practice with instant results and feedback.
CNA Eligibility and Qualifications
CNA Study Material on Eligibility and Qualifications. Prepare effectively with real exam-style questions.
CNA Emergency Procedure
Free CNA Test covering Emergency Procedure. Practice and track your CNA exam readiness.
CNA Ethics and Professionalism
CNA Exam Questions covering Ethics and Professionalism. Master CNA Test concepts for certification prep.
CNA Exam Structure and Content
Free CNA Practice Test featuring Exam Structure and Content. Improve your CNA Exam score with mock test prep.
CNA Feeding and Hydration
CNA Mock Exam on Feeding and Hydration. CNA Study Guide questions to pass on your first try.
CNA Infection Control
CNA Test Prep for Infection Control. Practice CNA Quiz questions and boost your score.
CNA Infection Control and Safety
CNA Questions and Answers on Infection Control and Safety. Free CNA practice for exam readiness.
CNA Isolation Precautions
CNA Mock Test covering Isolation Precautions. Online CNA Test practice with instant feedback.
CNA Legal & Ethical Behaviours
Free CNA Quiz on Legal & Ethical Behaviours. CNA Exam prep questions with detailed explanations.
CNA Legal & Ethical Behaviours 1
CNA Practice Questions for Legal & Ethical Behaviours 1. Build confidence for your CNA certification exam.
CNA Legal & Ethical Behaviours 4
CNA Test Online for Legal & Ethical Behaviours 4. Free practice with instant results and feedback.
CNA Mental Health and Social Services Needs
CNA Study Material on Mental Health and Social Services Needs. Prepare effectively with real exam-style questions.
CNA Mental Health and Social Services Needs 1
Free CNA Test covering Mental Health and Social Services Needs 1. Practice and track your CNA exam readiness.
CNA Mental Health And Social Services Needs 4
CNA Exam Questions covering Mental Health And Social Services Needs 4. Master CNA Test concepts for certification prep.
CNA Nutrition and Hydration Management
Free CNA Practice Test featuring Nutrition and Hydration Management. Improve your CNA Exam score with mock test prep.
CNA Patient Care Procedure
CNA Mock Exam on Patient Care Procedure. CNA Study Guide questions to pass on your first try.
CNA Personal Care Skills
CNA Test Prep for Personal Care Skills. Practice CNA Quiz questions and boost your score.
CNA Personal Care Skills 1
CNA Questions and Answers on Personal Care Skills 1. Free CNA practice for exam readiness.
CNA Personal Care Skills 4
CNA Mock Test covering Personal Care Skills 4. Online CNA Test practice with instant feedback.
CNA Personal Care Skills 5
Free CNA Quiz on Personal Care Skills 5. CNA Exam prep questions with detailed explanations.
CNA Personal Hygiene and Grooming
CNA Practice Questions for Personal Hygiene and Grooming. Build confidence for your CNA certification exam.
CNA Practice Test - Basic Nursing Skills #2
CNA Test Online for Practice Test - Basic Nursing Skills #2. Free practice with instant results and feedback.
CNA Practice Test - Basic Nursing Skills #2 1
CNA Study Material on Practice Test - Basic Nursing Skills #2 1. Prepare effectively with real exam-style questions.
CNA Preventing Patient Falls and Injuries
Free CNA Test covering Preventing Patient Falls and Injuries. Practice and track your CNA exam readiness.
CNA Promoting Resident Independence and Ch...
CNA Exam Questions covering Promoting Resident Independence and Choice. Master CNA Test concepts for certification prep.
CNA Proper Hand Hygiene and PPE Usage
Free CNA Practice Test featuring Proper Hand Hygiene and PPE Usage. Improve your CNA Exam score with mock test prep.
CNA Resident Rights and Communication
CNA Mock Exam on Resident Rights and Communication. CNA Study Guide questions to pass on your first try.
CNA Resident’s Rights
CNA Test Prep for Resident’s Rights. Practice CNA Quiz questions and boost your score.
CNA Resident's Rights 1
CNA Questions and Answers on Resident's Rights 1. Free CNA practice for exam readiness.
CNA Resident's Rights 4
CNA Mock Test covering Resident's Rights 4. Online CNA Test practice with instant feedback.
CNA Roles and Responsibilities
Free CNA Quiz on Roles and Responsibilities. CNA Exam prep questions with detailed explanations.
CNA Safety and Emergency Procedures
CNA Practice Questions for Safety and Emergency Procedures. Build confidence for your CNA certification exam.
CNA Safety and Emergency Procedures 1
CNA Test Online for Safety and Emergency Procedures 1. Free practice with instant results and feedback.
CNA Safety And Emergency Procedures 4
CNA Study Material on Safety And Emergency Procedures 4. Prepare effectively with real exam-style questions.
CNA Safety and Infection Control
Free CNA Test covering Safety and Infection Control. Practice and track your CNA exam readiness.
CNA Scope of Practice
CNA Exam Questions covering Scope of Practice. Master CNA Test concepts for certification prep.
CNA Skills and Competencies
Free CNA Practice Test featuring Skills and Competencies. Improve your CNA Exam score with mock test prep.
CNA Supporting Rehabilitation Activities
CNA Mock Exam on Supporting Rehabilitation Activities. CNA Study Guide questions to pass on your first try.
CNA The Nurse Aide's Role and Responsibili...
CNA Test Prep for The Nurse Aide's Role and Responsibilities. Practice CNA Quiz questions and boost your score.
CNA Time Management and Prioritization
CNA Questions and Answers on Time Management and Prioritization. Free CNA practice for exam readiness.
CNA Toileting and Elimination
CNA Mock Test covering Toileting and Elimination. Online CNA Test practice with instant feedback.
CNA Using Adaptive Devices
CNA Practice Questions for Using Adaptive Devices. Build confidence for your CNA certification exam.
The variety of cna jobs pediatrics offers keeps the work interesting even after years in the field. On a single shift at a children's hospital, you might take vitals on a newborn, help a six-year-old with crutches after a fracture, and sit with a teenager receiving chemotherapy. No two days feel the same, and that variety is a major reason pediatric CNAs report higher job satisfaction than their counterparts in long-term care or adult med-surg units.
Children's hospital cna roles also come with unique emotional rewards. You're part of a child's recovery story. Parents remember the CNA who held their baby's hand during a scary procedure or who made their child laugh on a rough day. Thank-you cards from families aren't uncommon -- and they mean something. These moments carry you through the harder shifts when outcomes aren't as hopeful.
Career advancement from pediatric CNA to pediatric nurse is a well-worn path. Many RN bridge programs give credit for CNA experience, and some hospitals offer tuition assistance specifically for CNAs pursuing nursing degrees. If you're using CNA work as a stepping stone -- and many people are -- pediatrics gives you clinical experience that directly applies to pediatric nursing programs.
Admissions committees notice that. Your time as a pediatric CNA isn't just a job; it's building the foundation for whatever comes next. Every skill you learn, every patient interaction you navigate, and every tough shift you survive adds to a resume that speaks for itself when you're ready to level up.
CNA Questions and Answers
About the Author
Registered Nurse & Healthcare Educator
Johns Hopkins University School of NursingDr. Sarah Mitchell is a board-certified registered nurse with over 15 years of clinical and academic experience. She completed her PhD in Nursing Science at Johns Hopkins University and has taught NCLEX preparation and clinical skills courses for nursing students across the United States. Her research focuses on evidence-based exam preparation strategies for healthcare certification candidates.
Join the Discussion
Connect with other students preparing for this exam. Share tips, ask questions, and get advice from people who have been there.
View discussion (3 replies)