Common MRI Findings: Brain, Spine and Joints Guide
Bone bruise MRI, brain white spots, bulging disc, empty sella, lipoma and more. What common MRI findings look like and what radiologists report.
You walked out of the imaging center with a thumb drive, a printed report, and a sinking feeling because half the words were Latin and the other half sounded ominous. Welcome to the strange world of MRI findings, where radiologists write in dense paragraphs that can describe a perfectly normal kidney or a serious tumor using almost identical vocabulary. The trick is learning which findings actually matter, which are incidental noise that millions of people share, and which need a follow-up appointment tomorrow morning.
Magnetic resonance imaging produces some of the most detailed pictures of the human body in modern medicine. A single brain scan can include twenty different sequences, each one tuned to highlight a different tissue property. T1 shows anatomy. T2 lights up water and edema. FLAIR nulls cerebrospinal fluid. Diffusion catches acute strokes within minutes. Every sequence the technologist runs adds another layer of information, and every layer is another chance for something unexpected to show up.
This guide walks through the most common findings radiologists report across brain, spine, joints, and soft tissue. We will cover what each finding looks like on a screen, what causes it, and what the next clinical step usually involves. Whether you are a patient trying to decode your report, a tech preparing for the registry exam, or a student rotating through radiology, the same framework applies: look at the location, look at the signal characteristics, look at the surrounding tissue, and ask whether the finding fits your symptoms.
MRI Findings by the Numbers
Before we walk through specific findings, it helps to understand how a radiology report is built. Every MRI report follows roughly the same skeleton: clinical history, technique, comparison studies, findings, and impression. The findings section is the long descriptive paragraph that lists everything the radiologist saw, whether or not it is clinically meaningful. The impression at the bottom is the short interpretive summary, where the radiologist tells your doctor which findings actually matter and what to do about them.
This structure matters because patients who read the findings section first often panic at language describing an incidental empty sella or a tiny T2 hyperintensity that the radiologist already classified as benign in the impression. Always read the impression first. If the impression says no acute pathology, the findings section is essentially a tour of normal variants and chronic changes that did not change the bottom line.
The other key piece of context is signal intensity. Radiologists use words like hyperintense, hypointense, and isointense to describe how bright or dark a structure looks compared to surrounding tissue on a specific sequence. A bone bruise MRI shows hyperintense signal on T2 and STIR sequences because the marrow is swollen with edema fluid. Empty sella shows cerebrospinal fluid filling the sellar space where pituitary tissue should sit.
Findings vs Impression
The findings section describes everything visible. The impression interprets what matters. Most patients should read the impression first because the findings section often lists benign incidentals that sound alarming in isolation. A radiologist who notes a small lipoma, an empty sella, or a tiny T2 hyperintensity is doing their job by documenting it - that does not mean any of those findings need action. Trust the impression and discuss any concerns with your ordering physician before searching individual terms online.
Brain MRI is where the most common worrying-sounding findings tend to appear. Brain MRI with white spots is probably the single most-Googled phrase after a head scan, and the answer is almost always reassuring. Small punctate T2 and FLAIR hyperintensities in the periventricular and deep white matter show up in roughly half of adults over fifty. They are most often chronic small vessel ischemic changes related to age, blood pressure, and vascular risk factors. They are not synonymous with multiple sclerosis, dementia, or stroke. The radiologist evaluates them based on number, location, shape, and whether they enhance with contrast.
Empty sella is another common incidental find. The sella turcica is a bony pocket at the base of the skull that houses the pituitary gland. In an MRI empty sella, cerebrospinal fluid fills part or all of that pocket because the pituitary has flattened or herniated. Most empty sellas are completely asymptomatic and require no treatment. A small subset are associated with hormonal disturbance and need endocrinology workup.
Other regular brain findings include arachnoid cysts, mucous retention cysts in the sinuses, brain mri cyst variants in the pineal region, choroid plexus cysts, and small venous angiomas. A cerebral hematoma MRI looks different depending on age - acute blood is T1 dark and T2 dark, subacute blood becomes T1 bright, and chronic hematomas leave hemosiderin staining that stays dark on T2 forever.
Common Findings by Body Region
White matter hyperintensities, empty sella, arachnoid cysts, brain metastases mri targets, microbleeds, mucous retention cysts, lacunar infarcts, and pineal cysts top the list. CJD mri shows cortical ribboning on DWI.
Disc bulges and protrusions at every level, facet arthropathy, Modic endplate changes, bulging disc in cervical spine mri causing cord deformity, cervical myelopathy mri features, Schmorl nodes, and hemangiomas in vertebral bodies.
Bone bruise mri marrow edema, meniscal tears, ligament sprains, rotator cuff tendinosis, labral tears, bone infection mri (osteomyelitis) marrow signal change, ganglion cysts, and Baker cysts behind the knee.
Hepatic and renal cysts, hemangiomas, mri lipoma in soft tissue, adnexal cysts, fibroids, endometriosis MRI deposits with characteristic T1 hyperintense foci, and incidental adrenal nodules.
Spine MRI is the workhorse study for back and neck pain, and it produces some of the most clinically actionable findings in radiology. A bulging disc mri image shows a disc that extends beyond the vertebral endplate by less than 90 degrees of its circumference. Protrusion means a focal extension less than 90 degrees, and extrusion means the disc material has broken through but stays connected to the parent disc.
Sequestration is when a fragment has fully separated. Each step up the severity ladder generally means more nerve root compression and more clinical symptoms, though plenty of patients have severe-looking imaging with mild symptoms and vice versa.
Cervical spine findings get extra attention because the spinal cord runs through the canal. A bulging disc in cervical spine mri can range from minimal indentation of the thecal sac to severe cord compression with myelomalacia. Cervical myelopathy mri features include high T2 signal within the cord at the level of compression, cord flattening, and sometimes secondary syrinx formation. Patients with these findings often need surgical consultation because chronic cord compression can produce permanent deficit even after decompression. The window between conservative care and surgery can be narrow when cord signal change appears.
Schmorl nodes are vertical herniations of disc material into the vertebral body endplate. They look dramatic but are usually asymptomatic and stable. Modic changes describe altered endplate signal that progresses through three stages - inflammatory, fatty, and sclerotic. Vertebral hemangiomas show characteristic polka-dot patterns on axial images and high T1 signal from internal fat. Tarlov cysts in the sacrum, dural ectasia in the thecal sac, and small synovial cysts at the facet joints round out the long list of benign incidentals that show up in nearly every lumbar spine report past age forty. None require treatment.
Findings by Tissue Type
Bone bruise mri appears as patchy hyperintense marrow signal on T2 and STIR with corresponding low T1 signal. The bruise often points to a recent impaction injury, microfracture, or ligament avulsion. Subchondral bone bruising under cartilage damage is common after ACL tears and meniscal injuries. Bone infection mri (osteomyelitis) shows similar marrow edema but adds enhancement after gadolinium, often with cortical disruption, periosteal reaction, and adjacent soft tissue inflammation. The two findings can look almost identical on basic sequences - contrast and clinical context separate them.
MRI lipoma is the textbook benign soft tissue mass. It follows fat signal on every sequence - bright on T1, bright on T2, and drops out completely on fat-saturated images. There is no enhancement after contrast because pure fat has no vascularity. Lipomas can grow anywhere fat exists, which means almost anywhere in the body. They are usually painless, soft, and mobile under the skin. Atypical lipomatous tumors and well-differentiated liposarcomas can look similar but show thick septations, nodular enhancement, or non-fatty components that prompt biopsy.
Endometriosis is one of the most clinically important pelvic MRI findings in women of reproductive age. Can endometriosis be diagnosed by mri? Often yes - deep infiltrating endometriosis shows characteristic T1 hyperintense, T2 hypointense lesions, especially when chocolate cysts contain blood products in different stages. Can endometriosis show on mri even when the implants are tiny? Sometimes, but small superficial peritoneal disease still escapes detection and requires laparoscopy. MRI is most useful for mapping deep disease before surgery, identifying ovarian endometriomas, and following known disease over time.
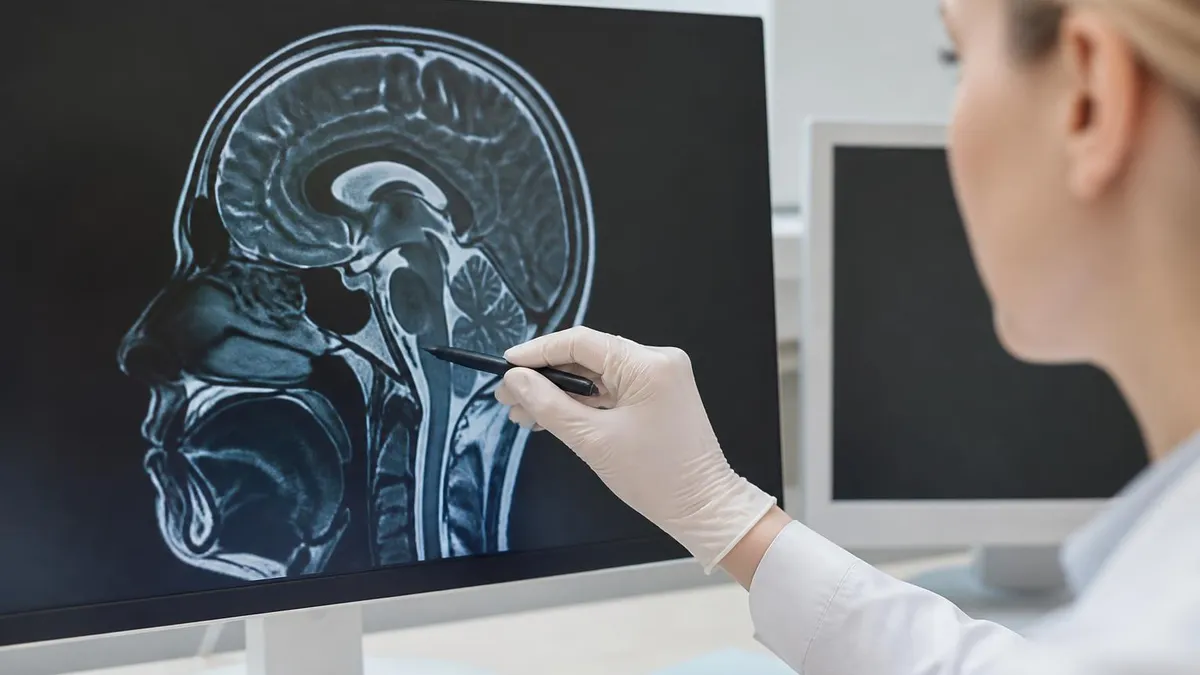
Can an mri detect dementia? MRI does not diagnose dementia directly because dementia is a clinical syndrome, not an imaging finding. However, MRI can identify patterns strongly associated with specific dementia subtypes - hippocampal and medial temporal lobe atrophy in Alzheimer disease, frontal and temporal atrophy in frontotemporal dementia, midbrain atrophy in progressive supranuclear palsy, and basal ganglia changes in vascular dementia. Combined with neuropsychiatric testing and sometimes amyloid PET, MRI guides differential diagnosis and helps exclude treatable mimics like normal pressure hydrocephalus or chronic subdural hematomas.
Acute stroke on diffusion-weighted imaging, ring-enhancing brain lesion with edema (possible metastasis, abscess, or high-grade tumor), cord compression with new myelopathy signal, epidural hematoma or abscess, intracranial hemorrhage, large pulmonary embolism on chest MRI, and active inflammation in pyogenic spondylodiscitis all require urgent specialist contact. If your radiologist's impression uses words like critical, urgent, or emergent, the ordering physician has already been called. If you receive results without that contact and the impression sounds alarming, do not wait - call the office immediately.
What happens after your MRI report lands in the inbox depends on three things: what was found, what your symptoms are, and your overall medical context. A small white matter hyperintensity in a 25-year-old with new vision loss reads completely differently than the same finding in a 75-year-old with poorly controlled hypertension.
The radiologist generates the report without knowing every detail of your history, which is why your ordering physician is the one who synthesizes the result into a plan. Bring a list of your current symptoms to the follow-up appointment so your doctor can match each one to a specific imaging finding rather than guessing which complaints correlate.
For brain mri cyst findings that look benign, the typical workup is no further imaging or a follow-up scan in 6 to 12 months to confirm stability. For bone bruise mri findings after trauma, protected weight-bearing and a recheck at 6 weeks is standard. For bulging disc mri image findings causing radiculopathy, conservative therapy with physical therapy, anti-inflammatories, and sometimes injections precedes any discussion of surgery.
For cervical myelopathy mri findings with cord signal change, surgical consultation usually happens within days. For brain metastases mri findings, oncology and radiation oncology referrals happen immediately because treatment windows matter and untreated CNS disease can progress quickly.
Repeat imaging is more common than patients expect. Many findings need a follow-up MRI in 3, 6, or 12 months to establish stability. Growth means biopsy or treatment. Stability over a year or two usually means benign and the radiologist may recommend stopping surveillance. Keep your prior CDs - they are essential for accurate comparison.
Questions to Ask After Your MRI Results
- ✓What does the impression actually mean in plain English?
- ✓Which findings explain my symptoms and which are incidental?
- ✓Do any findings require follow-up imaging, and if so when?
- ✓Should I see a specialist, and how urgently?
- ✓Are there treatment options or lifestyle changes that affect this finding?
- ✓Could the finding be a normal variant for someone my age?
- ✓If something looks worrying, what would the next test be to clarify?
Patients fall into a few predictable traps when reading MRI reports. The first is treating every adjective as a diagnosis. Words like prominent, mild, minimal, and small are descriptive, not diagnostic. A mild disc bulge is incredibly common and usually meaningless. Prominent ventricles in an 80-year-old reflect age-appropriate atrophy, not hydrocephalus. The radiologist uses qualifiers because precision matters - they are not hedging.
The second trap is comparing your findings to a friend's. Two patients with identical disc protrusions can have completely different symptoms. Anatomy does not perfectly predict pain. The body has remarkable capacity to accommodate structural change without producing problems, which is why imaging without symptoms is often misleading. Many incidental findings, including small mri lipoma deposits, brain mri cyst variants, and degenerative spine changes, never cause trouble in a lifetime.
The third trap is searching individual phrases online. The internet contains every possible diagnosis attached to every possible finding. A T2 hyperintense lesion can mean a benign cyst, a stroke, a tumor, an infection, or a normal variant depending on location, shape, signal characteristics, and clinical context. Your radiologist already considered all of those possibilities when writing the impression. The plain-English explanation should come from your ordering physician, who knows your story and can put the imaging in context.
MRI vs CT for Common Conditions
- +MRI superior for brain, spine, and soft tissue detail
- +No ionizing radiation, safe for repeated imaging
- +Better characterization of marrow signal and bone bruise mri
- +Can detect early ischemic stroke within minutes on DWI
- +Detects ligament, tendon, and cartilage injury CT cannot see
- +Multi-planar imaging without repositioning the patient
- −CT faster and more available for trauma and acute hemorrhage
- −CT better for acute lung pathology and pulmonary embolism
- −CT superior for cortical bone detail and acute fractures
- −MRI contraindicated with many older implants and pacemakers
- −Claustrophobia and motion can ruin MRI image quality
- −MRI costs more and scheduling delays are longer
If you are studying for the ARRT MRI registry, common findings are a major test category. The exam expects you to recognize classic signal patterns, name the sequence that best demonstrates a finding, and understand basic pathophysiology behind each appearance. A bone bruise mri question will reward you for knowing STIR and fat-saturated T2 as the most sensitive sequences.
A bulging disc mri image question will test your ability to differentiate bulge from protrusion from extrusion. A brain mri with white spots question will expect you to think about location and clinical context before jumping to multiple sclerosis. A cjd mri question will look for cortical ribboning on DWI as the highly specific finding.
Test preparation works best when you pair conceptual reading with thousands of practice questions. Memorizing the answer to one specific question rarely transfers, but seeing the same finding asked twenty different ways trains your eye and your reasoning. The same applies for clinical practice - radiology residents spend years building pattern recognition by reading thousands of cases.
The shortcut, if there is one, is repetition with feedback. Practice tests with detailed explanations help fix the why behind each answer, which is what separates technologists who pass the registry on the first try from those who repeat the exam two or three times before clearing the cutoff.
Beyond the registry exam, building a personal finding catalog is one of the most useful career habits a tech can develop. Every time you scan a patient and the radiologist calls something specific, look at the images yourself afterward. Match what you saw at the console to what got reported.
Over months and years, your eye starts to flag protocol changes the radiologist will appreciate - an extra coronal STIR when you suspect bone bruise, a contrast study when an osteomyelitis question arises, a thinner slice through the pituitary when the screening sequences hint at empty sella. The best techs are the ones who think one step ahead of the report.
MRI findings live on a spectrum from completely meaningless incidentals to urgent must-treat-today emergencies. The radiologist's job is to flag what matters, describe what does not, and pass the synthesis to your ordering physician. Your job as a patient is to read the impression first, write down questions, and have a conversation with your doctor before drawing conclusions from individual words.
Your job as a technologist is to capture the right sequences with diagnostic quality so the radiologist can do their reading correctly. Your job as a student is to learn the patterns and the language that connect imaging appearance to underlying biology.
Whether the finding is a bone bruise mri after a weekend skiing accident, an empty sella discovered during a headache workup, a brain mri cyst found incidentally, or a more concerning lesion that needs follow-up, the same framework applies. Look at location. Look at signal. Look at the surrounding tissue.
Read the impression. Talk to your doctor. Get your priors if you have any. Schedule the follow-up if one is recommended. MRI is a powerful tool, but it is only useful when its findings are interpreted in the full context of who you are and what symptoms brought you to the scanner in the first place.
One last practical note: keep your reports and image discs together in one folder, paper or digital, for life. You will move, change doctors, and switch insurance plans several times before that next scan, and the priors are gold for whichever radiologist reads your future imaging. A finding that looked alarming in isolation often becomes clearly benign when compared with a five-year-old study showing the same thing. Your future self will thank you.
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.