Adson Test: Complete Guide to Thoracic Outlet Syndrome Assessment
Complete guide to the Adson test covering procedure, positive findings, clinical applications, and interpretation for thoracic outlet syndrome evaluation.

The Adson test is a clinical assessment used to evaluate patients for thoracic outlet syndrome involving compression of nerves or blood vessels passing through the thoracic outlet area between the neck and shoulder. Named after Dr. Alfred Washington Adson who developed the test in 1927, the Adson maneuver helps clinicians identify vascular compression that may produce symptoms in the arm and hand. Healthcare providers including physicians, physical therapists, chiropractors, and other practitioners use the Adson test as part of comprehensive thoracic outlet evaluation.
Thoracic outlet syndrome encompasses several distinct conditions involving compression of the brachial plexus nerves, subclavian artery, or subclavian vein in the area between the collarbone and first rib. The syndrome can produce various symptoms including arm pain, hand numbness or tingling, weakness, color changes in the hand, and various other manifestations depending on which structures experience compression. Diagnosis remains challenging requiring combination of clinical history, physical examination findings, and sometimes imaging studies confirming compression presence.
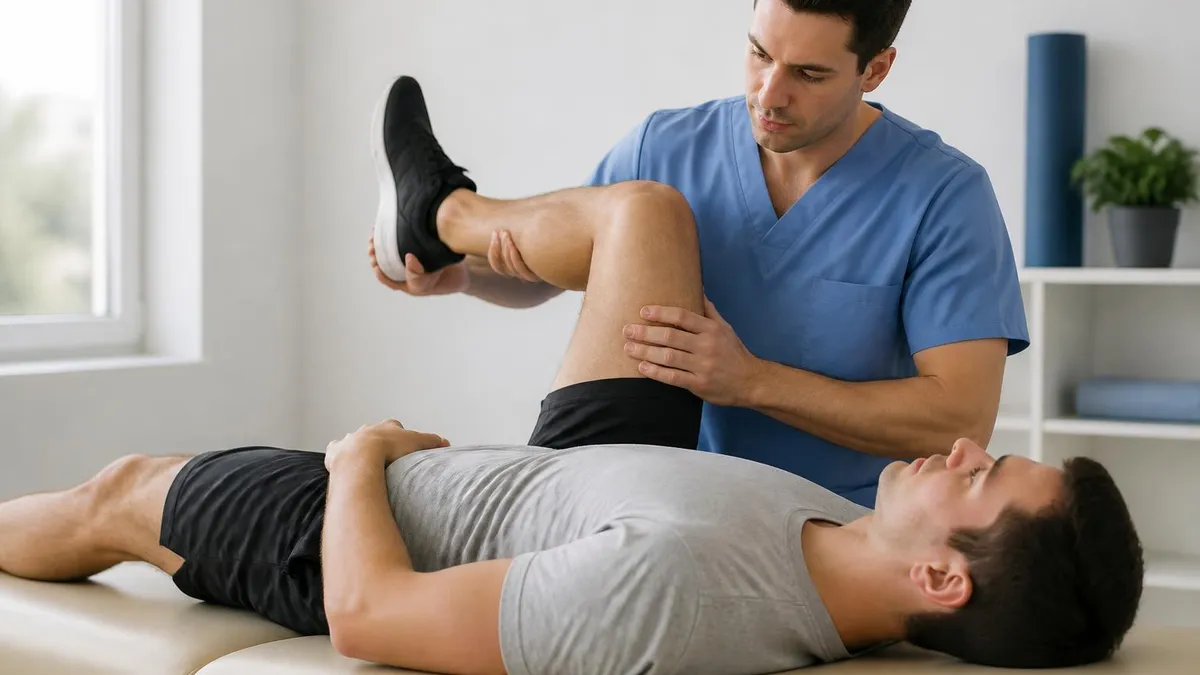
The Adson test specifically assesses vascular compression by detecting changes in radial pulse during specific patient positioning. The test involves having the patient extend the affected arm while turning the head and taking a deep breath. The clinician palpates the radial pulse at the wrist throughout the maneuver watching for pulse diminution or disappearance indicating possible vascular compression. The Adson test joins several other thoracic outlet provocative maneuvers in comprehensive evaluation rather than serving as standalone diagnostic tool.
Anatomy of the thoracic outlet helps explain why compression occurs in this specific body region. The thoracic outlet spans between the clavicle anteriorly and the first rib inferiorly with three potential compression sites. The interscalene triangle bounded by anterior and middle scalene muscles and the first rib produces the most common compression site. The costoclavicular space between clavicle and first rib represents the second compression site. The retropectoralis minor space behind the pectoralis minor muscle constitutes the third potential compression site producing different symptom patterns.
Telehealth applications of thoracic outlet evaluation have expanded with remote care growth. Some aspects of patient history and symptom assessment can occur through video visits. However, the physical examination including Adson testing requires in-person evaluation for proper pulse palpation. Hybrid approaches combining telehealth for initial assessment with in-person physical examination support efficient evaluation when distance or scheduling makes pure in-person evaluation difficult for patients seeking thoracic outlet assessment.
The Adson test assesses for thoracic outlet syndrome by detecting radial pulse changes during specific arm and neck positioning. The test was developed by Dr. Alfred Adson in 1927. Positive findings include pulse diminution or disappearance during the maneuver suggesting possible vascular compression at the thoracic outlet. The test is one component of comprehensive thoracic outlet syndrome evaluation.
Comprehensive evaluation combining clinical history, multiple provocative tests, and selective imaging or electrodiagnostic studies produces more reliable thoracic outlet syndrome diagnosis than any single examination component alone provides.
Procedure for the Adson test follows specific steps supporting reliable assessment. The patient sits or stands with the affected arm relaxed at the side. The clinician palpates the radial pulse at the wrist establishing baseline pulse quality. The patient extends the arm slightly with the shoulder externally rotated. The patient turns the head toward the affected side or away depending on the specific Adson variation being performed. The patient takes a deep breath and holds it. The clinician palpates the radial pulse throughout the maneuver watching for changes from baseline pulse quality.
Positive findings in the Adson test include diminution or complete disappearance of the radial pulse during the maneuver. The pulse change suggests possible compression of the subclavian artery as it passes through the thoracic outlet. Some patients may also experience reproduction of their symptoms during the test including arm pain, numbness, or tingling supporting clinical correlation with the pulse findings. Negative findings show preserved radial pulse throughout the maneuver suggesting absence of significant vascular compression in the tested position.
Risk factors for thoracic outlet syndrome include both anatomical and acquired factors. Cervical ribs representing supernumerary ribs above the first rib predispose to compression. Anomalous fibrous bands connecting cervical vertebrae to first rib produce similar predisposition. Repetitive overhead activities in athletes including swimmers, baseball pitchers, and volleyball players can produce muscle hypertrophy compressing thoracic outlet structures. Heavy backpack carrying, poor posture, and obesity contribute to thoracic outlet syndrome development in some patients.
Patient advocacy organizations provide resources supporting patients with thoracic outlet syndrome. Several patient organizations focus on rare disease awareness including thoracic outlet syndrome. Support groups connect patients sharing similar experiences. Educational resources help patients understand their condition and treatment options. Patient advocacy efforts have raised awareness of thoracic outlet syndrome supporting better diagnosis and treatment access for affected patients beyond just individual clinical care.
Thoracic Outlet Syndrome Types
Most common form involving compression of brachial plexus nerves. Produces arm pain, numbness, tingling, and weakness. Diagnosis often challenging requiring careful clinical evaluation. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Less common form involving compression of the subclavian vein. Can produce arm swelling, blue discoloration, and superficial vein prominence. Acute presentations may indicate effort thrombosis. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Rare form involving compression of the subclavian artery. Most serious form with potential for arterial damage and embolization. Adson test specifically targets this form. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Confirmed cases with objective neurological abnormalities including muscle wasting. Less common than disputed neurogenic forms but represents clear diagnostic category. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Most cases of neurogenic TOS without objective neurological deficits. Diagnosis based on clinical presentation rather than objective findings producing diagnostic challenges. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Sensitivity and specificity of the Adson test affect its diagnostic utility. Studies have produced varying estimates with sensitivity ranging from 30 to 80 percent and specificity ranging from 70 to 90 percent depending on study methods and patient populations. The relatively modest sensitivity means negative tests do not rule out thoracic outlet syndrome while the moderate specificity means positive tests support but do not confirm diagnosis. Combined with other provocative maneuvers and clinical findings, the Adson test contributes to overall diagnostic picture rather than serving as definitive test.
False positive results occur in some healthy individuals without thoracic outlet syndrome. Studies have shown that 50 percent or more of asymptomatic individuals may show pulse diminution during Adson testing. The high false positive rate limits the test diagnostic utility when used alone and emphasizes the importance of correlating findings with patient symptoms and other examination findings. The positional vascular compression that produces pulse changes in healthy individuals may not produce clinical symptoms requiring symptom correlation for clinical significance determination.
Demographics for thoracic outlet syndrome show specific patterns. Women experience the syndrome 3 to 4 times more frequently than men reflecting both anatomical and hormonal factors. Most patients present between ages 20 and 50 though presentations occur across the age range. Athletes in specific sports show higher rates than general population. Workers in certain occupations including assembly line workers, hair stylists, and others performing repetitive overhead work show higher rates than office-based workers without these specific physical demands.
Research developments continue advancing thoracic outlet syndrome understanding and treatment. Improved imaging techniques including dynamic MRI angiography support better diagnosis. Refined surgical approaches improve outcomes while reducing complications. Better understanding of predisposing factors supports targeted prevention strategies. Continued research will likely produce additional advances over coming years improving care for patients with this complex condition affecting quality of life substantially when present.
Adson Test Variations
The classic Adson test has the patient turn the head toward the affected side while extending and externally rotating the arm. The patient takes a deep breath and holds it. The clinician palpates the radial pulse looking for diminution or disappearance. The classic variation targets compression at the interscalene triangle where the brachial plexus and subclavian artery pass between the scalene muscles.
Each variation may identify different aspects of thoracic outlet compression supporting comprehensive evaluation across multiple positions and configurations.
Clinical context determines how to interpret Adson test findings appropriately. Positive Adson tests in patients with consistent thoracic outlet symptoms support the diagnosis when combined with other clinical findings. Positive tests in asymptomatic patients have less clinical significance though may identify patients at risk for developing symptoms. Negative tests in symptomatic patients do not rule out thoracic outlet syndrome given the test moderate sensitivity. Negative tests in asymptomatic patients have limited clinical implications. Integration with full clinical evaluation supports proper interpretation beyond just the test result itself.
Other provocative maneuvers complement Adson testing in comprehensive thoracic outlet evaluation. The Roos test involves holding both arms in surrender position while opening and closing the hands for 3 minutes. The Wright test extends and abducts the arm watching for pulse changes. The Costoclavicular maneuver brings the shoulders back and down compressing the area between the clavicle and first rib. The military brace position similarly tests costoclavicular space. Using multiple provocative tests produces more comprehensive evaluation than any single test alone provides.
Symptom patterns help distinguish thoracic outlet syndrome from other arm pain causes. Neurogenic patients typically describe arm pain, hand numbness or tingling particularly in the ulnar distribution, and weakness with extended overhead activity. Symptoms often worsen with arm elevation. Venous patients experience arm swelling, blue color, and superficial vein prominence. Arterial patients may have hand pain with activity, color changes, and digital ischemia in severe cases. The symptom patterns guide which specific tests to perform during evaluation.
Disability considerations affect some patients with severe thoracic outlet syndrome. Symptoms can substantially limit work capacity in jobs requiring overhead activity, repetitive motion, or sustained arm use. Disability benefits may be available for patients with severe documented thoracic outlet syndrome affecting work capacity. Documentation of symptoms, examination findings, and functional limitations supports disability claims when symptoms produce substantial work impairment exceeding minor inconvenience.

The Adson test alone cannot diagnose thoracic outlet syndrome. The moderate sensitivity and significant false positive rate require combining the test with clinical history, symptom assessment, other provocative maneuvers, and sometimes imaging studies. Clinical correlation determines whether positive Adson findings represent clinically significant compression versus normal anatomical variation without symptomatic impact.
Referral to vascular surgeons or specialized thoracic outlet centers may be appropriate for complex cases not responding to conservative management or showing significant vascular or neurological compromise requiring intervention.
Imaging studies sometimes complement physical examination findings in thoracic outlet syndrome evaluation. Plain radiographs may identify cervical ribs or anatomical variations that predispose to thoracic outlet syndrome. Chest CT scans with vascular contrast can identify vascular compression during specific arm positions. Magnetic resonance angiography supports evaluation of vascular structures without ionizing radiation exposure. Nerve conduction studies may identify neurological abnormalities in true neurogenic thoracic outlet syndrome though typically negative in disputed neurogenic cases.
Treatment for thoracic outlet syndrome varies based on specific type and severity. Conservative treatment including physical therapy, postural correction, and activity modification helps many patients with neurogenic syndromes. Surgical treatment including first rib resection and scalenectomy supports selected patients with severe symptoms not responding to conservative care. Arterial thoracic outlet syndrome typically requires surgical intervention given the risk of arterial damage from chronic compression. Venous thoracic outlet syndrome often requires anticoagulation plus consideration of surgical decompression.
Outcomes research on thoracic outlet syndrome treatment shows variable results across different patient groups and treatment approaches. Conservative treatment helps approximately 60 to 80 percent of neurogenic patients without surgery. Surgical outcomes show good to excellent results in 70 to 90 percent of properly selected patients. Recurrence after surgery occurs in 10 to 30 percent of patients depending on follow-up duration. Patient selection criteria substantially affect outcomes with appropriate patient selection producing better outcomes than indiscriminate surgical intervention.
Adson Test Administration
- ✓Position patient comfortably seated or standing with affected arm relaxed at side
- ✓Establish baseline radial pulse quality through careful palpation before beginning maneuver
- ✓Position the affected arm extended slightly with shoulder externally rotated as required
- ✓Instruct patient on head turn direction matching the specific Adson variation being performed
- ✓Have patient take deep breath and hold while you palpate radial pulse throughout
- ✓Note any pulse changes including diminution or complete disappearance during the maneuver
- ✓Document specific findings including symptom reproduction if patient reports clinical correlation
- ✓Compare findings between bilateral testing supporting identification of significant side-to-side differences
- ✓Combine Adson findings with other provocative tests producing comprehensive thoracic outlet evaluation
Patient education about test procedures supports cooperative participation and accurate assessment. Explaining what the test involves and what findings might mean helps patients understand the examination process. Some patients feel anxious about provocative testing concerned that movements might cause harm. Clear explanation that the test simply assesses positional vascular changes typically alleviates these concerns supporting better cooperation. Patient comfort with the testing process produces better assessment quality than testing with anxious or guarded patients struggling to follow instructions appropriately.
Differential diagnosis considerations affect thoracic outlet syndrome evaluation beyond just Adson testing. Cervical radiculopathy from neck disc problems can produce similar arm symptoms requiring careful differentiation. Carpal tunnel syndrome and other peripheral nerve entrapments produce hand symptoms that may resemble thoracic outlet patterns. Pancoast tumors at the lung apex can compress neurovascular structures producing thoracic outlet-like symptoms requiring imaging evaluation. Cardiovascular conditions including coronary artery disease can produce arm pain potentially confused with thoracic outlet syndrome requiring appropriate cardiac evaluation.
Physical therapy approaches for thoracic outlet syndrome include postural correction, scalene stretching, pectoralis minor stretching, scapular stabilization, and nerve gliding exercises. Specialized physical therapy programs designed for thoracic outlet syndrome produce better outcomes than generic physical therapy. Many academic medical centers have dedicated thoracic outlet syndrome physical therapy protocols with specifically trained therapists. The specialized care produces substantially better outcomes than non-specialized care making referral to experienced centers valuable for affected patients.
Historical context for the Adson test development provides perspective on its current use. Dr. Alfred Washington Adson developed the test at the Mayo Clinic in the 1920s during an era when thoracic outlet syndrome recognition was relatively new. Subsequent decades have expanded understanding of the syndrome while questioning some early diagnostic approaches. Modern thoracic outlet syndrome practice combines Adson testing with various other assessments reflecting accumulated experience about what diagnostic approaches produce reliable results in clinical practice.
Inter-rater reliability of Adson testing varies across practitioners with experience affecting consistent assessment. Trained practitioners produce more reliable results than novice clinicians performing the maneuver. Specific technique variations across practitioners can affect findings even within the same general test category. Quality training programs in physical examination emphasize standardized technique supporting more reliable Adson testing across practitioners. Continuing education refreshing examination skills supports practitioners maintaining reliable testing capabilities throughout careers.
Pregnancy considerations affect thoracic outlet syndrome management. Pregnancy-related fluid retention can worsen thoracic outlet symptoms in patients with underlying compression. Postural changes during pregnancy affect compression. Some women develop thoracic outlet syndrome symptoms specifically during pregnancy. Management during pregnancy typically emphasizes conservative approaches with surgical intervention generally postponed until after delivery when medically possible. Most pregnancy-related thoracic outlet symptoms resolve after delivery with fluid normalization and postural recovery.

Adson Test Statistics
Thoracic Outlet Provocative Tests
Original provocative maneuver assessing pulse changes during arm positioning and head turning with deep breath hold maneuver. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Arms held in surrender position with hands opening and closing for 3 minutes assessing for symptom reproduction or pulse changes. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Hyperabduction of arm assessing for pulse diminution suggesting pectoralis minor space compression of neurovascular structures. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Shoulders back and down compressing the area between the clavicle and first rib assessing this specific anatomical space. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Variant of Adson with traction on the arm and palpation of pulse during deep breath hold maneuver. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Passive elevation of the shoulders relieving compression assessing whether symptoms improve with thoracic outlet decompression. Specific symptom presentations vary across patients requiring individualized clinical assessment beyond just categorical assignment.
Documentation of Adson test findings supports both individual patient care and clinical research. Specific documentation should include the test variation performed, baseline pulse quality, pulse changes during the maneuver, symptom reproduction if present, and the clinical interpretation. Standardized documentation supports consistent clinical communication across providers. Research applications using Adson testing benefit from precise documentation supporting reproducibility of study findings. The documentation discipline supports both clinical practice and continuing learning about thoracic outlet syndrome diagnosis.
Limitations of physical examination in thoracic outlet syndrome diagnosis affect overall diagnostic approach. The variable sensitivity and specificity of Adson and other provocative tests means clinical examination alone may not establish diagnosis confidently. Imaging studies and electrodiagnostic testing supplement physical examination supporting comprehensive evaluation. The diagnostic challenges produce ongoing debate about optimal diagnostic approaches with some clinicians emphasizing physical examination while others emphasize objective testing approaches in thoracic outlet syndrome evaluation.
Successful thoracic outlet syndrome evaluation requires careful integration of multiple diagnostic elements with experienced clinical judgment supporting accurate diagnosis and appropriate treatment selection for affected patients seeking relief from arm symptoms that can significantly impact quality of life.
Continued education about thoracic outlet syndrome supports better recognition and management of this challenging condition across healthcare disciplines beyond just specialty practice alone.
Patient outcomes improve substantially with appropriate diagnosis and treatment selection through experienced specialty care providers.
Adson Test Considerations
- + —
- + —
- + —
- + —
- + —
- + —
- − —
- − —
- − —
- − —
- − —
- − —
BMV Questions and Answers
About the Author
Attorney & Bar Exam Preparation Specialist
Yale Law SchoolJames R. Hargrove is a practicing attorney and legal educator with a Juris Doctor from Yale Law School and an LLM in Constitutional Law. With over a decade of experience coaching bar exam candidates across multiple jurisdictions, he specializes in MBE strategy, state-specific essay preparation, and multistate performance test techniques.