Pictures of MRI of the Brain: What Every Sequence Shows and How to Read Them
Pictures of MRI of the brain decoded by sequence and plane. T1, T2, FLAIR, DWI, SWI and contrast explained for techs, students and patients.
If you have ever sat in a radiologist's reading room or scrolled through a hospital portal trying to make sense of your own scan, brain MRI pictures can feel like a puzzle. Slices of grey and white, dark dots that look ominous, bright crescents along the skull. Most patients see them once and never again. Technologists see them all day. The gap between those two experiences is exactly what this guide tries to close.
Pictures of MRI of the brain are not random snapshots. Every image you see has a job. One sequence is hunting for blood. Another is looking for water. A third tries to catch a tumor before it bleeds. Read in the right order, the pictures tell a story about the brain at a single moment in time. Read in the wrong order, they look like noise. So before any image gets opened, the protocol decides what story we are trying to tell.
This guide walks through what you will actually see on brain MRI pictures, why each sequence looks the way it does, and how a technologist or radiologist scans the images for findings. We will also cover the strange-looking artifacts, the bright spots that mean nothing, and the dark patches that mean a lot. By the end you will be able to look at a stack of brain MRI images and at least know which one is which, and that alone is half the job.
Brain MRI Pictures by the Numbers
Each MRI sequence highlights different tissue properties. T1 shows anatomy, T2 shows water and edema, FLAIR isolates lesions near fluid, DWI catches acute stroke, SWI finds blood, and post-contrast T1 reveals tumors and infections. Reading them together tells the full clinical story.
What Brain MRI Pictures Actually Show
A single brain MRI study is rarely a single picture. It is usually a stack — twenty, thirty, sometimes more than a hundred slices for each pulse sequence. Each sequence highlights a different tissue property. T1-weighted images make fat and fluid behave one way; T2 sends them the other way. Toss in diffusion, FLAIR, susceptibility, and post-contrast runs, and you have a small library of pictures from the same head taken minutes apart.
On any picture, you should be able to find four landmarks fast. The skull as a dark or bright outer rim depending on sequence. The cerebrospinal fluid, sitting in the ventricles in the center. The grey matter draped along the surface and around the basal ganglia. White matter pushed into the middle. Once you can pick those four out, every other finding gets easier because you have a reference frame.
Brain MRI pictures are taken in three planes. Axial cuts go through the head horizontally, like slicing a loaf of bread sideways. Sagittal cuts run from ear to ear, splitting the head into left and right. Coronal cuts run from the back of the head to the face. Each plane shows the same lesion from a different angle. A radiologist almost never trusts a finding seen on just one plane.
Why T1 and T2 Pictures Look So Different
The first thing that confuses new viewers is why two pictures of the same brain, taken in the same scanner, look so opposite. On a T1, cerebrospinal fluid in the ventricles is dark. On a T2, it is bright. The reason is timing. The scanner is sampling the same tissues at different points in their magnetic relaxation. Fluid takes a long time to give back its signal, fat gives it back fast. By picking when to listen, the scanner decides what is bright.
T1-weighted brain MRI pictures are the anatomy workhorse. Fat is bright, water is dark, brain looks roughly like brain. They make it easy to see structure. T2-weighted pictures flip the script. Water is bright, fat is dim, edema lights up. A stroke that is hours old, a tumor with surrounding swelling, a demyelinating plaque — all of these tend to be loud on T2, quiet on T1. Both pictures are necessary. Neither tells the whole story by itself.
FLAIR is a clever variation. It is T2-weighted, but the bright cerebrospinal fluid signal is suppressed. That sounds small. It is not. Without FLAIR, lesions sitting right next to the ventricles get drowned out by the bright fluid. With FLAIR, those same lesions stand out like headlights. For multiple sclerosis plaques and small vessel disease, FLAIR is often the first picture a radiologist opens. If you want to understand brain MRI with contrast, you also need to understand how FLAIR and T1 post-contrast work together, because they answer different questions.
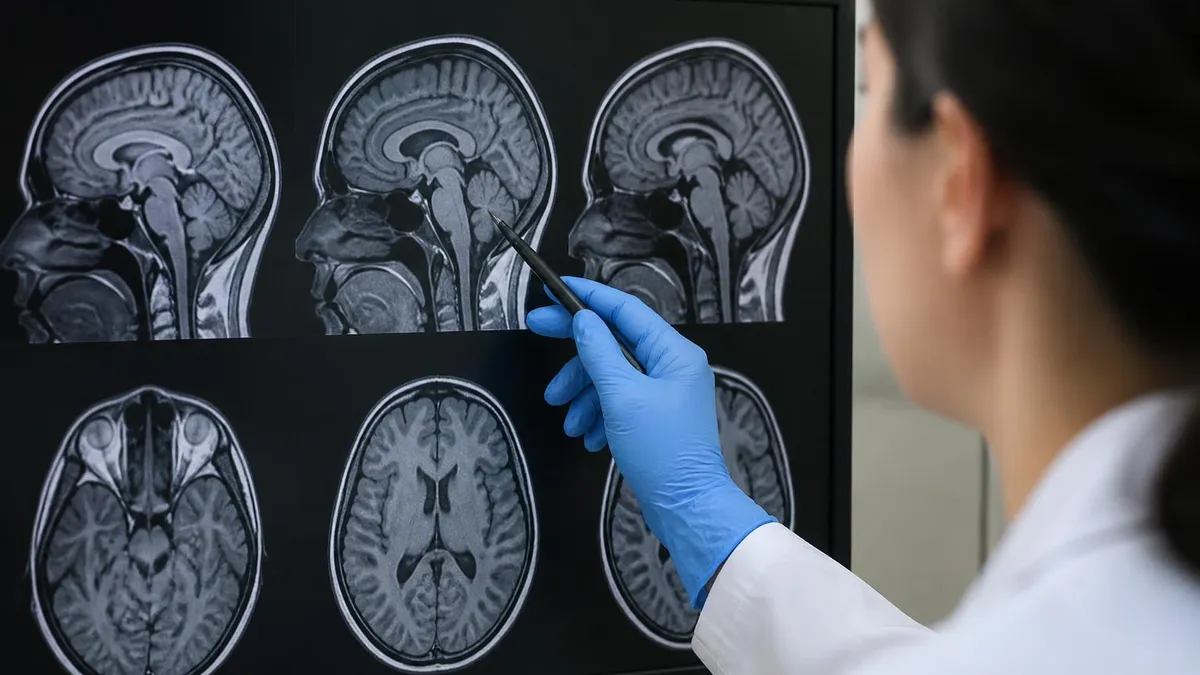
The Six Core Brain MRI Sequences
Anatomy workhorse. Fat is bright, fluid is dark. Used for structural detail and as the baseline before contrast injection.
Water is bright, fat is dim. Edema, inflammation, and many lesions stand out clearly on T2 imaging.
T2 with bright cerebrospinal fluid suppressed. Lesions near the ventricles pop out. Key for MS and small vessel disease.
Catches acute stroke within minutes. Bright on DWI plus dark on ADC equals restricted diffusion, the stroke signature.
Sensitive to blood products and calcium. Finds microbleeds, hemorrhage, and old blood that other sequences miss.
After gadolinium injection. Anything that lights up has a leaky blood-brain barrier — tumor, infection, active inflammation.
Reading Pictures of MRI of the Brain Like a Technologist
Technologists do not diagnose. We screen, we position, we capture, we hand off. But we look at every picture as it comes off the scanner, because a bad picture means a wasted scan and a frustrated patient. The first thing a technologist checks is coverage — does the image actually contain everything from the top of the skull to the foramen magnum, or did we cut off the brainstem? Then signal — is there enough? Then artifact — is motion ruining the study?
From there the eye moves to the obvious. Symmetry first. The brain is roughly symmetric, and asymmetry is suspicious until proven otherwise. A swollen lobe on one side, a missing sulcus, a midline shift, a ventricle squeezed flat — these are findings even a non-radiologist should spot. After symmetry, density. Bright where it should not be bright. Dark where it should be grey. Edges where edges should not exist.
Most pictures of MRI of the brain that a tech reviews live or die on diffusion. Diffusion-weighted imaging catches acute stroke earlier than any other sequence, sometimes within minutes. A bright spot on diffusion that is dark on its matching ADC map is a stroke until proven otherwise. Techs learn this not because they call the diagnosis, but because they may need to alert the radiologist before the patient leaves the table.
Common Findings You Will See on Brain MRI Pictures
Some findings appear on so many brain MRI pictures they barely make the report. Small white matter hyperintensities in older adults — tiny bright dots scattered through the deep white matter on FLAIR — are usually chronic small vessel ischemic changes. They are not strokes in progress. They are the slow accumulation of vascular wear over years. Most people over 60 have some.
Volume loss, often called atrophy, looks like wider sulci and bigger ventricles. It is normal with aging, exaggerated in dementia. A radiologist comments on it when it is out of proportion to age. Mucosal thickening in the sinuses is so common it almost does not warrant mention, except that techs sometimes catch a frank fluid level that needs attention. Pineal and choroid plexus cysts are bright on T2, do nothing, and freak patients out unnecessarily.
The serious findings are what training is built around. Mass effect — when something is pushing brain out of the way. Restricted diffusion — stroke, abscess, certain tumors. Enhancement after gadolinium — tumor, infection, or active inflammation. Hemorrhage — which looks dramatically different depending on its age, evolving from bright to dark and back again as blood breaks down. Each of these has a typical pattern, and patterns are what radiologists are trained to recognize.
Three Imaging Planes
Horizontal slices through the head, like cutting a loaf of bread sideways. The most common viewing plane. Best for ventricle shape, symmetry, and surveying the whole brain quickly.
How Contrast Changes the Pictures
Gadolinium contrast is given through an IV and it does one main thing — it lights up anything with a leaky blood-brain barrier. Healthy brain has a tight barrier. Contrast does not cross. Tumors, infections, active demyelinating lesions, and abnormal vessels all break that barrier in different ways. After contrast, those areas become bright on T1.
The protocol almost always includes a pre-contrast T1 and a post-contrast T1. You compare the two pictures side by side. Anything new and bright on the post-contrast image is enhancing. A solid enhancing mass is the classic picture of certain brain tumors. A ring of enhancement around a dark center can mean abscess, necrotic tumor, or a few other things. Patchy enhancement scattered through white matter can be active multiple sclerosis.
Contrast is not used for every brain MRI. Routine screening, headache workups in low-risk patients, and many follow-ups skip it. Anytime there is a real concern for tumor, infection, or active inflammation, contrast goes in. Patients with poor kidney function need careful screening before any gadolinium dose, and that screening is part of the technologist's job.
Strange Looking Things That Are Not Findings
Plenty of bright or dark spots on brain MRI pictures are not real. They are artifacts. Motion artifact creates ghosting — a faint repeated image smeared across the picture. It happens when a patient moves during acquisition, which on long sequences can be even brief shifting. Susceptibility artifact creates dark blooming around metal, dental work, surgical clips, even some makeup. Wraparound artifact folds the back of the head onto the front when the field of view is too small.
Pulsation artifact from the basilar artery and the CSF can mimic findings. Chemical shift artifact at fat-water interfaces puts bright and dark bands where there should be a smooth edge. Gibbs ringing — fine parallel lines near sharp tissue boundaries — is a Fourier transform artifact, not a lesion. Techs are taught to recognize each of these because telling a radiologist about a "lesion" that turns out to be a coil artifact wastes time.
The other thing that looks strange but is normal — variation. Brains are not identical. Asymmetric ventricles in a healthy person. A prominent perivascular space that looks like a dot of fluid. A normal variant of vascular anatomy. Reading hundreds of brain MRI pictures teaches you what normal looks like, and once you have that baseline, the abnormal jumps out.
What Technologists Check on Every Brain MRI
- ✓Coverage from the top of the skull to the foramen magnum
- ✓Adequate signal-to-noise without overwhelming artifact
- ✓Symmetry between left and right hemispheres
- ✓Ventricle size and midline alignment
- ✓Diffusion-weighted images for any acute stroke signal
- ✓Sequence labeling and protocol completeness
- ✓Patient motion or breathing artifacts before patient leaves
- ✓Susceptibility blooming around dental work or implants
The Sequences a Standard Brain MRI Includes
A routine brain MRI usually has a handful of core sequences. Sagittal T1, axial T2, axial FLAIR, axial diffusion-weighted imaging with its ADC map, axial susceptibility weighted imaging or gradient echo for blood, and then a post-contrast T1 set in multiple planes if contrast is given. That gives you anatomy, edema-sensitive imaging, lesion detection, stroke detection, blood detection, and an enhancement check.
Specialty protocols add more. A seizure protocol adds high-resolution coronal sequences through the temporal lobes. A pituitary protocol adds thin slices through the sella. A stroke protocol may add perfusion imaging and MRA — magnetic resonance angiography — to look at the vessels themselves. The protocol is chosen based on the clinical question. There is no one-size-fits-all set of pictures.
Scan time varies. A basic brain MRI without contrast can finish in 20 to 30 minutes. With contrast and specialty sequences, you might be on the table for 45 minutes or longer. The pictures keep coming the whole time. For details on what to expect during your own scan, the brain MRI take guide breaks the timing down sequence by sequence.
What Patients See vs What Radiologists See
When a patient gets a copy of their pictures on a CD or a portal link, they usually see a viewer that lets them scroll through axial T1 or T2 only. That is a small fraction of the actual study. The radiologist who read the scan saw every sequence in every plane, on a high-resolution monitor calibrated for greyscale. They scrolled fast, paused on findings, compared to prior studies, measured, and dictated a report.
So when a patient looks at their own brain MRI pictures and panics, they are usually looking at the wrong picture or the wrong slice. The bright crescent along the skull is not a tumor — it is subcutaneous fat. The dark spots in the temples are normal. The bright dot deep in the white matter might be nothing, might be everything. Without the full study, you cannot tell. This is why we say read the report, not the pictures.
None of this means patients should not look. Curiosity is healthy. Asking the radiologist or the ordering physician to walk you through the findings is reasonable. Just do not diagnose yourself from one axial slice on a phone screen. The pictures are powerful, but they need context.
Patient-facing viewers usually show one or two sequences in one plane. Radiologists read the full study on calibrated monitors with priors for comparison. A bright spot on your phone screen might be normal fat, a known variant, or an artifact. Read the report, not the pictures.
How Pictures of MRI of the Brain Fit Into Diagnosis
An MRI picture is one piece of a diagnostic puzzle that includes history, physical exam, labs, and sometimes other imaging. A finding on a brain MRI is interpreted in context. A bright lesion in a 25-year-old with optic neuritis means one thing. The same lesion in a 75-year-old with hypertension means something else. Pictures alone almost never settle a diagnosis. They guide it.
Follow-up MRIs are how we watch things evolve. A small finding that does not change over a year is very different from one that grows in three months. Comparison studies are essential. A radiologist always asks for priors when they exist, because the trend matters more than the snapshot. This is why you should keep copies of your own imaging — not for self-diagnosis, but for the next radiologist who will compare against them.
Brain MRI is also used to rule things out. A patient with a new headache and a normal MRI has a different anxiety than one with an abnormal one. The negative finding has clinical weight too. The picture that shows nothing wrong is still useful, because it changes what we look for next.
What Technologists Need to Know About the Pictures
For technologists studying for certification, recognizing brain MRI pictures by sequence and plane is non-negotiable. You need to see a slice and know within a second whether you are looking at T1, T2, FLAIR, DWI, ADC, SWI, or post-contrast T1. The exam will test it. The job will test it constantly. Techs who can read a sequence at a glance run better scans because they catch protocol mistakes before the patient leaves.
Recognizing artifacts is the next layer. A motion-corrupted DWI looks similar to ischemia if you do not know what motion artifact looks like. A susceptibility artifact from dental hardware looks like a hemorrhage if you have never seen it before. Building that visual library takes hundreds of scans. There is no shortcut. The MRI registry exam covers this in the safety and image quality sections.
Finally, knowing when to call. A tech who sees obvious findings — large mass, midline shift, fresh blood, restricted diffusion across a vascular territory — should know to flag the radiologist immediately rather than letting the patient walk out. The radiologist makes the call. The tech makes sure the radiologist gets the chance. That is a real skill, and it is built by looking at pictures every day until they start to make sense.
Final Thoughts on Reading Brain MRI Pictures
Pictures of MRI of the brain are not mysterious once you know what each sequence is doing. T1 for structure, T2 and FLAIR for edema, DWI for stroke, SWI for blood, post-contrast for enhancement. Six tools, each answering a specific question. Stacked together, they give a radiologist enough information to read a brain in detail no other modality matches.
For patients, the takeaway is that any single image is one piece of a much bigger study. For technologists, the takeaway is that recognizing the sequences and the artifacts is half of what makes a good scan a good scan. For students and certification candidates, the takeaway is that pattern recognition only comes from looking at hundreds of pictures with someone who can tell you what you are seeing. The pictures are not the diagnosis. They are the evidence the diagnosis is built from.
Findings That Appear on Almost Every Brain MRI
- ✓Small white matter hyperintensities on FLAIR in adults over 50
- ✓Mild volume loss proportional to patient age
- ✓Mucosal thickening in the paranasal sinuses
- ✓Asymmetric ventricle size as a normal variant
- ✓Pineal or choroid plexus cysts that mean nothing clinically
- ✓Prominent perivascular spaces near the basal ganglia
- ✓Mild motion or pulsation artifact on long sequences
- ✓Susceptibility blooming around dental hardware or implants
Brain MRI vs Brain CT for Most Findings
- +Far better soft tissue contrast than CT
- +No ionizing radiation, safer for young or repeat scans
- +Detects acute stroke hours before CT can
- +Sees demyelinating plaques and small tumors CT misses
- +Multiple sequences answer different clinical questions
- −Longer scan time, harder for claustrophobic patients
- −More expensive than CT in most healthcare systems
- −Cannot be used with many implanted devices without screening
- −Less sensitive than CT for acute skull fracture and bone detail
- −Pictures are harder for non-specialists to interpret
What Happens During a Brain MRI Scan
Screening and Safety Check
Positioning on the Table
Localizer Scan
Sequence Stack Acquisition
Contrast Injection if Ordered
Image Review and Patient Release
MRI Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.