Home Health CNA: Duties, Pay, and How to Get Started
Home health CNAs provide personal care in patients' homes. Learn about duties, pay ($30K-$42K), certification requirements, and how to find home health jobs.

What Is a Home Health CNA?
A home health CNA is a Certified Nursing Assistant who provides personal care and basic nursing services to patients in their own homes rather than in a hospital or nursing facility. You visit patients where they live — houses, apartments, assisted living communities — and help them with daily activities they can't safely do alone: bathing, dressing, toileting, meal preparation, medication reminders, mobility assistance, and monitoring vital signs. It's the same CNA skill set applied in a fundamentally different environment, and that environment changes almost everything about how the work feels day to day.
Home health is one of the fastest-growing sectors in healthcare because the population is aging and most people prefer to receive care at home rather than in institutions. The demand for home health CNAs has been climbing steadily for years and shows no sign of slowing down — the Bureau of Labor Statistics projects much-faster-than-average job growth for home health aides and personal care aides through the next decade.
For CNAs who want independence, schedule flexibility, and one-on-one patient relationships (rather than the fast-paced, multi-patient environment of a nursing facility), home health offers a distinctly different version of the CNA career.
Working as a home health CNA is different from facility-based CNA work in several important ways. You work independently without a nurse or supervisor in the room — you're the healthcare professional present in the patient's home, making real-time judgments about the patient's condition and reporting concerns to the supervising nurse by phone.
You typically see one patient at a time for 2–8 hours rather than caring for 8–12 patients simultaneously. You drive between patients' homes, which means you need reliable transportation. And you build deeper relationships with patients and families because you're entering their personal space and often become a trusted part of their daily routine.
This guide covers what home health CNAs do, how much they earn, what certification and training is needed, and how to find and succeed in home health positions. Whether you're a new CNA considering home health as your first role or an experienced facility CNA looking for a change of pace, the information here helps you evaluate whether home health is the right fit.
- What you do: Provide personal care (bathing, dressing, toileting, mobility), vital signs, meal prep, medication reminders, and companionship in patients' homes
- Where you work: Patients' private residences — houses, apartments, assisted living. You travel between locations
- Requirements: CNA certification (state-specific), valid driver's licence, reliable transportation, clean background check
- Typical pay: $14–$20/hour ($30,000–$42,000/year). Varies by state, agency, and experience. Some agencies pay mileage reimbursement
- Schedule: More flexible than facility work — shifts range from 2-hour visits to 8-12 hour live-in shifts. Some agencies offer self-scheduling
- Supervision: Work independently in the home; report to a supervising RN by phone. The RN creates the care plan you follow
- Growth sector: Home health is projected to grow 22%+ over the next decade — much faster than average for all occupations
How to Become a Home Health CNA
Step 1: Complete CNA Training and Certification
Step 2: Get a Clean Background Check and Reliable Transportation
Step 3: Apply to Home Health Agencies
Step 4: Complete Agency Orientation and Home Health Training
Step 5: Build Your Caseload and Schedule

Home Health CNA Duties and Daily Responsibilities
The core duties of a home health CNA are the same personal care skills you learned in CNA training — but the setting changes the context significantly. In a patient's home, you're adapting your skills to their specific environment, equipment, and preferences rather than working in a standardised facility room with hospital equipment at hand.
Personal care assistance is the primary function: helping patients bathe (often in their own shower or tub rather than a facility shower chair), dress, use the toilet, brush teeth, shave, and manage hair care. For patients with limited mobility, this includes safe transfers from bed to wheelchair, wheelchair to toilet, and other position changes — often without the ceiling lifts and Hoyer lifts available in facilities. Body mechanics and safe transfer techniques are critically important in home health because you're often working alone without another aide to help.
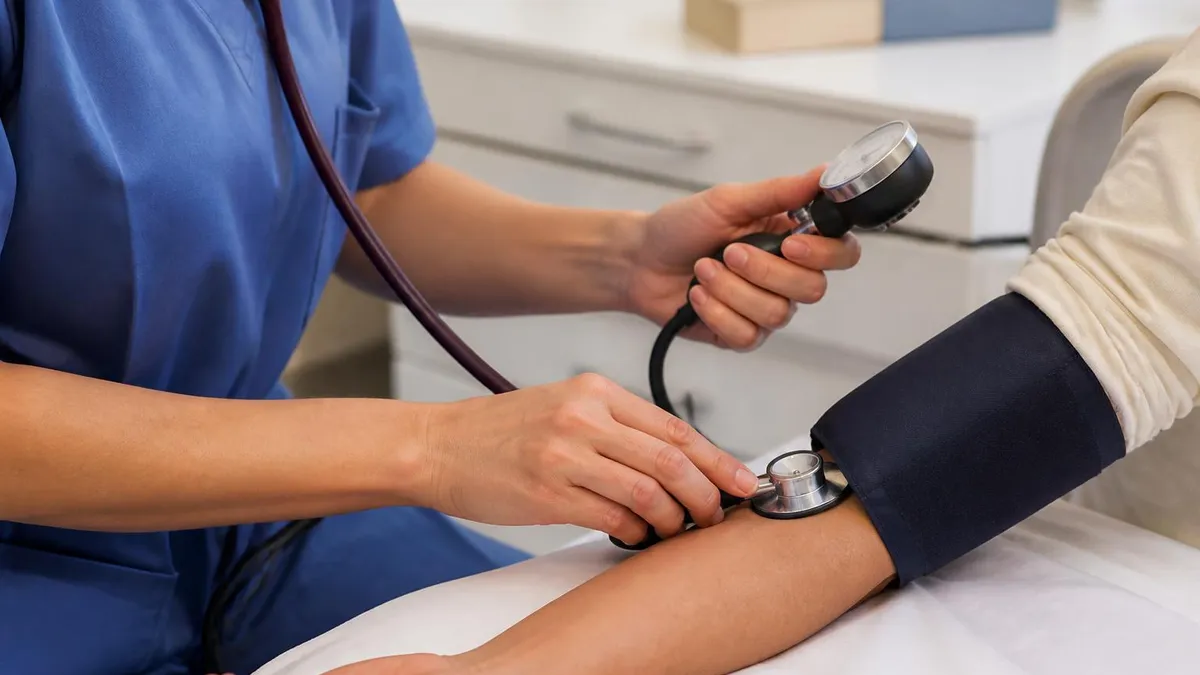
Vital signs monitoring (blood pressure, pulse, temperature, respiratory rate, weight) is typically done at each visit and documented for the supervising nurse. You report any significant changes — elevated blood pressure, fever, sudden weight gain, increased confusion — to the nurse immediately. In home health, you're often the first healthcare professional to notice subtle changes in a patient's condition because you see them regularly and know their baseline. Your observations and timely reporting can prevent hospitalisations.
Meal preparation and nutrition support involves preparing meals according to any dietary restrictions (diabetic, low-sodium, renal diet), ensuring adequate fluid intake, and monitoring whether the patient is actually eating. Some patients need feeding assistance. Grocery shopping or meal planning may also be part of the care plan depending on the agency and the patient's insurance coverage. Nutrition is a bigger focus in home health than in facilities because there's no facility kitchen providing three meals a day — the CNA may be the only person ensuring the patient eats properly.
Light housekeeping related to the patient's immediate environment — changing bed linens, tidying the bathroom after bathing assistance, washing dishes used during meal preparation — is common in home health. You're not a housekeeper, and heavy cleaning isn't part of the CNA role, but maintaining a safe and sanitary environment in the patient's living space is. Some patients and families blur this boundary — being clear about your role and referring to the care plan when boundaries are tested is an important professional skill.
Documentation is done either on paper forms or through a mobile app (increasingly common) at each visit. You record what care was provided, the patient's condition, vital signs, any concerns or changes observed, and the time spent. Documentation in home health must be thorough because the supervising nurse relies on your notes to make clinical decisions without being physically present. Incomplete or vague documentation can lead to missed clinical problems and creates compliance risk for the agency.
Companionship and emotional support are often undervalued in job descriptions but are among the most important aspects of home health CNA work. Many home-bound patients are socially isolated — you may be the only person they interact with all day. Conversation, encouragement, and genuine human connection are therapeutic in ways that go beyond physical care tasks. Patients who feel emotionally supported and valued tend to have better health outcomes, better appetite, and greater willingness to participate in their own care. This relational dimension is what makes home health feel less like task completion and more like meaningful caregiving.
Home Health CNA vs Facility CNA: Key Differences
In a facility, a nurse is down the hall if you have a question or concern. In home health, you're alone with the patient — the supervising nurse is available by phone but isn't physically present. This means more independent judgment: you decide when something is concerning enough to call, you handle unexpected situations in real time, and you manage the visit without direct supervision. For CNAs who want more autonomy, this is liberating. For those who prefer having immediate backup available, it can feel isolating.
Facility CNAs care for 8–12 patients per shift and may rotate between halls or units. Home health CNAs see the same patients regularly — often for months or years — and develop deep one-on-one relationships. You become part of the patient's life in a way that facility rotations don't allow. Many home health CNAs cite these relationships as the most rewarding aspect of the work. The trade-off: when patients decline or pass away, the emotional impact is more personal because of the depth of the relationship.
Home environments lack the assistive equipment that facilities have — hospital beds with adjustable height, ceiling lifts for transfers, shower chairs bolted to walls, and call light systems. You may need to help a 200-pound patient transfer from a regular bed to a wheelchair without a Hoyer lift, or assist bathing in a standard tub without grab bars. Body mechanics, patient handling skills, and the ability to advocate for needed equipment (requesting the agency provide a shower chair, for example) are more important in home health.
Facility work means fixed 8 or 12-hour shifts assigned weeks in advance. Home health offers more scheduling flexibility — you can often choose morning or afternoon visits, pick up extra patients when you want more hours, or reduce your caseload during slower weeks. Some agencies offer self-scheduling where you build your own schedule around patient availability. The trade-off: home health income can be less predictable if patient cancellations or hospitalisations reduce your hours unexpectedly.
Home Health CNA Pay and Benefits
Home health CNA compensation varies by state, agency, experience, and whether you work for an agency or through a private arrangement:
- Hourly range: $14–$20/hour for most home health CNA positions, with experienced CNAs in high-cost-of-living areas earning $18–$22+
- Annual salary: $30,000–$42,000 for full-time home health CNAs (40 hours/week)
- Mileage reimbursement: Many agencies pay $0.50–$0.67 per mile for travel between patients — this adds meaningful income for CNAs driving 50+ miles per day
- Weekend/holiday premiums: Some agencies pay $1–$3/hour extra for weekend, holiday, or evening shifts
- Private duty (non-agency): CNAs who work directly for families (without an agency) can earn $18–$30/hour, but sacrifice benefits, consistent scheduling, and liability coverage
Finding Home Health CNA Jobs
Home health CNA positions are abundant in virtually every market — the challenge isn't finding openings but identifying agencies that offer fair pay, reasonable caseloads, and supportive management. Here's how to find and evaluate opportunities.
Online job boards (Indeed, ZipRecruiter, Care.com) list home health CNA positions from both agencies and private families. Search 'home health CNA,' 'home health aide,' or 'in-home caregiver' plus your city. Filter by pay range and schedule requirements. Agency positions provide more stability, benefits, and liability coverage than private-duty arrangements, though private-duty may pay higher hourly rates for experienced CNAs.
State Medicaid waiver programmes are a major source of home health CNA jobs. These programmes fund in-home care for elderly and disabled Medicaid recipients, and they contract with agencies to provide CNA services. Your state's Medicaid website or aging services department can point you toward agencies participating in these programmes. Waiver programme positions tend to offer consistent hours because the patients have ongoing, funded care plans.
When comparing agencies, ask about: hourly pay rate (not just 'competitive pay'), mileage reimbursement policy, how patients are assigned (can you refuse cases?), maximum driving distance between patients, what happens when a patient cancels (do you still get paid for that time slot?), and what supervision and support is available when you're in the field. The best agencies treat their CNAs as professionals, provide responsive supervisory support, and don't overload them with unrealistic caseloads or excessive driving.
Networking with other home health CNAs provides the most honest information about which agencies to work for — and which to avoid. CNA forums, local healthcare Facebook groups, and conversations with other aides at training sessions or certification renewals give you insider perspectives that agency recruiters won't share. An agency with great marketing but high turnover and frequent missed paycheques isn't a good employer regardless of what their job posting says.
Consider trying per diem or part-time home health first if you're transitioning from facility work. This lets you experience the home health environment — the independence, the driving, the one-on-one care model — without fully committing before you know whether it fits your work style. Many CNAs who try a few home health shifts find they strongly prefer it to facility work; others discover they miss the team environment and immediate backup that facilities provide. A trial period removes the guesswork from the decision.
Is Home Health CNA Right for You?
- ✓You prefer working independently without constant supervision — home health requires self-direction and comfort making decisions alone
- ✓You enjoy one-on-one patient relationships rather than caring for many patients simultaneously
- ✓You have reliable personal transportation and don't mind driving between patient homes throughout the day
- ✓You're comfortable entering patients' private homes and adapting your care to different environments and household situations
- ✓You can maintain professional boundaries — patients and families may ask for help beyond your scope or try to blur personal and professional lines
- ✓You're a strong communicator who can clearly report patient concerns to a supervising nurse by phone without visual cues
- ✓You want schedule flexibility — home health offers more control over your hours than facility-based work in most cases
Home Health CNA: Pros and Cons
- +Greater independence and autonomy — you manage patient visits independently without a supervisor looking over your shoulder
- +Deeper patient relationships — seeing the same patients regularly for months or years creates meaningful connections that facility rotations don't allow
- +Schedule flexibility — many agencies offer self-scheduling, and the variety of shift lengths (2-hour visits to 12-hour shifts) accommodates different lifestyle needs
- +Growing demand — the aging population and preference for home-based care create strong, consistent job availability with no sign of decreasing
- −Working alone — no immediate backup if a patient falls, has an emergency, or if you feel uncomfortable in a home environment
- −Travel between patients — driving adds unpaid time (unless mileage is reimbursed), vehicle wear, and weather challenges that facility CNAs don't face
- −Income variability — patient cancellations, hospitalisations, or deaths reduce your hours unpredictably. Full-time hours aren't always guaranteed
- −Limited equipment — patients' homes often lack assistive devices (lifts, hospital beds, shower chairs), making physical care more demanding on your body

Safety Considerations for Home Health CNAs
Working in patients' homes involves safety considerations that don't exist in controlled facility environments. Being aware of potential risks and knowing how to manage them protects both you and your patients.
Personal safety in unfamiliar homes is the primary concern most new home health CNAs have. You're entering private residences — some in safe neighbourhoods, others in areas with higher crime rates. Practical safety measures include: always letting your agency know your schedule and location, keeping your phone charged and accessible, trusting your instincts if a home environment feels unsafe, and knowing that you have the right to leave any situation where you feel threatened. Reputable agencies have policies for handling unsafe environments and won't punish you for refusing a visit due to safety concerns.
Infection control in home settings requires adapting hospital-grade practices to residential environments. You bring your own gloves and hand sanitiser because the patient's home won't have a supply closet. Hand hygiene between tasks, proper handling of soiled linens and personal care supplies, and maintaining clean technique during wound care (if in your scope) are your responsibility to maintain without institutional reminders and supplies.
Ergonomic safety — protecting your back and joints during patient care — is more challenging in homes without assistive equipment. Beds that are too low, bathrooms without grab bars, and cramped spaces that don't allow proper body mechanics all increase injury risk. Advocate for needed equipment through your agency: many insurance programmes cover hospital beds, shower chairs, and other assistive devices for home patients. If a transfer feels unsafe without a lift, communicate this to your supervising nurse rather than risking injury.
Home Health CNA: Key Numbers
Advancing Your Career From Home Health CNA
Home health CNA experience is valuable for career advancement because it demonstrates independence, clinical judgment, and the ability to work without direct supervision — qualities that employers and nursing programmes value highly.
Many home health CNAs advance to Home Health Aide (HHA) certification, which expands their scope to include more complex tasks like medication administration in some states. The HHA certification builds on CNA training with additional home health-specific education. Some agencies require HHA certification for certain patient assignments, and it typically comes with a pay increase.
The LPN (Licensed Practical Nurse) pathway is a common next step for CNAs who want to advance their clinical scope significantly. LPN programmes take 12–18 months and qualify you to administer medications, perform assessments, and work under less supervision. Home health LPNs earn $45,000–$60,000+ and handle more complex patients than CNAs. Many LPN programmes give credit for CNA experience, and your home health background makes you a stronger LPN applicant because you've already demonstrated the independent judgment that LPN practice requires.
Even without advancing to a new credential, experienced home health CNAs can progress within the field by specialising in higher-acuity patients (ventilator-dependent patients, patients with complex wound care needs, paediatric home health), becoming a field trainer who orients new CNAs, or transitioning into an office-based care coordinator role that schedules and manages other aides.
Longevity and reliability in home health are valued — agencies invest in retaining experienced CNAs who have strong patient relationships and consistently positive performance evaluations from patients and families. Building a reputation as a reliable, skilled, and compassionate home health CNA creates career stability that transcends any single agency.
The RN pathway (through an ADN or BSN programme) is the most significant advancement. CNAs who earned their nursing degrees often cite their home health experience as formative — the one-on-one patient care, the clinical observation skills, and the independent decision-making all translate directly to nursing practice. Several CNA-to-RN bridge programmes specifically value home health experience in their admissions criteria.
In some states, 'Home Health CNA' and 'Home Health Aide (HHA)' are different credentials with different scopes of practice. A CNA certification qualifies you for personal care and basic nursing tasks. An HHA certification (required in some states, optional in others) adds home health-specific training and may expand your scope to include medication assistance, more complex vital signs monitoring, or specific medical device management. Check your state's requirements — some states require HHA certification specifically for Medicare-funded home health; others accept CNA certification alone. Your agency should clarify which credential they require and provide any additional training needed for your role.
The Emotional Rewards and Challenges of Home Health
Home health CNA work is uniquely rewarding emotionally — and uniquely challenging. The depth of relationship you develop with patients who you see regularly in their most personal environment creates bonds that facility work rarely matches. You're not just a caregiver passing through a patient's room; you become a consistent, trusted presence in their daily life. Many home health CNAs describe their patients as extended family.
The reward of helping someone maintain independence in their own home is significant. For elderly patients, staying home rather than moving to a facility represents dignity, comfort, and connection to their life history. You're the person who makes that possible — your care allows them to stay in the environment they choose rather than being institutionalised. That sense of purpose and direct impact keeps many CNAs in home health for their entire careers.
The challenges are real too. Patient decline and death hit harder when you've known someone for months or years in their personal space. Boundaries can blur when families treat you as a friend or family member rather than a healthcare professional — which creates complications when you need to set limits or transition away from a case.
And working alone means processing difficult emotions without the immediate support of colleagues who understand what you're going through. Finding peer support — through agency support groups, CNA networks, or informal connections with other home health aides — helps manage the emotional demands of the work.
Home Health CNA Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.