MRI Side Effects: Contrast Reactions, Claustrophobia, and What's Actually Common
MRI side effects: gadolinium contrast reactions, claustrophobia rates, transient warmth, peripheral nerve stimulation. Truly rare vs commonly-feared risks...
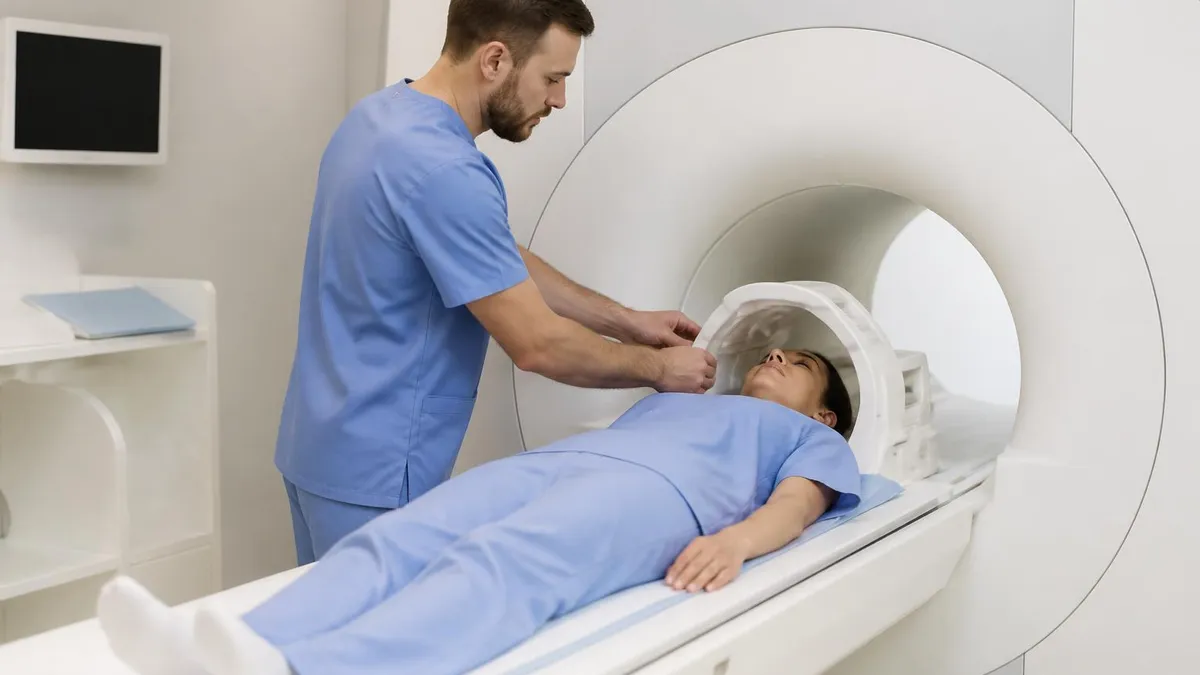
MRI side effects in actual practice are mostly minor and uncommon. The scan itself uses magnetic fields and radio waves — no ionizing radiation like X-rays or CT scans. The most common "side effects" patients experience are: mild claustrophobia during the scan (anxiety in the enclosed scanner bore), the loud knocking sounds that are normal for MRI sequences, and occasional sensations of warmth from radiofrequency energy. None of these are harmful; they're sensory experiences that some patients find unpleasant.
The more substantive side effects involve gadolinium-based contrast agents (GBCAs) when contrast is administered for specific scan types. Most MRI scans don't use contrast. When contrast is needed (typically for cancer detection, vascular imaging, or specific soft tissue conditions), the gadolinium agents are generally well-tolerated but have known risks worth understanding.
Acute contrast reactions are uncommon but possible. Mild reactions (nausea, headache, dizziness) occur in roughly 0.07-2.4% of contrast administrations. Moderate reactions (urticaria, vomiting, breathing difficulty) are rarer at 0.004-0.7%. Severe reactions (anaphylaxis-like) are very rare at less than 0.01%. For comparison, iodinated CT contrast has higher acute reaction rates — gadolinium is generally considered the safer contrast option.
Nephrogenic Systemic Fibrosis (NSF) is a serious but rare complication associated specifically with patients who have severe kidney disease (eGFR less than 30). NSF causes thickening and hardening of skin and connective tissues. Modern protocols screen kidney function before administering gadolinium, and risk has been substantially reduced by switching to macrocyclic gadolinium agents (more stable molecules less likely to release free gadolinium). NSF risk for patients with normal kidney function is essentially zero.
Gadolinium retention in brain tissue has been observed after repeated contrast exams. FDA has issued safety communications about this. The clinical significance remains uncertain — no specific health effects have been definitively linked to gadolinium retention in patients with normal kidney function. The FDA recommends using macrocyclic agents preferentially and limiting unnecessary repeat contrast exams. For patients with multiple contrast MRIs over years, this is worth discussing with the ordering physician.
This guide covers MRI side effects in detail — both the common minor experiences (claustrophobia, warmth, noise) and the substantive concerns (contrast reactions, kidney implications, gadolinium retention). It's intended for patients preparing for MRI scans, family members supporting patients, and healthcare workers helping educate patients about what to expect.
MRI Side Effects Quick Facts
- No radiation: MRI doesn't use ionizing radiation. No radiation-related side effects.
- Claustrophobia rates: ~5-10% of patients experience significant anxiety during scan
- Contrast reactions: Mild 0.07-2.4%, moderate 0.004-0.7%, severe less than 0.01%
- Common sensory experiences: Loud knocking sounds (normal), occasional warmth, mild claustrophobia
- NSF risk: Only patients with severe kidney disease (eGFR less than 30). Modern macrocyclic agents reduced risk substantially.
- Gadolinium retention: Detected in brain tissue after multiple contrast exams. Clinical significance uncertain.
- Pregnancy considerations: Non-contrast MRI generally safe; gadolinium not recommended in 1st trimester
- Implant safety: Pre-screening eliminates risk for patients with known implants
Claustrophobia during MRI scans affects roughly 5-10% of patients to varying degrees. The MRI scanner bore is typically 60-70 cm (24-28 inches) in diameter, and patients lie inside this enclosed cylinder for 20-60 minutes depending on the scan type. For some patients, this enclosed environment triggers anxiety ranging from mild discomfort to panic. About 1-2% of scheduled MRI scans are abandoned due to severe claustrophobia.
Modern MRI scanners come in different bore sizes. Standard closed-bore MRI scanners have the 60-70 cm bore most patients experience. Wide-bore scanners (70-80 cm) accommodate larger patients and reduce claustrophobic feelings. Open MRI scanners have C-shaped or open-side designs that significantly reduce claustrophobia but typically produce lower-quality images. The trade-off: open MRI works well for many scans but isn't optimal for high-resolution imaging.
Techniques for managing claustrophobia. Thorough pre-scan explanation of what to expect. Headphones with music (reduces noise stress). Mirror that lets patients see outside the bore. Brief breaks between sequences for severe anxiety. Mild oral sedation (Valium, Xanax) for patients with significant anxiety — prescribed by the ordering physician, taken before scan. The combination of these techniques helps most claustrophobic patients complete their scans.
For severe cases where sedation isn't sufficient, sedated MRI (with anesthesiology services) or open MRI alternatives are options. The cost and complexity is higher but the scan still happens. For patients who absolutely cannot tolerate MRI, alternative imaging (CT scan, ultrasound) may serve depending on the clinical question — though sometimes MRI is the only way to answer specific questions about soft tissue or specific organs.
The loud knocking sounds during MRI are normal and not actually a side effect, though many patients find them disturbing. The sounds come from rapidly switching gradient coils that generate the magnetic field gradients. Volume reaches 100-130 dB during sequences (similar to a jackhammer or rock concert). Hearing protection is mandatory — every patient gets earplugs or noise-canceling headphones. Permanent hearing damage from MRI is extremely rare with proper hearing protection.
Transient warmth during scans is common but generally harmless. The radiofrequency pulses that create the imaging signal generate small amounts of heat in body tissues. Most patients don't notice; some feel mild warmth, particularly during longer sequences or in larger body parts. Excessive warmth (skin burns) is the failure mode prevented by proper safety protocols — keeping skin from contacting metal coils, not creating closed conductive loops with patient positioning, and removing conductive items from the patient's body before the scan.
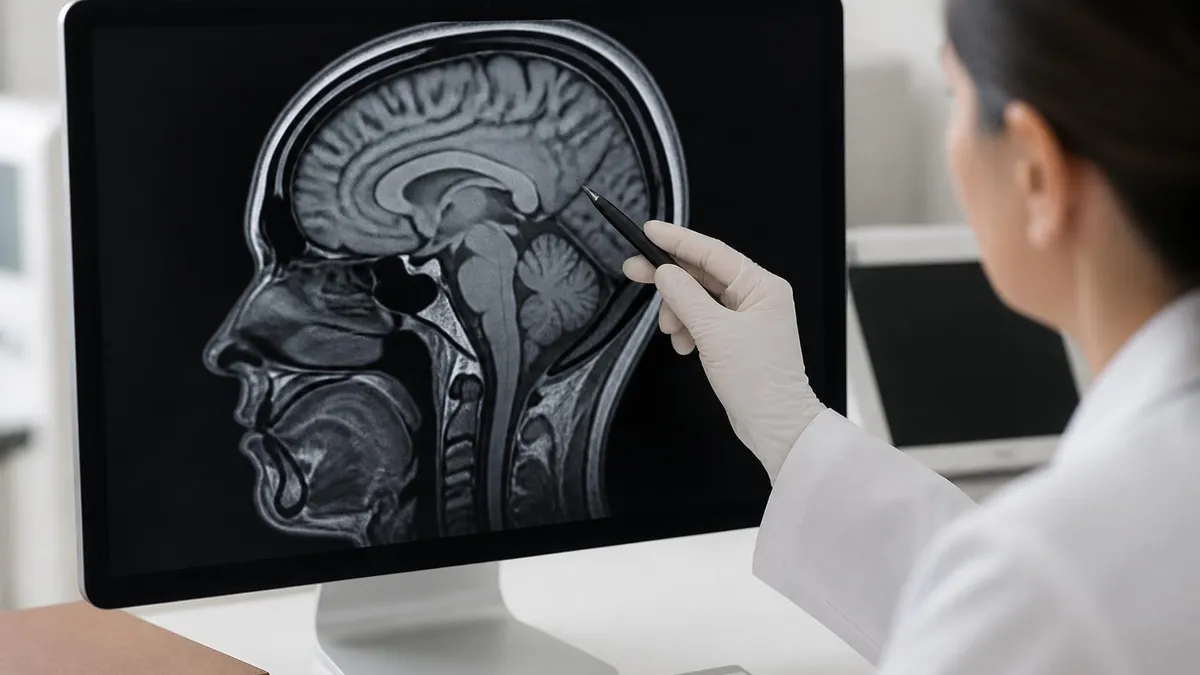
Common MRI Experiences
Normal during sequences. 100-130 dB volume. Hearing protection mandatory. Some find anxiety-inducing.
5-10% of patients. Wide-bore scanners or open MRI for severe cases. Sedation possible. Manageable with techniques.
From RF pulses. Mild, harmless for most. Excessive warmth preventable with proper positioning.
Brief muscle twitching from rapid gradient switching. Uncommon. Not harmful but can be startling.
Some patients near the bore opening feel slight vertigo. Brief sensation. Resolves on standing.
From gradient coil operations. Some patients describe feeling vibrations. Not harmful.
Gadolinium contrast side effects in detail. Most MRI scans do NOT use contrast. The exception is when specific clinical questions require contrast enhancement — typically cancer staging, vascular imaging, specific soft tissue conditions, and central nervous system imaging where contrast significantly improves diagnostic accuracy. For non-contrast scans, the only side effects are sensory ones discussed above.
When contrast is needed, the most common gadolinium-based contrast agents (GBCAs) are: Gadovist (gadobutrol), Magnevist (gadopentetate), Dotarem (gadoterate meglumine), Eovist (gadoxetate disodium), Multihance (gadobenate dimeglumine), and others. Each has slightly different characteristics. Macrocyclic agents (Gadovist, Dotarem, ProHance) are generally considered safer than linear agents (Magnevist, Optimark) because the macrocyclic chelate is more stable and less likely to release free gadolinium.
Acute reaction symptoms range widely. Mild reactions include: nausea, vomiting, headache, dizziness, mild skin warmth, brief itching at injection site. These resolve within minutes to hours without specific treatment. Moderate reactions include: hives (urticaria), more substantial itching, breathing difficulty, low blood pressure. These typically require observation and sometimes antihistamines or other symptomatic treatment. Severe reactions (anaphylactoid) include: laryngeal edema (airway swelling), severe hypotension, cardiac arrhythmia. These are emergencies requiring immediate intervention.
For patients with previous contrast reactions, the imaging center should be informed before the scan. Risk of recurrent reaction is higher for patients with prior reactions but still uncommon. Premedication protocols (corticosteroids and antihistamines started 12-24 hours before the scan) can reduce recurrent reaction risk for patients with prior reactions. Sometimes the alternative is to perform the MRI without contrast and accept reduced diagnostic accuracy.
Nephrogenic Systemic Fibrosis (NSF) is a specific complication for patients with severe kidney dysfunction. It causes thickening and hardening of skin and connective tissue, sometimes affecting internal organs. Onset can be days to months after contrast exposure. Modern protocols screen kidney function (eGFR) before contrast administration. Patients with eGFR less than 30 typically don't receive gadolinium; patients with eGFR 30-60 may receive macrocyclic agents only after individual risk assessment.
NSF risk has been dramatically reduced by: kidney function screening, preferential use of macrocyclic gadolinium agents, lower contrast doses, and dialysis for severely kidney-impaired patients if contrast is essential. Reported NSF cases in the past 10 years are dramatically reduced compared to the 2000s when the problem was first identified. For patients with normal kidney function, NSF risk is essentially zero.
MRI Side Effect Frequency
Gadolinium retention in brain tissue is a more recent concern that emerged in scientific literature around 2014-2015. Research showed that small amounts of gadolinium can deposit in specific brain structures (dentate nucleus, globus pallidus) after multiple contrast-enhanced MRI exams. The amounts are detectable by sensitive MRI sequences and by post-mortem tissue analysis.
The clinical significance of gadolinium retention is uncertain. No specific neurological symptoms have been definitively attributed to brain gadolinium retention in patients with normal kidney function. Several large studies have failed to find clear clinical effects. However, the long-term implications remain under study, and the FDA issued safety communications recommending judicious use of contrast.
The FDA's recommendations: use macrocyclic gadolinium agents preferentially (more stable, less likely to release free gadolinium). Limit unnecessary repeat contrast exams. Inform patients about gadolinium retention before contrast-enhanced exams. For patients receiving multiple contrast MRIs (cancer surveillance, MS monitoring, vascular disease follow-up), discuss the cumulative exposure with the ordering physician.
For patients concerned about gadolinium retention, several considerations help: most MRI scans don't need contrast — confirm with your physician whether contrast is essential for the specific clinical question; for cancer surveillance, consider whether the frequency of contrast MRIs can be reduced; for chronic conditions requiring repeat imaging, ask whether alternative imaging modalities (CT, ultrasound) might serve some monitoring needs. The decision is medical and depends on the individual case.
Pregnancy and MRI: non-contrast MRI is generally considered safe during pregnancy. The FDA has approved MRI for diagnostic purposes throughout pregnancy. However, contrast (gadolinium) is generally avoided in pregnancy, particularly in the first trimester. Animal studies have shown some fetal effects from gadolinium exposure; human data is limited. The standard recommendation: use non-contrast MRI whenever possible; reserve contrast for cases where the diagnostic benefit clearly outweighs unclear fetal risks.
Breastfeeding mothers can typically continue breastfeeding after gadolinium MRI. The American College of Radiology recommends continued breastfeeding because the amount of gadolinium that crosses into breast milk is very small, and the amount absorbed by the infant from the GI tract is even smaller. Some mothers prefer to pump and discard for 24 hours as a precaution, though this isn't medically required.
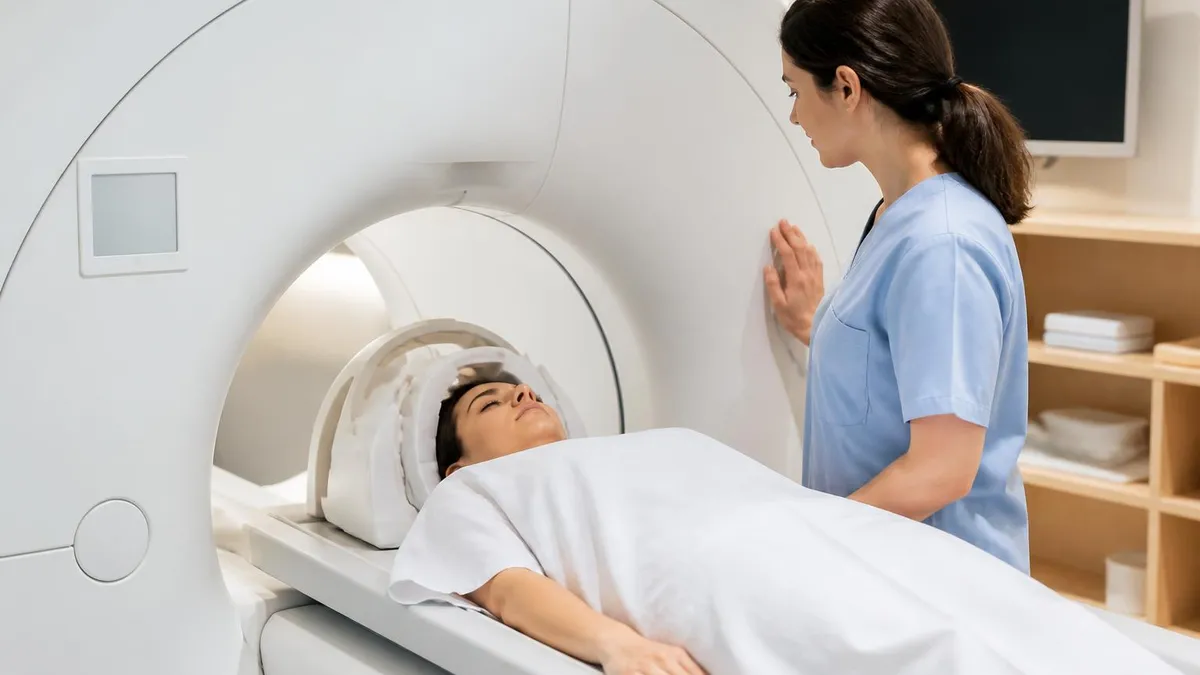
MRI Side Effects by Type
- Loud knocking: Normal, from gradient coils. Hearing protection mandatory.
- Warmth: From RF pulses. Mild, harmless for most.
- Vibration: From gradients. Some sensation; not harmful.
- Claustrophobia: 5-10% experience significant anxiety. Wide-bore or open MRI alternatives available.
- Peripheral nerve stimulation: Brief twitching from rapid gradient switching. Uncommon but startling.
Most MRI scans do NOT involve contrast administration. Brain MRIs, joint MRIs, spine MRIs, and many other types are typically done without contrast. Contrast is added when specific clinical questions require it — cancer staging, vascular imaging, central nervous system inflammation, specific soft tissue conditions. If you're worried about contrast side effects, ask the ordering physician whether your specific scan requires contrast. Many concerned patients are reassured to learn that their scheduled scan is non-contrast and most of the side effect concerns don't apply.
What to do if you experience side effects. During the scan: communicate with the technologist through the call button. If you feel unwell, dizzy, or panicked, press the button. The scan can be paused or stopped. The technologist monitors you continuously via camera and microphone. Don't try to "tough it out" if you're genuinely uncomfortable.
After contrast administration: stay in the waiting area for 15-30 minutes after the scan if contrast was used. Most reactions occur within this window. If you feel any symptoms (nausea, dizziness, hives, breathing difficulty), inform the imaging staff. Delayed reactions (1-24 hours after the scan) are less common but possible — if you experience symptoms after leaving, contact your physician or go to the emergency room.
For patients planning multiple contrast MRIs over years (cancer follow-up, multiple sclerosis monitoring, chronic disease management): discuss cumulative gadolinium exposure with your physician. Some clinics now keep cumulative dose records. The benefit-risk decision changes when you've already had 10+ contrast scans versus when you're considering your first one.
For pregnant women requiring MRI: discuss with both the ordering physician and the MRI department. Non-contrast MRI is the standard option; the diagnostic benefit must clearly outweigh any (mostly theoretical) fetal risks. Gadolinium contrast is generally avoided during pregnancy unless absolutely essential. Most pregnancy-related imaging can be done without contrast.
For patients with prior contrast reactions: the imaging center needs to know in advance. Premedication protocols substantially reduce recurrent reaction risk. Sometimes the safer option is performing the MRI without contrast and accepting somewhat reduced diagnostic accuracy. The conversation between you, the ordering physician, and the imaging center determines the right approach for your specific case.
For patients with severe kidney disease: discuss with your nephrologist and the ordering physician before contrast MRI. Modern protocols typically avoid gadolinium for eGFR less than 30; for eGFR 30-60, individual assessment determines approach. Sometimes alternative imaging (non-contrast MRI, CT, ultrasound) provides the needed information without contrast risk.
Reducing MRI Side Effect Risk
Ask if contrast is required. Many scans don't need it. Avoids contrast-related concerns entirely.
Tell imaging center about any previous contrast reactions, allergies. Premedication may be required.
eGFR test before contrast for at-risk patients. Most centers do this automatically; confirm if you have CKD.
Mention concerns to ordering physician. Consider wide-bore or open MRI for severe anxiety. Mild sedation available.
Imaging center provides earplugs or headphones. Use them. Hearing damage from MRI is rare but real risk.
Most reactions occur within this window. Imaging center expects you to wait. Inform staff of any symptoms.
Special populations and MRI side effect considerations. Pediatric patients: same physical safety considerations as adults, but anxiety management is more challenging. Many children require sedation for MRI scans to lie still through the procedure. Sedation has its own risks (mostly related to airway management) that require anesthesiology support. Contrast safety in pediatrics is generally similar to adults, with some specific dosing considerations.
Elderly patients: more likely to have underlying conditions (chronic kidney disease, cardiac conditions, prior contrast reactions) that affect MRI safety planning. Pre-scan screening is more thorough. The procedure itself is generally well-tolerated; the duration of lying still can be physically challenging for elderly patients with arthritis or other mobility issues.
Patients with implants (pacemakers, defibrillators, neurostimulators, cochlear implants, certain aneurysm clips): MRI safety depends on the specific implant. MR-conditional implants can be scanned at certain field strengths with specific protocols. MR-unsafe implants are contraindicated. Pre-scan implant verification is mandatory — bring your implant card and have the model number available.
Patients with tattoos: most modern tattoos are safe for MRI. Some older or amateur tattoos contain iron-oxide pigments that can heat slightly. First-degree skin burns over heavily tattooed areas are reported occasionally but rarely serious. Inform the technologist about any large tattoos in the imaging area.
Patients with anxiety disorders: pre-scan anxiety can be substantial even without specific MRI fears. The combination of medical anxiety + claustrophobia in patients with general anxiety can make MRIs particularly difficult. Discussion with the ordering physician about mild sedation or other anxiety management approaches helps. Some patients benefit from a practice run (visiting the imaging center, seeing the scanner before scan day).
Patients with PTSD or trauma history: the loud sounds, enclosed space, and lying still during MRI can trigger trauma responses for some patients. Telling the technologist beforehand allows for additional support — pauses between sequences, more frequent check-ins via intercom, support person allowed in the room (sometimes). Mental health pre-treatment can also help for patients with severe trauma responses.

Managing MRI Side Effects
Before Scheduling
Pre-Scan Day
Day of Scan
During Scan
After Contrast (if used)
Returning Home
The MRI technologist monitors you throughout the scan via camera, microphone, and intercom. The call button (squeeze ball) lets you signal them anytime. If you feel anxious, uncomfortable, or experiencing any side effect, use the call button. The technologist can pause the scan, check on you, and potentially restart after you've recovered. Many patients try to "tough out" discomfort because they don't want to disrupt the scan or delay the diagnosis. This is the wrong instinct — communicating is what the technologist is trained for, and a brief pause is much better than aborting the scan entirely or having a worse experience.
Long-term considerations for repeat MRI patients. For patients with conditions requiring ongoing surveillance (multiple sclerosis, cancer follow-up, chronic vascular disease, hereditary tumor syndromes), the cumulative effect of multiple MRIs is a legitimate concern worth discussing with physicians.
For multiple sclerosis patients, brain MRI is the standard surveillance tool. Annual or more frequent scans are common. Most are non-contrast; some require contrast for new lesion identification. Discussion with your neurologist about when contrast is truly needed vs. when non-contrast follow-up suffices reduces cumulative exposure.
For cancer patients in remission, follow-up MRI may be required for years. Whether each scan needs contrast varies by cancer type and surveillance protocol. Many cancer follow-up protocols can use alternating contrast/non-contrast scans to reduce cumulative exposure without sacrificing surveillance quality.
For patients with chronic vascular disease (aneurysm monitoring, vascular abnormalities), some surveillance can shift between MRA (magnetic resonance angiography, sometimes non-contrast) and contrast-enhanced MRI. The specific approach depends on the condition and the imaging questions.
The cumulative gadolinium exposure conversation has emerged in the past decade as evidence about gadolinium retention has accumulated. There's no specific "too many" threshold established; the FDA has not set a maximum cumulative dose. The general principle: use contrast when it provides clear diagnostic benefit, avoid unnecessary repeat contrast for surveillance when alternatives can serve.
For most patients receiving 1-5 contrast MRIs over their lifetime, gadolinium retention is unlikely to cause any clinically significant effect. For patients facing 20-50+ contrast MRIs over decades of disease management, the conversation about cumulative exposure is more important and may influence imaging protocols. The decision is medical and individual to each patient's clinical situation.
MRI Pros and Cons
- +MRI has a publicly available content blueprint — you know exactly what to prepare for
- +Multiple preparation pathways accommodate different schedules and budgets
- +Clear score reporting shows specific strengths and weaknesses
- +Study communities share current insights from recent test-takers
- +Retake policies allow recovery from a difficult first attempt
- −Tested content scope requires substantial preparation time
- −No single resource covers everything optimally
- −Exam-day performance can differ from practice test performance
- −Registration, prep, and retake costs accumulate significantly
- −Content changes between versions can make older materials less reliable
MRI Questions and Answers
MRI is one of the safest imaging modalities available — no radiation, generally well-tolerated, with substantive side effects mostly limited to contrast administration in specific patient populations. The most common patient experiences (loud sounds, brief warmth, mild claustrophobia) are sensory rather than dangerous. The substantive concerns (contrast reactions, kidney implications, gadolinium retention) are well-studied and manageable with appropriate screening and protocols.
For most patients undergoing MRI, the practical recommendation is: don't avoid an MRI you need because of side effect concerns. The diagnostic benefit usually outweighs the risks substantially. For specific concerns (claustrophobia, prior contrast reactions, kidney disease), discuss with the ordering physician and imaging center beforehand to plan accommodations. The technology has matured significantly over decades of clinical use, and most side effect concerns have established management protocols. Trust the process and communicate any concerns proactively.
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.