What Does MRI Show? Complete Guide to Magnetic Resonance Imaging
What does MRI show? Complete guide to brain, spine, joints, abdomen, and cardiac MRI findings, plus sequences, contrast use, and clinical applications.
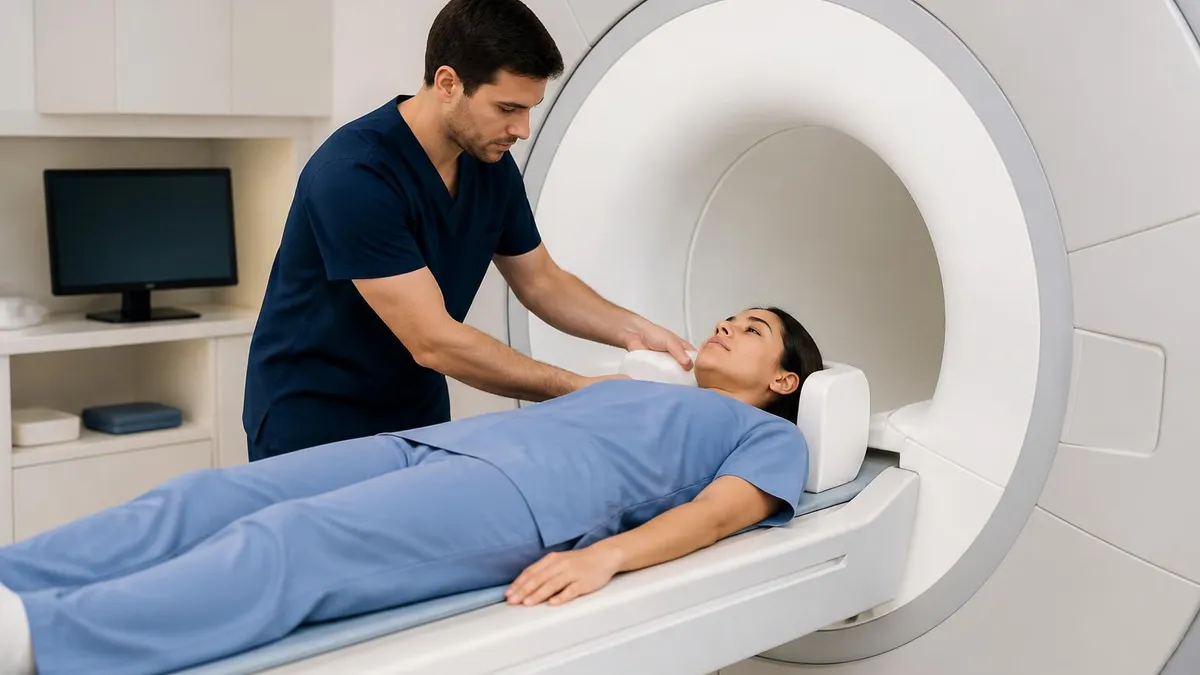
When a clinician orders an MRI, the first question patients ask isn't always about the machine or the noise. It's about the picture. What will the radiologist actually see when those images load on the workstation? The answer is broader than most people expect.
Magnetic resonance imaging visualizes soft tissue in a way no other modality can match, mapping water content, fat, blood flow, inflammation, and the subtle architecture of nerves and joints. A single scan can confirm a torn meniscus, flag an early demyelinating lesion, stage a tumor, or rule out a vascular malformation.
The exam tells a story about anatomy and physiology at the same time, and that combination is what makes MRI indispensable across neurology, orthopedics, oncology, cardiology, and abdominal medicine.
This article walks through what MRI shows organ by organ, why certain sequences highlight certain pathologies, and what the technologist and radiologist look for during interpretation.
If you're studying for the ARRT MRI registry or the ARMRIT exam, the mental model here will help you connect protocol selection to clinical question. If you're a patient or referring provider, you'll come away with a clearer sense of what the report is describing and why your physician chose MRI over CT, ultrasound, or nuclear medicine.
MRI by the Numbers
The physics in one sentence
Before we get into the specifics, it helps to remember the physics in one sentence. MRI generates contrast by exciting hydrogen protons inside the body with a radiofrequency pulse, then listening to the signal those protons emit as they relax back to equilibrium inside a strong magnetic field.
Different tissues relax at different rates. By manipulating timing parameters the scanner emphasizes one tissue characteristic over another. That's why a T1-weighted brain scan looks completely different from a T2-weighted brain scan of the same patient acquired five minutes later. Same anatomy, different physics, different diagnostic information.
The technologist controls these timing parameters, called TR and TE, alongside dozens of other variables that shape the final image. Sequence selection isn't a single decision either. A complete brain exam typically includes six to ten different acquisitions, each designed to highlight a specific tissue property or pathology.
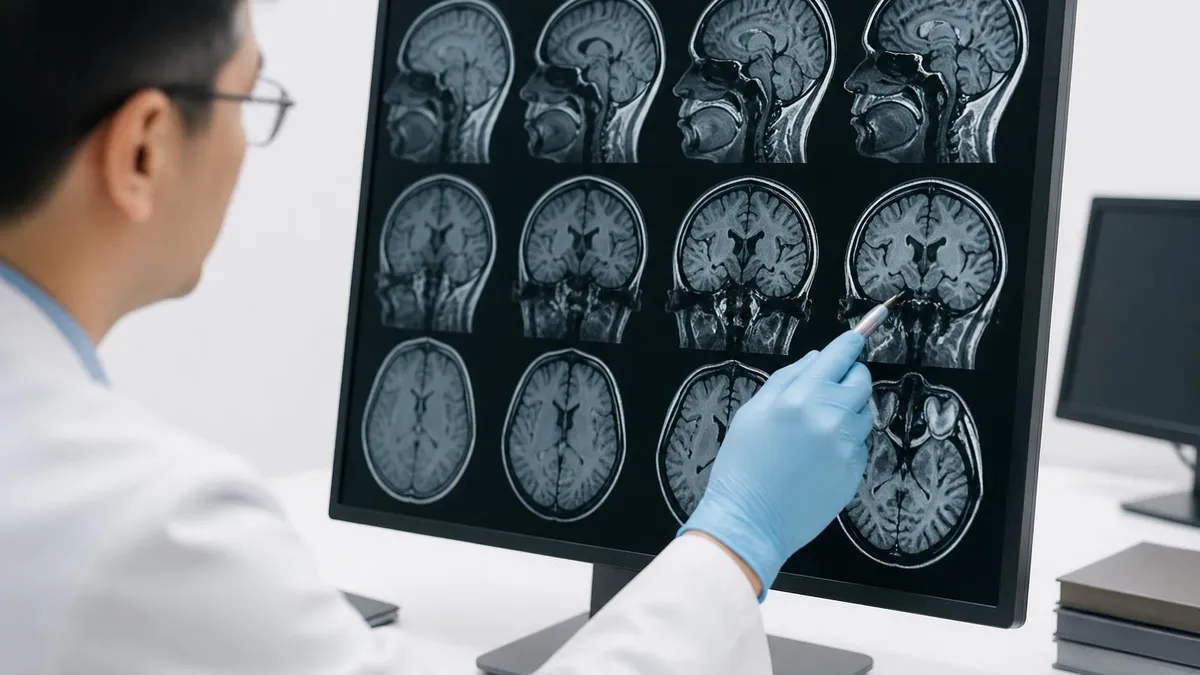
The core principle
MRI doesn't show one thing. It shows whatever the pulse sequence is designed to highlight. A radiologist reading a knee study toggles between proton density, T2 fat-suppressed, and T1 images to see cartilage, fluid, and marrow separately. The machine is the same. The questions being asked are different.
What MRI shows in the brain and spine
Neuroimaging is the largest single application of MRI worldwide, and for good reason. The brain is mostly water and lipid, two substances MRI distinguishes with surgical precision.
On a standard brain protocol the radiologist evaluates gray and white matter contrast, ventricular size and shape, the corpus callosum, brainstem, cerebellum, cranial nerves, vascular structures, and the meninges.
T1 sequences provide anatomic detail and are the workhorse for post-contrast imaging when looking for tumors, infection, or breakdown of the blood-brain barrier. T2 and FLAIR sequences make pathology jump off the screen because most disease processes increase tissue water content, and water is bright on T2.
Multiple sclerosis lesions, small vessel ischemic disease, encephalitis, abscess, and acute infarct all become visible on FLAIR before they're appreciable on any other sequence. Diffusion-weighted imaging adds another layer entirely, detecting restricted water movement within minutes of an ischemic stroke long before CT shows hypodensity.
Susceptibility-weighted imaging picks up microbleeds, cavernous malformations, and calcifications that other sequences miss. The combination of these acquisitions transforms a question like why is this patient having seizures into a confident diagnosis of mesial temporal sclerosis or a low-grade glioma.
For the spine, MRI shows disc hydration, herniations, nerve root impingement, cord signal abnormalities, marrow infiltration, and ligamentous injury. It's the only modality that reliably visualizes the spinal cord itself, which is why every suspected myelopathy ends up in the magnet.
Whether the question is cervical radiculopathy from a paracentral disc, lumbar canal stenosis from facet hypertrophy, or intramedullary tumor in a young adult with progressive weakness, the MRI report builds the surgical plan.
What MRI Shows by Body System
Tumors, stroke, demyelination, hemorrhage, hydrocephalus, infection, congenital anomalies, cranial nerve disorders, epilepsy workup, dementia evaluation
Disc disease, stenosis, cord compression, syrinx, marrow lesions, infection, post-surgical changes, scoliosis evaluation
Ligament tears, meniscal injury, cartilage defects, marrow edema, soft tissue masses, occult fractures, tendinopathy, joint effusions
Liver lesions, pancreatic ducts, adrenal masses, prostate cancer, uterine fibroids, ovarian cysts, rectal staging, inflammatory bowel disease
Cardiomyopathy characterization, viability assessment, congenital heart disease, pericardial disease, valve function, myocarditis
Aneurysms, dissections, stenoses, malformations via MR angiography with or without contrast, peripheral arterial disease
Musculoskeletal MRI and the soft tissue advantage
Orthopedic surgeons used to operate on a hunch and an X-ray. MRI changed that completely.
Today no major joint surgery happens without prior MRI confirmation of the suspected pathology, because the modality shows ligaments, tendons, menisci, labrum, articular cartilage, and bone marrow with a clarity that arthroscopy can only confirm.
A knee MRI demonstrates whether the anterior cruciate ligament is intact, partially torn, or completely ruptured. It localizes meniscal tears to the anterior horn, body, or posterior horn and grades them by morphology.
It identifies bone bruises from impaction injuries, occult fractures invisible on radiographs, and chondral defects that explain persistent pain after a normal X-ray. The radiologist also comments on extensor mechanism integrity, popliteal cyst formation, and incidental findings like loose bodies in the joint space.
Shoulder MRI maps the rotator cuff tendon by tendon. The radiologist measures any tear, comments on retraction and atrophy, evaluates the labrum for SLAP and Bankart lesions, and assesses the long head of the biceps tendon. Subacromial bursitis, acromioclavicular arthropathy, and glenohumeral synovitis round out the standard report.
Hip MRI catches labral tears, femoroacetabular impingement morphology, avascular necrosis at stages invisible to CT, and stress fractures of the femoral neck before they complete.
Wrist, ankle, elbow, and small joint imaging follows the same principle. Whenever soft tissue matters and surgical planning depends on tissue integrity, MRI is the answer.
Common MRI Sequences and What They Show
Anatomy sequence. Fat is bright, water is dark, gray matter is darker than white matter. Used as a baseline for post-contrast imaging because gadolinium shortens T1 and makes enhancing tissue bright. Excellent for showing brain anatomy, marrow signal, and subacute hemorrhage in the methemoglobin phase.
Abdominal and pelvic imaging
The abdomen is the technical frontier of body MRI because peristalsis and respiration both move the organs you're trying to image. Modern protocols solve this with breath-held acquisitions, navigator-triggered sequences, and rapid single-shot techniques.
The payload is impressive. Liver MRI characterizes lesions with confidence using a combination of T1 in and out of phase, T2, diffusion, and dynamic contrast with extracellular or hepatobiliary agents.
The radiologist can usually distinguish a benign hemangioma from focal nodular hyperplasia from hepatocellular carcinoma without biopsy, something CT cannot reliably do.
MRCP visualizes the biliary tree and pancreatic duct using heavily T2-weighted sequences that make fluid-filled structures bright on a black background. It has replaced diagnostic ERCP for most indications because it's noninvasive and provides comparable anatomic detail.
Patients with suspected choledocholithiasis, primary sclerosing cholangitis, or postoperative biliary complications routinely get MRCP before any interventional procedure is considered.
Pelvic MRI is the gold standard for prostate cancer detection and staging using the PI-RADS framework, for endometriosis mapping, for uterine and adnexal mass characterization, and for rectal cancer staging.
The high soft tissue contrast lets surgeons plan margins and oncologists decide on neoadjuvant therapy. In rectal cancer specifically, the report drives the multidisciplinary tumor board discussion about whether the patient receives chemoradiation before surgery or proceeds directly to total mesorectal excision.
Gadolinium-based contrast agents enhance vascular structures, breakdown of the blood-brain barrier, and tumor neovascularity. They're generally safe but require kidney function review before administration in patients with reduced GFR due to historical concerns about nephrogenic systemic fibrosis with older linear agents. Modern macrocyclic agents have dramatically reduced this risk and remain the standard of care.
Cardiac MRI and the rise of tissue characterization
Cardiac MRI used to be a niche application. It's now a frontline tool for ischemic and nonischemic cardiomyopathy evaluation because it does something echocardiography cannot. It characterizes the myocardium itself.
Late gadolinium enhancement reveals scar from prior infarction, the distribution patterns of infiltrative diseases like amyloidosis and sarcoidosis, and the midwall fibrosis typical of dilated cardiomyopathy.
T1 and T2 mapping quantify edema and diffuse fibrosis without contrast, opening windows into myocarditis, iron overload, and amyloid burden that no other imaging modality provides.
The exam also delivers gold-standard measurements of ventricular volumes, ejection fraction, and mass, which matter for decisions about device therapy and surgical timing.
For congenital heart disease, MRI follows patients across decades because it avoids the cumulative radiation burden of repeat CT and catheterization while answering anatomic and functional questions in the same study.
Stress perfusion CMR detects inducible ischemia in patients who can't tolerate exercise testing or have body habitus limiting echocardiographic windows, and the diagnostic accuracy rivals invasive coronary angiography for major epicardial disease.
MRI Exam Workflow Checklist
- ✓Confirm clinical question matches modality strength before scheduling
- ✓Screen for ferromagnetic implants, pacemakers, and cochlear devices
- ✓Review renal function if contrast is planned
- ✓Educate patient about scan duration, noise, and breath holds
- ✓Verify IV access for contrast or stress agents if applicable
- ✓Position patient with appropriate coil for the body part
- ✓Acquire localizers and confirm coverage before main sequences
- ✓Monitor patient throughout exam, especially if sedated
- ✓Verify image quality at the console before patient leaves the magnet
- ✓Transfer studies to PACS and confirm radiologist receipt
Vascular imaging without iodinated contrast
MR angiography shows arterial and venous anatomy throughout the body with or without contrast injection. Time-of-flight techniques exploit the inflow of fresh unsaturated blood into the imaging slab to generate bright vessel signal against a suppressed stationary background.
They're routine for circle of Willis evaluation in stroke and aneurysm workups. The 3D reconstructions let neurointerventionalists plan coiling and clipping approaches before the patient ever reaches the angiography suite.
Phase contrast adds velocity quantification, useful for shunt assessment and CSF flow studies in normal pressure hydrocephalus and Chiari malformation workups.
Contrast-enhanced MRA delivers fast, high-resolution arterial trees of the carotids, renal arteries, mesenteric circulation, peripheral arteries, and aorta. The bolus timing must be precise so the gadolinium is in the artery of interest during acquisition rather than the venous return phase.
For patients who can't tolerate iodinated contrast or radiation, gadolinium-enhanced MRA or non-contrast techniques like quiescent interval slice selective offer credible alternatives to CT angiography.
The diagnostic accuracy is high enough that vascular surgeons frequently operate based on MRA findings alone. In the setting of suspected dissection, MRI also shows the intramural hematoma and the dissection flap with exceptional clarity.
MRI Strengths and Limitations
- +Superior soft tissue contrast versus all other modalities
- +No ionizing radiation, safe for repeat imaging in young patients
- +Multiplanar acquisition without repositioning
- +Functional information alongside anatomy through diffusion, perfusion, and spectroscopy
- +Tissue characterization via multiple contrast mechanisms in a single exam
- +Noninvasive alternative to many diagnostic procedures including ERCP and angiography
- −Long scan times that strain claustrophobic or pediatric patients
- −Contraindicated or complicated by certain implants and foreign bodies
- −Higher cost and limited availability compared to CT and ultrasound
- −Sensitive to motion artifact from breathing, peristalsis, and patient movement
- −Acoustic noise requires hearing protection during the exam
- −Limited evaluation of calcifications, cortical bone detail, and lung parenchyma
What MRI shows that other modalities miss
The honest answer to what does MRI show is a different question entirely. What does MRI show that nothing else can?
Several things. Early ischemic stroke within the first hour. Multiple sclerosis plaques during a clinically isolated syndrome workup. Cartilage thickness and integrity for surgical planning.
Prostate cancer with enough specificity to guide targeted biopsy. Liver lesion characterization without sampling. Cardiac scar distribution that distinguishes ischemic from nonischemic cardiomyopathy.
Soft tissue tumor staging that determines neurovascular involvement. Pituitary microadenoma detection with dynamic contrast. Endometriosis mapping deep to peritoneal surfaces. These are the diagnostic questions that justify the cost and the time in the magnet.
Other modalities have their own strengths. CT remains faster for trauma and acute hemorrhage. Ultrasound is portable and excellent for many obstetric and superficial applications. Nuclear medicine answers metabolic questions MRI cannot.
The choice of imaging is never about which modality is best in isolation. It's about which one answers the specific clinical question with the least risk and the highest yield. MRI wins that calculation more often than any other modality when soft tissue is the issue.
This is why MRI utilization continues to grow even as alternatives mature. The breadth of clinical questions answerable in a single 30-minute exam keeps expanding as new sequences enter clinical practice. Synthetic MRI, MR fingerprinting, and ultrashort echo time imaging are already changing what radiologists see in everyday studies.
MRI Questions and Answers
How radiologists read an MRI study
The radiologist begins by reviewing the clinical history and prior imaging if available. Context shapes interpretation. A bright T2 lesion in a 28-year-old woman with optic neuritis has a different differential than the same lesion in a 75-year-old with hypertension and atrial fibrillation.
The reading workflow then scrolls through each sequence in a standardized order. Anatomic sequences first, then pathology-sensitive sequences, then post-contrast comparisons. Multiplanar reformats let the reader confirm findings on at least two orthogonal views before committing to a diagnosis.
For musculoskeletal studies, the radiologist walks the joint compartment by compartment. Knee reads cover the anterior, posterior, medial, and lateral compartments separately, with structured language for each ligament, tendon, meniscus, and cartilage surface.
For neurologic studies, the cortex, white matter, deep gray nuclei, posterior fossa, ventricles, and extra-axial spaces each get attention before incidental findings in the orbits, sinuses, and skull base are reported.
Post-contrast imaging adds a final layer. Enhancement patterns distinguish active demyelination from chronic plaques, viable tumor from necrosis, and acute infection from resolved disease.
The dictation finishes with an impression that prioritizes findings by clinical relevance. A small unrelated finding might appear in the body of the report but the impression leads with what matters for the patient's care plan.
Specialized MRI applications worth knowing
Beyond the routine indications, MRI supports a growing list of specialized exams that answer narrow questions exceptionally well.
Breast MRI screens women at high genetic risk for cancer and evaluates the extent of newly diagnosed disease before surgical planning. Dynamic contrast enhancement curves help separate benign lesions from malignancy with sensitivity that mammography cannot match.
Fetal MRI complements ultrasound for complex anomalies of the central nervous system, airway, and abdominal organs. The exam typically waits until the second or third trimester when fetal motion is less of a problem and the structures of interest are large enough to resolve.
Whole-body MRI screens for metastatic disease in patients with melanoma, multiple myeloma, and hereditary cancer syndromes without the radiation burden of repeated CT or PET-CT.
MR spectroscopy quantifies tissue metabolites and adds confidence to brain tumor characterization, mitochondrial disease workup, and prostate lesion evaluation. Functional MRI maps eloquent cortex before tumor resection so surgeons can preserve language and motor areas.
The diagnostic value of MRI depends on matching the right sequences to the clinical question. A negative MRI ordered without the right protocol can miss the diagnosis entirely, while a well-protocolled study delivers answers no other modality can provide. Always communicate the clinical concern to the imaging team so they can build the protocol that fits.
Bringing it together
What MRI shows depends entirely on the question being asked and the sequences chosen to answer it. The same magnet that maps brain anatomy can stage prostate cancer, characterize a liver lesion, evaluate a torn rotator cuff, detect early stroke, or quantify cardiac scar burden.
Understanding which sequence answers which question is the difference between a useful study and a wasted one. For technologists and radiologists, that understanding starts with the physics and grows with experience.
For referring clinicians and patients, it starts with knowing that MRI is uniquely suited to soft tissue evaluation and that the radiologist's report reflects a carefully designed combination of acquisitions, each chosen because it shows something the others cannot.
The next time you see an MRI ordered, you'll have a better sense of what's about to appear on the radiologist's screen and why it matters to the care plan that follows.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.